Not so long ago, treatments for macular degeneration were very limited (and not very effective). One of the few available options was laser photocoagulation, used to ablate tissue as a means to stop bleeding. Then photodynamic therapy and anti-VEGF agents appeared, and laser—never seen as an ideal option—started looking even less advantageous.
Here, a number of surgeons share whether they believe the laser still has a place in the treatment of AMD.
Staying Extrafoveal
Although surgeons agree that the laser is unacceptable for use in the fovea, not everyone agrees about whether it's still a valuable tool for treating extrafoveal lesions.
"In new-onset wet AMD, abnormal blood vessels have started to develop," says Carl Regillo, professor of ophthalmology at
"At this point, I very rarely use laser photocoagulation to treat choroidal neovascularization," agrees Thomas A. Ciulla, MD, retina specialist at the Midwest Eye Institute and assistant professor of ophthalmology at the Indiana University School of Medicine. "We usually treat any lesions in or close to the fovea with intravitreal injections, sometimes combined with photodynamic therapy. Using photoablation close to the fovea can cause a scotoma, leading to vision loss or difficulty reading, and in cases of myopic degeneration you may see a secondary atrophy of the retinal pigment epithelium surrounding the laser scar in the months or years following treatment, enlarging the scotoma. We may still use the laser far from the fovea, but those lesions are uncommon."
"I was never a big user of laser photocoagulation, and I've never done a subfoveal laser coagulation," says Fareed Ali, MD, FRCS(C), director of clinical research at the Canadian Centre for Advanced Eye Therapeutics in
Unintended Consequences
Beyond the fact that laser photocoagulation doesn't address the underlying causes of macular degeneration and damages tissue in hopes of achieving a beneficial effect, many surgeons are concerned about triggering an even stronger recurrence. "Some clinicians believe the laser 'seeds' the choroidal neovascularization membrane so that it recurs—and does so very aggressively at the edge of the laser scar," notes Dr. Ciulla. "It's possible that the laser elicits a localized inflammatory response, which could be somewhat angiogenic. In addition, in many cases you're disrupting the antiangiogenic Bruch's membrane barrier. That, in and of itself, can cause choroidal neovascularization membranes to form."
Faik Gelisken, MD, attending physician in the Department of Ophthalmology at the
Other studies suggest that there may be additional unintended consequences of laser treatment. In one small study reported at this year's Association for Research in Vision and Ophthalmology meeting, researchers found that in patients with bilateral central macular drusen, peripheral laser photocoagulation appeared to correlate with changes in central drusen area—in both the treated eye and the fellow untreated eye—at two years of follow-up. (Kesting S, et al. IOVS 2009;50:ARVO E-Abstract 187) Treated eyes received 200 argon laser spots, 500 µm in diameter. In most treated eyes, drusen area significantly decreased, while in the untreated eyes the change was split between significant increases and decreases. (The authors noted no CNV or visual acuity changes in either eye.)
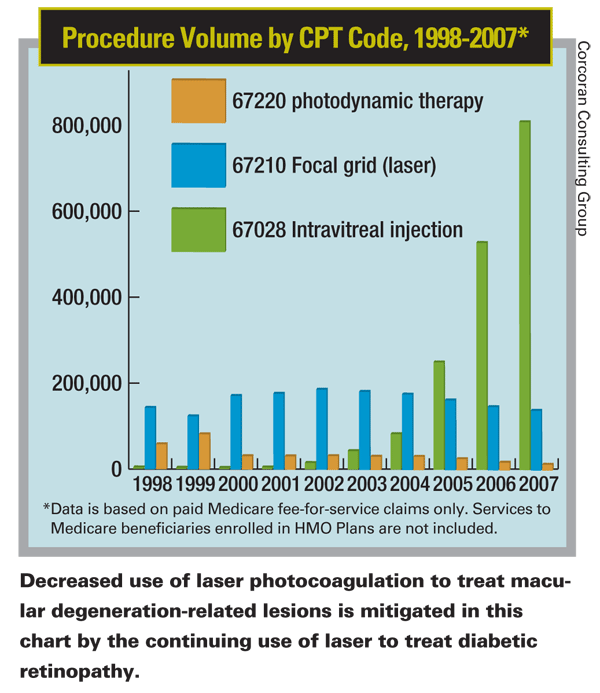
In Defense of Photocoagulation
"Laser photocoagulation has always had a limited role in treating macular degeneration, and that may be truer now than ever," says Dr. Regillo. "On the other hand, some surgeons may have the impression that there's no role for laser anymore, and that's not the case. For selected patients it can provide a permanent cure for wet AMD without the need for ongoing injections.
