Dry-eye disease, also known as dysfunctional tear syndrome, is still an under-diagnosed and under-attended problem, although it is very common.1 Some clinicians inappropriately diagnose different conditions as dry eye, while others rarely make a diagnosis of dry eye and, thus, under-diagnose it. Despite recent guidelines, such as those from the International Task Force,2 diagnosing and treating dry-eye disease can be challenging in some patients.
In many cases, dry eye is diagnosed based largely on the patient's symptoms, and patients' subjective descriptions of their symptoms vary. Unfortunately, the signs and symptoms do not always correlate all that well. Interestingly, patients with more severe dry-eye disease tend to complain about visual problems from a compromised corneal surface, but they do not have many symptoms. On the other hand, patients with seemingly less- severe dry eye may have symptoms way out of proportion with the signs.
We do have various tests available that can be used to document and support diagnosis and initiate appropriate treatment based on severity grade. Therefore, in my dry-eye clinic, I have implemented a multi-step strategy in the care of dry-eye patients. Most importantly, I take the time to listen to the patient's explanation of her symptoms as the signs of dry eye disease can sometimes change with environmental factors. Then I examine the ocular surface to determine the severity grade to help devise the best and most effective strategy for each individual patient.
Talking with Patients
With all new patients, but especially potential dry-eye patients, it is very important to listen carefully to what they say. I often start off by asking them what it is that bothers them and the reasons for their visit to the clinic. Then, I give them time to explain. They usually explain their situation well. Dry-eye patients are very educated. They know when their symptoms started and exactly what it is that they experience. If clinicians let their patients talk, patients will explain it to them clearly.
I find this is very helpful particularly in the differential diagnosis. For example, if a patient is complaining of worsening of her symptoms earlier in the morning upon awakening, this might mean an evaporative type of tear deficiency rather than an aqueous type. If a patient complains of experiencing pain at night severe enough to wake her up from sleep, it probably means corneal epithelial erosion even though you might not see it at the slit lamp at the time of the exam. These patients may also have lid closure problems, such as nocturnal lagophthalmos, in addition to their dry eye.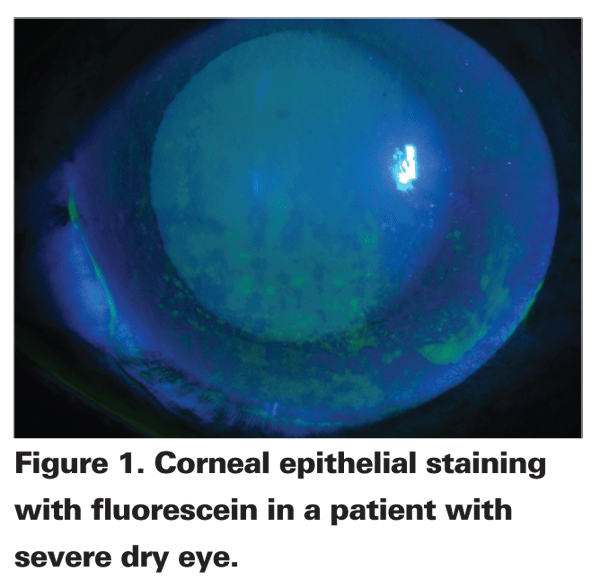
Once I have listened to the patient carefully, I start asking questions. Although in any patient who presents with complaints of burning, itching, dryness, discomfort, redness and excessive tearing, the first thing that comes to mind should be dry-eye syndrome, other ocular surface conditions that might cause these symptoms should be ruled out. For example, allergies often go hand-and-hand with dry eye, but they require different treatments. As a matter of fact, the allergy treatments with antihistamines sometimes might aggravate the patient's dry eye. Other possible conditions, such as infectious conditions, also need to be ruled out. For example, patients with adenoviral conjunctivitis or Thygesons's superficial keratitis sometimes get misdiagnosed as having dry eye just because the patient is complaining of excessive tearing. My favorite misdiagnosis is anatomically blocked tear ducts in patients complaining of excessive tearing and some burning and redness. Because dry eye is known to cause some reflex excessive tearing intermittently in some cases, these patients are diagnosed as having dry eye and referred to dry-eye clinics rather than oculoplastics!
I also ask questions and make observations to see if the patient has an underlying problem that might be causing the dry eye. For instance, does he have any known medical problems, such as rheumatoid arthritis or thyroid disease? Is the patient female and postmenopausal? I have developed a questionnaire that I use for all new patients, but especially for dry-eye patients, with questions related to all of their systems not just the eyes.
I take my time and look for certain findings that might be clues for underlying but previously undiagnosed conditions. I look at the hair, the face and the hands of the patient. I look for skin diseases, such as rosacea, psoriasis, eczema, etc. I check to see if there are lid abnormalities, such as sag or retraction of the lids, as occurs in thyroid disease. If they have certain changes in their hand joints, they might have a rheumatoid arthritis.
I take notice of the patient's behaviors as well. For instance, Sjögren's syndrome patients usually come in with a bottle of water and they talk as if their mouth is very dry. In severe cases you can actually hear them breathe because their nose is so dry. It is important to pay attention to every detail, because the treatment strategies as well as the prognosis are different in the patients with underlying medical conditions.
Questions concerning family history are also important. For example, if Sjögren's syndrome or thyroid disease runs in their family that would be suspicious for an underlying cause.
Severity and Durations of Symptoms
Ophthalmologists also have to pay close attention to the severity and the duration of the symptoms, which are very important in planning the treatment of dry eye. In some cases, patients may explain that they are only bothered by symptoms some of the time. For example, if they experience symptoms only intermittently while checking e-mails or surfing the Internet and the ocular surface seems healthy, then it might not be necessary to put them on a long-term prescription medicine, and you probably do not need to see this patient within a short period of time.
