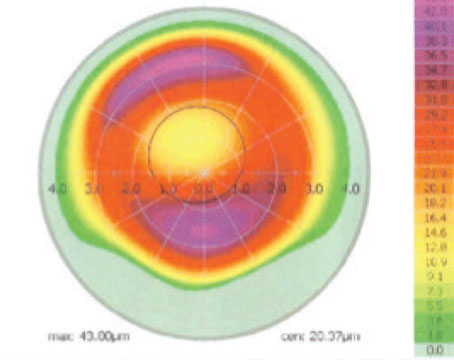
In a retrospective study of patients who underwent LASIK surgery between 2005 and 2014, researchers from Holon, Israel, wanted to compare the astigmatism induced surgically by spherical hyperopic LASIK versus myopic LASIK in nonastigmatic eyes. The researchers calculated the mean absolute SIA and performed risk-factor analysis for induced astigmatism. Differences between H-LASIK and M-LASIK were analyzed.
The study analyzed eyes of 3,877 patients who underwent M-LASIK and 549 patients who underwent H-LASIK, and who were non-astigmatic preoperatively and received a non-astigmatic treatment. Three months after surgery, hyperopic treatment induced more astigmatism (0.49 ±0.48 D) than did myopic treatment (0.36 ±0.4 D) (p<0.001). In the H-LASIK group, the risk factors for induced astigmatism greater than 0.5 D were a higher preoperative refractive error (p=0.003) and larger optical zone (7 vs. 6 mm).
In the M-LASIK group, eyes with SIA greater than 0.5 D tended to have steeper corneas preoperatively (43.8 ±1.5 vs 43.6 ±1.4 D; p=0.001), a higher spherical equivalent (-3.43 ±1.53 vs. -3.07 ±1.45; p<0.001), and smaller treatment zones (6 vs 7 mm). In H-LASIK, the mean induced astigmatic axis was 74.6 degrees.
Based on the results of this retrospective study, researchers concluded that there was a consistent trend toward more SIA in H-LASIK and in higher refractive error correction. In H-LASIK, larger optical zones induced more SIA, while in M-LASIK smaller ones caused it.
Cornea 2017;36:1040-1043
Karmona L, Mimouni M, Vainer I, et al.
Visual and Refractive Outcomes of SMILE
Researchers from Hong Kong investigated the effect of the learning curve on small-incision lenticule extraction during surgeons’ first two years of experience.
SMILE was performed using the 500-kHz VisuMax femtosecond laser by the same surgeon. The initial 100 patients after the surgeon started operating independently were Group 1; the most recent 100 patients were Group 2. The same laser settings and technique were used. The visual and refractive outcomes were compared between groups at postoperative week one and at six months. Vector analysis was performed for eyes with astigmatic correction.
Two hundred right eyes of 200 patients were included. Age, preoperative corrected visual acuity, manifest refraction and central corneal thickness were similar between groups (p≤0.154). Postoperatively, the efficacy index at one week was better in Group 2 (Group 1: 0.85 ±0.16 vs. Group 2: 0.91 ±0.10; p=0.019) but was similar between groups at six months (Group 1: 0.91 ±0.14 vs. Group 2: 0.94 ±0.08; p=0.181). The safety index was higher in Group 2 at one week (Group 1: 0.93 ±0.10 vs. Group 2: 0.95 ±0.08; p=0.045) and six months postoperatively (Group 1: 0.97 ±0.07 vs Group 2: 0.99 ±0.03; p=0.011). Vector analysis showed that postoperative residual astigmatism and misalignment of astigmatic correction were lower in Group 2 than in Group 1 (p≤0.039) at one week and six months. The duration of docking and duration of lenticule extraction were shorter in Group 2 (p≤0.034).
Researchers concluded that the study showed that faster visual recovery, a better safety profile and more accurate astigmatic correction could be attained with increasing surgical experience.
Cornea 2017;36:1044-1050
Chan T, Ng A, Cheng G, et al.
Access to YAGs: Optometrists vs. Ophthalmologists
Researchers from the Mayo Clinic in Rochester, Minn., wanted to quantify Medicare beneficiary proximity to his or her YAG-capsulotomy-providing ophthalmologist or optometrist in Oklahoma by calculating driving distances and times.
The cross-sectional cohort study used 2014 Oklahoma Medicare 100-percent and 5-percent data sets and Google Maps distance and travel- time application programming interfaces. These data sets were obtained to identify the office street addresses of Oklahoma ophthalmologists and optometrists who submitted claims to Medicare for a YAG laser capsulotomy, and the county addresses of the corresponding Medicare beneficiaries who received the laser capsulotomies. The shortest travel distances and travel times between the beneficiary and the laser provider were calculated by using Google Maps distance and travel time interfaces.
In 2014, 90 (57 percent) of 157 Oklahoma ophthalmologists and 65 (13 percent) of 506 Oklahoma optometrists submitted a total of 7,521 and 3,751 YAG laser capsulotomy claims to Medicare, respectively. By using the Medicare Limited 5-percent dataset, there was no difference in driving distance between beneficiaries who received a laser capsulotomy from an ophthalmologist (median: 39 miles; interquartile range: 13 to 113 miles) compared with an optometrist (median: 46 miles; IQR: 13 to 125 miles; p=0.93) or in driving time to an ophthalmologist (median: 47 minutes; IQR: 19 to 110 minutes) compared with an optometrist (median: 50 minutes; IQR: 17 to 117 minutes; p=0.76).
