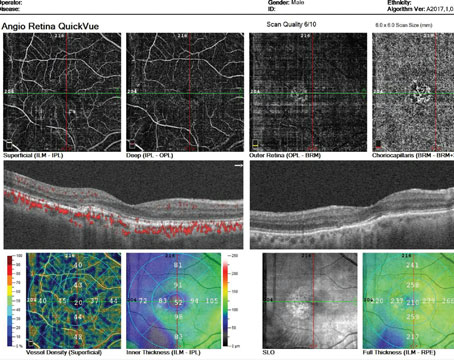
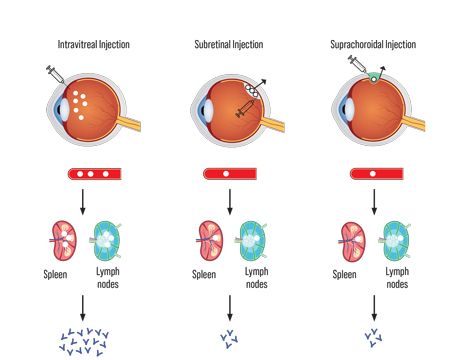
Phil Rosenfeld, MD, PhD, of the Bascom Palmer Eye Institute, introduced the use of bevacizumab as an off-label therapy for neovascular diseases of the posterior segment of the eye. In current ophthalmic use, bevacizumab is delivered almost exclusively as an intravitreal agent. However, Dr. Rosenfeld initially employed bevacizumab intravenously as a therapy for wet age-related macular degeneration and showed it was successful.1 Soon thereafter, Dr. Rosenfeld and his colleagues employed bevacizumab via the intravitreal route, and a myriad of subsequent studies performed worldwide confirm its safety and efficacy as a therapy for wet AMD.2-5
Since 2006, a wealth of data has emerged linking genetic variants in complement system proteins to AMD.6-9 During that time, the expectation of successful therapy for AMD based on complement system manipulation has been entertained. Seeking to mirror his path to success with bevacizumab for wet AMD, Dr. Rosenfeld set up a clinical trial to test whether a currently Food and Drug Administration-approved anti-complement drug—eculizumab—delivered via an intravenous route might be successful in slowing progression of dry AMD, the so-called COMPLETE trial.
Background and Methods
Eculizumab (Soliris, Alexion Pharmaceuticals) is an antibody to human complement factor 5. It is FDA-approved for an exceedingly rare disease called paroxysmal nocturnal hemoglobinuria (PNH). The standard dose is 900 mg intravenously every two weeks. Eculizumab is said to be the most expensive drug in the world, with a years’ worth of therapy costing $400,000.
The COMPLETE trial was a prospective, randomized, Phase II, single-center, placebo-controlled trial; the results were presented as a poster at ARVO 2012 (Garcia Filho C, et al. IOVS 2012;53:ARVO E-Abstract 2045). There were three arms in the trial:
• Eculizumab 900 mg intravenously weekly for four weeks then 1,200 mg every two weeks for six months (high dose);• Eculizumab 600 mg intravenously weekly for four weeks, then 900 mg every two weeks for six months (standard dose); and• Placebo (saline) intravenously weekly q four weeks, then every two weeks for six months.
• Change in drusen volume as measured by spectral domain optical coherence tomography; and• Change in geographic atrophy area as measured by color photographs, fundus autofluorescence (FAF) and OCT.
Other measured endpoints included: normal luminance and low luminance visual acuity; change in choroidal thickness on OCT; and conversion from dry AMD to neovascular AMD.
Systemic side effects and the degree of complement inhibition in the blood were monitored as well.
Results of the Trial
The major result of the trial was that intravenous eculizumab at the doses studied over six months failed to detectably slow the progression of GA. In addition, there was no detectable change in drusen volume or VA in the treated patients studied versus the controls. Systemic complement inhibition was achieved and no serious systemic side effects were noted.
