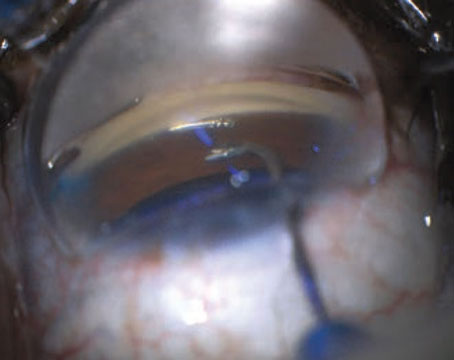
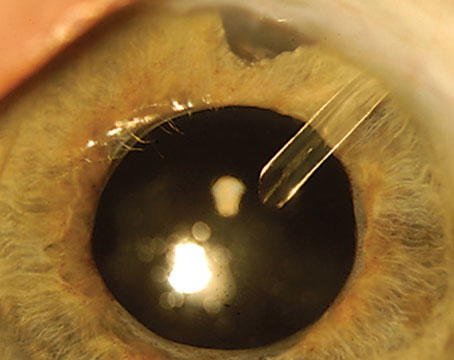
“The biggest issue in medical therapy is compliance,” says Michael Stiles, MD, in private practice in Overland Park, Kan. And, the need for frequent dosing with the currently available medications makes compliance challenging.
Some newer preservative-free and combination medications are already addressing the issues of compliance and safety, and some new drug delivery systems are in the pipeline that will hopefully take medication compliance completely out of patients’ hands.
Zioptan
Two concerns with glaucoma medications are their safety and tolerability, because patients will typically have to take them for the rest of their lives. Zioptan (tafluprost, Merck) was the first preservative-free prostaglandin approved by the Food and Drug Administration. It has been on the market for just over two years, and it has been shown to be as effective as the preserved prostaglandins.
A recent study found that treatment with once-daily preservative-free tafluprost was effective, well-tolerated and safe in treatment-naïve patients.1 The study included 579 treatment-naïve patients: 349 had primary open-angle glaucoma; 105 had ocular hypertension; 71 had normal-tension glaucoma; 27 had exfoliative glaucoma; and 27 had other glaucomas. At month three, significant reductions in mean IOP were seen in all patients. Preservative-free tafluprost lowered mean IOP significantly in patients with primary open-angle glaucoma and ocular hypertension who had IOP levels of 20 to 23 mmHg or higher from 21.9 ±1.1 mmHg at baseline to 16.5 ±2.2 mmHg. Overall, patients with higher baseline IOP values showed a better response than patients with lower baseline IOP levels. At three months, 97.9 percent of all patients remained on therapy.
Mildred Olivier, MD, in private practice in Hoffman Estates, Ill., notes that preservative-free prostaglandins are especially “great for younger people who will perhaps be on drops for a longer period of time, because preservatives can have damaging effects to the conjunctiva.”
Simbrinza
 |
The FDA approval is based on data from two pivotal Phase III trials that included approximately 1,300 patients.2,3 The studies evaluated the safety and efficacy of Simbrinza administered three times daily, compared to separate three-times-per-day dosing of one or the other component. Both studies met their primary endpoints and demonstrated that Simbrinza is statistically superior compared to either component regarding mean IOP at month three for all times points. In both studies, Simbrinza achieved a 5-mmHg to 9-mmHg reduction from baseline to month three. Patients’ mean IOP at baseline was 22 mmHg to 36 mmHg.
In the two, three-month clinical trials, the most frequently reported adverse reactions in patients treated with Simbrinza (occurring in approximately 3 to 5 percent of patients) were blurred vision, eye irritation, dysgeusia, dry mouth and eye allergy. Discontinuation of Simbrinza treatment (mainly due to adverse reaction) was reported in 11 percent of patients. The safety profile of the combination agent is comparable to each of the individual components.
“So far, my experience with Simbrinza has been very positive. I have had good results, and patients seem to tolerate it well. However, I have had difficulty with some insurance companies, because it is not always a well-covered medication,” says Richard Lehrer, MD, in private practice in Alliance, Ohio.
According to Dr. Olivier, compliance is much better with combination drugs. “However, my concern with any combination drug is that you’d like to know that each one of them works well for a patient before you commit her to two drugs. Additionally, combination drugs can be more costly to the patient. Our goal is to make the medications easier to take,” she says.
Rescula
Rescula (unoprostone isopropyl, CIBA) was first approved in 2000. While unoprostone was developed from a prostaglandin metabolite, it is considered to be a docosanoid, with different properties from those of prostaglandin analogs. The labeled dosing frequency was twice daily.
