The number of treatments in the U.S. Food and Drug Administration pipeline for dry-eye disease is staggering. Each novel pharmaceutical is going through different phases of clinical trials all with the same goals: Effectiveness and market approval.
“I think that the realities of cost and regulatory approval and the complexity of trying to meet both clinical sign and symptom endpoints for these is hard,” says Rebecca Petris, the president of the Dry Eye Foundation and a dry-eye disease patient. “But the market is continually growing, so it’s clearly a very attractive area for the industry.”
This article will review several dry-eye disease treatments undergoing Phase III trials along with treatments nearing market availability.
Never Giving Up
Aldeyra submitted its New Drug Application for its drug Reproxalap in 2023. The FDA responded with some discrepancies over the clinical trials. According to the company, the FDA stated that the NDA didn’t demonstrate efficacy in treating ocular symptoms associated with dry eye and that the pharmaceutical company would need to conduct at least one additional efficacy trial to receive market approval.
“[Aldeyra] came to an agreement with the FDA about a new mini trial with a really interesting structure,” says Ms. Petris. “Once they’ve presented that with their resubmission, then it’s expected to be another six-month review period from the FDA. So, it’s definitely not dead. They’re heading into their next phase of it.”
In April, researchers for Aldeyra presented the results for a pivotal dry-eye disease chamber crossover trial at ASCRS 2024.1 The researchers tested the efficacy of 0.25% Reproxalap ophthalmic solution compared to a vehicle in dry-eye patients. A total of 63 patients were selected for the trial, receiving four doses of Reproxalap or the vehicle daily for about one to two weeks. Researchers observed the primary endpoint of ocular redness during the chamber and Schirmer test 10 minutes after the fourth dose.
According to the report, Reproxalap demonstrated statistically significant diminished ocular redness and increased Schirmer score by ≥10mm in subjects. Compared to the vehicle, Reproxalap statistically significantly lowered symptoms assessed in the chamber following treatment. Patients treated with Reproxalap experienced mild adverse events, the most common being mild, transient irritation upon instillation, which lasted approximately one minute for each individual.
In a company statement, Aldeyra states that the FDA didn’t have issues with safety or manufacturing. The company says that data from their Phase IIb clinical trial proved that Reproxalap effectively reduced patients’ symptoms leading to ocular surface improvement. They say that drug improved symptoms such as ocular discomfort, dryness, grittiness, stinging and burning, as well as provided better osmolarity and Schirmer test scores compared to vehicle.
 |
|
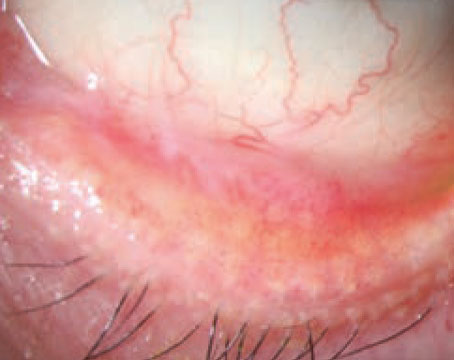
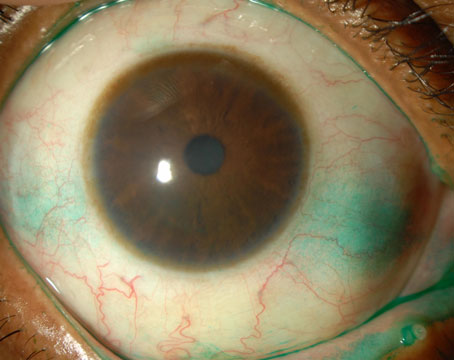
Lacrifill is a one-time disposable prefilled syringe containing sterile hyaluronic-acid gel. It can be administered in the canaliculi in both eyes if needed. The most common adverse event presented in the original Lacrifill study (n=63) was epiphora (7.8 percent). |
On the Cusp of Release
Nordic Pharma’s Lacrifill has 510(k) approval but isn’t yet available. Nordic says it’s set to release the treatment in the coming months. Lacrifill is a canalicular gel dermal filler used to block tear drainage that has been given labeling from the FDA to stay resident in the eye for up to six months before irrigating and readministering the treatment.
“The reason for that is that when we did the study, the FDA wanted us to do a much longer study,” says Mark Packer, MD, the founder of Packer Research Associates and former chief medical officer for Visant Medical, the pharmaceutical company originally developing Lacrifill before Nordic acquired the product. “We wanted to do six months. We thought that would be sufficient. They wanted us to do longer. We weren’t really sure at the time how long the stuff would last. We were pretty confident at about three months based on prior clinical work we had done but we didn’t know beyond that.
