Epidemiology
BSRC is a disease seen almost exclusively in the Caucasian population with a mean age of onset of 53 years. A slight female preponderance is present, ranging from a reported 51.7 percent to 72.7 percent in various studies. Given its rarity, little data exists on the true national or global prevalence of the disease although it accounts for between 0.6 and 1.5 percent of cases referred to specialty uveitis centers, or 6 to 7 percent of those with posterior uveitis.1
Pathogenesis
Retinal autoimmunity is thought to play an important role in the pathogenesis of BSRC, possibly by enhanced expression self-peptides to T-lymphocytes through the A29 molecule or through molecular mimicry with microbial antigen. The HLA-A29 haplotype, which is found in 85 to 98 percent of patients with BSRC, confers significantly increased risk for the development of this disease.2,3 However, it should be noted that it is present in 7 percent of the general Caucasian population.4
Clinical Findings
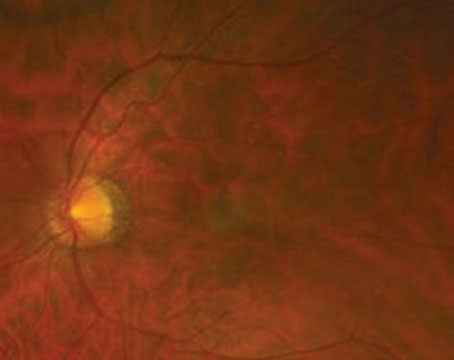
Patients often present in the subacute phase of the disease with floaters, photopsias, scotomata, nyctalopia, and poor color and contrast sensitivity.5 Not infrequently, they may complain of blurry vision despite fairly good Snellen visual acuity. This may be attributable to metamorphopsia and poor contrast sensitivity.1 Photophobia and pain are infrequent findings as are clinical signs and structural complications of anterior segment inflammation such as posterior synechiae; however, mild vitritis is almost universally present.1 Macular edema as seen clinically, angiographically or by optical coherence tomography is the most common cause of central vision loss in patients with BSRC.1 Retinal vasculitis manifests predominantly as a periphlebitis, is best delineated by fluorescein angiography and is an important sign of disease activity.6,7 Funduscopic findings include ovoid cream-colored lesions at the level of the choroid and retinal pigment epithelium, which are typically post-equatorial in location, have a nasal and radial distribution, and are best visualized by indirect ophthalmoscopy8,9 (See Figure 1). Funduscopic findings later in the disease include vascular attenuation,6 nerve pallor and diffuse retinal atrophy with pigmentary changes6,10,11 progressing ultimately to extinguished amplitudes on electroretinography.
Imaging
FA yields inconsistent findings and typically fails to highlight the birdshot lesions themselves. It may, however, highlight important components of active disease including retinal vasculitis, macular edema and optic nerve head leakage (See Figure 2). Late findings include retinal vascular attenuation, optic atrophy, epiretinal membrane formation6,7 and the uncommon occurrence of choroidal neovascularization.12,13
Indocyanine green angiography (See Figure 3) on the other hand discloses multiple hypofluorescent spots, which correspond to funduscopic lesions and are typically more numerous than those appreciated on clinical examination or on FA. They are typically larger than those seen with multiple evanescent white dot syndrome (MEWDS) or multifocal choroiditis and panuveitis (MCP), and smaller than those seen with acute posterior multifocal placoid pigment epitheliopathy (APMPPE) or Vogt-Koyanagi-Harada disease (VKH) with a distribution around the choroidal vessels and not clustered on the optic nerve.
