Presentation
A 52-year-old Asian woman with no previous ocular history presented to the Wills Eye Emergency Room with a history of decreased vision in both eyes for the past five days. In addition, she reported symptoms of headache, malaise and mild neck stiffness for the past one to two weeks. The patient described her blurred vision as rapid in onset, painless and non-progressive.
Medical History
The patient had a history of chronic hypertension, controlled with thiazide diuretics. The patient did not have a history of ocular trauma or surgery. She did not experience fevers, chills, nausea, vomiting, rashes, skin changes, joint pains, shortness of breath or other neurological symptoms. The patient’s social history was unremarkable.
 |
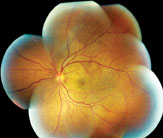 |
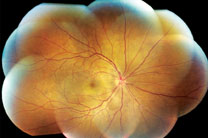
| Figure 1. Fundus photograph montage of the right eye (left) and Figure 2, a montage of the left eye. Both demonstrate multiple serous retinal detachments and retinal striae throughout the posterior pole, extending up to the optic disk. There is also mild erythema of both optic nerve heads.
| |
On exam, the patient’s visual acuity was 20/100 in the right eye and 20/400 in the left eye. Her pupils were symmetric, and there was no relative afferent pupillary defect. Her motility was full and her visual fields were full to confrontation in both eyes. Intraocular pressures were 19 mmHg in the right eye and 21 mmHg in the left eye.
The patient’s slit lamp examination was significant for the presence of 1+ white blood cells in the anterior chambers of both eyes. There were no keratic precipitates or iris nodules in either eye. She had 2+ nuclear sclerotic cataracts in both eyes.
Dilated fundus examination demonstrated bilateral serous retinal detachments with prominent peripapillary retinal striae, mild erythema of the optic nerve heads, and scattered subretinal white spots in the midperiphery of both eyes (See Figures 1 and 2).
What is your differential diagnosis? What further workup would you pursue?



