Since their approval by the FDA, the Apthera IOL (Bausch + Lomb) and the EVO+ ICL (Staar Surgical) have given surgeons new options for enhancing patients’ vision. Their designs have the potential to fill a niche for patients who might otherwise be challenging to please or have characteristics that disqualify them from alternatives. Surgeons who have been working with these lenses since the clinical trials say they’re useful assets in their armamentarium, so we asked them to share the lessons they’ve learned and techniques they’ve honed. Here’s what they had to say.
Apthera IOL
Initially brought to market by AcuFocus before being acquired by Bausch + Lomb, the Apthera (originally called the IC-8) is a non-toric extended-depth-of-focus IOL for patients with up to 1.5 D of astigmatism. Meant to be implanted in the non-dominant eye, the Apthera uses small-aperture technology and is available in +10 D through +30 D in 0.5-D increments.
 |
| TECLens’ partnership with SERVImed will allow for the incorporation of Ribocross with CXLens treatment. The riboflavin solution is maintained in a scleral lens reservoir. (Courtesy Bausch + Lomb) |
John Hovanesian, MD, a cornea, cataract and refractive surgeon at Harvard Eye Associates in Laguna Hills, California, took part in the FDA clinical trials for the Apthera. “I’ve been using it for approximately three years now, and I had a chance to use it even prior to that in El Salvador to experience it and see patients with it,” he says. “It’s a very unique lens that serves an important purpose that no other tool can fill. While it may not be for every patient, it’s certainly for every surgeon. It’s important enough, it’s unique enough that everybody should know about how and where it works.”
• On- and off-label candidates. Patients had to meet strict criteria to be included in the FDA study, which was designed for monovision in normal eyes. Another surgeon who was involved in the study, William F. Wiley, MD, medical director of the Cleveland Eye Clinic, says that not only did patients have success with the Apthera, but it was technically easier to implant than previous small-aperture options.
“Our practice was familiar with small-aperture optics, including the Kamra corneal inlay, which we found did well optically, but there were some technical challenges with it surgically,” Dr. Wiley says. “It was hard to get it perfectly aligned or centered, and there were some biocompatibility issues with it being in the cornea. When we had the opportunity to have the same aperture optics, but now putting it into an IOL, it made it technically much easier as well as helped with biocompatibility. Now there aren’t any issues because it’s encapsulated within the intraocular lens.”
Patients who are already familiar with monovision in their contact lenses are great candidates for the Apthera, Dr. Wiley continues. “Studies show that, for monovision patients, it’s a great alternative. Patients who’ve had a lot of success with contact lens monovision were used to having some accommodation where, when they wore contacts, their natural lens had some accommodation, and if the eye was targeted for -1, they’d still have natural accommodation that would give the full range of vision with contacts,” he says. “But once you go to pseudophakic monovision, monofocal IOLs are so rigid as far as their depth of focus, that patients didn’t really adapt as well. They always say they love monovision in their contacts, but they don’t like it with the IOL. With the small-aperture, it gives true depth of focus, more similar to what patients might have experienced with their contact lenses where you target maybe a -1, but now that aperture can bring in that -1 for better near vision while maintaining some of the distance vision as well. So it tends to be more analogous to what they’d seen with a contact.”
 |
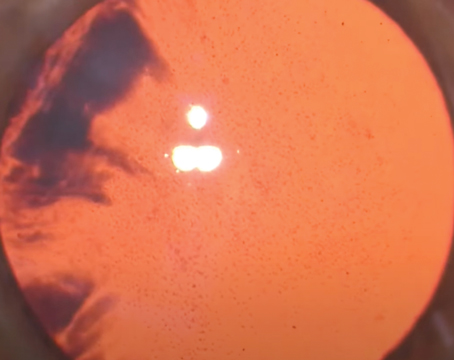
| Surgeons say they commonly use the Apthera IOL off-label in patients with keratoconus or previous radial keratotomy. (Courtesy Uday Devgan, MD) |
It’s this distance vision ‘x-factor’ that surgeons say sets the Apthera apart. “With monofocal IOLs set for monovision you have to subliminally ignore (but sometimes consciously) the eye that’s out of focus and use one eye for distance and the other for near,” says John Vukich, MD, the founder and medical director of Summit Eye Care in Wisconsin, and a principal investigator in the clinical trials for Apthera. “You lose depth perception and binocularity with monovision. With Apthera, you maintain binocularity at distance. You don’t have to alternatingly suppress one eye vs. the other. You maintain binocular summation or quality of vision, meaning that two eyes together in focus are better than one eye only.
