Lissamine staining, the Schirmer test and the recently developed Ocular Surface Disease Index are among the standard dry-eye diagnostic tools. In this article, experts in the field explain how they use these tools as well as steps they take to go beyond the standard and resolve more patients' dry-eye complaints.
Symptoms
The initial conversation with new patients is an integral factor not only in helping identify dry eye, but also in determining the severity level of "known" dry-eye patients. Although some of the questions may seem obvious, they are indeed important, explains Christopher J. Rapuano, MD, co-director of the cornea service at Will's Eye and professor of ophthalmology at Jefferson Medical College of Thomas Jefferson University.
"The first thing I ask patients is: What brought you here? I also ask them what symptoms they have and what treatments have they tried," he says, noting that patients often indicate that their eyes feel dry, scratchy, gritty, sandy or have the foreign body sensation; and artificial tears provide only temporary relief.
Fluctuating vision is a key, but not-so-obvious symptom that dry-eye experts look for. "Patients often say their vision fluctuates throughout the day without other symptoms. This is often a symptom of ocular surface problems, such as dry eye or blepharitis," Dr. Rapuano says.
Eric D. Donnenfeld, MD, in practice in 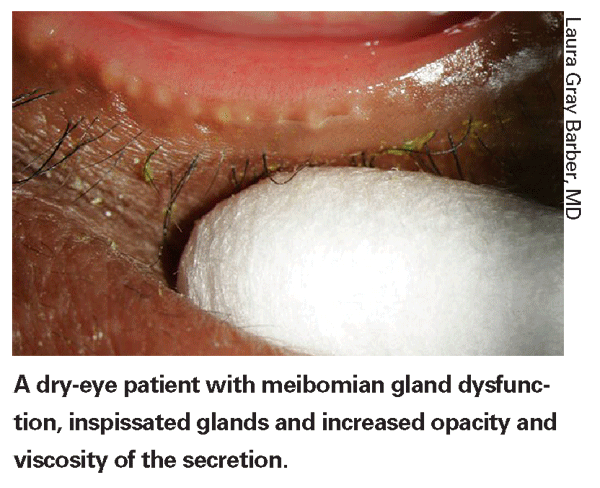
Any type of visual fluctuation that changes between blinks or during the course of the day is dry eye until proven otherwise, according to Dr. Donnenfeld. "The only exception is patients who have radial keratotomy, where the vision can fluctuate throughout the course of the day. For the most part, this symptom is a gold standard for me that this patient needs to be managed for dry eye. For instance, following cataract surgery or LASIK or PRK, patients often will complain of visual fluctuation and they will assume it is a problem with refractive surgery when in reality the cause of their problem is ocular surface disease and dry eye. Managing that will generally solve the problem," he says.
While it is known that the timing of symptoms is important, it bears repeating says Dr. Rapuano. "If the dry-eye symptoms tend to be when the patient wakes up in the morning, it tends to be blepharitis. If it is worse and worse throughout the day, then it tends to be a dry-eye type problem," he says.
In addition to a comprehensive ocular history, Dr. Rapuano reminds clinicians to ask about lid surgery, including blepharoplasty and lid lifts. "Patients do not think of this as surgery or they don't want to volunteer the information," he says. "I explain that it is important for us to know everything if we are going to take care of their eyes, and then they understand."
Many younger patients have contact lens intolerance. "I see young patients with dry eyes," he adds. "Many times it is related to chronic contact lens wear. For example, they started wearing them at age 12 and they are 25 or 30, and they have been wearing them more than half their life. We know that certainly can damage tear-producing cells and cause chronic dry eye."
Dr. Donnenfeld also is on the lookout for a history of contact lenses intolerance. "Many times patients are pre-selecting themselves for refractive surgery because they are unhappy contact lens wearers," he says. "When I see a patient who comes in with a history, I automatically do an aggressive ocular surface disease evaluation looking specifically for dry eye."
Age and Gender
When seeing a patient for surgical consultation who is female and over 40 (or postmenopausal women), Dr. Donnenfeld always considers dry eye. "These are the patients we really have to target in our preoperative evaluation and I have put them all on topical cyclosporine before LASIK or cataract surgery," he says.
