It's often said that about 50 percent of patients with glaucoma don't know they have it. But when you look at most prevalence studies, the percentage is even higher—about 80 percent of patients may fall into this category. So there's an enormous population of people who are at risk of losing vision from "the sneak thief of sight," who may not take action until they've already lost a significant portion of their vision.
This is certainly a good argument for glaucoma screening—something that many of us already do. However, glaucoma screening in its current form has several limitations, and like all medical screening it requires time, money and manpower. So it's legitimate to ask whether screening for glaucoma is worth the costs, and whether more of us should be undertaking it in our communities.
Glaucoma Screening: The Benefits
Screening in a traditional sense means identifying people who are at high risk of having a specific disease; it normally involves one or two tests. It's different from a diagnostic exam where you try to determine whether or not the patient has the disease. This distinction is important because, in glaucoma, for example, we don't have enough manpower to do a complete examination of everybody in the
It's not hard to see the potential benefits of such an endeavor. One, of course, is that you do find individuals with glaucoma who clearly would not have gone to a clinic for an eye exam. Many people are far more willing to be tested with an FDT perimeter at a health fair than to visit a doctor's office. And if you find a sign of trouble, that gets these people into the health-care system.
Furthermore, there are benefits beyond simply detecting disease. Screening also educates people about the signs and symptoms of glaucoma. Even if passers-by don't participate in the screening, they see the sign that says that glaucoma can occur in family members of those who have the disease. It starts a discussion between the person and his family; then members of the family go and have an eye exam. Simply educating people about glaucoma is extremely important.
The educational value of community screenings is difficult to measure—but knowledge is a powerful weapon against a silent, asymptomatic disease that can rob you of your vision. Sadly, every week a patient comes into our clinic who has had undiagnosed glaucoma for a long time, without any treatment. Earlier treatment could have allowed him to retain a significant part of his vision.

Glaucoma Screening: The Downsides
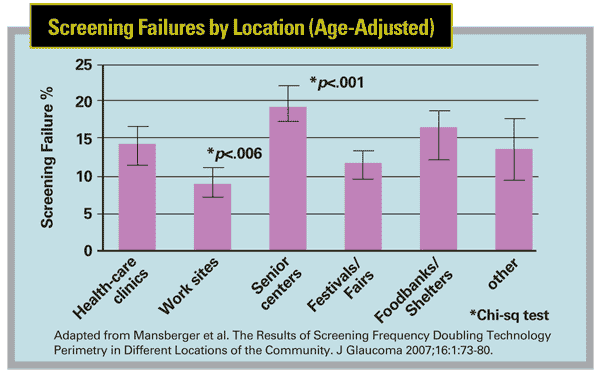
But are these benefits worth the resources required? The costs are not negligible. In one of our studies we found that an eight-hour day of testing at a community fair involving two technicians costs approximately $300 in labor (no equipment or overhead costs included) and this allowed the testing of about 100 participants. A group this size averaged a 10.7 percent screening failure rate. If you assume a predictive value of 40 percent, this screening would detect four participants with glaucoma at a cost of $75 per case of glaucoma detected. Using similar math for a senior center, with a greater percentage of screening failures—around 27 percent in our study—the screening cost comes to about $27 per case uncovered.1
Here are some other considerations:
• Is screening accurate? Screening tests are not 100-percent accurate, so we may inappropriately label someone as having a disease he doesn't have. That person with a false positive result walks away from a screening more depressed and anxious, robbing him of his perceived health. Conversely, some patients who really do have early glaucoma may not be picked up by the screening test; they walk away believing they won't need to have an eye exam for a long time.
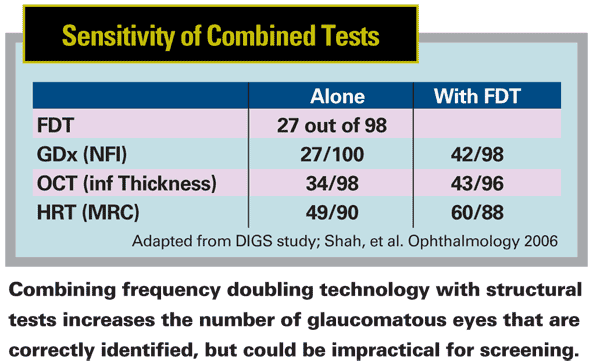
So how accurate is our current glaucoma screening protocol? We conducted a study in which we announced via a newspaper article that we were doing a free screening in our office; those who came in had the FDT screening test followed by a full eye exam.2 This study was in large part meant to determine how well the FDT instrument did compared to the full eye exam. We found that 36 percent of patients who failed the FDT screening test did, in fact, have glaucoma. Perhaps even more interesting, we found that the majority of those who failed the screening test had at least one of a host of different ocular diseases; 24 percent had cataract; 17 percent had retinal disease; 12 percent had miscellaneous problems, including other diseases such as anterior ischemic optic neuropathy. Only 25 percent were considered normal upon examination. So, the screening we conducted was not necessarily specific for glaucoma.