“When I discuss this with patients I describe it as blended vision,” he continues. “We don’t call it monovision because that’s not really accurate. There are many patients for whom they may have tried monovision with contact lenses and rejected it because it wasn’t comfortable or they just couldn’t habituate to it. Those patients do extremely well with the Apthera because they’re not losing the binocularity. It’s a great solution that patients do very well with.”
However, now that the Apthera has been in clinical use for nearly two years, its usefulness beyond “normal eyes” is becoming apparent.
“The second personality of Apthera, if you will, is for the irregular eye,” says Dr. Hovanesian. “This is really where most of these lenses get used, certainly in my practice. These are patients with keratoconus or radial keratotomy and highly irregular surfaces where there’s not just an issue with cataract, but an issue with irregularity that you can’t correct with anything but maybe a scleral or RGP lens. Here, we have a lens implant that can provide not only an improvement in uncorrected acuity but an improvement in best-corrected acuity because it gives them small-aperture optics.”
Dr. Wiley echoes this experience. “Beyond what the FDA indications were, we also find that aperture optics can give a great solution for more unique situations,” he says. “In particular, when someone’s had radial keratotomy or has keratoconus, we can prove in the lane that they see better through a pinhole device and now we can offer that through small-aperture optics with an IOL. We’ve also found this niche application with irregular astigmatism that takes people who just weren’t seeing well with typical correction now have the ability to have some of that best-corrected vision improved and we’ve been excited about that.”
The pinhole mitigates some of the inherent aberrations or irregularities in the visual system experienced by those with RK, says Dr. Vukich. “One of the things that’s really quite helpful is that many patients who’ve had RK have fluctuations in vision,” he says. “They may have a different prescription in the morning than they do at night—there could be a 1.5 D of change over the day. With the Apthera, if we just set it for that endpoint, the depth of focus mitigates that fluctuation because the depth of focus eliminates that perception of quality change or perception of refractive correction.
Another off-label use for Apthera is bilateral implantation. “I’ve used it bilaterally, although it’s indicated for unilateral use,” notes Dr. Hovanesian. “The way I approach it is: when you have a patient with bilateral keratoconus, they want to be better in both eyes, so I’ll implant Apthera in the more irregular eye first. Afterwards, I’ll ask them to judge how much dimming they noticed and if they’d tolerate a similar amount in the other eye. If they feel positive about that, then I’ll implant it in the other eye. I’ve done that a number of times now and so have other surgeons with good results because the gain in acuity offsets whatever dimming they experience. Apthera certainly can be used bilaterally.”
• Preop considerations and targeting. “You’ll conduct the routine cataract/IOL preop testing, but you do have to be more mindful of certain things that wouldn’t make them a good candidate, such as anything that may interfere with the optical pathway, including a central corneal scar, prominent vitreous floaters, any kind of macular pathology—anything on that central visual axis,” Dr. Wiley says.
“We do show patients pinhole optics with a pinhole occluder in the lane,” he continues. “It’s interesting, when the occluder drops in, they’ll say, ‘I’m seeing distance and some near vision. This is great.’ Those are patients where you might be more encouraged to use it, but some patients say, ‘Wait a minute, it’s much more dim, you’ve turned the lights down. I don’t like this.’ We do counsel patients that this lens is going to allow less light in, but the light that does get into the eye will be more clear. There’s a tradeoff and some patients appreciate that or some patients don’t, so it’s a good idea to show them what it’s like when in the lane and rule out anybody that might have an issue with it after surgery.”
Make sure to check how the patient dilates, advises Dr. Hovanesian. “You want to be able to dilate the pupil to look at the retina in the future,” he says. “Make sure that you’ve got a patient who dilates to 6 mm or more because the outside diameter of the mask is about 3.5 mm and if they only dilate to a 4 mm pupil, it’s going to be pretty hard to ever look at the retina.”