Laurie Gray Barber, professor of ophthalmology at the
Dr. Barber adds that she asks female patients who line the inside of their eye lashes with eyeliner (rather than outside the lash, thus placing the makeup onto the ocular surface) to stop this practice. The meibomian gland can't provide healthy lipids to prevent the tear film from evaporating if it is covered with chemicals, she says.
Exam
During the exam, Dr. Rapuano notes that it can be helpful to check the vision, and then place some tear drops in the patient's eyes and re-check the vision. "Sometimes, I do this to show patients how bad their vision is without drops, especially for those who insist they do not have dry eye or those who already have been treated for dry eye," he says, adding that this illustrates that their vision improves when the surface is smoothed out.
As part of the standard workup, the slit lamp and staining provide needed clues to the patient's dry-eye severity. "I examine with and without tears, and then perform a good slit lamp exam without drops," Dr. Rapuano says. "Then I will put the fluorescein drops in as my first test. This will give me an idea if there is staining on the cornea and conjunctiva and tells me if there is anatomic pathology that puts them into a different category than those patients who just have symptoms with no objective evidence of a major problem. Depending on the patient and my concerns, I may use either rose 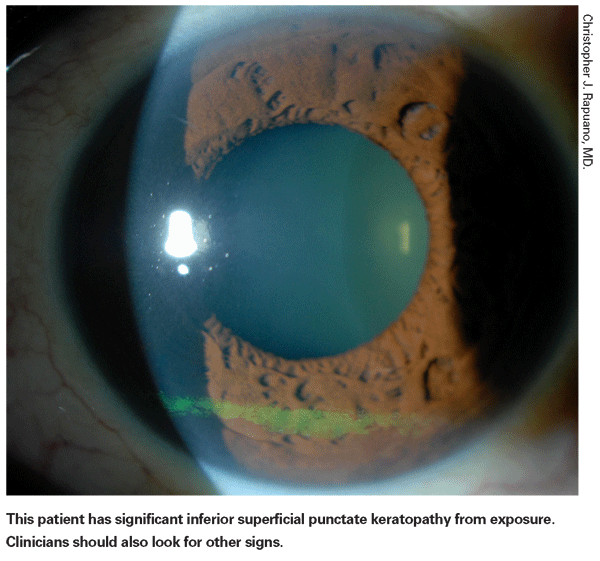
Dr. Rapuano also performs the Schirmer test (with anesthesia). "I give the patient drops and make sure I dry the eyes out so there are no excess tears, and then I put the Schirmer strips in for five minutes," he says. "There is obviously a big range in Schirmer testing. If it is a Schirmer test above 15, it tells me it is not major dry-eye problem; and if the Schirmer test is below 5, then it is probably a pretty significant dry-eye problem. There is a big range between 5 and 15 where the test is often not that helpful."
Recommended Therapies
For mild patients, avoidance or altering of a behavior or using occasional artificial tears may alleviate symptoms. For example, patients may use tears on a plane or while driving in a car, or they may considering not using an antihistamine that contributes to their dry eye symptoms.
For conventional aqueous deficiency dry eye, Dr. Donnenfeld starts with lubrication with tears to stabilize the ocular surface. "Gels and ointments at night are very good. A new tears product, Blink (AMO) is exciting. I have found that this has a very good characteristic of coating the tear film very well," he says, adding that he uses other tears such as Optiva (Allergan) and TheraTears (Advanced Vision Research) as well as others.
Dr. Barber notes that if a patient does have staining of the cornea or conjunctiva, her next step is to start the patient on topical cyclosporine 0.05% (Restasis). "There is a teaching process involved," she says. "I explain that they are using artificial tears and yet are still having symptoms, and that I can see disease of the ocular surface. Therefore, they need something that will decrease the inflammation in their tears. I also explain that it takes a long time to develop dry eye and it may take a little bit of time before the eyes are symptom-free."
