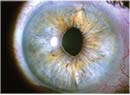
Untreated allergies may be the culprit, according to Deepinder K. Dhaliwal, MD, L.Ac., professor of ophthalmology at the University of Pittsburgh School of Medicine, director of refractive surgery and the cornea service at UPMC Eye Center and founder and director of the university’s Center for Integrative Eye Care. “The bottom line is that allergy promotes inflammation,” she says. “When you’re an allergic individual and you have untreated allergies, you have more inflammatory mediators circulating and causing damage. We know that in PRK, people that are atopic have more haze and regression. Patients with LASIK and allergies have a higher chance of having DLK. Even in cataract surgery, if someone’s really atopic, they could have more inflammation or they could want to rub their eye, which could result in problems with wound deposition.” To help ensure good visual outcomes and patient well-being, Dr. Dhaliwal has instituted the “Pittsburgh Protocol” to control local allergy symptoms perioperatively and to maintain that control after surgery.
Identifying Problems
“For refractive surgery, we do two evaluations: One is just to see if you’re a candidate; the other is to dilate your eyes and get the precise measurements. So at the first visit, we identify all allergy patients and start them on the correct therapy,” says Dr. Dhaliwal. “I will not operate on anyone who has untreated allergies. So at the University of Pittsburgh, what we do now is ask everybody, ‘What are you allergic to?’ We always ask about allergies, but a lot of times patients may not even know the specific things they’re allergic to. That’s why it’s really important to question them and get an appropriate history taken. Then, on the exam, we’ll rule out any dryness,” she says.
Itching is the main symptom of allergic conjunctivitis: If it’s absent, then ocular allergy may not be the culprit. Dr. Dhaliwal distinguishes between seasonal allergic conjunctivitis, which is episodic in nature depending on the specific allergen (airborne pollen from grasses, plants or trees), and perennial allergic conjunctivitis arising from chronic exposure to dust mites, molds and pet dander.
Before tailoring the treatment to the allergy symptom, Dr. Dhaliwal also needs to find out what medications patients already take. “We have them write down every single thing that they take,” she says, noting that that’s another way she gets tipped off to a patient’s underlying allergy issues. “A lot of people don’t think an allergy pill is medication,” she observes. “Because they get it over the counter, they consider it more as a supplement or something like that. The problem is that systemic antihistamines cause drying that’s detrimental to the ocular surface and leads to more problems down the road.” Dr. Dhaliwal seeks alternative therapies for allergic patients taking oral antihistamines. “In the Visx manual, it even says that patients on Claritin had a much longer time to re-epithelialization. I wouldn’t purposely have somebody on oral antihistamines if their ocular surface was dry, because I know that they’ll have healing issues,” she says.
Topical Treatment Options
Once she’s confirmed a problem and sussed out medicines that could contribute to ocular dryness, Dr. Dhaliwal works to find the right treatment or combination of treatments to target a patient’s allergy symptoms. “The most important thing is to identify the patient’s issues and treat them locally. We treat what’s causing their symptoms: Do they have allergic conjunctivitis? Allergic rhinitis? Or do they have more of a pharyngeal asthma? Allergic conjunctivitis is very well treated with topical combination antihistamine/mast-cell-inhibitor drops like Zaditor (Alcon). Those are really great. There are so many different varieties, and they’re available over the counter now,” she says. Other combination mast-cell-inhibitor/antihistamine drops include olopatadine HCL (Patanol); ketotifen fumarate (Alaway); azelastine HCl (Optivar); epinastine HCl (Elestat); and bepotastine (Bepreve). Topical steroid drops include loteprednol etabonate (Alrex and Lotemax). Topical drops may have the added benefit of helping to wash out some offending allergens.1
“If they have more of a rhinitis, there’s Flonase (GlaxoSmithKline), which is fluticasone, a nasal steroid. For patients with more of an allergic-asthma component to their symptoms, we ask them to try Singulair (Merck). It’s a wonderful pill because it helps to curb the allergic response, but it does not cause any drying of the eyes. So those types of medicines have really been
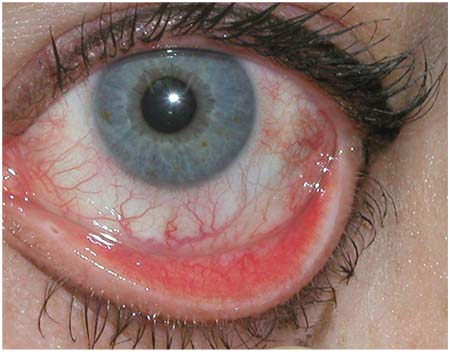 |
| Patients with ocular allergies may benefit from targeted multisymptom relief, including combination antihistamine/mast-cell-stabilizer eye drops. |
Dr. Dhaliwal says that this period of localized treatment dovetails with the approximately three-week period when patients must abstain from contact lenses prior to surgery. “They need to keep their contact lenses out for about three weeks, so typically, we’ll try to optimize them in two to three weeks, and then we do surgery,” she explains, adding that the Pittsburgh Protocol allergy-treatment regimen also extends for about a week postoperatively.