Preop OCT is proving to be a helpful technology, he continues. “Any of these lenses depends upon a healthy macula,” says Dr. Hovanesian. “With any of the advanced lenses, there’s some forgiveness of very mild maculopathy, but we do an OCT on everybody because it’s surprising the number of patients who have epiretinal membranes that aren’t visible by slit lamp, especially when you’re looking through a cataract. We think OCT is important for challenging patients or patients who are choosing a refractive lens.”
When it comes to targeting the Apthera, Dr. Wiley advises to lean toward an intermediate vision. “When we do a pinhole aperture in the lane, somebody could be at -1 but when you drop the pinhole in they now have better distance vision,” he says. “With small-aperture optics, the defocus curves work on both sides of that resting refraction so it can help give a -1 vision better distance, but also better near vision. So if you start at plano you’re losing some of the depth of focus on the back side of that defocus curve. But if you target -1 or -1.25, you’re maximizing the near vision and also gaining a little bit of distance vision on top of that -1 refraction.”
This might differ for those with keratoconus. “There’s been some discussion that because someone with keratoconus has a multifocal cornea, they can look through multiple points in that cornea,” Dr. Wiley says. “We’ve noticed that the Apthera forces them to look through a very central part of their visual axis and sometimes that portion of the cornea may be flatter than where they’re used to. That might suggest we have to target even more minus than we think. They’re losing some myopia based on where they’re forced to look.”
For the diurnal fluctuations in patients with RK, Dr. Hovanesian says it’s good to aim somewhere in the middle of the refractive range they experience. “If the cornea varies between a 42 and a 44, then you might aim for treating it as though the keratometry is 43 and they’ll end up with better acuity throughout the day,” he says. “Or aim for the flatter of the two options. Aim for the 42 and then during the part of the day when their cornea ends up being steeper, they’ll end up with better uncorrected near vision.”
• Implantation techniques. “One unique thing about implantation of the Apthera is that it requires a 3.2-mm incision, which is a little larger than most of our lenses that go through a 2.4-mm or even a 2.2-mm incision instead, so that requires an extra step,” says Dr. Hovanesian.
Dr. Wiley says to make sure that the lens is well-centered. “It’s a stiffer lens so it’s going to center itself within the bag, but if you had any kind of pathology that might allow it to decenter, that could pose an issue. You want to make sure the bag itself is normal,” he says.
As mentioned earlier, the patient’s ability to dilate is important. The Apthera is contraindicated for patients with a dilated pupil size less than 7 mm. “They don’t want you implanting it in a small pupil because if you have to do a YAG laser you might not be able to go around the Apthera,” notes Dr. Wiley. “There are mandatory online courses that surgeons have to do to make sure they understand how to do that technical component of the YAG laser.”
“Just like any implant, patients can develop posterior capsular opacity,” warns Dr. Hovanesian. “It’s important that we YAG these the right way. What we don’t want to do is YAG through the mask, because you’ll cause damage to the lens and it will absorb the YAG energy and cause delamination of the lens. Damage to the mask seems to be generally well-tolerated, just like pitting of the optic when the YAG laser hits the posterior surface of any lens, but nonetheless it’s damage we hope to avoid. When you’re doing a YAG you often need to dilate the pupil somewhat widely and you YAG in an inverted U pattern so that you create a flap of the posterior capsule and it will tend to fall backward and remain attached at the bottom 6 o’clock position. Sometimes it’s necessary to YAG through the aperture in the middle of the lens, but do that cautiously.”
• Refractive misses. Surgeons who are experienced with the Apthera say that refractive misses are uncommon, but there are options if it happens.
“I suppose it’s more forgiving, in particular on astigmatism,” says Dr. Wiley. “It can correct up to 1.5 D of astigmatism just by the aperture effect. If you have a patient you’re not sure exactly where the visual axis is, the Apthera can be a little more forgiving as far as correcting some of the astigmatism, but can be more forgiving on a refractive miss. The FDA study did indicate that. However, the only downside is some of the eyes we’re doing it on now are more challenging to hit the target.”