|
As with other posterior uveitides, OCT is invaluable in the detection and quantification of macular edema, intraretinal and subretinal fluid associated with choroidal neovascularization.16 High-resolution OCT is particularly useful in the evaluation of reversible and irreversible macular changes in BSRC. Macular thinning and loss of the inner segment—outer segment (IS/OS) demarcation has been noted using both time domain and spectral domain OCT but are more accurately visualized with the latter modality. The degree of measurable macular thinning was associated with a loss of thickness of the segment subtending the proximal border of the outer plexiform layer and the Bruch’s membrane/choroid interface suggesting that macular atrophy in BSRC occurs largely in the outer retina.17,18 Restoration of macular outer retinal architecture has been described with the institution of systemic immunomodulatory therapy (IMT).19
Psychophysical Testing
Electroretinography and perimetry are invaluable in the longitudinal follow-up of patients with BSRC. Visual field abnormalities are common and include generalized constriction of the peripheral visual field, central and paracentral scotomata, and enlargement of the blind spot.6,8,9,20,21 While reports of visual field testing in the literature are fraught with inconsistency, these defects have been shown to both progress over time in association with disease activity8,9,20,22,23 and to improve under systemic IMT,5,24-26 suggesting that standardized evaluations may provide data that is useful in the longitudinal management of these patients.1
A characteristic electroretinographic abnormality in BSRC is a prolongation of 30 Hz flicker implicit time.27,28 In addition to cone B wave implicit times, dim rod scotopic amplitudes are also severely attenuated with both indices declining with progression of the disease.29 Institution of IMT has been shown to stabilize or even partially reverse the decline of electroretinographic changes, which can occur even in the absence of overt signs of inflammation.30
Differential Diagnoses
The diagnosis of BSRC is a clinical one, and while highly associated with the disease, HLA-A29 positivity in and of itself is not diagnostic of the disease, as HLA-A29-negative cases exist. Conversely, the absence of the typical clinical features of BSRC in the presence of the HLA-A29 positivity should prompt consideration of an alternative diagnosis, as 7 percent of the general population carries this haplotype. A thorough medical and ophthalmic history, review of systems, directed laboratory investigations, and imaging studies serve to differentiate the various inflammatory, infectious and neoplastic entities that may mimic BSRC (See Table 1). Infectious entities that may produce white dots in the retina and choroid, such as syphilis and tuberculosis, must be considered in the differential diagnosis, as these require specific antimicrobial therapy.
|
In contrast to birdshot, the cream-colored lesions of APMPPE have a plaque-like morphology, are located predominantly in the posterior pole, and exhibit characteristic angiographic features of early blockage and late staining. Moreover, the acute lesions of AMPPE typically resolve with retinal pigment epithelial hyperpigmentation, whereas those with BSRC do not.35,36
Another white dot syndrome to be distinguished from BSRC includes MCP, which typically exhibits smaller, discrete, punched out hyper- and hypo-pigmented lesions that block early, stain late, and are typically clustered around the optic nerve.37
Bilateral choroidal lesions appearing in the acute uveitic phase of VKH disease may be distinguished from those of BSRC by the presence of exudative retinal detachment with pinpoint areas of hyperfluorescence at the level of the RPE with subneurosensory pooling on FA versus retinal vascular inflammation. In addition, VKH is a systemic disease with characteristic extraocular differentiating features.38
Finally, patients with primary intraocular lymphoma may present with multiple bilateral yellowish lesions and vitritis; however, their subretinal, sub-RPE location in the clinical context usually distinguishes them from those seen in BSRC.39-42
Clinical Course
BSRC is often described as having two distinct phases with an acute phase, dominated by significant vitritis, cystoid macular edema and vision loss followed by a subsequent period of clinically silent, insidious global photoreceptor loss punctuated by waxing and waning inflammatory episodes. While some investigators have suggested that as many as 20 percent of patients with birdshot may have self-limited disease,8 in the majority of patients, long-term follow-up suggests a course marked by multiple inflammatory exacerbations and progressive visual loss replete with structural complications and global retinal dysfunction over the long term, independent of previous oral corticosteroid therapy.2,6,7,9,10,23,24
|
Treatment
While periocular, ocular, intravitreal and systemic corticosteroids may be effective in the short-term management of vitritis and macular edema, they are of inconsistent efficacy in the long run. Unacceptably high maintenance doses of prednisone are required, resulting in frequent development of serious adverse effects when used as chronic monotherapy.
