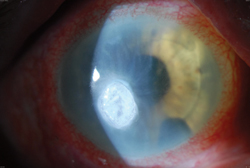
• Cyanoacrylate. Though not officially approved for use on the eye, cyanoacrylate has been used by ophthalmologists for more than 30 years. “The main indication for cyanoacrylate is the management of perforated corneal ulcers, both sterile and infectious,” says Christopher Rapuano, MD, director of the cornea service at Philadelphia’s Wills Eye Institute. “It works well for that indication. We also use it for ulcers where the cornea is very thin and might perforate in the next couple of days or weeks; we just fill it with glue and let it heal before it perforates. Since it’s not FDA-approved, I have patients sign a consent form that states what we’re doing and that it’s not FDA-approved but it’s a standard treatment.”
Dr. Rapuano says that, when working with cyanoacrylate, controlling moisture in the area of operation is key. “Cyanoacrylate polymerizes as soon as it touches something like water, aqueous or saline,” he explains. “So, if you have a perforation and aqueous is coming out, as soon as cyanoacrylate hits the aqueous it will solidify. This is good and bad. In the presence of moisture, it’s good in that it will solidify pretty instantly. But if you have a dry divot and put down the glue, it will remain as a liquid for several minutes until the moisture around the glue polymerizes it. The danger is that, if it hasn’t polymerized and you touch it with something like a Weck-Cel, it will start to polymerize as you’re touching it, and you’ll get this wick that comes off the glue. So, you have to be really patient and not touch any wet glue with either an instrument or a Weck-Cel. So, when I’m 95-percent sure it’s polymerized, I’ll flood it with saline or proparacaine so I’m sure it’s polymerized. Also, you don’t want to put a contact lens on it when it’s in its liquid state because I’ve seen glue adhere to soft contact lenses. However, you almost always have to cover the polymerized cyanoacrylate with a soft contact lens because the surface is very rough and you don’t want to cause the patient discomfort or have the lids poke at it with each blink and risk dislodging it.”
Dr. Rapuano says it works very well for sterile perforations, but in infections it can be more challenging. “In infected perforations, the tissue tends to be mushier and the cyanoacrylate doesn’t stick that well,” he says. “Sometimes for sterile perforations it stays on for many months. In those cases you just have to keep changing the contact lens and following the patients. Once the cornea heals, the glue will pop off.”
• Fibrin glue. This is a biologically derived tissue sealant (as opposed to the synthetic cyanoacrylate) that’s indicated for use in controlling bleeding. Like cyanoacrylate, even though it’s not specifically approved for ophthalmic surgeries, ophthalmologists have found several uses for it. “Fibrin glues such as Evicel, Tisseel and Artiss are used to secure tissue to the surface of the eye,” says Dr. Rapuano. “Specifically, this takes the form of securing conjunctival tissue during pterygium surgery with conjunctival auto-grafts, and securing amniotic membrane tissue in pterygium surgery or another surgery where amniotic membrane is used to cover some abnormality or conjunctival defect.”
An interesting evolving technique using fibrin glue was developed by Chennai, India, surgeon Amar Agarwal. In complicated cases in which an intraocular lens can’t be fixated normally, Dr. Agarwal has built upon ideas first proposed by German surgeon Gábor Scharioth, MD, PhD. In Dr. Agarwal’s glued-haptic technique, the surgeon first creates two partial-thickness, limbal-based scleral flaps 180 degrees apart. Then, the surgeon performs an anterior vitrectomy. With the help of an assistant, the surgeon externalizes the haptics through the sclerotomies, then tucks the ends of the haptics into a Scharioth intralamellar tunnel he creates with a 26-ga. needle at the location of the externalization. The surgeon then closes the scleral flaps over the externalized haptics with fibrin glue.1
|
• ReSure sealant. ReSure is made of a polyethylene glycol hydrogel, which is a different material from cyanoacrylate or fibrin glue, and is approved for the sealing of clear corneal incisions used in cataract removal/IOL implantation. It actually comes as two separate materials, a polyethylene glycol solution and a trilysine amine solution, which, when mixed together by the user, form the sealant. An applicator that comes in the ReSure kit is used to apply the mixture to the eye.
Fairfield, Conn., surgeon Robert Noecker has used ReSure for both on- and off-label uses, and has gotten to know its idiosyncrasies. “This is a sealant, and is a derivative of the product DuraSeal, which is used by neuro-surgeons to seal the dura during cerebrospinal leaks,” he says. “The key difference between a sealant and a glue is that the former is meant to go into a crevice and seal it, and it doesn’t necessarily hold tissue together. Once the sealant is set in place, it takes on this rubber consistency and is very durable. It will stick around for at least a few days, and its advantage is it minimizes the use of sutures.
“I’ve used it for clear corneal wounds, and for instances in which I’ve removed a glaucoma tube shunt or there’s a scleral defect and I wanted to seal the area,” Dr. Noecker adds. “If you want to create a situation on the sclera where there’s no flow or you want to seal up a hole you no longer need, it can be very useful. However, if the situation has a vigorous flow rate, it probably won’t work that well. But, if you can get the area temporarily dry, it will seal scleral defects.” Dr. Noecker says he’ll often use it to seal wounds in cases where he’s corrected astigmatism with a toric lens or incisions.
Dr. Noecker says working with ReSure has taught him some things. “The key is to be prepared to act quickly,” he says. “You have about a five-second working time. This is important to note because when most people work with it, they’re a little slow their first time. The sealant comes in a tray with a blue solution and a more particulate white component that you mix together. There will be a temptation to get all the white dissolved before you apply the sealant. The truth is, however, if you take all that time to get it dissolved, your window for working with it has closed. Be quick.
“Another thing I’d recommend doing is mix it under the operating microscope right next to the incision you want to seal,” Dr. Noecker continues. “This way, when it’s ready, the distance you have to move it is only a centimeter. Also, I’d tell surgeons to make sure the eye is dry. If there’s an active leak or the surface is too wet, ReSure will tend to stick to itself rather than to the tissue you want to seal. The other thing is that it’s best to get the application surface of the eye oriented in a horizontal plane, which may mean turning the patient’s head a bit just so the sealant doesn’t tend to flow away from where you’re applying it. Since this will most likely be a temporal clear corneal incision you’re sealing, you’ll want the head oriented a little horizontally, or the patient looking a little toward his nose. It only takes a few seconds to set it in place, but you don’t want it to run away from the incision.”
Since ReSure costs somewhat more than a suture, Dr. Noecker says it’s not something a surgeon will use in everyone. “It’s more expensive than a suture, so you have to take that into account,” he says. “As a skilled surgeon, will I use it on every case? No. But I will use it on premium cases such as femtosecond cataract. Fortunately, the risk of problems is low for cataract surgery, but there are cases in which I want to drive that chance of a problem down even lower by using the sealant in a particular patient.” REVIEW
1. Agarwal A, Jacob S, Kumar DA, Narasimhan S. Handshake technique for glued intrascleral haptic fixation of a posterior chamber intraocular lens. J Cataract Refract Surg. 2013;39:3:317-22.