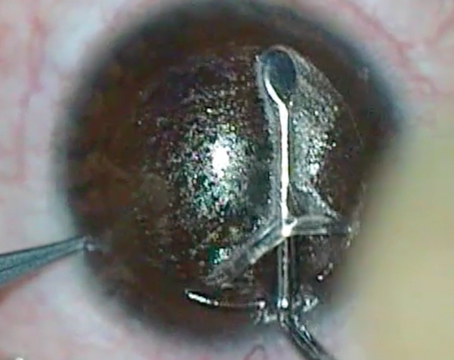
Suction Breaks
Surgeons say suction loss can result from a number of factors, but it doesn’t have to bring an end to the case.
“There are three main causes for suction loss,” says Chicago surgeon Surendra Basti, user of the IntraLase. “The most common reason is that you didn’t place the suction ring properly the first time, so making an adjustment can be useful in certain patients. In patients with narrow palpebral fissures, sometimes space is limited. If you turn the patient’s head away from the eye that’s having surgery, that causes the eyeball to rotate away from the nose, and creates a little extra space to place the suction ring.
“The second reason suction is lost is if a patient is a lid-squeezer,” Dr. Basti continues. “Sometimes, as soon as you separate the lids to put the suction ring in, he starts to squeeze. If you prompt the patient not to do that and add an anesthetic drop, that can help keep the eye anesthetized and help keep him from squeezing the lid shut. Also, putting a little anesthetic in the fellow eye and prompting the patient to keep it open can actually facilitate keeping the surgical eye open.
“The third common cause of suction loss is something that the surgeon can’t do much about, unfortunately,” says Dr. Basti. “Sometimes patients just have loose, boggy conjunctiva. In these cases, the conjunctiva closes the suction port rather than the eyeball itself, giving pseudo-suction. When this happens it’s challenging, and it’s not always possible to work around it. If you’re not able to do the case in such a patient, you can instead perform a surface ablation.”
Rochester surgeon Scott MacRae uses the Ziemer femtosecond laser, which uses a handpiece on an articulated arm to deliver the energy to the cornea. “Getting the handpiece onto the cornea and getting it centered take a bit of moving and angulation of the patient’s head,” Dr. MacRae says. “Often, I’ll have my assistant push down slightly on the lid speculum to get more clearance if it’s a small orbit.” Dr. MacRae notes that a special lid speculum, the ASICO AE1016 speculum, has been “fabulous” for helping to get the eye open to achieve suction. “It has 10-mm blades to open the lids wider, and a hexagonal shape to better fit the Ziemer’s suction ring,” he says.
Vancouver, Wash., surgeon Brian Will says that, though he doesn’t usually use a speculum, he may use an open-wire lid speculum if there’s a lot of redundant conjunctiva. The speculum’s design “tends to shove the conjunctiva back to the fornix, and gives you better exposure to get the vacuum ring into the eye,” he explains. “Another thing that really helps is using some downward compression, particularly if you’ve lost vacuum. Retropulsing the globe, so to speak, sort of forces the eye back into the orbit. In these cases, I’ll release the snapper that clips the pincers open and leave the pincers closed. That way, I can bring the cone down and use it to push the globe back a bit. I then gently crack the pincers open a little just to get the cone to start moving down into the docking port.”
|
“If a suction break occurs early, such as with a squeezer, you don’t have to change anything,” says Dr. Basti. “Redo the placement of the suction ring and restart the laser. But if it occurs once the laser is working on the eye, especially if it’s gone past the first few millimeters, it’s more challenging. If the laser hasn’t gone well into the cornea, and you’re just starting the procedure, changing the suction ring, but not the cone, is a good strategy. Sometimes these rings are defective. “If the break occurs when half the flap has been created, you can’t complete the case,” Dr. Basti adds. “Your choices are to abort and do surface ablation or redo the flap creation. If you choose to make a new flap, you have to start deeper than the original one, at least 40 to 50 µm deeper, as long as there’s adequate corneal thickness. However, when you then try to lift the new flap, be careful. You want to be in the plane of the new flap, not the partial one. I find it’s useful to enter the interface of the new flap distal to the aborted flap’s edge.”
Surgeons say if the suction break occurs during the creation of the side cut, you can place the ring again and program the laser to do only the side cut. To help ensure the cut isn’t made outside the diameter of the flap, surgeons recommend programming the laser to make the side cut 0.2 to 0.3 mm smaller than the flap.
A String of Pearls
In addition to methods for dealing with suction loss, surgeons also have several techniques they use to avoid complications in other phases of flap creation.
• Chilled, neutral proparacaine. Dr. Will says that using chilled proparacaine that’s pH-neutral is helpful in avoiding epithelial sloughing. “Proparacaine ships from its maker with a 4.5 pH—very acidic,” he says. “This is to keep it active for as long a period as possible, but it’s not helpful for the eye. We instill 15 drops of 0.1 mmol sodium hydroxide per bottle, which will bring most proparacaine solutions to a pH of 7. This markedly changes the negative effect of the proparacaine on the epithelium. Also, we have our proparacaine shipped to us on ice and then we freeze it solid—the maker doesn’t condone this but it doesn’t say you can’t do it, either. Then, the day before surgery, I thaw the bottles I want to use. Chilling the proparacaine and titrating its pH to neutral keeps the epithelium a lot healthier postop, and it minimizes the inflammatory mediators being released by the epithelium. Also, if you get some loose epithelium during the case, this preparation means you will almost never see that turn into a basement membrane issue or recurrent erosion.”
• Lifting the flap. Dr. MacRae says occasionally he’ll encounter areas of the flap that are difficult to lift. “Rather than ripping across that area, take the instrument you’re using for separation and come at the area from multiple directions,” he advises. “Come from the right, the left, above and below. That will slowly weaken the area that’s bound down.”
For retreatments where you’re relifting the flap, Dr. MacRae developed the MacRae flap flipper (ASICO), in which he has no financial interest. He adds that the Storz E9103 instrument is similar and works well, also. “The flipper is like a dandelion digger, with sharp inner blades,” he explains. “You sort of ski along the edge of the flap with it, and it cuts the edge where the epithelium is and separates the flap from the bed. However, one of the problems with this approach is you get some scrolling of the epithelium, which causes an epithelial defect. So, when I do a relift, rather than using the cutting edge of the flap flipper, I get into the interface with it and then lift it slightly, doing what I call ‘localized lifts’ that gradually lift the flap from the bed. This method avoids scrolling and the possible epithelial ingrowth that can occur in the area of the epithelial defect.”
• Corneal scars. If a patient has a pre-existing scar, the LASIK can still be successful, say surgeons. “The key is understanding what caused the scar,” says Dr. Will. “If it’s herpetic, don’t operate. If it’s from trauma, get a sense of how deep and opaque it is at the slit lamp. If you can’t determine that at the slit lamp, the OCT or Pentacam might help. During the surgery, I usually want to cut the flap below the scar if I can, depending on the corneal thickness and the amount of treatment. However, if it’s a mild to moderate scar, a new laser like the iFS or the 60 kHz IntraLase can cut right through it. If it’s denser, though, try to go deeper if possible.” REVIEW