Surgery on the eyelids is a delicate blend of science and art. So, too, is the art of informing patients of the pros and cons of cosmetic eyelid surgery. A good informed consent form, presented personally by the physician, does not simply inform. It can actually strengthen the doctor-patient relationship. If a problem occurs after surgery, the quality of that bond can make the difference between a trusting, though troubled, patient and an angry, litigious one.
Informed consent optimizes patient care, minimizes malpractice lawsuits that have accompanied recent increases in cosmetic surgery, and fosters patients' understanding of surgery.1 In my state, the process requires documentation that the patient was made aware of a risk after discussion with the physician, so it can't be delegated.2
In this article, I'll describe how I prepare patients for the risks and benefits of their procedure and which patients may not be ideal surgical candidates. I'll also explain how a consent form I use has been helpful in my practice. Each point in the consent is carefully covered in the preoperative office consultation.
Patient Selection
The patients who seek cosmetic blepharoplasty may have high, sometimes unreasonable, expectations of surgery. They may also have fears of the surgery. I use the informed consent as part of the patient education process to help make some of these expectations realistic, address any fears, and screen out patients who are not good candidates.
The most common questions cosmetic patients ask me are: Will the surgery change the shape of my eyes? Is it going to cause scarring? How much pain will be involved? When can I resume normal activities, such as vigorous exercise or work? Can you guarantee a good result?
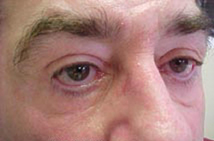 |
| This patient underwent blepharoplasty and developed lower eyelid retraction that necessitated two secondary procedures. He has continued experiencing lower lid retraction and symptoms of exposure. |
I tell patients that blepharoplasty isn't an exact science and that complications such as scarring vary among individuals. I show them photos of excellent, average and even sub-optimal outcomes. In addition, I tell them why the suboptimal results may have occurred and what I can do and they can do (such as pre- and postop care) to minimize the likelihood of such outcomes. I present the surgical risks but also offer a corresponding prevention or treatment to help allay any potential fears.
For example, when I mention the risk of excessive bleeding, I also tell the patient we'll stop blood-thinning medications before surgery.
Some patients may not be suitable candidates for cosmetic eyelid surgery. As I educate the patient about the pros and cons of surgery, I determine the patient's personality and motivations for the procedure. Several key factors are helpful in screening out patients who may not be suitable candidates for eyelid surgery. In my experience, such unsuitable patients tend also to be potentially litigious.
 |
| Note the appearance approximately three months after bilateral lateral tarsal strip procedures, lysis of scar tissue, topical application of mitomycin, posterior lamellar Alloderm grafting and periosteal midface lift. |
I am leery, also, of patients with obsessive-compulsive disorder or serious depression. It is important to pay attention to the patient's level of concern about complications or to an exceedingly harsh judgment of an alleged unattractive facial feature. The history must divulge all medications that the patient has been prescribed, including anti-depressants and anti-anxiety medications.
Other warning signs include patients who display a lot of anger and criticism of other surgeons they have seen, as well as those who say things like, "I can't live with this problem anymore." Other pa-tients may be unusually upset about a small but real defect.
The Consent Form
My informed consent form balances the copious suggestions from my malpractice insurer with my professional duty as a surgeon to inform patients of realistic risks and, benefits of and alternatives to surgery. It uses understandable language that is not cluttered with legal and medical jargon.
It is best to have your consent form reviewed by your malpractice carrier or attorney before using it. As an additional precaution, have a staff member on hand when you are discussing the risks of surgery and the informed consent form with the patient. The employee can serve as a witness to the process in case a malpractice suit does occur. Because laws vary from state to state and needs vary in individual practices, don't attempt to simply copy the summary below and begin using it as your own. It won't offer the legal protection you need.
I begin my consent form with a caveat: "The major risks of blepharoplasty (cosmetic eyelid) and blepharoptosis (drooping of the upper eyelid margins) are listed below. No list is complete. Even in the best of hands, the final surgical result cannot be guaranteed and, rarely, the condition may be worse than prior to surgery and require revisional surgery."
Then I describe possible complications, their relative risks, symptoms, and treatment. These include:
• orbital hemorrhage with potential for permanent visual loss;
• postoperative bruising that can be minimized by cold compresses and invariably dissipates;
• infection that requires treatment with antibiotics and, rarely, hospitalization;
• undercorrection with the potential for residual upper and lower lid skin and bulging fat and asymmetry;
• overcorrection with scarring in some patients that may result in decreased frequency, amplitude and velocity of the blink and subsequent dry eye; severe overcorrection may result in eyelid closure problems and permanent effects on vision;
• permanent double vision, an extremely rare complication that may necessitate prisms or even eye muscle surgery; and
• in extremely rare cases, abnormal scarring, persistent lid swelling and other unusual skin changes can occur, especially in patients with thin, sensitive skin.
I also describe exactly which lid features the surgery will not generally improve, such as crow's feet, smile lines or circles around the eye.
I describe the added risks of revisional blepharoptosis repair, which could include: effects on the contour or shape of the upper eyelid that distort its appearance; problems with the ability to close the eye; eyelid position abnormalities; cosmetic appearance problems; and possible effects on the upper eyelid position of the unoperated eye.
A signed informed consent form is no substitute for face-to-face patient education. Rather, it's a tool to use as part of the process of building a patient/physician relationship that will be your ultimate protection against patient litigation. Ultimately, an educated, well-selected patient is most satisfied with the entire surgical experience.
Dr. Mauriello is a clinical associate professor of ophthalmology at the University of Medicine and Dentistry of New Jersey in Newark, N.J.
1. Gurney M. Ten Years Experience in Aesthetic Surgery Malpractice Claims. Aesthetic Surg J 2001;21:569-571.
2. Arnold T. Professional Liability: Informed Consent Doctrine. NJ MED 2002;99:24-27.