“In the negotiation with the FDA, they said, ‘Fine, you can do it for six months, but at six months you’ve got to wash it out. You’ve got to remove it from everybody. We don’t want people out there with this investigational gel in their canaliculus,’ ” continues Dr. Packer. “So, at six months you’ve got to wash it out. That was kind of the negotiation, so that’s what we did and that’s why it’s temporary. But it absolutely lasts six months. There’s no question about that.
“Basically, [Visant was] a small startup company,” Dr. Packer explains. “We wanted to move forward. We didn’t want to be studying for a whole year or two, which the FDA would’ve been happy with. So, we do have plans around that because we don’t even know how long it would last if you didn’t wash it out in six months. I think it might be a year, but I don’t really have any basis for that. It’s just a gut feeling. So, that’s a really interesting study and that’s definitely a part of the plan.”
When it was originally developed, the clinical research for Lacrifill only supported up to three months with speculation for use up to six months. John P. Fezza, MD, a facial cosmetic surgeon who developed Lacrifill and owns the patent behind it, first proposed the idea of using cross-linked hyaluronic acid gel to treat dry eyes.2 In his published research, he explained how the gel can be placed in the lower canaliculus, which would block tear drainage similar to punctal plugs.
Although the final follow-up period for Dr. Fezza’s study was set at six months after treatment, he focused on observing the three-month follow-up period to assess the safety and efficacy of the gel. A total of 63 patients completed the study, all of which demonstrated an improvement in corneal fluorescein staining. Dr. Fezza noted that Schirmer’s tests demonstrated an average increase over baseline of 3.67 mm after three months of treatment. Both breakup time and tear meniscus height at baseline over the three-month period increased (87 percent and 57 percent, respectively).
At the time of writing this article, the latest data for six-month follow-up hasn’t been published, but Dr. Packer notes that this information will be made public in the coming months.
Dr. Packer mentions that the procedure is very easy to perform. “It’s like doing a lacrimal irrigation, which I think was probably the first procedure I ever learned in residency to determine the patency of the lacrimal system,” he says. “So, it’s just like squirting some saline down through the punctum, through the canaliculus, and ultimately into the nose. You get a prefilled sterile syringe that has 0.6 mL [of solution], and that is enough if you needed to actually occlude all four canaliculi, but in the study that we did, it was just the inferior.”
 |
|
According to Global Market Insights, the dry-eye treatment market is expected to grow from $6 billion in 2022 to $12.3 billion in 2032. |
Further Analysis
 |
| Slit lamp images of a cornea undergoing treatment with RGN-259. (A) Image of a prominent epithelial defect at onset of treatment. (B) Image of healed epithelial defect 31 days after treatment. Photo: RegeneRx. |
RegeneRx Biopharmaceuticals is awaiting market approval for its moderate-to-severe dry eye treatment, RGN-259 (also indicated for neurotrophic keratitis). RGN-259 is an eye-drop solution containing the regenerative protein thymosin ß4.
In a company statement from 2021, the ARISE-3 Phase III clinical trial has been completed. Although the drug didn’t meet the primary endpoint, it did meet the secondary endpoint of improvement of ocular grittiness. This improvement was statistically significant and was observed at one and two weeks after treatment, the company says. No serious adverse events were reported, although mild-to-moderate events were analyzed in both the RGN-259 group and placebo group. The most common adverse event was mild pain upon instillation, which was reported in 6.6 percent of RGN-259 patients and 4.6 percent of placebo recipients.
According to a post-hoc analysis by GtreeBNT using the exact cohort from the Phase III trial, patients showed significant improvement in fluorescein staining scores after two weeks of treatment.
“While the trial didn’t meet its primary outcome measures, there was a statistically significant symptom effect in favor of RGN-259 in a short period of time in addition to its safety,” stated J.J. Finkelstein, the RegeneRx president and chief executive, in the official statement. “Statistically significant clinical improvements in various signs and symptoms of dry-eye syndrome have now been observed in all three Phase III clinical trials, ARISE-1 -2 and -3, and further analyses are ongoing.”
Both RegeneRx and GtreeBNT will continue their efforts towards achieving market approval and are exploring the possibility of a pre-Biologics License Application with the FDA using the results from the three ARISE clinical trials.
 |
|
Click table to enlarge. |
Smooth Sailing (So Far)
Alcon acquired AR-15512, a topical transient receptor potential melastatin 8 (TRPM8) agonist, after the acquisition of Aerie Pharmaceuticals in 2022. In January of this year, Alcon announced that its Phase III COMET trials for AR-15512 had achieved positive topline results. “I saw on their results announced in January that they were talking about a 10-mm increase in the Schirmer’s score,” points out Ms. Petris.
According to Alcon, subjects from the COMET-2 and COMET-3 trials met the primary endpoint of the proportion of subjects with at least a 10-mm increase in Schirmer’s score at day 14 of the trials, which was statistically significant. Additionally, data from the secondary endpoints in the trials demonstrated the rapid onset and sustained tear production associated with AR-15512 compared to the vehicle. Some patients met this secondary endpoint at day one, while others were persistent up until day 90 of the trials. No serious ocular events were reported.
