Vanessa Vera, MD
Iqbal Ike Ahmed, MD, FRCSC
Laser peripheral iridotomies are an effective way to treat angle-closure glaucoma. Nevertheless, any procedure that alters the eye anatomically can have unintended side effects, and for some patients, that's the case with LPIs. Creating a hole through the iris invites optical aberration, and many patients experience dysphotopsias following the procedure. However, it's possible that altering the position of the perforation could minimize this potential problem.
For many years, laser peripheral iridotomies have been placed superiorly, between 11 and 1 o'clock. Although there has been some anatomical justification for this choice of location, such as avoiding certain blood vessels, the primary reason for choosing this location was to cause the PI to be covered by the eyelid most of the time. The belief was that this would prevent the creation of visual aberrations.
Ironically, this placement could be having the opposite effect.
What brought this potential problem to our attention was patient complaints of visual disturbances following superior placement of LPIs. Some previous studies1,2 had suggested that the superior location of the PI might be responsible for these dysphotopsias; this was supported by anecdotal reports of cases in which patients described the presence of a visual symptom (such as a line) which disappeared when the eyelid was moved either lower or higher than its normal position. In addition, our group has been performing temporal PIs for many years, and as a result we've noted a reduction in the number of patients with linear dysphotopsia complaints.
For this reason we decided to conduct a formal prospective, randomized controlled study to assess whether changing the position of the LPI would alter the likelihood of experiencing dysphotopsia symptoms.
Testing the Theory
To conduct the comparison, we performed laser peripheral iridotomy on both eyes of patients who required this type of intervention. Before treatment, subjects were asked whether they already had any of the visual symptoms we hoped to avoid creating postoperatively: the presence of haloes; lines; crescents; ghost images; glare; shadows; blurry vision; or any other visual aberration. Then, one eye, chosen randomly, received an LPI (superior or temporal location chosen randomly); the other eye received an LPI at the opposite location. The order in which the eyes were treated was also randomized.
We suspected there might be a significant difference in the pain experienced when the PI was placed at the two locations as well, so following the procedure we asked patients to rank the pain in each eye on a scale from 0 to 10. (Of course, patients had no idea at that point which eye had received the LPI in which position.)
Finally, at the postop visit a month after the procedure, we documented the position of the PI in each eye—the distance from the limbus, size of the opening and whether the PI was completely covered by the eyelid, partially covered or exposed. We also measured the palpebral fissure and marginal reflex distance, and noted the presence or absence of cataract. Then, with the patient having experienced a month of normal living under varied light conditions, we asked if he had any changes in vision or was experiencing any of the dysphotopsias mentioned earlier.
We're still analyzing the data, but preliminary results suggest that patients with the superior PI had more complaints of linear dysphotopsias than patients in whom the PI was placed temporally. Most patients described the visual phenomenon as a line in the inferior field of vision that became more evident under bright conditions. The line's color varied from patient to patient; some described it as white; some described it as having a pink or bluish tint. Other types of visual phenomena such as crescents or haloes were also occasionally described, but the occurrence of those didn't reach statistical significance.
Analysis of the pain data is also preliminary, but we've already noted that temporal PIs seem to require less use of laser power to perforate the tissue, and the data so far suggest that temporal PIs were scored as less painful than superior PIs. For example, one patient reported the temporal PI pain as 2 out of 10; the superior PI was 8 out of 10. (Because of randomization, this trend can't be explained by which eye was done first or second.)
Why Switch to Temporal?
The reason for switching to a temporal site for the PI is to ensure that the PI is completely exposed, rather than partially or completely covered by the eyelid. Positioning the iridotomy temporally also provides easier ac-cess for the surgeon than positioning it nasally. Furthermore, in patients with significant superior pannus, visualization is easier with a temporal or nasal approach.
Why would a partially or completely covered PI produce more dysphotopsia than an exposed PI? A current theory is that the tear film at the edge of the eyelid creates a prism that bends the light and allows it to get underneath the lid and through the PI, finally hitting the retina. The nature of the refractory path creates a focused image on the retina. In contrast, when light passes through an exposed PI, there is no prism effect, so any light cast on the peripheral retina is blurred and doesn't create a clear image that the brain can perceive. This idea has been previously suggested1-4; we're working with optics experts to see whether we can prove that this is, in fact, what's happening in these patients. In the meantime, we haven't observed any increased risks associated with placing the PI at the temporal location.