Was the screening worth the effort? That depends on your perspective; only 36 percent turned out to have verifiable glaucoma, but 75 percent had some ocular condition that might benefit from treatment.
• Do patients actually follow-up?In one study designed to determine the extent of follow-up, we conducted screenings and then called those who had negative results three to six months after screening, asking whether they had had an eye exam, and if so, what the diagnosis was.3 When participants had a visual field defect that was repeatable with FDT screening, we'd give them a sheet that explained the result, a 1-800 toll-free number to call for providers in their area who were willing to see them, and the offer of a free eye exam at Devers Eye Institute. About 69 percent followed up within six months of the screening test. (Other studies have found a follow-up rate as low as 41 percent.)4 We found that older age, female gender and having a high school education were more likely to be associated with follow-up.
The unfortunate reality is that even when people learn about the risk of glaucoma, even if they have a printout that says they're at risk, and even though they're provided free health care and free transportation, a significant proportion do not follow up. It may be that they're fearful about the possibility of losing their vision, and think that if they don't have an eye exam it's less likely to happen. (Ignorance, as they say, is bliss.) In one of our studies, the number one reason given for failure to follow up was that the participants just didn't believe the results. They didn't have symptoms, so despite the printout of the visual field with the dark spot on it, they didn't believe it. (See table, above.) Hopefully, as our understanding improves, we'll find ways to improve the follow-up percentages.
• Is the value of screening proven? The Association for Healthcare Research and Quality, which offers recommendations on whether screening of different kinds should be adopted, has said that screening for glaucoma isn't ready for prime time, unlike some other screening processes (such as screening for breast cancer). They're not saying it's a bad idea; they're just saying that the evidence showing the value of glaucoma screening isn't yet sufficient to earn their recommendation. For example, we don't yet know which stage of glaucoma is optimal to detect. Maybe we only need to pick it up when the patient has moderate disease in order to prevent changes in quality of life, as opposed to picking it up before the patient has any visual field loss. We don't have conclusive data either way.
•Does screening benefit the practice? At a fundamental level, screening makes sense based on our job description as ophthalmologists; helping the community and educating people is a part of our mission. And, we know from research that screenings do help educate the community regarding glaucoma and eye disease.
Will screening in the community bring more patients into your practice? There isn't any definitive data on this, but my experience has led me to believe it's unlikely, for two reasons: First, our follow-up study found that only about two-thirds of those identified as potentially having a problem actually pursued it. Second, if you uncover evidence that something may be wrong, many of those who do follow-up will go to a different doctor either because they already have a family eye doctor, or because they'd like to get a second opinion. (Remember, many people don't want to believe a negative result.) So bringing patients into your practice is not a major reason to do screening.
Making the Most of Screening
If you plan to offer screening in your community, there are several things you can do to help make it worth the effort:
• Use the right technology. For screening, you want a test you can do rapidly that's accurate, portable and highly associated with the disease. Tonometry is a poor screening tool because a large proportion of patients with glaucoma don't have elevated IOP—and conversely, a large proportion of people have high IOP but no glaucoma. Therefore, most glaucoma screening tests examine the visual field and/or optic disc.
Both of the latter approaches have pros and cons, but a visual field test has one major advantage: When a visual field test finds a defect and the result is repeatable, that will be highly associated with disease affecting peripheral vision. The disease may not always be glaucoma; it could be retinitis pigmentosa or cataract, or a number of other things. But if an individual has a visual field defect, it will usually be associated with real disease and decreased quality of life. (Of course, the patient could simply be having trouble taking the test; that's one reason we repeat the test when the outcome isn't positive.)
Among the visual field tests, there are several advantages to screening with FDT perimetry. One is that it's a quick test—it usually takes three minutes per eye or less. A second advantage is that you can have a fair amount of refractive error and still get an accurate result. That makes it good for screening out in the community where a large number of people have some uncorrected refractive error. Third, it's very portable; it fits in a little suitcase and you can carry it anywhere. We did screening with the FDT in
It's important to note that there are two different FDT instruments: the screening device and the Humphrey Matrix. They look similar but provide different mechanisms of testing: The Matrix has a slightly smaller spot size, so it checks more locations, which makes it feasible for monitoring glaucoma progression. The screening FDT, with its larger spot size, isn't ideal for following patients with glaucoma, but this large spot size makes it easier for participants at a screening to reliably perform the test. (The screening instrument is the one that's been used in most of the visual field studies done with FDT.)