Moving Forward
A Phase III clinical trial for ST-100, Stuart Therapeutics’ vezocolmitide drug candidate, has begun, with an enrollment of 320 subjects in a randomized, placebo-controlled trial aiming to evaluate the safety and efficacy of the drug. According to Stuart Therapeutics, this novel treatment is based on the company’s PolyCol technology, a collagen mimetic platform, and used to restore disease-damaged collagen.
In 2022, Stuart Therapeutics announced the success of its Phase II clinical trial for ST-100. A total of 160 subjects were enrolled for the study, each receiving either 20 µg/mL ST-100, 50 µg/mL of ST-100 or a placebo twice daily. The primary endpoint observed, similar to previously mentioned trials, was a statistically significant difference between the percentage of patients achieving a ≥10 mm increase in Schirmer’s score at 28 days. Other points assessed were the ocular surface staining scores, which were statistically significant at treatment day seven, and overall ocular discomfort graded on the Ora Calibra Scale which the company says improved at treatment day 14.
Reviewing and Reassessing Trials
According to Palatin, the company is expected to meet with the FDA to discuss a regulatory approval path for their dry-eye treatment, PL9643, a melanocortin agonist. After not meeting its Phase III co-primary sign endpoint and secondary sign endpoints, Palatin is moving forward to the next stages of development.
“Our comprehensive data analysis is ongoing, and upon completion, we plan to meet with the FDA to discuss and get feedback on the design of the next pivotal Phase III clinical trial,” mentioned Carl Spana, PhD, the president and CEO of Palatin, in a company statement.
The company says that, in its Phase III MELODY-1 trial, the co-primary symptom endpoint was met as well as multiple secondary symptom endpoints. Symptom endpoints assessed pain while sign endpoints assessed conjunctival staining. As initially stated, the sign endpoints weren’t met, but PL9643 demonstrated a clinically meaningful visual analog score reduction of >10 points from baseline and other statistically significant results for the co-primary symptom endpoint.
After analyzing PL9643 for safety, the researchers indicated that the treatment was well-tolerated with fewer ocular adverse events in the PL9643 group (5.6 percent) compared to the vehicle (6.3 percent). Additionally, some subjects discontinued treatment during the trial, which resulted in a lower number of patients in the PL9643 group discontinuing treatment (7 percent) compared to the vehicle group (11.1 percent).
Another Treatment Indication
“If Dompé could get an indication for Sjogren’s for Oxervate [cenegermin-bkbj], that would be a real coup to have something specific for Sjogren’s,” comments Ms. Petris. “It’d be a coup for them. It would definitely be a coup for the Sjogren’s world.”
In 2022, Dompé announced it had enrolled the first patient in the Phase III trial for Oxervate with an indication for severe Sjogren’s dry eye. Now, the PROTEGO-1 PHASE III trial has completed enrollment and is actively undergoing investigation. The study will determine the safety and efficacy of cenegermin ophthalmic solution at 20 µg/mL versus a vehicle over four weeks.
According to Clinicaltrials.gov’s listing of Clinical Trial NGF0121, Oxervate will need to achieve the co-primary endpoint of >10 mm/5 min. in Schirmer’s tests along with a co-primary endpoint for change from baseline in SANDE global score. Secondary endpoints will assess a change from baseline in Schirmer’s test, change from baseline in cornea and conjunctival vital staining with fluorescein, change from baseline in tear-film breakup time, change from baseline SANDE scores for severity and frequency, number of patients experiencing a worsening in SANDE scores as well as an Impact of Dry Eye in Everyday Life questionnaire.
In conclusion, dry-eye treatments will continue to develop, especially since there’s no perfect solution to mitigate the disease’s symptoms. Both Dr. Packer and Ms. Petris agree that physicians need to work with their patients to help them better understand their symptoms and explain that there will be more options as treatments are approved.
“I think in the mass for the patient world, knowing how much is in the pipeline is very important, because when you have a disease that has so much impact on someone’s daily life, and often gets labeled with terms like ‘chronic’ and ‘progressive,’ people struggle with hope,” says Ms. Petris. “They struggle to find hope that things can get better. And the pipeline is that promise that there’s hope that there are things being worked on.”
Dr. Packer has previously worked on Lacrifill with the original developer of the drug, Visant Medical. Ms. Petris has no financial interests to disclose.
1. Garg, S. Reproxalap improves ocular redness, tear production, symptoms in a pivotal dry eye disease chamber crossover trial. https://ascrs.confex.com/ascrs/24am/meetingapp.cgi/Paper/98564. Accessed on April 17, 2024.
2. Fezza, JP. Cross-linked hyaluronic acid gel occlusive device for the treatment of dry eye syndrome. Clinical Ophthalmology 2018;12;2277-2283.