Given the guarded visual prognosis, the early introduction of steroid-sparing IMT at the outset, has been advocated in the treatment of birdshot retinochoroidopathy, as extended treatment is anticipated in most patients.43 Indeed, numerous studies have demonstrated that both preservation of visual function with a reduction of inflammation and macular edema, and preservation of global retinal integrity as well as the induction of long-term remission are possible in patients with birdshot managed with steroid-sparing IMT. 8,23,24,26,30,44-46
Systemic immunomodulatory options include anti-metabolites, T-cell transduction/calcineurin inhibitors, biologics, intravenous immunoglobulin (IVIg)47 and emerging use of other biologic therapies alone or in combination. For patients unable to tolerate systemic corticosteroids or IMT, the sustained-release fluocinolone acetonide implant (Retisert)may be a viable alternative.48,49 The efficacy of this implant and the decision to use it as initial therapy should be tempered by the almost universal development of cataract and high incidence of ocular hypertension and glaucoma, requiring incisional surgery in more than a third of patients.44
Symptomatic patients with BSRC who present with or develop vitritis, retinal vasculitis, macular edema or evidence of peripheral retinal dysfunction should be treated. In an initial retrospective study of 19 patients with BSRC and in the subsequent study of 28 in patients from the same institution treated with very low initial doses of cyclosporine (2.5 mg/kg/day) alone or in combination with antimetabolites (methotrexate, azathioprine, mycophenolate mofetil) or daclizumab, a favorable visual outcome, inflammatory control, stabilization of electroretinographic parameters and the absence of demonstrable nephrotoxic side effects were achieved.24,30
Similarly, a recent retrospective analysis of 76 HLA-A 29-positive birdshot patients, 46 of whom were followed for five years and 18 for more than 10 years, demonstrated that visual outcomes were better for those treated with methotrexate as compared to untreated individuals and corticosteroid-based regiments.11,30
While the use of methotrexate or cyclosporine alone may be superior to the long-term use of systemic corticosteroids in the treatment of BSRC, monotherapy with cyclosporine, in our experience, has been associated with need for exceedingly prolonged therapy with the recurrences of inflammation with tapering of this medication.
In an effort to achieve durable remission of inflammation within two years, the combination of cyclosporine or mycophenolate has been exploited in 49 patients (98 eyes), over a mean follow up time of 52 months. At that one-year time point, vitreous inflammatory scores, the presence of angiographic leakage, but not the presence of cystoid macular edema, were significantly reduced from baseline, with 67 percent of patients achieving inflammatory control with no deterioration of electroretinographic indices.46
The use of monoclonal antibodies to tumor necrosis factor α (TNF-α) is an emerging treatment alternative to conventional IMT, either alone or in combination. In a recent retrospective report of 22 patients with BSRC refractory to conventional IMT treated with infliximab, inflammatory control was achieved in 88.9 percent of patients at the one year follow-up.51 Over the course of the study, six patients discontinued infliximab due to adverse effects.
In summary, birdshot retinochoroidopathy is a chronic, progressive sight-threatening disease, which requires the early introduction of immunomodulatory therapy in an effort to limit ocular structural damage, preserve global visual function and induce long-term remission. Markers of active and progressive disease, which may influence treatment decisions, include not only clinical indices of intraocular inflammation, but also those seen on imaging studies, particularly fluorescein angiography, perimetry and electroretinography. REVIEW
Dr. Vitale is a professor of ophthalmology and visual sciences. chief of the Uveitis Division and a member of the Vitreoretinal Division at John A Moran Eye Center, University of Utah. Contact him at (801) 581-2352 or e-mail: albert.vitale@hsc.utah.edu. Dr. Shakoor is a retina fellow at the Moran Eye Center.
1. Shah KH, Levinson RD, Yu F, et al. Birdshot chorioretinopathy. Surv Ophthalmol 2005;50:519-41.
2. Nussenblatt RB, Mittal KK, Ryan S, Green WR, Maumenee AE. Birdshot retinochoroidopathy associated with HLA-A29 antigen and immune responsiveness to retinal S-antigen. Am J Ophthalmol 1982;94:147-58.
3. Baarsma GS, Priem HA, Kijlstra A. Association of birdshot retinochoroidopathy and HLA-A29 antigen. Curr Eye Res 1990;9 Suppl:63-8.
4. Brezin AP, Monnet D, Cohen JH, Levinson RD. HLA-A29 and birdshot chorioretinopathy. Ocul Immunol Inflamm 2011;19:397-400.
5. Ladas JG, Arnold AC, Holland GN. Control of visual symptoms in two men with birdshot retinochoroidopathy using low-dose oral corticosteroid therapy. Am J Ophthalmol 1999;128:116-8.
6. Gass JD. Vitiliginous chorioretinitis. Arch Ophthalmol 1981;99:1778-87.
7. Ryan SJ, Maumenee AE. Birdshot retinochoroidopathy. Am J Ophthalmol 1980;89:31-45.
8. Gasch AT, Smith JA, Whitcup SM. Birdshot retinochoroidopathy. Br J Ophthalmol 1999;83:241-9.
9. Priem HA, Oosterhuis JA. Birdshot chorioretinopathy: Clinical characteristics and evolution. Br J Ophthalmol 1988;72:646-59.