Dr. Rapuano agrees that cyclosporine treatment takes time and patients must be educated. "One of the nice things about Restasis is that it is a twice-a-day medication," he says. "It is not just palliative, but it works well on a continual basis. It is important when patients start using Restasis that they don't stop using tears. Many patients make that mistake and stop taking their tears with the new medicine, but it takes Restasis a while to kick in. If they stop the tears, they will feel worse. This is an important thing to tell patients, even though it may be obvious to the clinician." He also mentions to patients that later the artificial tears may not be needed as much. 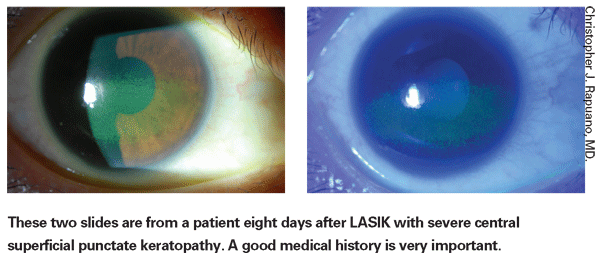
Dr. Donnenfeld has enhanced his regimen to try to provide faster relief. "I find that you can speed the return of ocular surface function and reduce burning and irritation by using low-dose corticosteroids with the cyclosporine," he says. "I will use loteprednol four times a day for a week or two and then taper down to twice a day for an additional month to get the patient started more quickly. They get faster relief and fewer cyclosporine side effects."
After cyclosporine, Dr. Rapuano proceeds to thicker tears, and then punctual plugs, if needed. "I like to use Restasis before punctual plugs because it is more physiologic," he says. "We are getting more, better tears being made all the time, and we are still getting the washing out effect of the tears. When we use plugs we get the tears to stay in the eyes longer, which is good, but we are not getting the same kind of washout effect. If the Restasis is not working well enough alone, or if they can't tolerate it, then plugs are often a good idea."
For more severe dry eye, Dr. Barber chooses punctal plugs but only after the patient has been treated with topical anti-inflammatory medication for three months. "I like the tear film to be healthier before I place the plugs," she says. "The premise of the plugs is to keep tears on the ocular surface longer. However, if the tears are toxic and sitting on the eye longer, you are not benefiting the patient at all." Dr. Barber has recently started using six-month dissolvable plugs instead of the umbrella-shaped ones that protrude slightly from the punctum. "I started using the plugs that are placed completely into the lacrimal duct and dissolve over four-to-six months," she says. "I have a wait-and-see approach. It seems like so many of the umbrella-shaped punctal plugs come out or irritate the patient down the road."
Very severe or end-stage dry-eye patients may require lacriserts, permanent punctual occlusion or other treatments. While these are not the norm, Dr. Rapuano says he treats some these patients at his practice.
Treating Other Conditions
"Many dry-eye patients have associated blepharitis, and they need to be treated for that, too. Otherwise, just treating the dry eyes will probably not be enough," explains Dr. Rapuano.
For patients who have meibomian gland dysfunction and blepharitis in addition to the normal therapy of hot compresses, Dr. Donnenfeld recommends nutritional supplements with flaxseed and fish-oil combinations that improve the quality of the meibomian gland secretions.
"I also have been using very successfully topical azithromycin ophthalmic solution [AzaSite 1%, InSite Vision] drops," he says. Patients put the drops in for one month at night before sleeping, and the drops adhere to the lid margin. "Because of the intrinsic solubility of azithromycin, it gets absorbed into the lid margin where the combined anti-inflammatory and anti-infectious characteristics of azithromycin make it an ideal drug for treating meibomian gland dysfunction," he says. Dr. Barber also azithromycin ophthalmic solution to treat blepharitis, as well.
Patient Follow-up
Dr. Rapuano usually sees patients again in about three months or six months if they have a mild case of dry eye. If the patient starts Restasis, several months are needed in order to allow time for it to begin to work well. Other, more severe cases require a shorter follow-up time.
By following the Ocular Surface Disease Index and considering these additional pertinent factors of dry eye, ophthalmologists can more quickly zero in on dry eye cases and get patients on their way to effective treatment.



