Presentation
A 57-year-old Caucasian woman presented after noticing gradual ptosis of
the left upper lid, occurring over a period of one month.
|
Medical History
The patient’s past medical history was significant for mild gastroesophageal reflux disease and a recent diagnosis of multiple myeloma. She had no known history of diabetes or hypertension. She was on one chemotherapeutic agent, lenalidomide, and denied tobacco, alcohol or illicit drug use. Her family history was significant for cancer. Her ocular history was significant only for presbyopia. Her review of systems was otherwise negative.
Examination
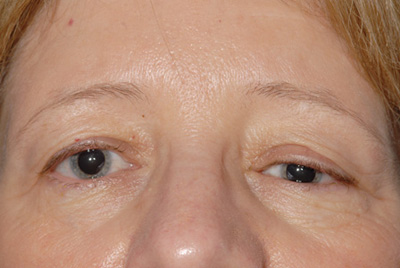
Best-corrected visual acuity was 20/20 in each eye. Pupils were 3 mm in each eye with no afferent pupillary defect present. Extraocular movements were full in both eyes, and the patient denied pain. The mean reflex distance (MRD1) measured 4 mm in the right eye, and 2 mm in the left eye (See Figure 1). Levator excursion measured 14 mm in the right and 13 mm in the left eye. Hertel exophthalmometry was 15 mm in both eyes with a base of 108 mm. The slit-lamp and dilated fundus examination was unremarkable.
What is your differential diagnosis? What further workup would you pursue?