Of interest was that none of the eculizumab treated patients (n=20) converted from dry to wet AMD during the course of the study but two of the 10 (20 percent) of the placebo treated patients did.
Future Directions
The most likely reason why eculizumab failed in the COMPLETE study is that progression of geographic atrophy is independent of complement activation. This is consistent with previous genetic studies showing that the growth of geographic atrophy was independent of the number of at-risk alleles carried by the subjects.
Interestingly, the COMPLETE study did show that the growth of drusen volume was dependent on the number of complement at-risk alleles carried by the subjects; yet despite this, complement inhibition had no effect on drusen volume. The failure to detect a linkage between complement-dependent drusen growth and systemic complement inhibition suggests that the delivery method (intravenous) was inadequate to stop complement inhibition at the critical site. Alternative explanations include the possibility that the trial duration was too short, or that the trial had too few patients, and so was inadequately powered to identify a therapeutic response.
It is intriguing to speculate that a different endpoint may have been successful, such as halting the progression from dry AMD to wet AMD using complement blockade, since no patient who received eculizumab converted to wet AMD during the trial. COMPLETE did not look at this as an outcome directly, however, and the study was inadequately powered to make any definitive conclusions regarding this specific endpoint.
The COMPLETE study gave us several other nuggets of important information that may help to guide future dry AMD studies. These include:
• SD-OCT, FAF and fluorescein angiography all can image geographic atrophy successfully.• Increasing drusen volume in an eye is most closely associated with the number of high-risk complement alleles in the patient’s genotype, as opposed to other measureable clinical factors.• A baseline visual acuity measurement called the “low luminance deficit” correlated most closely with the risk of GA enlargement.
So to summarize, systemic complement inhibition does not appear to be a successful strategy in slowing down GA in the short term. Ongoing studies of complement inhibition using the intravitreal route may yield different results. REVIEW
Dr. Duker is director of the New England Eye Center, and a professor and chair of ophthalmology at Tufts Medical Center, Tufts University School of Medicine. You can reach him by e-mail at: jduker@tuftsmedicalcenter.org.
1. Moshfeghi AA, Rosenfeld PJ, Puliafito CA, et al. Systemic Bevacizumab (Avastin) for Neovascular Age-Related Macular Degeneration. Ophthalmology 2006;113:2002.
2. Rosenfeld PJ, Fung AE, Puliafito CA. Optical coherence tomography findings after an intravitreal injection of Bevacizumab (Avastin) for macular edema from central retinal vein occlusion. Ophthalmic Surg Lasers Imaging 2005;36:336-339.
3. Rosenfeld PJ, Moshfeghi AA, Puliafito CA. Optical coherence tomography findings after an intravitreal injection of Bevacizumab (Avastin) for neovascular age-related macular degeneration. Ophthalmic Surg Lasers Imaging 2005;36:270-271.
4. The IVAN Study Investigators. Ranibizumab versus Bevacizumab to Treat Neovascular Age-related Macular Degeneration. Ophthalmology 2012;119:1399-1411.
5. CATT Research Group. Ranizumab and bevacizumab for treatment of age-related macular degeneration. Ophthalmology 2012;119:1388-1398.
6. Klein RJ, Zeiss C, Chew EY, et al. Complement factor H polymorphism in age-related macular degeneration. Science 2005;308(5720):385–389.
7. Hageman GS, Anderson DH, Johnson LV, et al. A common haplotype in the complement regulatory gene factor H (HF1/CFH) predisposes individuals to age-related macular degeneration. Proc Natl Acad Sci USA 2005;102(20):7227-7232.
8. Haines JL, Hauser MA, Schmidt S, et al. Complement factor H variant increases the risk of age-related macular degeneration. Science 2005;308(5720):419-421.
9. Gold B, Merriam JE, Zernant J, et al. Variation in factor B(BF) and complement component 2 (C2) genes is associated with age-related macular degeneration. Nat Genet 2006; 38(4):458-462.