• The UniversIOL Calculator. Samir Sayegh, MD, PhD, of Champaign, Ill., and his co-workers began developing this IOL calculator in response to what they saw as shortcomings in other calculators, especially with regard to toric lens calculation. The UniversIOL calculator is a web-based calculator that combines the major available lens formulas with a toric IOL calculator.
“The first thing we concentrated on was getting the sphere correct, and we provide a number of tools to do this,” Dr. Sayegh explains. “We don’t propose a new formula per se as some others might, but bring together all the high-quality third- and fourth-generation IOL formulas in one calculator. The user has the ability to use any one of these or a combination of them that would give him the best of all the formulas’ calculations. The calculator also tells you how much the formulas differ from each other to give you a sense of how close you’ll be to your target. The calculator also contains all the IOLs made so you can tell it which ones you work with. In other words, one IOL may get you close, but another might get you closer to your target. That’s the idea of this kind of database approach to getting the spherical equivalent right.”
Dr. Sayegh says the calculator will also perform a toric calculation at the same time as the sphere. “Previously, the standard approach for a surgeon using a toric lens would be to calculate the spherical power on a device such as the IOLMaster, and then go to an on-line toric calculator and re-enter the data to get a toric lens that corresponds to the sphere he or she had selected,” says Dr. Sayegh. “This is time-consuming and risks entering incorrect data. Our calculator lets surgeons do the whole computation at once, though it also offers the standard approach of sequential data entry in case surgeons are more comfortable with that.” He says that, since there may be some inaccuracies with the use of a constant toricity ratio used by some calculators, the UniversIOL also offers the option of using the more accurate variable toricity approach. Also, since the calculator has many variables, surgeons can lock in certain ones that they use frequently so they don’t have to re-enter them each time.
Dr. Sayegh says that using the calculator’s hybrid approach has achieved 95-percent accuracy in terms of eyes within 0.5 D of the predicted result, and nearly 1,000 eyes have been done using the calculator. Though the calculator will be released for general use in May 2016, Dr. Sayegh says high-volume practices can get early access by contacting him directly at sayegh@umich.edu. “Fairly high volume surgeons with high-quality measurements usually result in solid, standardized ways of doing the calculations that bring the best results,” explains Dr. Sayegh. To see what the calculator looks like, visit 2020eyecenter.com/iol-calculator/.
• The Hoffer H-5 formula. In the March 2005 installment of Technology Update, Santa Monica surgeon Kenneth J. Hoffer told readers about his H formula, calling it a “work in progress,” since it still had some shortcomings. Now, however, almost 11 years and thousands of surgery cases later, he reports that his work is complete in the form of his new H-5 formula. “In 2013 I came up with a formula improvement called the Hoffer H-5 formula,” Dr. Hoffer explains. “It uses gender and race to change the average mean values in the Holladay-2 and Hoffer formulas. To create it, since it’s based on gender and race, we decided to collect eyes especially from Europe, the Middle East, Asia and South America. That took quite a lot of time, especially getting everyone involved at the various clinical and university practices to fill out the spreadsheets with all the necessary data. In the end, we had 9,800 eyes. We realized, though, that when you’re getting data from so many disparate offices and clinics from around the world, they were using different methods to collect it, so it wasn’t always going to be perfect. So, we decided the best way to analyze the data was to look at what the prediction errors were. We focused on all the eyes that were within ±0.25 D of the predicted result. We figured data that yields a result within ±0.25 D has to be pretty accurate.”
The next step for Dr. Hoffer and his co-workers was to take the eyes that made the cut, which wound up being 2,700 that were within the required ±0.25 D of prediction, and run the results compared to other popular IOL formulas. “Since it’s based on the Holladay-2, but with the addition of gender and race—even though it changes some of the Holladay-2’s parameters—we figured the Holladay-2 would be the formula against which to test it. Unfortunately, I was informed that a bulk input of the data into the Holladay IOL Consultant software wouldn’t be possible. That meant I’d have to hire someone to sit for several months and input 9,800 eyes. Since that wasn’t going to happen readily, we tested it against other popular formulas: the Hoffer Q; the Holladay-1 and the SRK/T. We couldn’t test it against the Haigis because we weren’t able to personalize the factors a0, a1 and a2. I’m pleased to say that the results from the H-5 came out as a statistically significant improvement over the other formulas.”
