In September 2006, the journal Cornea published the recommendations of a panel of 17 dry-eye experts who used the Delphi consensus method to establish guidelines for diagnosing and treating dry-eye syndrome.1 The panel, assembled by ophthalmologists at the Wilmer Eye Institute at Johns Hopkins University in Baltimore, chose the Delphi approach because it had already been successful in establishing diagnostic and/or treatment standards in connection with other complex medical problems such as cardiovascular disease.
Rather than relying primarily on current diagnostic tests, the panel recommended basing decisions mainly on patient signs and symptoms, including the presence or absence of lid margin disease and tear distribution anomalies, as well as on the severity of the disease as defined by multiple suggested criteria. Furthermore, the panel recommended the use of a new term for dry-eye disease—dysfunctional tear syndrome, or DTS—which they felt better represented the nature of the disease. The latter recommendation generated a minor controversy. (For a summary of the panel's recommendations, see chart below.)
Since then, other panels have added to and elaborated on the diagnosis and treatment recommendations of the Delphi panel, most notably the Dry Eye Workshop (DEWS) group.2 This panel followed many of the conventions established by the Delphi panel, adding additional criteria and more specific signs and symptoms for each of the Delphi panel's four levels of severity, and providing additional treatment recommendations.
In this article, surgeons discuss how the guidelines have impacted their practices, and what, if anything, they would like to see revised.
Changing the Way We Think
"The idea behind the guidelines was to get people to think about dry eye in the context of a framework, as opposed to simply prescribing tears," says Christopher J. Rapuano, MD, co-director of the cornea service and refractive surgery departments at Wills Eye Hospital, and professor of ophthalmology at Jefferson Medical College of Thomas Jefferson University in Philadelphia. "I don't agree with 100 percent of either the
Penny A. Asbell, MD, FASCS, MBA, professor of ophthalmology and director of cornea and refractive surgery at the Mount Sinai School of Medicine in
"What makes them significant is that they are a very public statement that 1) dry-eye disease is a real problem; 2) it can be differentiated according to severity; and 3) there are several different treatment options to consider," she continues. "By providing a framework for thinking about dry-eye disease, the guidelines will enable professionals to consider dry-eye disease in their differential diagnosis and then offer the best treatment options to their dry-eye patients.
"Cornea specialists like myself have been thinking about ocular surface disease and how to treat or prevent it for a long time," she observes. "But thanks in part to work like that done by the Delphi and DEWS panels, we are all now focusing more on the association between ocular surface disease and common ocular conditions, including the use of glaucoma drops that can cause irritation; changes in vision; how ocular surface disease will impact quality of vision; and how it may affect the outcome of refractive surgeries such as LASIK. The DEWS report, the Tear Film and Ocular Surface Society report and the 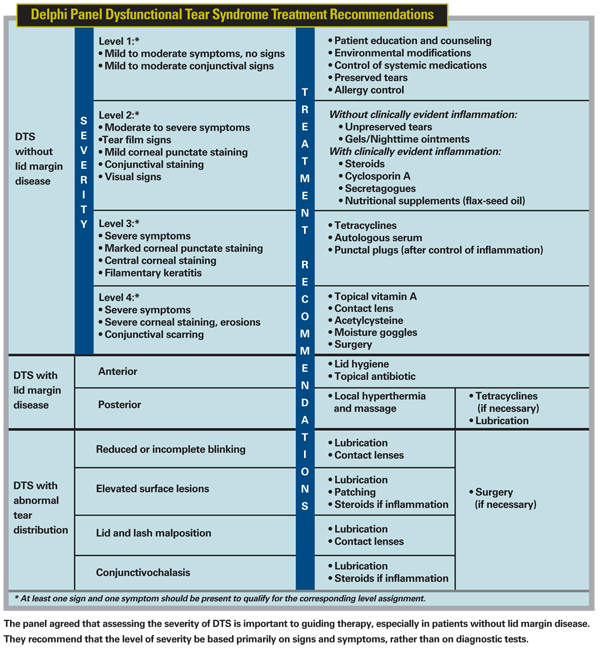
Steven E. Wilson, professor of ophthalmology and director of corneal research at the Cleveland Clinic's Cole Eye Institute, participated in the Delphi dry-eye panel; he also published a follow-up study evaluating the clinical implementation of the guidelines in 2007.3 "The Dry Eye Workshop guidelines that were published the following year are very similar, so I think it's been borne out that this is a rational approach to diagnosis and treatment of the disease," he notes. "In fact, I had been using a similar approach before we created the guidelines, but they certainly validated what I was doing."