• Minimize potential testing problems. To maximize the effectiveness of the test, have the patient wear any refractive correction that's needed. Make sure the patient is comfortable and minimize any external audio or visual distractions. Perhaps most important, if you do screening with a visual field test and get an abnormal result, repeat the test. We've found that at least 30 percent of abnormal visual field results reverted to normal upon repeat testing, so this is extremely important. (However, you don't need to repeat a normal first test.)
• Target the right population. One factor that certainly impacts the effectiveness of screening is the population you're targeting. Our studies found, for example, that the proportion of abnormal results using FDT was much higher when screening in an elderly population.5So, it makes sense to target those groups with the highest risk of having disease and losing vision from glaucoma.
• Screen out in the community, not in your office. If you want to screen hundreds or thousands of people, you have to go out into the community, as several studies have demonstrated.1,6,7 Most people don't want to come to a clinic. However, they're generally willing to do a screening if it's taking place where they happen to be, whether that's a health fair, next to a rock concert or in their senior center. (Besides, if someone is already in your clinic, you might as well do a full eye exam.)
Another advantage to screening out in the community is that those you screen will often return with other friends or family members. That almost never happens if the others have to make the trip to your clinic. In any case, it's usually health-care workers who come to in-clinic screenings, not people from outside.
• Consider using a questionnaire. Many organizations use questionnaires to identify people who are at higher risk of glaucoma. The questionnaire can include questions about family history, age and ethnicity. Have you had trauma? Do you use steroids? Do you have diabetes? Are you over the age of 60? Have you had an eye exam in the past two years? These are all known risk factors for glaucoma. A certain score would indicate a higher risk for developing glaucoma. At the end, you can put an invitation for people to come to a free screening in their neighborhood. Such a survey could be published in the local newspaper, sent out via a mass mailing, handed out at a health fair or posted on the Internet.
Of course, this isn't an accurate way to determine someone's risk of glaucoma, but that's not necessarily the point. Such a questionnaire educates people about the risk factors for glaucoma, and alerts them to investigate further if they have risk factors. It's a simple but effective way to educate the community.
So: Should We Be Screening?
There's no question that screening helps identify people who are at risk for glaucoma, which is extremely valuable; at the least, it gets them into the health-care system; at best, it helps to prevent vision loss and blindness. FDT helps, because it actually does identify people with vision loss in a fairly efficient fashion, and if you find someone with vision loss, you've served him pretty well. Beyond that, the big advantage of screening out in the community is educating people about glaucoma, which we know benefits the community.
So: is it reasonable to recommend it on a large scale at this point? As the AHRQ has noted, we don't have sufficient evidence that glaucoma screening is worthwhile, at least relative to its costs. And, as noted, there are potential downsides to screening, although we believe those only impact a small minority of those screened. For the vast majority, appropriate screening and counseling about the results is beneficial.
In any case, plenty of ophthalmologists are out there doing screening. And there's value to it that's difficult to measure—such as educating the community about glaucoma and introducing people into the health-care system. Other side benefits may also be taking place, such as individuals getting their blood pressure checked at the same time. These are all things that wouldn't fall under the umbrella of AHRQ recommendations, but they are valuable. So if you want to help your community and you have the resources, screening may be a good way to do so.
1. Mansberger SL,
2. Cioffi GA, Mansberger S, Spry P, Johnson C, Van Buskirk EM. Frequency doubling perimetry and the detection of eye disease in the community. Trans Am Ophthalmol Soc. 2000;98:195-9
3. Mansberger SL, Edmunds B, Johnson CA, Kent KJ, Cioffi GA. Community visual field screening: prevalence of follow-up and factors associated with follow-up of participants with abnormal frequency doubling perimetry technology results. Ophthalmic Epidemiol 2007;14:3:134-40.
4. Quigley HA, Park CK, Tracey PA, Pollack IP. Community screening for eye disease by laypersons: the Hoffberger program. Am J Ophthalmol 2002;133:3:386-92.
5. Mansberger SL, Johnson CA, Cioffi GA, et al. Predictive value of frequency doubling technology perimetry for detecting glaucoma in a developing country. J Glaucoma 2005;14:128–134.
6. Ellish NJ, Higginbotham EJ. Differences between screening sites in a glaucoma screening program. Ophthalmic Epidemiol 2002;9:225–237.
7. Levi L, Schwartz B. Glaucoma screening in the health care setting. Surv Ophthalmol 1983;28:164–174.