10. Rothova A, Berendschot TT, Probst K, van Kooij B, Baarsma GS. Birdshot chorioretinopathy: Long-term manifestations and visual prognosis. Ophthalmology 2004;111:954-9.
11. Rothova A, Norel AO, Los LI, Berendschot TT. Efficacy of Low-Dose Methotrexate Treatment in Birdshot Chorioretinopathy. Retina 2011.
12. Brucker AJ, Deglin EA, Bene C, Hoffman ME. Subretinal choroidal neovascularization in birdshot retinochoroidopathy. Am J Ophthalmol 1985;99:40-4.
13. Godel V, Baruch E, Lazar M. Late development of chorioretinal lesions in birdshot retinochoroidopathy. Ann Ophthalmol 1989;21:49-52.
14. Koizumi H, Pozzoni MC, Spaide RF. Fundus autofluorescence in birdshot chorioretinopathy. Ophthalmology 2008;115:e15-20.
15. Giuliari G, Hinkle DM, Foster CS. The spectrum of fundus autofluorescence findings in birdshot chorioretinopathy. J Ophthalmol 2009;2009:567693.
16. Gallagher MJ, Yilmaz T, Cervantes-Castaneda RA, Foster CS. The characteristic features of optical coherence tomography in posterior uveitis. Br J Ophthalmol 2007;91:1680-5.
17. Birch D, Williams P, Callanan D, Wang R, et al. Macular atrophy in birdshot retinochoroidopathy: An optical coherence tomography and multifocal electroretinography analysis. Retina 2010;30:930-7.
18. Forooghian F, Yeh S, Faia L, Nussenblatt R. Uveitic foveal atrophy: Clinical features and associations. Arch Ophthalmol 2009;127:179-86.
19. Forooghian F, Gulati N, Jabs DA. Restoration of retinal architecture following systemic immunosuppression in birdshot chorioretinopathy. Ocul Immunol Inflamm 2010;18:470-1.
20. Fuerst DJ, Tessler HH, Fishman GA, Yokoyama MM, Wyhinny GJ, Vygantas CM. Birdshot retinochoroidopathy. Arch Ophthalmol 1984;102:214-9.
21. Priem HA, De Rouck A, De Laey JJ, Bird AC. Electrophysiologic studies in birdshot chorioretinopathy. Am J Ophthalmol 1988;106:430-6.
22. de Courten C, Herbort CP. Potential role of computerized visual field testing for the appraisal and follow-up of birdshot chorioretinopathy. Arch Ophthalmol 1998;116:1389-91.
23. Oh KT, Christmas NJ, Folk JC. Birdshot retinochoroiditis: long term follow-up of a chronically progressive disease. Am J Ophthalmol 2002;133:622-9.
24. Vitale AT, Rodriguez A, Foster CS. Low-dose cyclosporine therapy in the treatment of birdshot retinochoroidopathy. Ophthalmology 1994;101:822-31.
25. Le Hoang P, Girard B, Deray G, et al. Cyclosporine in the treatment of birdshot retinochoroidopathy. Transplant Proc 1988;20:128-30.
26. Thorne JE, Jabs DA, Peters GB, Hair D, Dunn JP, Kempen JH. Birdshot retinochoroidopathy: Ocular complications and visual impairment. Am J Ophthalmol 2005;140:45-51.
27. Holder GE, Robson AG, Pavesio C, Graham EM. Electrophysiological characterisation and monitoring in the management of birdshot chorioretinopathy. Br J Ophthalmol 2005;89:709-18.
28. Zacks DN, Samson CM, Loewenstein J, Foster CS. Electroretinograms as an indicator of disease activity in birdshot retinochoroidopathy. Graefes Arch Clin Exp Ophthalmol 2002;240:601-7.
29. Sobrin L, Lam BL, Liu M, Feuer WJ, Davis JL. Electroretinographic monitoring in birdshot chorioretinopathy. Am J Ophthalmol 2005;140:52-64.
30. Kiss S, Ahmed M, Letko E, Foster CS. Long-term follow-up of patients with birdshot retinochoroidopathy treated with corticosteroid-sparing systemic immunomodulatory therapy. Ophthalmology 2005;112:1066-71.