In other cases in which the patient is constantly bothered by her symptoms and the clinical exam reveals a deficient tear film with ocular surface changes, immediate action is warranted. In these cases, patients often say they can't do the computer work or reading that they might need to do on a regular basis as required by their jobs, for example; they already take artificial tears regularly without much relief. If testing reveals staining of the ocular surface, which means a compromised ocular surface, then there is no point in telling this patient to just increase the amount of the tears used or switch to another brand. This is the type of patient that definitely needs a long-term treatment with a prescription medicine, such as cyclosporine eye drops. A follow-up visit should be scheduled in a short period of time for this type of patient to ensure the health of the ocular surface.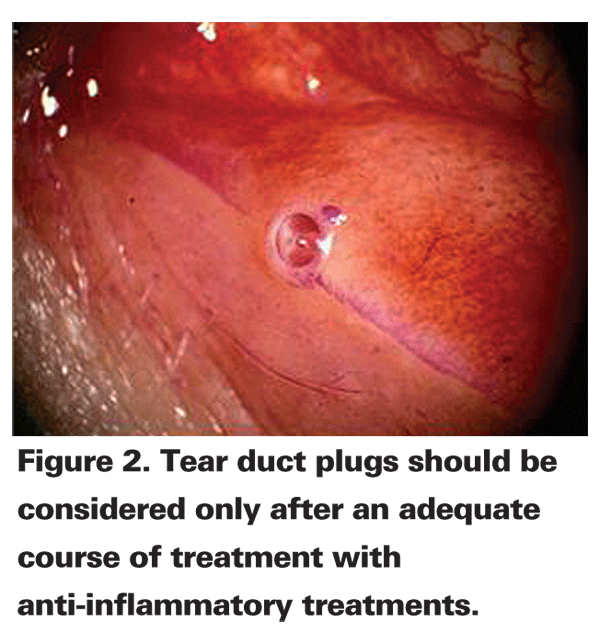
From the patient's perspective, the definition of intermittent and mild symptoms is subjective, and thus varies from patient to patient. For example, some patients complain bitterly. They say that they have severe dry eye all the time, and they can't go out or do computer work because their eyes are so sensitive, yet upon inspection of the tear film, Schirmer's testing and ocular surface staining, the results show otherwise. Then I suggest that the patient do several things: implement or continue a healthy lifestyle; eat a balanced diet; drink water as much as possible; and avoid natural diuretics such as coffee or alcohol. I also recommend an artificial tear product to be used on a regular basis. If they don't respond to these measures, then I would go to the next level, which is topical cyclosporine. I believe that it makes sense to treat dry eye with prescription medicines before ocular surface changes occur.
Testing
Examining the ocular surface and testing periodically provides the documentation needed to track the dry-eye progress and response to treatment objectively. At our dedicated dry-eye clinic, we perform almost all of the related dry-eye testing for all new patients, including the Schirmer's test (with and without anesthesia); tear-film breakup time; quality of meibominan gland secretion; lissamine green staining of the conjunctiva; fluorescein staining of the cornea; and either impression cytology or a biopsy of the conjunctiva in more severe-looking cases. At each follow-up visit, we definitely repeat the ocular surface staining, inspection of the tear film and meibomian gland secretion test to determine the efficacy of the treatment. Other tests, such as the Schirmer's or impression cytology of the conjunctiva for goblet cell counts, are done less frequently.
If the patient is complaining of severe symptoms and there are significant findings, (i.e., staining of the surface, Schirmer's levels are depressed, or the tear-film breakup time is decreased), then another modality, such as a steroid eye drop, could be added to the cyclosporine regimen, albeit for a short period of time, until the cyclosporine has kicked in. In severe cases, tear duct plugs or cauterization of the tear ducts should be considered only after an adequate period of anti-inflammatory treatments in order to not get an adverse reaction from the "toxic tears" full of harmful mediators. I usually reserve autologous serum tears for patients with corneal problems due to severe dryness, as it is difficult to maintain the patients on it forever. Also, these are the patients who need to be followed very closely to track progress and check for possible corneal ulcers, if they don't already have them.
We recently reviewed the records of our dry-eye patients and noted that the great majority of the patients have a combined aqueous and evaporative type of dry-eye disease. This is an important finding, as patients with clinically significant posterior blepharitis or meibomian gland dysfunction need to be treated with separate, more targeted modalities for that. I prefer azithromycin (AzaSite) eye drops rather than oral tetracyclines. It is a topical broad-spectrum antibiotic with significant anti-inflammatory effects similar to oral tetracyclines but without potential systemic side effects, such as liver problems or interactions with other drugs that the patients might be on.
Based on the clinician's judgment, patient complaints and testing, a severity grade for dry eye can be formulated and then the appropriate treatment can begin. It is important to establish a follow-up schedule based on the severity grade. Ophthalmologists really have to listen to the dry-eye patient for the best diagnosis and treatment. Initiation of anti-inflammatory treatments such as topical cyclosporine, earlier rather than later, is preferable to prevent worsening of the condition.
Dr. Akpek is an associate professor of ophthalmology and director of the Ocular Surface Diseases and Dry Eye Clinic at the Wilmer Eye Institute at
1. Lemp MA, Baudouin C, Baum J, et al. The definition and classification of dry eye disease: Report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007;5:75-92.
2. Dysfunctional tear syndrome: A Delphi approach to treatment recommendations. Cornea. 2006;25:900-7.