Dr. Hovanesian says he favors surface ablation for refractive misses with IOLs. “However, our accuracy goes down for patients who’ve had prior kerato-refractive surgery because we know that epithelial remodeling in the cornea can have unexpected results,” he says. “So, I sort of lean toward PRK, but with caution. We don’t have a ton of those with Apthera because the lens is forgiving and because, frankly, going into this, we set the expectation with patients who have irregular corneas. We’re not really doing this as a refractive procedure—we’re doing it to improve their acuity, we’re doing it to try to avoid a corneal transplant, to avoid a scleral contact lens in the future. But the lens is limited. Technology isn’t perfect. They have to temper their anticipated results.”
“It’s a great lens, but like any of the presbyopic lenses there are pluses and minuses to using it,” Dr. Wiley summarizes. “Some patients might notice glare or halo with nighttime activities, which seems to be on par with what we’ve seen with other presbyopic lenses.” In the FDA study,1 the most common visual disturbances at 12 months in the Apthera group with severe ratings were starbursts (3.6 percent), halos (3.6 percent) and glare (3 percent). Of all visual symptoms, including blurred and hazy vision, over 80 percent of subjects reported ‘never experienced’, ‘experienced symptom but not bothered at all’ or ‘a little bothered’ at 12 months in both the Apthera IOL and control groups, according to the study.
 |
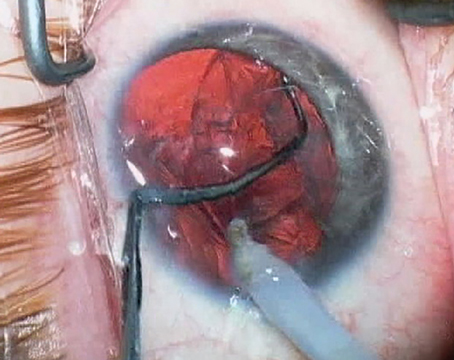
| One of the surgical pearls for implanting the EVO ICL, offered by Deepinder Dhaliwal, MD, is to create the first paracentesis at an angle toward where the footplates will be tucked, which makes the surgery go more smoothly. (Courtesy Deepinder Dhaliwal, MD) |
EVO+ ICL
The second generation of the Visian implantable collamer lens, the EVO/EVO+ Visian ICL was FDA approved in 2022. The phakic lens is approved for high myopes ranging from -3 to -20 D, with the ability to correct from 1 to 4 D of astigmatism.
“EVO is intended for the treatment of myopia and myopic astigmatism, specifically for patients who are looking for a refractive outcome and don’t have cataracts,” says Dr. Vukich. “It’s absolutely an improvement in the ICL line. EVO simplifies the treatment since they don’t need laser iridotomies, and it makes the surgery easier for the patient. The EVO ICL tends to be even more forgiving regarding the postoperative amount of vault. This is reassuring from a surgeon standpoint.”
ICL technology is well-known, and advancements are bringing it to the level of LASIK correction, speculates Dr. Vukich. “It’s been around for more than 20 years and it continues to gain market share,” he says. “It’s a very popular option in Asia where there’s a higher prevalence of myopia. But within the United States now, we see a progressive increase in using the EVO in what would be considered to be the LASIK range. The EVO goes down to -3 D, the lowest power available, and we’re seeing an increased uptake in the -3 to -6 D diopter range, which used to be the exclusive territory of LASIK. The continued increase in uptake for the ICL has obvious reasons: it’s removable, the quality of the optics is very high, and it provides stable rehabilitation.”
In the past, Dr. Wiley says he typically only used the ICL for extreme cases, but now trusts it in more routine refractive cases as an alternative to LASIK, SMILE or PRK. “In particular, we’ve made an effort in our practice to try to minimize offering PRK,” he says. “We offered PRK for thinner corneas, dry-eye patients or patients who were worried about operating on a problematic corneal surface. Granted, PRK has those safety profiles that would make it safer than LASIK as far as ectasia or dryness, but we also found that it’s just not a practice-builder. It takes a few weeks to get the best vision. Patients don’t have that immediate wow effect, so it’s sort of an anticlimactic experience to say the least for the patients. Now, any patient that we may have offered PRK we try to encourage the ICL, which has the same or even better wow effect that we see with LASIK or SMILE.”
