“Emmetropic presbyopes are the hardest patients to treat,” says John Hovanesian, MD, who is in private practice in Laguna Hills, Calif. “These patients have had good distance and near vision their entire lives and don’t want to wear reading glasses. Most of these patients, typically the younger ones, have a bias against monovision, which would be the only other option.”
Currently, three corneal inlays are in various stages of development. The Flexivue Microlens (Presbia) is a refractive inlay that alters the index of refraction by using a bifocal optic. The Raindrop (ReVision Optics) is a reshaping inlay that changes corneal curvature, and the Kamra (AcuFocus) inlay, which was recently approved by the Food and Drug Administration, employs small-aperture optics to increase the depth of focus.
All are implanted in the nondominant eye. “All of the inlays are considered modified monovision, because they are all intended to be done in a single eye. One of the advantages of this is that you retain better distance vision while still gaining good near vision,” says Richard Lindstrom, MD, who is in private practice in Minneapolis.
Each of the inlays has advantages and disadvantages. “One of the advantages of all of the inlays is that they are removable and, for the most part, reversible. It’s not like a corneal laser procedure, which creates a multifocal corneal shape that is irreversible,” adds Michael Gordon, MD, who is in private practice in La Jolla, Calif.
Flexivue Microlens
The Microlens is a transparent, hydrogel-based, concave-convex lens. It has a plano central area to provide distance vision, surrounded by rings with different add powers to provide intermediate and near vision.
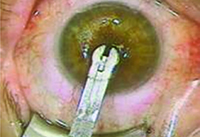 |
| Figure 1. Presbia’s insertion tool places the Flexivue Microlens into the pocket. (Image courtesy Richard Lindstrom, MD.) |
In a study conducted in Greece, 47 patients were implanted with the Flexivue Microlens and were followed for 12 months.2 One year postoperatively, patients’ mean uncorrected near visual acuity significantly improved from 0.68 ±0.03 logMAR to 0.14 ±0.9 logMAR in the operated eyes and from 0.53 ±0.13 logMAR preoperatively to 0.13 ±0.13 logMAR binocularly. UCNVA of the operated eyes was 20/32 or better in 75 percent of patients 12 months after inlay implantation, and mean uncorrected distance visual acuity in operated eyes significantly decreased from 0.06 ±0.09 logMAR preoperatively to 0.38 ±0.15 logMAR, but it did not change significantly binocularly.
Dr. Gordon participated in Flexivue’s clinical trial. “We have had great success with the Flexivue in my hands in the clinical trial,” he says. “Most people love it. We are seeing great patient acceptance. They are reading glasses-free. They do not have issues driving at night from glare. The beauty is that it is a refractive inlay, meaning that it comes in powers. Younger presbyopes can have a lower-power implant. As these patients get older, the lower-power implant can be removed, and a higher-powered one can be implanted. The Flexivue has a lot of potential, I believe, and is probably 1.5 years away from approval. It’s reversible. It’s upgradable. It’s very well-tolerated, and it’s easy to implant. I have been impressed with the Flexivue both as a product and as a surgical procedure.”
Raindrop
This corneal inlay is a clear, permeable, positive meniscus-shaped hydrogel implant with a diameter of 2 mm, a center thickness of 32 µm, and approximately the same refractive index as the cornea. While it has no refractive power, it alters the eye’s refractive power by increasing the central radius of curvature of the part of the cornea overlaying the implant. It is thinner at the edge than it is at the center, so when implanted, it creates a hyperprolate corneal shape, which results in a multifocal cornea. Oxygen and nutrients freely pass through the highly permeable hydrogel material used for the inlay.
Two studies have been conducted recently, and both used keratotomy to create a flap with a diameter greater than 8 mm and a depth of 130 to 150 µm using a femtosecond laser.3,4 An inserter for the Raindrop inlay is provided by the manufacturer, and the inlay is placed on the stromal bed and correctly positioned over the center of the pupil. Then, the flap is replaced over the inlay.
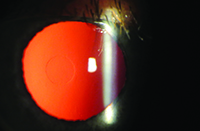 |
| Figure 2. The Raindrop inlay. (Image courtesy John Hovanesian, MD.) |
Mean photopic contrast sensitivity in the eye with the inlay was similar to preoperative levels at both the six-month and 12-month follow-up visits.
All participants in this study completed a patient questionnaire concerning spectacle wear and satisfaction. Twelve months after implantation of the inlay, 95 percent of patients said that they were satisfied or very satisfied with their near and intermediate vision. All patients reported that they were very satisfied with their distance vision and the overall visual outcome. Additionally, 84 percent reported rarely, if ever, wearing glasses.
The second study included 16 hyperopic presbyopic patients who were implanted with the Raindrop inlay immediately after laser corneal correction of the hyperopia.4 Mean UCNVA in the implanted eye was 20/21 (Snellen) ±0.04 (logMAR) after 12 months, and mean uncorrected intermediate visual acuity was 20/26 ±0.07. Uncorrected distance visual acuity was 20/31 ±0.14 after 12 months, and mean binocular UCNVA was 20/21 ±0.03 after 12 months. Additionally, mean binocular UCIVA was 20/26 ±0.08, and mean UCDVA was 20/19 ±0.11 after 12 months.
Patient satisfaction questionnaires were also completed by all patients in this study. Fourteen of the 16 patients said that they were satisfied or very satisfied with their near, distance and overall vision.
“The Raindrop has finished clinical trials, and data are being submitted to the FDA,” Dr. Lindstrom says. “It works similarly to presby-LASIK. There is some loss of distance vision with this approach, and it looks like you only lose a line or two at distance and you gain three to four lines at near, so it is a reasonable trade-off. It has similar advantages and disadvantages to a multifocal IOL or contact lens, so most eye doctors are familiar with the optics.”
