A 35-year-old man presented to the Wills Eye Institute’s Cornea Service complaining of two weeks of pain, light sensitivity and decreased vision in the left eye. Prior to his referral he was treated for bacterial keratitis for two weeks with initial improvement. After tapering off antibiotic drops, he returned 10 days later complaining of redness and decreased vision. At this point, he was started on gatifloxacin drops every hour, prednisolone four times daily, and referred to Wills Eye Institute for further management.
Medical History
Past ocular history was significant for keratoconus in both eyes. He wears daily wear soft contact lenses in the right eye and a hybrid contact lens in the left eye. He denied any history of trauma, swimming, hot tub use or showering with his contact lenses. He had no past medical history, prior medication use or allergies.
Examination
Ocular examination revealed corrected visual acuity of 20/25 in the right eye, uncorrected visual acuity of 20/400 in the left eye. Pupils were equal and reactive to light. Intraocular pressure was 18 mmHg in the right eye and 19 mmHg in the left eye. Visual fields were full to confrontation and extraocular movements were full in both eyes.
| ||||||
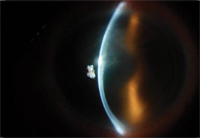
On slit lamp exam, the right cornea showed keratoconus with a Fleisher ring and inferior pannus. Examination of the left cornea revealed a triangular infiltrate measuring 0.8 x 1.0 mm, with fine satellite infiltrates superiorly, inferior stromal edema and large white keratic precipitates. The anterior chamber had 3+ white blood cells but no hypopyon (See Figure 1). The posterior exam was unremarkable.
What is your differential diagnosis? What further workup would you pursue?
What is your differential diagnosis? What further workup would you pursue?
- See more at: http://www.revophth.com/content/d/wills_eye_resident_case_series/i/2417/c/41029/#sthash.x427xWBf.dpufWhat is your differential diagnosis? What further workup would you pursue?
- See more at: http://www.revophth.com/content/d/wills_eye_resident_case_series/i/2417/c/41029/#sthash.x427xWBf.dpuf