Dr. Wiley continues, “We used to have a -9 or -10 cut off for ICL and we’d do LASIK or SMILE all the way up to those ranges, but now we’ve dropped our threshold and are trying to offer ICL as mandatory above a -6.50 or so. As much as you can do LASIK on a -6.50 or -7 patient, they do well, but their enhancement rates are a little higher, they have a little higher chance of having glare, halo or abnormal side effects. With the ICL we just don’t see those. We’re trying to encourage the ICL more and more for anybody in the range of ICL approval, but mandatory in patients who were considering PRK or patients in the higher-to-moderate range of myopia.”
• Candidate selection. As with earlier iterations of the lens, anterior chamber depth is an important factor in patient selection.
“The number one reason why we wouldn’t use an ICL would be related to anterior chamber depth,” says Dr. Vukich. “The FDA requires 3 mm of true anterior chamber depth, from corneal endothelium to epithelium of the lens. The EVO lens does occupy space so you need an appropriate amount of it.
“We’d also avoid using this in anyone with a preexisting cataract,” he continues. “It’s proven to be a very safe lens. We implant this routinely in patients who have other conditions. For instance, if someone has elevated pressure/glaucoma, that isn’t a contraindication. It’s not a multifocal, so if someone is presbyopic, they’ll still need to have reading glasses as is the case with any refractive procedure.”
The EVO is ideal for patients with superior vision demands who also want to avoid corneal resurfacing. “I have a lot of engineer-type patients who are very particular about their vision,” says Deepinder Dhaliwal, MD, who is a professor of ophthalmology and the chief of refractive surgery at the University of Pittsburgh Medical Center. “They’re interested in very high-quality optics, and the EVO ICL can meet or exceed their expectations because the cornea is untouched and because of that, the quality of vision is phenomenal.”
It can also be an option for patients hesitant to undergo LASIK for whatever reason. “When they realize that EVO is an additive technology, and we’re not removing corneal tissue or cutting across corneal nerves, it’s really kind of exciting to them, and comforting to them, too.” says Dr. Dhaliwal. “Don’t get me wrong, custom LASIK results are also phenomenal, but initially there’s dryness, and some glare and halo. The fact that it’s removeable is seen as a benefit by many patients.”
• Preop considerations. One of the advantages of the ICL is that it’s based purely on the refractive error, says Dr. Vukich.
“You don’t need to have an axial length, you don’t need to have a careful assessment of the topography,” he says. “We’re not looking at changing the shape of the cornea like you would a corneal refractive procedure. If you can refract the patient to a given level of acuity, you can then use that same refractive power on an ICL and fully expect to achieve the same level. We’ll get keratometry, we’ll get topographies and we’ll look at the surface of the cornea as it relates to dryness or surface quality because all of those things will influence the quality of vision, but the actual refraction itself is what drives the selection of power.”
Dr. Dhaliwal says it’s important to follow a system when performing any refractive surgery, including EVO. “Before the actual surgery, you have to pick the ICL and there’s nuances there,” she says. “The power is really easy. There’s an online calculator that you use, and there are four sizes. We’re using OCT with the Anterion device to get certain measurements and using the LASSO formula to help us, but also, just looking at white-to-white in different ways. The white-to-white value built into the calculator was from the Orbscan. If the white-to-white that you input isn’t from an Orbscan device, then you’re likely going to have to make a modification to the size of the lens. Sizing is not a scary thing. It’s totally doable, and Staar Surgical will help surgeons pick the appropriate size of the ICL if a surgeon has questions.”
Properly sizing the ICL is an integral part of the process, adds Dr. Wiley. “We've been a big fan of using multiple sizing methods, looking at IOLMaster, Pentacam and using a handheld digital caliper for manual white-to-white,” he says. “There’s some great software available, in particular, Roger Zaldivar, MD, has software called the ICL Guru that uses ultrasound measurements. It seems like that’s going to really be a more precise method for sizing.”
EVO’s central port has made it more flexible when it comes to the vault, as well. “It’s made it less concerning to have a smaller vault now that we know that we’re getting good aqueous flow around the lens,” says Dr. Wiley. “In the past, we might have been erring a little bit on a larger vault size or larger ICL size. But now, if there’s a toss up between the higher or lower vault lens, we’ll go with a lower vault lens knowing that the central port allows good aqueous flow. We just don’t have this concern as we did in the past for low vault sizing, such as cataract formation. Our European colleagues have informed us that the risk of cataracts with EVO is much lower than it was with traditional ICL so that’s made us all feel more comfortable with lower vaulting lenses. That’s given us a margin of error and safety that’s made it more forgiving.”