Kamra
The Kamra is currently the only FDA-approved corneal inlay. The current version is a 5 µm thin microperforated artificial aperture made of polyvinylidene fluoride with incorporated nanoparticles of carbon. It has a total diameter of 3.8 mm and a central aperture of 1.6 mm. The inlay has 8,400 holes that range in size from 5 to 11 µm in diameter to allow water and nutrition flow to prevent corneal thinning and epithelial decompensation.
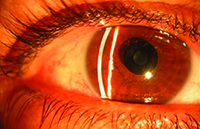 |
| Figure 3. The Kamra inlay. (Image courtesy Richard Lindstrom, MD.) |
Currently, the inlay is implanted in a lamellar pocket created with a laser that is 220 µm or deeper. Creating a pocket with a femtosecond laser reduces the impact on corneal nerves and reduces the risk of dry eye postoperatively.
Minoru Tomita, MD, PhD, of the Shinagawa LASIK Center, Tokyo, and colleagues have conducted two large studies using the Kamra inlay.5,6 One study included 223 eyes in 223 patients who had previously undergone LASIK and then were implanted with the current version of the Kamra inlay.5
The patients’ mean age was 53.6 years (range: 44 to 65 years), and mean manifest spherical equivalent was −0.18 D (range: −1.00 to +0.50 D). The mean UCDVA in the operated eye decreased from 20/16 preoperatively to 20/20 after the inlay had been implanted for six months. Mean UCNVA improved from J8 to J2. Patients’ dependence on reading glasses and their satisfaction with vision without reading glasses significantly improved by six months postoperatively.
An earlier study conducted by Dr. Tomita and colleagues included 360 eyes in 180 patients who underwent simultaneous corneal inlay implantation and LASIK to treat presbyopia in patients with hyperopia, myopia or emmetropia.6 Preoperative UCDVA and UCNVA were significantly different between the three groups of patients, while no significant difference was seen six months postoperatively.
Hyperopic presbyopic patients had an improvement of three lines in UCDVA and seven lines in UCNVA at six months after implantation. Emmetropic presbyopic patients had an improvement of one line in UCDVA and six lines in UCNVA, and myopic presbyopic patients had an improvement of 10 lines in UCDVA and two lines of UCNVA.
Postoperatively, patient satisfaction with regard to spectacle independence and overall vision was significantly increased in hyperopic and emmetropic patients. However, it was not significantly increased in myopic patients who had good UCNVA preoperatively.
“The Kamra uses small-diameter aperture optics and hyperfocality,” Dr. Lindstrom says. “This is basically the optical system that is used in a disposable camera that allows a decent picture at distance, intermediate and near. The eye needs to be set slightly myopic. The ideal target for the Kamra would seem to be -0.75. You get a close to 3-D increase in depth of focus, which allows functional distance, intermediate and near vision. The negative is that if you use small-diameter aperture optics in a dusky mesopic environment, you still have a small aperture, so things are dimmer in a low-light environment. You need significant light for this system to operate well. That’s why you only do it in one eye.”
“One consideration with this implant is that it is dark in color,” Dr. Hovanesian adds. “If it is centered over the pupil, it looks beautiful, but in lighter-colored eyes when viewed from the side, sometimes it can show. It works very well in terms of achieving near vision while not too badly degrading distance vision.”
He also explains that all three implants have some need for follow-up, and the follow-up care for these patients is not as simple as with LASIK. “You need to be watchful for signs of intolerance or signs of dry eye, and there is an explant rate of about 10 percent. This is better than LASIK because our alternative to this procedure is to just give a patient monovision, and of course monovision degrades the patient’s distance vision in the treated eye,” he says.
Although the three inlays have different mechanisms of action, they all look promising. “All of these approaches work,” Dr. Lindstrom says. “Each one arguably has some features that one doctor might like over another. I’m an advocate of all of these. I’d love to see them all get approved.” REVIEW
Dr. Gordon is an investigator for Presbia and serves on its Medical Advisory Board. Dr. Lindstrom is a board member at AcuFocus. Dr. Hovanesian is an investigator for ReVision Optics.
1. Arlt EM, Krall EM, Moussa S, Grabner G, Dexl AK. Implantable inlay devices for presbyopia: The evidence to date. Clin Ophthalmol 2015;9:129-137.
2. Limnopoulou AN, Bouzoukis DI, Kymionis GD, et al. Visual outcomes and safety of a refractive corneal inlay for presbyopia using femtosecond laser. J Refract Surg 2013;29(1):12-18.
3. Garza EB, Gomez S, Chayet A, Dishler J. One-year safety and efficacy results of a hydrogel inlay to improve near vision in patients with emmetropic presbyopia. J Refract Surg 2013;29(3):166-172.
4. Chayet A, Barragan Garza E. Combined hydrogel inlay and laser in situ keratomileusis to compensate for presbyopia in hyperopic patients: One-year safety and efficacy. J Cataract Refract Surg 2013;39:1713-1721.
5. Tomita M, Kanamori T, Waring GO, Nakamura T, Yukawa S. Small-aperture corneal inlay implantation to treat presbyopia after laser in situ keratomileusis. J Cataract Refract Surg 2013;39:898-905.
6. Tomita M, Kanamori T, Waring GO, et al. Simultaneous corneal inlay implantation and laser in situ keratomileusis for presbyopia in patients with hyperopia, myopia, or emmetropia: six-month results. J Cataract Refract Surg 2012;38:495-506.