It doesn’t necessarily follow that patients will discontinue their targeted pharmacotherapy once they’re through the early postop period, however. Dr. Dhaliwal says that some of her refractive and cataract surgery patients with severe allergy symptoms seek longer-term relief, consulting with allergists for comprehensive testing and the initiation of immunotherapy. “We have people get allergy tests, and then allergy shots if they need them,” she says. “That’s been very beneficial for a bunch of patients who have significant allergies. Some people initially put up a bit of a stink about it and say, ‘Allergy shots? I thought that was just for kids!’ Obviously, instituting immunotherapy takes much longer, and it’s not as though I’d have them start doing allergy shots before their surgery: That would take too long. But we do educate patients, telling them, ‘You know, you don’t have to live like this.’ ”
Dr. Dhaliwal notes that a patient seeking the lasting relief immunotherapy provides may no longer be limited to subcutaneous treatment. “What’s really cool is that now they have sublingual immunotherapy, so you can take a pill to help you get over your allergy to, say, ragweed.” FDA-approved sublingual immunotherapies include tablets to combat allergic reactions to grass pollens, ragweed and dust mites. “I don’t currently have any patients who’ve had experience with that, but I’m looking forward to seeing it work,” she says. “It’s something that could be really beneficial.”
Allergen Avoidance
Nonpharmacologic options for allergic refractive and cataract surgery patients include cold compresses to stop itching and prevent eye rubbing; artificial tears; and simple allergen avoidance. Dr. Dhaliwal says that this last measure is frequently overlooked. “People forget this, but if you just avoid going outside when the pollen levels are high, for example, you’re going to be okay,” she says. “When you come inside after a high-pollen day, you’ve got to take a shower, wash your hair and change your clothes immediately upon getting in the house. But a lot of people don’t do that: They end up rubbing their eyes. They sleep on a pillow that has pollen all over it from their hair, and then they wonder why they wake up with itchy eyes in the morning. We do a lot of basic education. We spend a lot of time with our patients talking about allergy avoidance, whether it’s environmental, triggered by animals or anything else. If patients are allergic to cats and dogs, but have pets that sleep in the same bed with them, we have them change the sheets and make sure that the animals are not in the room during the perioperative and postoperative periods. I tell them, ‘Have at least one room that is going to be animal-free. After surgery, take your nap there, and that’s your special place to stay, where you can just rest and recover without any animal dander near you to make you itch.’ Obviously, if patients rub their eyes after LASIK, it’s a big problem,” she says, since they might disrupt the flap or set the stage for epithelial ingrowth.
“We really don’t want people to be exposed to their allergens,” she stresses, adding that avoidance of seasonal allergens can dictate the timing of surgery if necessary. “If a patient has a springtime issue, we can always do it later in the year,” she says. “I just ask them, ‘When are your allergies the worst?’ and then try to avoid operating during that time period, if possible.”
Although she has not done any comparative studies on the outcomes of her allergic patients since instituting the Pittsburgh Protocol, Dr. Dhaliwal is convinced of its value. “I haven’t done any head-to-head studies because if I have a patient with allergies, I treat them,” she says. Localized treatment with rapid onset of action and extended duration has helped her cataract and refractive surgery patients enjoy better visual outcomes, and sometimes even long-term allergy-symptom relief.
“Its funny, but very many people are really happy after getting off their systemic antihistamines,” Dr. Dhaliwal reports. “I’ve had patients say, ‘I feel better off of them, and I’m going to continue on this localized therapy even though I’m healed postoperatively.’ ” REVIEW
Dr. Dhaliwal is a consultant for Bausch + Lomb and a Visx trainer.
1. McGill JI, Holgate ST, Anderson DF, Bacon A. Allergic eye disase mechanisms. Br J Ophthalmol 1998;82:1203–14.