Periocular spasms, which include myokymia, benign essential blepharospasm and hemifacial spasms, can often be difficult to diagnose because the signs and symptoms can be subtle. However, if the possibility of a periocular spasm is entertained, through thorough history gathering and a detailed examination, the diagnosis is readily reached.
Patients with periocular spasms often complain of difficulty opening their eyes or keeping their eyes open. Others may note increased blinking or intermittent spasms.
These spasms may be so severe as to limit a patient's functioning.
Spasms may be associated with other symptoms. These can include dry-eye symptoms such as foreign body sensation, grittiness or ocular pain. Patients also have photophobia and may note difficulty with fluorescent lighting or computer CRT screens.
These symptoms can precede the periocular spasms. Symptoms and spasms can progress and can be unilateral or bilateral. Patients with long-standing spasms can develop eyelid malpositions such as ptosis or entropion. Spasms can involve the midface (Meige's syndrome) or even become more generalized.
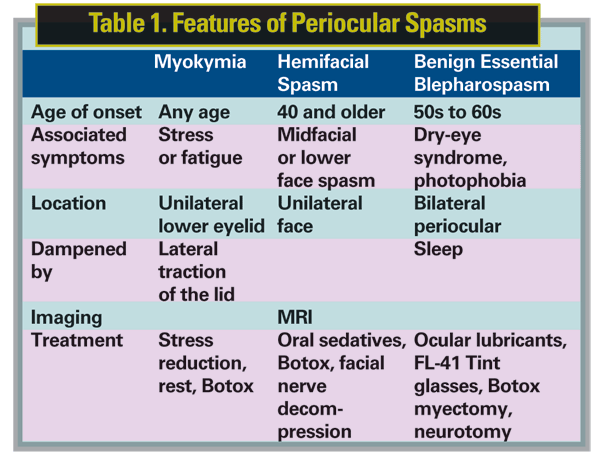
It is important to differentiate periocular spasms, if possible. Myokymia is twitching of one eyelid, usually associated with fatigue. Fine orbicularis twitching can often be observed. These can be dampened with lateral tugging on the eyelid. Patients typically do not have the associated dry-eye symptoms or photophobia. It is usually self-limited and resolves with rest.
Hemifacial spasm is a unilateral spasm of both upper and lower eyelids which also generalizes to the face. Patients complain of spasms of not only one eye, but also the midface and often the lip or mouth. These spasms do not cross the midline, by definition.
The spasms do not dampen with rest, and often can be witnessed while a patient is asleep. Hemifacial spasms can be associated with an anatomical compression of the facial nerve and therefore an MRI is warranted in the workup.
Benign essential blepharospasm is a bilateral periocular spasm. It has the associated symptoms of dry eyes and photophobia, as discussed earlier. Unlike hemifacial spasm, the symptoms do dampen with rest and often disappear during sleep. This disease is not related to an anatomic lesion and therefore imaging is not necessary.
Treatment first involves addressing the associated symptoms of dry eyes and photophobia. These symptoms are not just bothersome but can induce the spasms. For dry eyes, typical therapy includes aggressive ocular lubrication, punctal occlusion or topical cyclosporine A (Restasis). For photophobia, FL-41 rose-tinted glasses are very helpful in improving photophobia symptoms and dampening spasms.1
Treatments for the spasms include oral therapy, injectable therapy, and for severe cases, surgical intervention. Common oral medications and sedatives such as clonazepam are helpful in dampening the spasms. Therapy is started at a low dose and titrated until symptoms improve or side effects of sleepiness are not tolerable. Other medications used to treat neurologic diseases such as Parkinson's or seizures have been tried, with varying degrees of success.
Oral medications have been supplanted by injectable therapy, which is much more effective at treating spasms without the systemic side effects. The main injectable therapy is botulinum A therapy (Botox), in which the neurotoxin blocks the release of acetylcholine in the neuromuscular junction. This, in turn, causes muscle weakness/paralysis.
The botulinum toxin is injected into specific muscle areas to dampen or stop the spasms.2 Typical dosing involves injections into the pretarsal orbicularis of the upper and lower eyelids. Additional injections can be given to the forehead and midface to address additional muscle groups. Dosing is started low (2.5 to 5 units per injection site) and can be titrated up for effect. Treatments should last around three months.
Side effects from injections can include ptosis, if toxin is injected into the levator; dry eye, both from weakened closure of the eye and injection into the lacrimal gland; and double vision, if toxin gets to an extraocular muscle. In rare cases, patients can develop tolerance to the injection, associated with higher dosing and longer duration of therapy.
This is related to the development of antibodies to the toxin. If suspected, the presence of antibodies can be tested. Changing to botulinum toxin B is effective in these cases as an alternative to botulinum toxin A.
In cases where medical therapy is not effective, surgical therapy can be of benefit. This can include partial or complete excision of muscle groups (orbicularis), nerve decompression for hemifacial spasms or neurotomy for complete ablation of branches of the facial nerve.3 However, surgical therapy is not reversible and therefore is reserved for severe cases.
Dr. Bernardino is at the Yale School of Medicine, Department of Ophthalmology, Section of Ophthalmic Plastics and Orbital Surgery. Contact him at
1. Blackburn MK, Lamb RD, Digre KB, Smith AG, Warner JE, McClane RW, Nandedkar SD, Langeberg WJ, Holubkov R, Katz BJ. FL-41 tint improves blink frequency, light sensitivity, and functional limitations in patients with benign essential blepharospasm. Ophthalmology 2009;116:997-1001
2. Frueh BR, Felt DP, Wojno TH, Musch DC. Treatment of blepharospasm with botulinum toxin. A preliminary report. Arch Ophthalmol 1984;102:1464-8.
3. Bates AK, Halliday BL, Bailey CS, Collin JR, Bird AC. Surgical management of essential blepharospasm. Br J Ophthalmol 1991;75:487-90.