Implanting the EVO
“The lens is designed and sized to go from 3 to 9 o’clock; it always goes in the horizontal meridian,” Dr. Vukich says. “Unlike an IOL, which is rotated to the axis of the astigmatism you need to correct, the ICL always goes in at 3 to 9. Now, there can be a slight clockwise or counterclockwise bias that would go with the lens that you’d use to correct—you can’t have 180 different implant powers. It’s plus or minus 21 degrees clockwise or counterclockwise, but essentially it’s in the horizontal meridian.”
It requires a 2.8-mm incision, he continues. “The surgery itself is absolutely within the skill set of any trained anterior segment surgeon. It’s essentially a cataract incision without having to do the additional steps of removing a cataract once you’re inside, with the lens simply injected through the incision into the anterior chamber and then positioned posterior to the iris,” says Dr. Vukich.
“EVO is an easier procedure,” states Dr. Wiley. “It eliminates the YAG peripheral iridotomy and those workflow concerns that made that extra step more costly, time-consuming, and annoying for the patient and the team. It’s also much safer with the port.”
For the best results from the EVO, Dr. Dhaliwal offers the following pearls:
• Dilation. Make sure your patients are really well-dilated because it makes the surgery a lot easier.
• Paracentesis. “My first paracentesis is angled towards where the footplates are going to be tucked,” she says. “For example, if I’m operating on a right eye, then my first paracentesis is more at 5:30 and it’s angled nasally so that when I insert the Batlle ICL manipulator in the anterior chamber to tuck the footplate, it’s easy because I’m already in the same direction where I’m going to tuck the footplate. My instrument isn’t causing any corneal striae and it’s a little closer to those footplates so I don’t have to go all the way across the anterior chamber. This has been unbelievably helpful for me.
“After creating the first paracentesis, we instill Shugarcaine, followed by OcuCoat,” Dr. Dhaliwal continues. “Then we make our second paracentesis angled toward the main incision. We create our main incision and then gently insert and unfold the ICL (which has been loaded in the injector before the procedure is started). It’s elegant in its simplicity.”
• Leave room for the ICL to unfold. The anterior chamber should be about 70 percent full of OcuCoat so that there’s room for the ICL to unfold. Too much viscoelastic is a common mistake. Dr. Dhaliwal says she burps the incision to make sure that the anterior chamber has space for an easy unfolding of the ICL.
• Retract, depress and slide. During insertion, monitor that the leading right footplate has the orientation dot. “I’m very slow and methodical as I’m inserting the ICL to ensure the ICL is in the correct orientation,” she says. “Continue to depress the plunger until the ICL has fully unfolded. The orientation dots should be on the leading right and trailing left footplates. After that, we tuck the footplates. We place OcuCoat on top of the ICL after inserting to help it settle down closer to the iris. Then we use the Batlle manipulator to just tuck the footplates under the iris. We contact the ICL in the periphery at the footplate/optic junction and retract, depress and slide it underneath the iris.
“Another thing that’s helpful is to use the manipulator in between the footplates in the periphery of the ICL to rotate it to get the footplate closer to facilitate tucking,” continues Dr. Dhaliwal. “When I first started, I was scared to rotate the ICL. I would just try to get my manipulator to the footplate, wherever it was, but that was challenging because it could be an awkward position. Now I rotate the footplate closer to my manipulator, so it’s much easier. There’s a ‘no-fly zone’ in the optic—never touch the optic.”
• Be delicate. Be mindful that this is a phakic eye. “If you’re a very gentle cataract surgeon, you’ll be an excellent EVO ICL surgeon,” she says. “That’s the bottom line. If you have a gentle technique and you respect the anatomy and the structures, then you can do the EVO ICL very easily. If you’re a heavy-handed surgeon pushing on the eye, then you’ll need to modify your technique for EVO. It’s very different from a cataract lens implant where you don’t have to be as gentle. You have to switch gears.”