Based on these results, researchers stated that, for Medicare beneficiaries, there was no difference in geographic access to YAG laser capsulotomy whether performed by an Oklahoma ophthalmologist or optometrist as determined by calculated driving distances and times.
Ophthalmology 2017;124:1290-1295
Mahr M, Erie J
Brolucizumab vs. Aflibercept For Neovascular AMD
In a prospective, randomized, double-masked, multicenter, two-arm, Phase II study, researchers compared the efficacy and safety of brolucizumab with aflibercept to treat neovascular age-related macular degeneration.
The study examined 89 treatment-naïve participants, aged 50 and above, with active choroidal neovascularization secondary to AMD. The eligible participants were randomized 1:1 to intravitreal brolucizumab (6 mg/50 μl) or aflibercept (2 mg/50 μl). Both groups received three monthly loading doses and were then treated every eight weeks (q8) with assessment up to week 40. In the brolucizumab group, the final q8 cycle was extended to enable two cycles of treatment every 12 weeks (q12; to week 56); participants on aflibercept continued on q8. Unscheduled treatments were allowed at the investigator’s discretion. The primary and secondary hypotheses were noninferiority (margin: five letters at a one-sided alpha level 0.1) in best-corrected visual acuity change from baseline of brolucizumab versus aflibercept at weeks 12 and 16, respectively. BCVA, central subfield thickness and morphologic features were assessed throughout the study.
The mean BCVA change from baseline (letters) with brolucizumab was noninferior to aflibercept at week 12 (5.75 and 6.89, respectively [80 percent confidence interval for treatment difference: -4.19 to 1.93]) and week 16 (6.04 and 6.62 [-3.72 to 2.56]), with no notable differences up to week 40. Outcomes exploring disease activity during the q8 treatment cycles suggest greater stability of the brolucizumab participants, supported by receipt of fewer unscheduled treatments versus aflibercept (six vs. 15) and more stable CSFT reductions. In addition, from post hoc analysis, a greater proportion of brolucizumab-treated eyes had resolved intraretinal and subretinal fluid compared with aflibercept-treated eyes. Approximately half of the brolucizumab-treated eyes had stable BCVA during the q12 cycles. Brolucizumab and aflibercept adverse events were comparable.
During the matched q8 phase, the BCVA in brolucizumab-treated eyes appeared comparable to aflibercept-treated eyes, with more stable CSFT reductions, receipt of fewer unscheduled treatments and higher rates of fluid resolution. The brolucizumab safety profile was similar to aflibercept over 56 weeks of treatment. Researchers claim that a 12-week treatment cycle for brolucizumab may be viable in a relevant proportion of eyes.
Ophthalmology 2017;124:1296-1304
Dugel P, Jaffe G, Sallstig P, et al.
Macular Degeneration and Aspirin Use
Researchers from Glendale, Calif., reviewed current literature on the benefits that aspirin provides for patients’ cardiovascular health compared with the risk of worsening age-related macular degeneration. They performed a review and critically analyzed six cardiovascular and four ophthalmological trials regarding risks and benefits of aspirin use. The prospective, randomized cardiovascular trials comprised 167,580 subjects, while the three smaller ophthalmological data sets had 12,015 subjects.
The meta-analysis of the literature demonstrated a statistically significant 32-percent reduction in the risk of nonfatal stroke with regular aspirin users. The study also documented that aspirin users decreased the risk of fatal vascular deaths by 15 percent. Of the three ophthalmological studies highlighting the adverse affects of aspirin associated with AMD, all suggested an exacerbation of AMD without statistical significance or broad confidence bands.
Overall, the researchers say the number, size and quality of the cardiovascular studies recommending aspirin use are far superior to the fewer, smaller and conflicting studies suggesting a possible adverse effect of aspirin use in relation to AMD. The benefits of aspirin usage include preserving the duration and quality of life by decreasing stroke and heart-attack risk, according to the results. Researchers say that these benefits seem to far outweigh the theoretical risks of possibly exacerbating wet AMD, which can be reasonably controlled with anti-VEGF therapy.
Retina 2017;37:1630-1635
Small K, Garabetian C, Shaya F
Gamma-Irradiated Corneal Patch Graft Thickness
This cross-sectional study of graft thickness using anterior segment optic coherence tomography was conducted at Johns Hopkins Hospital to measure gamma-irradiated sterile cornea patch graft thickness as a function of time after surgery, estimate the rate of graft thinning, and determine risk factors for graft thinning. They examined 107 patients (120 eyes, 120 ADDs) 18 years or older who underwent aqueous drainage device surgery at Johns Hopkins with GISC patch graft between July 1, 2010, and October 31, 2016.
Of the 107 patients included in the analysis, the mean age was 64 ±16.2 years. The mean time of measurement after surgery was 1.7 years (range: one day to six years). Thinner grafts were observed as the time after surgery lengthened (regression coefficient, -60 µm per year since surgery; 95% CI: -80 to -40 µm). The odds ratio of undetectable grafts per year after ADD surgery was 2.1 (95% CI: 1.5-3.0; p<0.001). Age, sex, race, type of ADD, quadrant of ADD placement, diagnosis of uveitis or dry eye, and prior conjunctival surgery weren’t correlated with the presence or absence of the graft.
This study showed that on average, the longer the time after surgery, the thinner the graft. These findings suggest that placement of a GISC patch graft is no guarantee against tube exposure, and that better strategies are needed for preventing this complication.
JAMA Ophthalmol 2017;135:941-946
Moledina A, Wang J, Jampel H, et al.