As once-daily true prostaglandin analogs entered the marketplace, Rescula disappeared from the U.S. market. In December 2012, the FDA approved a new drug application for Rescula, and it re-entered the market. It is now considered a docosanoid in the prostone family rather than a prostaglandin analog.
“I have found it to be effective in some patients,” Dr. Olivier says. “In fact, some patients have a surprising decrease in pressure. I like it because it doesn’t have many side effects. You do have to dose it twice a day, but just this week I had a patient whose pressure was the same after trying three different medications. They were just not working. I put her on Rescula, and it’s the only drop that reduced her pressure. I typically use it in people who have earlier forms of glaucoma, like ocular hypertensives. However, in these patients, I will typically try a once-a-day medication first. Then, if I have to go to a second drop and I already have to do twice a day, then Rescula is a drop that I will try. Or if I haven’t had any success with the prostaglandins as a first line, then I will try Rescula because the side effects are still fewer than the side effects of brimonidine, a topical beta-blocker, or a carbonic anhydrase inhibitor,” Dr. Olivier says.
New Classes & Delivery Systems
None of the currently available medications are ideal, so researchers are continuing to investigate new classes of drugs that look promising. For example, “A couple of companies are working on rho-kinase inhibitors, and results seem to be very positive,” Dr. Lehrer says. “Hopefully, they will be available very shortly and will be beneficial for our patients to improve outflow and lower pressures.”
Dr. Olivier agrees, noting that “Rho-kinase inhibitors offer new mechanisms of action with equivalent IOP reduction with a unique ability to lower pressures in the normal range.”
A Phase II study is currently underway to evaluate the ocular hypotensive efficacy of rho-kinase inhibitor (AR-12286 0.5% and 0.7%) ophthalmic solutions in patients diagnosed with exfoliation syndrome and ocular hypertension or open-angle glaucoma treated for six months.4 Primary data is scheduled to be available in September 2014.
The newest area of interest is evaluating new delivery systems that would take the responsibility for medication compliance away from patients. “The delivery systems are a very hot topic right now. There is quite a bit of research going on as far as drug delivery systems, such as subconjunctival injections and punctal plugs containing medication. These options would prevent patients from having to take their medications every day. There are quite a few companies developing these technologies, and they are currently in Phase II and III studies,” Dr. Lehrer says.
Dr. Stiles agrees, noting that researchers are also looking at medications that can be placed in a slow-release material that can be inserted in the fornix of the conjunctiva on the outside of the eye, or that’s implantable and can release medication in the sub-Tenon’s space. “There has been a lot of research done on those types of medications. This is medical therapy’s answer to try to maintain medical therapy as an effective way of treating glaucoma by eliminating the compliance issue,” he adds.
Drug delivery systems currently in clinical development include conjunctival, subconjunctival and intravitreal inserts, punctal plugs, and drug depots.
One example is a hybrid dendrimer hydrogel/poly(lactic-co-glycolic acid) nanoparticle platform that is being developed to deliver glaucoma therapeutics topically.5 It is designed to release the drug slowly, and it is compatible with many of the currently used glaucoma drugs.
Another example is a timolol maleate-loaded chitosan film that was recently found to be safe and efficient as an ocular drug delivery system in the treatment and prevention of glaucoma.6 Chitosan is a cationic polysaccharide biopolymer with mucoadhesive properties, and this study compared the efficacy and safety of chitosan-coated timolol maleate mucoadhesive film with the use of a 0.5% timolol maleate commercial ophthalmic solution in a rabbit model. Twice a day for 15 days, 0.5% timolol maleate commercial ophthalmic solution was administered in five eyes and was compared to chitosan-coated timolol maleate in five eyes. In the control group of five eyes, saline was used twice a day. The maximum timolol maleate release times from chitosan films were also recorded. The animals were sacrificed, and the right eyes of the rabbits in all three groups were removed for histologic analyses.
Timolol maleate was released from the film for four weeks, with 85 percent of the drug being released during the first two weeks. However, in vivo IOP levels were lowered over a 10-week period. No significant difference with regard to lowering IOP was seen between the eyes that received the commercial ophthalmic solution and the eyes that received the films. Additionally, no signs of ocular discomfort or irritation were seen on ophthalmic examination by slit-lamp biomicroscopy. No alterations in ophthalmic structures that came in direct contact with the films were observed in histopathological studies, and the rabbits showed no signs of ocular discomfort during the experimental assays.