31. Brinkman CJ, Rothova A. Fundus pathology in neurosarcoidosis. Int Ophthalmol 1993;17:23-6.
32. Brod RD. Presumed sarcoid choroidopathy mimicking birdshot retinochoroidopathy. Am J Ophthalmol 1990;109:357-8.
33. Yoshioka T, Yoshioka H, Tanaka F. [Birdshot retinochoroidopathy as a new ocular sign of the sarcoidosis]. Nippon Ganka Gakkai Zasshi 1983;87:283-8.
34. Read RW, Rao NA, Sharma OP. Sarcoid choroiditis initially diagnosed as birdshot choroidopathy. Sarcoidosis Vasc Diffuse Lung Dis 2000;17:85-6.
35. Ryan SJ, Maumenee AE. Acute posterior multifocal placoid pigment epitheliopathy. Am J Ophthalmol 1972;74:1066-74.
36. Gass JD. Acute posterior multifocal placoid pigment epitheliopathy. Arch Ophthalmol 1968;80:177-85.
37. Dreyer RF, Gass DJ. Multifocal choroiditis and panuveitis. A syndrome that mimics ocular histoplasmosis. Arch Ophthalmol 1984;102:1776-84.
38. Moorthy RS, Inomata H, Rao NA. Vogt-Koyanagi-Harada syndrome. Surv Ophthalmol 1995;39:265-92.
39. Chatzistefanou K, Markomichelakis NN, Christen W, Soheilian M, Foster CS. Characteristics of uveitis presenting for the first time in the elderly. Ophthalmology 1998;105:347-52.
40. Gupta R, Murray PI. Chronic non-infectious uveitis in the elderly: Epidemiology, pathophysiology and management. Drugs Aging 2006;23:535-58.
41. Kirsch O, Lautier-Frau M, Labetoulle M, Offret H, Frau E. [Characteristics of uveitis presenting de novo in the elderly]. J Fr Ophtalmol 2003;26:720-4.
42. Sen HN, Bodaghi B, Hoang PL, Nussenblatt R. Primary intraocular lymphoma: diagnosis and differential diagnosis. Ocul Immunol Inflamm 2009;17:133-41.
43. Jabs DA, Rosenbaum JT, Foster CS, et al. Guidelines for the use of immunosuppressive drugs in patients with ocular inflammatory disorders: recommendations of an expert panel. Am J Ophthalmol 2000;130:492-513.
44. Kempen JH, Altaweel MM, Holbrook JT, et al. Randomized comparison of systemic anti-inflammatory therapy versus fluocinolone acetonide implant for intermediate, posterior, and panuveitis: The multicenter uveitis steroid treatment trial. Ophthalmology 2011;118:1916-26.
45. Becker MD, Wertheim MS, Smith JR, Rosenbaum JT. Long-term follow-up of patients with birdshot retinochoroidopathy treated with systemic immunosuppression. Ocul Immunol Inflamm 2005;13:289-93.
46. Cervantes-Castaneda RA, Gonzalez-Gonzalez LA, Cordero-Coma M, Yilmaz T, Foster CS. Combined therapy of cyclosporine A and mycophenolate mofetil for the treatment of birdshot retinochoroidopathy: A 12-month follow-up. Br J Ophthalmol 2013.
47. LeHoang P, Cassoux N, George F, Kullmann N, Kazatchkine MD. Intravenous immunoglobulin (IVIg) for the treatment of birdshot retinochoroidopathy. Ocul Immunol Inflamm 2000;8:49-57.
48. Srivastava SK, Nguyen QD, Callanan D, Goldstein DA, Albini TA. The Use Of The Fluocinolone Acetonide (Retisert) Implant In Patients With Birdshot Choroidopathy. Invest Ophthalmol Vis Sci 2011;52:2751.
49. Rush RB, Davis J, Goldstein D, Tessler H, Lin P, Meghpara B. Birdshot Chorioretinopathy and Fluocinolone Acetonide Intravitreal Sustained Release Devices: An Analysis of Efficacy and Complications. Invest Ophthalmol Vis Sci 2009;50:6044.
50. Cervantes-Castaneda RA, Bhat P, Fortuna E, Acevedo S, Foster CS. Induction of durable remission in ocular inflammatory diseases. Eur J Ophthalmol 2009;19:118-23.
51. Artornsombudh P, Gevorgyan O, Payal A, Siddique SS, Foster CS. Infliximab Treatment of Patients with Birdshot Retinochoroidopathy. Ophthalmology 2012.