• Remove the viscoelastic. Dr. Dhaliwal says she uses a lot of irrigation when removing the OcuCoat. “I use BSS in a 5cc syringe with a hydrodissection cannula until I don’t see any more movement of the OcuCoat,” she says. “Then I use bimanual I/A. I do both. And because my paracenteses are a little bigger than for cataract surgery—closer to 1.5 mm—fluid can exit there. I want the viscoelastic to come out through all incisions.”
• No miochol at the end of the case. Dr. Dhaliwal says she doesn’t use miochol at the end of the case because she wants to keep the pupil dilated in case there’s a little residual viscoelastic behind the ICL. “I also don’t like to constrict the pupil in high myopes,” she explains. “There’s a risk of RD, and I don’t want my patients to have a headache. We want their experience to be as pleasant as it can be. I always check their intraocular pressure an hour or two after surgery before they leave.”
Postop Considerations
Once a patient has undergone EVO implantation, keep the following in mind:
• Side effects and recovery expectations. Patients can be fully corrected within hours after the procedure. “Unlike LASIK, in which there’s pretty significant re-contouring of the cornea that occurs, and unlike a cataract operation where there’s a fair amount of manipulation because of the amount of time the instrument is in the eye, the ICL is a small incision, but that incision is only used for the injection of the implant,” Dr. Vukich says. “There’s minimal edema and you don’t see swelling of the cornea because it’s a very gentle procedure. Usually by the next day we’ll see patients already at their best potential acuity.”
Glare was initially a worry for Dr. Dhaliwal. “I thought I’d have more patients complaining about the glare around the central port in the EVO ICL,” she says. “When I switched from the Visian, which doesn’t have a central opening in the optic, to the EVO ICL, which actually has five openings, I was a little worried patients would be affected by the glare after surgery. But after one month, patients typically say they don’t notice it anymore. There is quick neuroadaptation to the central port.
“The other beautiful thing is that we don’t have to do iridotomies anymore, so only one surgery is required,” continues Dr. Dhaliwal. “And the recovery is a little faster than my LASIK patients because there’s no corneal flap that has to heal. I’m not worried about DLK or dryness and the ICL is very biocompatible. Our patients use steroids for two weeks: four times a day for one week, and then twice a day for another week and that’s it. When I look at these eyes after surgery, they’re quiet.”
• Counseling patients as their vision changes. Patients who are receiving the EVO ICL are pre-presbyopic, and the day will come when their vision changes naturally due to age and/or cataract development.
Dr. Dhaliwal notes that EVO patients can be candidates for any IOL technology down the road that they want since their corneal optics are unchanged. “We know that moderate to high myopes will develop cataracts at an earlier age,” she says. “They’re happy to learn that having EVO ICL surgery won’t burn any bridges for future technology. Also, unlike post-corneal refractive surgery, there are no special formulae that need to be employed when selecting an IOL. Biometers can easily measure through the ICL.”
Dr. Vukich counsels patients that the EVO doesn’t stop the hands of time. “I tell my patients who are 20- or 21-years-old, ‘Look, you’re going to get gray hair and wrinkles someday, too.’ They laugh but the reality is, there’s a natural order and progression of changes and the EVO just sets the refractive error back to zero,” he says. “Of course, when they hit age 45 their vision will be different. There really isn’t a solution for presbyopia at this point, so they’ll need to wear reading glasses—that’s the solution. Who knows, maybe by the time these 20-year-olds are in their 40s there will be a better solution.”
Ultimately, the EVO continues to gain traction in the market, due in part to its accessibility. “It’s within the skill set of any trained anterior segment surgeon,” concludes Dr. Vukich. “You don’t need an excimer laser or a femtosecond laser. You don’t need all of the infrastructure that’s associated with LASIK. What you have is essentially something that can provide a positive service for patients by giving them an emmetropic result.”
Dr. Dhaliwal is a medical advisor for STAAR Surgical. Dr. Hovanesian consults for Bausch + Lomb. Dr. Vukich is a consultant for Bausch + Lomb and a principal investigator/medical monitor in the Apthera clinical trials, and a medical monitor/senior medical advisor for STAAR Surgical. Dr. Wiley is a consultant for Bausch + Lomb and STAAR Surgical.
1. Hydrophobic Acrylic Small Aperture Intraocular Lens Directions for Use. https://www.accessdata.fda.gov/cdrh_docs/pdf21/P210005C.pdf. Accessed April 2, 2024.