The size of the perforation may also make some difference. A larger hole may result in
less diffraction of the light that passes through the PI, decreasing the likelihood of a visible dysphotopsia; a smaller hole might tend to produce the pinhole effect, creating sharper unwanted images on the retina. (Of course, a very small perforation could also reduce the effectiveness of the PI as a means for allowing aqueous flow.)
Managing Unhappy Patients
Even in the best of circumstances, some patients may still experience dysphotopsias after placement of an LPI, and the reality is that a few will be very upset by them. The situation may be analogous to implanting premium multifocal intraocular lenses; some patients don't mind the haloes and other effects that can accompany these lenses, but a few patients are miserable and demand that the lenses be removed.
We've heard about several doctors with patients who are demanding that something be done to eliminate or reduce post-LPI visual effects; there are even forums on the Internet where patients complain bitterly about the effects. They often say that their doctor failed to warn them about this possibility, and now they can't live with them—even that the visual effects are ruining their lives. Such comments may seem a bit extreme, but it's clear that none of us will benefit from having a patient who ends up feeling this way. This is especially true considering that we perform an LPI to prevent glaucomatous visual loss.
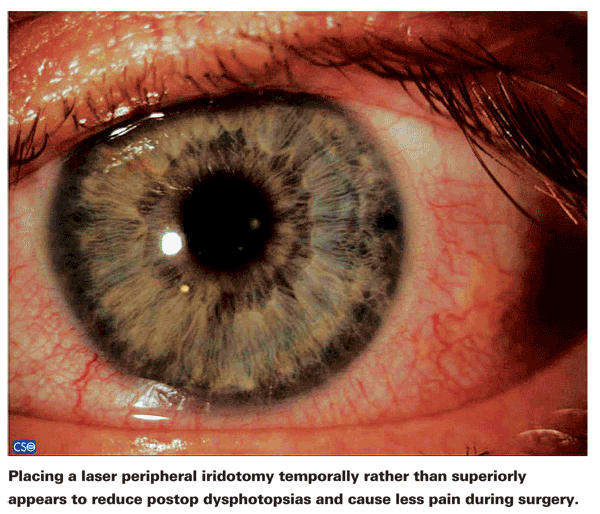
What can a clinician do to minimize the likelihood of such an unhappy outcome? First and foremost, it's essential to warn patients before performing an LPI that such effects may occur afterwards. (Fortunately, if a dysphotopsia does occur postop, it often resolves over time.) Second, placing the LPI temporally rather than superiorly does seem to mitigate the occurrence of such effects, and may reduce the pain associated with the procedure as well.
Finally, if a patient does end up with dysphotopsias that he's unable to tolerate, it's possible to create a small tattoo on the cornea directly in front of the PI, making the cornea somewhat opaque in that one spot. This has the effect of diffusing the light that passes through the PI, and hence should minimize or eliminate the dysphotopsia. Obviously, this option should be reserved for cases in which the patient is unwilling to accept anything less. Other options could include suturing of the LPI, or even enlarging the LPI to reduce the amount of diffraction. Contact lens wearers could try lenses with an opaque periphery.
A Step in the Right Direction
Fortunately, most patients who experience such visual effects after an LPI report that they only see them under certain lighting conditions and are willing to live with them. Nevertheless, even a few unhappy patients can be difficult to manage, so it behooves us to look for ways to minimize these unwanted aberrations. Hopefully, the strategies described here will help to accomplish that.
Dr. Vera recently completed her fellowship in glaucoma and advanced anterior segment surgery with Dr. Ahmed, who is an assistant professor at the
1. Murphy PH, Trope GE. Monocular blurring. A complication of YAG laser iridotomy. Ophthalmology 1991;98:1539-1542.
2. Spaeth GL, Idowu O, Seligsohn A, Henderer J, et al. The effects of iridotomy size and position on symptoms following laser peripheral iridotomy. J Glaucoma 2005;14:5:364-367.
3. Weintraub J, Berke SJ. Blurring after iridotomy. Ophthalmology 1992;99:479-480.
4. Islam N, Franks WA. Therapeutic corneal tattoo following peripheral iridotomy complication. Eye 2006;20:389–390. doi:10.1038/sj.eye.6701861.