Other alternatives used for extended drug release include particulate drug delivery systems or injectable formulations such as microspheres, liposomes and nanospheres/nanoparticles.7 The delivery includes trapping the drug in the nanocarrier matrix and delivering it into the eye. After administration, the bioactive agent is released in a controlled fashion by diffusion through the matrix or by degradation of the polymer matrix. Additionally, once the nanomicrocarriers are injected, they can act as a reservoir system for drug release for a prolonged time period.
Researchers have evaluated the release of timolol maleate from biodegradable microspheres. They are administered by subconjunctival injection, which is less invasive than intravitreal injection, and drug release has been sustained for more than three months.8
Liposomes are another polymeric particulate delivery system being studied for ocular drug delivery. For example, investigators have developed and studied brimonidine tartrate liposomes for their IOP-lowering effects in glaucoma. There was a constant delivery of therapeutics with a linear release profile.9 Additionally, after topical application, the IOP-lowering effect of the drug was sustained.
Recently, the IOP-lowering ability of a latanoprost-loaded liposome injected subconjunctivally in rabbit eyes was compared with conventional daily administration of latanoprost eye drops.10 The liposomes were well-tolerated, and sustained delivery was achieved for approximately 50 days. No adverse effects in ocular tissue were seen with subconjunctival injection, and the IOP-lowering effect was superior to latanoprost eye drop administration.
Other potential drug delivery systems include nonbiodegradable ocular devices that are already approved for intravitreal drug delivery in other ocular diseases and could be adapted for glaucoma management. Examples include Vitrasert, Retisert and Iluvien.
However, even with these new medications and delivery systems, surgical alternatives will still have a role. “There will be patients who fail medical therapy or don’t tolerate medical therapy and need to go on to surgery,” Dr. Lehrer says. “Every time a new drug gets approved, it bumps down our surgery practice because we try the new drug to see if it can keep patients out of surgery for a while. Sometimes this works, and sometimes it doesn’t. Right now, I don’t think there is a medication that will keep everyone out of surgery.” REVIEW
1. Lanzl I, Hamacher T, Rosbach K, et al. Preservative-free tafluprost in the treatment of naïve patients with glaucoma and ocular hypertension. Clin Ophthalmol 2013;7:901-910.
2. Katz G, DuBiner H, Samples J, et al. Three-month randomized trial of fixed-combination brinzolamide 1%/brimonidine 0.2% versus brinzolamide 1% versus brimonidine 0.2% in patients with open-angle glaucoma or ocular hypertension. Glaucoma. In press.
3. Nguyen QH, McMenemy MG, Realini T. Phase 3 randomized 3-month trial with an ongoing 3-month safety extension of fixed-combination brinzolamide 1%/brimonidine 0.2%. J Ocul Pharmacol Ther 2013;29(3):290-297.
4. Glaucoma Associates of New York. A prospective study to assess the hypotensive efficacy of Rho-kinase inhibitor AR-12286 ophthalmic solution 0.5% and 0.7% in patients with exfoliation syndrome and ocular hypertension glaucoma. Not yet published. http://clinicaltrials.gov/ct2/show/results/NCT01936389.
5. Yang H, Leffler CT. Hybrid dendrimer hydrogel/poly(lactic-co-glycolic acid) nanoparticle platform: An advanced vehicle for topical delivery of antiglaucoma drugs and a likely solution to improving compliance and adherence in glaucoma management. J Ocul Pharmacol Ther 2013;29(2):166-172.
6. Fulgencio GDE O, Viana FA, Ribeiro RR, Yoshida MI, Faraco AG, Cunha-Junior Ada S. New mucoadhesive chitosan film for ophthalmic drug delivery of timolol maleate: In vivo evaluation. J Ocul Pharmacol Ther 2012;28(4):350-358.
7. Manickavasagam D, Oyewumi MO. Critical assessment of implantable drug delivery devices in glaucoma management. J Drug Deliv 2013;2013:895013.
8. Bertram JP, Saluja SS, McKain J, Lavik EB. Sustained delivery of timolol maleate from poly(lactic-co-glycolic acid)/ poly(lactic acid) microspheres for over 3 months. J Microencapsul 2009;26(1):18-26.
9. Prabhu P, Kumar N, Dhondge G, et al. Preparation and evaluation of liposomes of brimonidine tartrate as an ocular drug delivery system. Int J Res Pharm Sci 2010;1(4):502-508.
10. Natarajan JV, Chattopadhyay S, Ang M, et al. Sustained release of an anti-glaucoma drug: Demonstration of efficacy of a liposomal formulation in the rabbit eye. PLoS ONE 2011;6(9)e24513.