Dr. Hoffer says one of the reasons the formula is accurate is because it allows the surgeon to customize the IOL calculation for a particular patient. “For instance, if the patient is a Japanese woman, the formula goes to the “Asian, female” section on the input data, and it would then use the mean for an Asian female axial length, lens thickness, anterior chamber depth and K reading,” explains Dr. Hoffer. “We replaced the means for average humans used in the Holladay-2 for actual means for particular genders and races.”
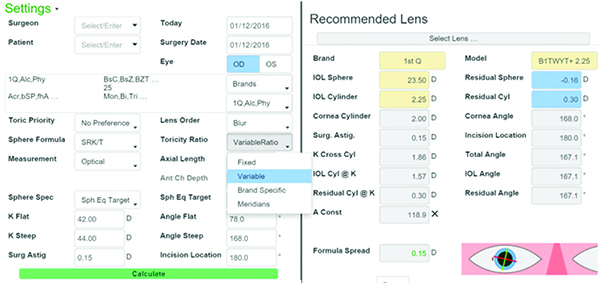 |
| The UniversIOL calculator offers various methods to factor in the toricity when calculating a toric intraocular lens, including brand-specific values, fixed toricity and variable toricity, which some surgeons consider to be the most accurate way to calculate the value. (Image courtesy Samir Sayegh, MD, PhD.) |
Dr. Hoffer says he hopes the specific averages built into the formula will enable surgeons to get better results. “Ultimately, the goal is to develop a formula that’s useful in all eyes,” he says.
• Radial basis function approach. On the leading edge of IOL calculation is this mathematical approach, from a team of surgeons and engineers led by Mesa, Ariz., biometry guru Warren Hill, MD. The RBF method uses artificial intelligence and pattern recognition to select an IOL for a patient.
Dr. Hill says that going outside the world of ophthalmology has allowed the problem of IOL power selection to be approached in a completely different way. “The goal of this project was nothing less than reinventing the way we think about it,” Dr. Hill says. “Our core team investigators, the engineers at the company MathWorks and a dedicated group of physician beta testers in eight countries have successfully developed and validated a new way to select the power of an intraocular lens that is independent of vergence formulas, or a knowledge of the effective lens position.” The details of this project were presented as the Charles D. Kelman Lecture at the 2015 annual meeting of the American Academy of Ophthalmology.
Dr. Hill says his team devised this approach by fitting a large and highly accurate LenStar database to a sophisticated pattern recognition and data interpolation model called a radial basis function, which is based in artificial intelligence. “Radial basis function algorithms are used throughout the world in a wide range of technologies as diverse as facial recognition software, thumbprint security scanners, automobile engine calibration methods, electrocardiogram interpretation and financial forward forecasting software for the stock market,” Dr. Hill says. “In creating the Hill-RBF algorithm for IOL power selection, the objective was to discover if the power of an intraocular lens could be predicted significantly better than by using vergence formulas. Following extensive modeling, we found that four variables—the desired spherical equivalent, axial length, central corneal power and anterior chamber depth—were all that was needed to accurately predict the necessary IOL power.” Dr. Hill points out that current methods mostly limit possibilities to situations that are already understood. On the other hand, pattern recognition has the ability to learn tasks based solely on data, independent of what is previously known, so there is no calculation bias. “Short eyes, long eyes, unusual anterior segments simply represent patterns of data,” he says.
Based on a review of over 260,000 cases submitted for optical biometry lens constant optimization over more than a decade, Dr. Hill says that the vast majority of ophthalmologists have a ±0.50 D accuracy ranging from 76 to 80 percent. Approximately 6 percent of physicians are at 84 percent ±0.5-D accuracy and less than 1 percent are at 92 percent or better. In a recent retrospective study of 3,212 cases by 13 surgeons in eight countries, Dr. Hill says the ±0.50 D weighted mean accuracy of the Hill-RBF method was 95 percent.
The next step involves prospective testing and making the Hill-RBF model available to ophthalmologists worldwide. “Haag-Streit will soon incorporate this into the LenStar EyeSuite,” Dr. Hill says, “and, in an act of generosity, it has also agreed to make this technology available to ophthalmologists as an open-access, web-based calculator, much in the same way that Graham Barrett made his Barrett Universal II formula and the Barrett Toric Calculator available. By the time of the ASCRS meeting in May, there’s a good chance it will be available as a LenStar upgrade.” To learn more about the Hill-RBF lens selection method, you can visit rbfcalculator.com. REVIEW
Dr. Hill is a consultant to Haag-Streit. Dr. Sayegh has no financial interest in the products mentioned. Dr. Hoffer licenses the use of his formula.