"I think most surgeons would agree that when the neovascularization is several hundred microns away from the foveal center, laser is the preferred option," he continues. "You really don't want to commit patients to injections for the rest of their lives when you might be able to control the problem with one application of traditional laser photocoagulation. I don't think you can throw away the laser and claim to be offering complete care for wet macular degeneration."
Not every surgeon agrees. "I don't think you'll need a lifetime of Lucentis to treat an extrafoveal problem," says Dr. Ali. "A few injections, possibly in combination with a steroid, should close off the bleeding within a relatively short period of time. Besides, laser has a high recurrence rate—20 to 50 percent, depending on which studies you go by."
Dr. Ciulla concedes that a patient would benefit if a single laser treatment resolved the issue. "The problem is, if neovascularization does return, it can do so very aggressively," he notes. "And if aggressive lesions occur following laser treatment, patients may assume that the laser made it worse."
The Best of Both Worlds?
Another possibility is combining laser photocoagulation with other treatments, especially the anti-VEGF compounds. Dr. Regillo says the combination might make sense when the laser is treating a lesion that's close to the fovea. "The closer the neovascularization is to the foveal center, the greater the likelihood of a recurrence," he explains. "This may be related to the margin you allow with the laser, which gets smaller as you get closer to the center. The drug might help to prevent that recurrence—but many surgeons wouldn't even attempt to use the laser when the lesion is close to the center."
Dr. Gelisken was the lead author on one retrospective, interventional pilot study, reported at this year's ARVO meeting, that examined the safety and efficacy of combining intravitreal bevacizumab and laser photocoagulation when treating extrafoveal choroidal neovascularization secondary to AMD. (Gelisken F, et al. IOVS 2009;50: ARVO E-abstract 186) Nine eyes of nine patients received laser photocoagulation treatment for well-defined extrafoveal lesions; intravitreal bevacizumab was then injected three times at six-week intervals. (Additional injections were done if fluorescein angiography revealed further leakage.)
The average number of injections required by one year was 4.1 (range: 3 to 8). Four eyes needed extra injections, and one eye developed subfoveal recurrent CNV. At the one-year visit, best-corrected visual acuity had improved (although not significantly); mean central retinal thickness decreased significantly, from 223 to 179 µm (p=0.024). The authors noted that the combination was well-tolerated and effective in most eyes.
What about simply using anti-VEGF drugs by themselves to treat extrafoveal choroidal neovascularization? Dr. Gelisken notes that he hasn't seen any studies reporting on the effectiveness of intravitreal anti-VEGF monotherapy for treating extrafoveal CNV. "That makes it difficult to compare anti-VEGF monotherapy with this combination therapy," he notes. "However, in our small case series only one eye had subfoveal recurrent CNV with profound vision loss; most of the patients had reasonable near and distance vision."
Is Laser's End in Sight?
Dr. Gelisken admits that thermal laser therapy for extrafoveal CNV is not very popular at the moment. "Nevertheless, this type of treatment is still the only one proven for treating extrafoveal CNV secondary to macular degeneration," he says. "Of course, the well-known limitations of thermal laser therapy in such eyes cannot be ignored."
There are other considerations that could influence laser's popularity. "Laser photocoagulation generates greater reimbursement than intravitreal injections, and it's less work for the doctor," notes Dr. Ciulla. "Nevertheless, I think more and more retina specialists are favoring retinal therapy."
"Unless something surprising comes from one of the current studies, I think the laser will be used less and less," says Dr. Ali. "Of course, I wouldn't get rid of my laser because I still use it for diabetes. But for macular degeneration, because of clinical efficacy and medico-legal considerations, you have to have an extremely good reason for doing anything other than anti-VEGF therapy these days. That's become the gold standard."
However, Dr. Ali concedes that it's still possible to make an argument for using the laser in some situations. "In the case of an extrafoveal problem, it may be a valid approach to attempt the laser; then, if the problem recurs, switch to an anti-VEGF injection," he says. "Perhaps you could use laser if a patient was hesitant to get the injection, and then you'd have the injection to fall back on. That may be a reasonable way to proceed."
Dr. Ciulla has received research grants from Genentech and Novartis. Dr. Ali has received financial compensation from Novartis for advisory board participation, travel and participation in clinical trials. Dr. Regillo has received research grant support from Genentech and Regeneron, and has done ad hoc consulting for Genentech.