 |
Volume Uptick
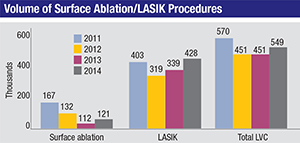
Last year marked the first time in several years that there was an increase in the average LASIK volume reported on the survey. The total number of procedures reported was 549,000, which is an increase of 22 percent over last year’s 451,000. Dr. Duffey notes though, that many sources still find volumes to be flat, so he’d like to see more data to declare this a solid trend.
“The sample size isn’t huge, but it’s pretty consistent year in and year out,” says Dr. Duffey. “Usually when it shows something, that trend will show on other indicators, as well. But as a general rule of thumb, I like to see a two-year trend. I think this coming year will really tell us if we’re truly up or not. I know in my practice I’m up a little from previous years. I hope that we’ve possibly reached the valley, if you will, and will start to see an upward trend. Some of the trend may be related to the economy, and some may be related to the good press we’re getting from the studies sponsored by ASCRS and AAO, as well as the independent studies such as Frank Price’s contact lenses vs. LASIK study and PROWL-1 and PROWL-2. So, with a combination of these things, the future is looking a bit better.”
 |
 |
Bilateral Surgery
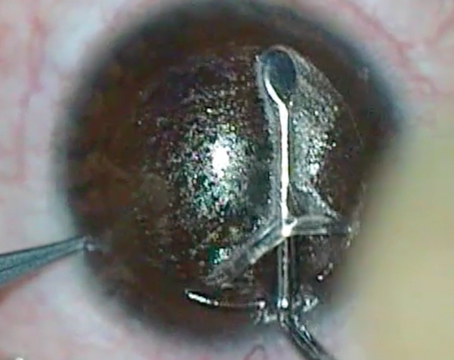
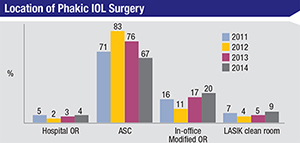
Interestingly, 23 percent of the surgeons say they do bilateral phakic lens implantation. Also, though 67 percent of the respondents usually implant phakic lenses in an ambulatory surgery center and 4 percent operate at a hospital, a fifth of them implant phakic lenses in an in-office modified operating room and 9 percent use a LASIK clean room. Dr. Duffey prefers to use his ASC, but explains where the in-office modified OR and LASIK room fit in: “The move to doing intraocular procedures in these locations is done mostly to save money; when a phakic lens is done, if you take the patient over to the ASC, a lot of your fee goes to the surgery center. I think for some to make it financially viable, they’ll establish an environment in their office that’s not really a sterile OR and make it as clean as they can.
“I used to have a LASIK clean room,” he continues. “It was an extra exam lane that we reserved for lasers. We added an air filter and dehumidifier, and were more conscientious about keeping it cleaner than just a standard exam room. I also use a minor OR in my office in which I do minor extraocular procedures such as pterygium removals, SFKs and conjunctival cyst excisions. I’ll rarely repair an emergency corneal perforation in it for a patient who doesn’t have insurance, or a gluing procedure for a corneal perforation. It’s my own bias, but I wouldn’t want to do an elective intraocular procedure in a minor OR where I normally do my external disease surgeries.”
Femtosecond Cataract Surgery
The survey has begun to feel out surgeons regarding femtosecond laser for cataract and correcting astigmatism in conjunction with cataract surgery.
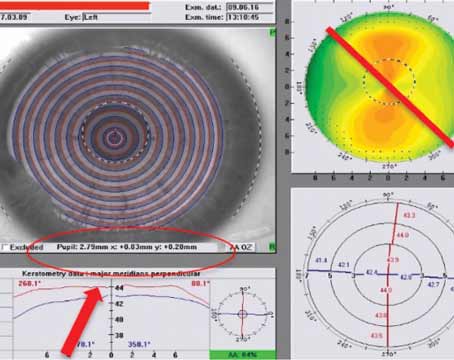
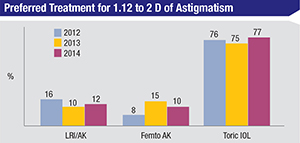
On the survey, the respondents say about 19 percent of their cases are done with the femtosecond laser. What was interesting, however, is that only 54 percent of the respondents use it to correct astigmatism, which was the main reason put forth for using the laser in order to get reimbursed in the first place. Eighty-four percent use it for the capsulotomy and 82 percent to fragment the nucleus. “It’s also interesting that only about half use it for the primary and secondary incisions,” says Dr. Duffey. “For me, 100 percent include AK. That was the indication that was put out there for it first, yet there are plenty of surgeons on the current survey using it for the capsulotomy and lens fragmentation alone.”
Dr. Duffey posits a reason why more corneal entry incisions aren’t being made with the femtosecond laser. “In my personal experience, the primary and secondary laser incisions are a little more difficult to open, and placing them exactly at the limbus vs. a little more anterior or posterior can be challenging to accomplish consistently. Sometimes, you get in there and you might wish that you’d been 0.5 mm more anterior or posterior with the incision; you can work around that, however. My biggest issue is that you can’t make a primary or secondary incision within 5 degrees of an AK incision. If you try to program it otherwise, the system won’t allow it. To eliminate that problem, I just do the capsulorhexis, lens fragmentation and AK with the laser. Then, in the OR, I’ll place my primary and/or secondary incisions manually where I want them. If they coincide with the AK, I still go at the same axis, only underneath it. I’ve spoken with Alcon about it and they say a fix for it will possibly be in a future software update.” REVIEW