A Guide for Diagnosis
"Dry eye can be difficult to diagnose, particularly in the early dry eye patient," notes Bruce Koffler, MD, director of the Koffler Vision Group in
Dr. Wilson agrees. "One of the benefits of the guidelines is that they provide an easily understandable approach that can be applied not only by corneal specialists but by comprehensive ophthalmologists and other doctors," he says. "I've had good feedback not only from people in the office but also residents and fellows who've trained with us.
"Also," he continues," a lot of the data that goes into making the diagnosis and treatment decision can be gathered by the clinic staff prior to the ophthalmologist seeing the patient. Today, we don't have as much time as we'd like with each patient; having the staff be able to help gather information makes it more likely that patients will get the appropriate care for their disease."
Steven C. Pflugfelder, MD, a professor and director of the Ocular Surface Center at the Cullen Eye Institute at Baylor College of Medicine in Houston, who participated in both the Delphi panel and subsequent DEWS panel, notes that one major difference between the Delphi and DEWS panel recommendations is that the Delphi panel divided dry eye into subcategories based on the presence or absence of meibomian gland disease. "The DEWS panel felt it was better to be all-inclusive because there's a lot of overlap between the conditions," he explains. "I agree, because many dry-eye patients, especially older patients, have a component of meibomian gland disease and it's hard to separate it from their other problems."
Dr. Rapuano observes that one helpful aspect of the guidelines is their emphasis on a variety of ways to make the diagnosis. "You shouldn't just rely on Schirmer testing or tear breakup time," he says.
Along those lines, Dr. Wilson notes that the guidelines do leave room for the doctor's judgment. "They don't specify all the things you have to do to diagnose a given patient," he says. "That's important because there's high variability in the tests that ophthalmologists choose to perform. For example, some doctors do a Schirmer's test in every patient. Others do it rarely and rely more on patient symptoms and staining."
A Guide for Treatment
Certainly a key aspect of the guidelines is their framework for choosing an appropriate treatment. "There are reasonable ways to grade this disease, and we have different treatment options depending on the grade," says Dr. Rapuano. "If a patient has moderate disease, maybe I should be considering the treatment I've been saving for the most severe disease. Or vice versa; maybe I've been putting everybody on steroids, and I should consider saving that for more serious cases. I believe cornea specialists were already using this kind of system, but the audience for the
"Of course, these guidelines aren't strict rules," he notes. "Patients will have different presentations and different desires. A patient may say, 'I can't afford Restasis; I want punctal plugs as the next step.' Just because punctal plugs come later in the guidelines doesn't mean you have to do Restasis first."
"I think guidelines with very focused recommendations are a good idea, especially for doctors who aren't dry-eye gurus," says Dr. Pflugfelder. "The guidelines make it easier to decide whether to add or subtract therapies based on the presence of irritation symptoms and a few simple tests you can do in your office.
"Patients notice the difference, too," he adds. "We get referred patients, many of whom haven't been using anything except artificial tears, when in fact they need therapeutic agents. I think they appreciate the fact that there are more options that can be offered to them based on their level of severity. Sometimes they're surprised they weren't offered these options sooner by their doctor, but many doctors aren't familiar with the guidelines; they may elect to refer the patient rather than take the time to become familiar with the guidelines themselves. In fact, the guidelines really aren't that complicated."
Dr. Koffler says he and his staff haven't tried to follow the guidelines strictly. "However, they help us to look at dry eye as a disease entity with multiple origins and multiple therapies which we can consider using based on severity levels," he notes. "Also, the severity levels help us to decide what treatment we're going to use next. I think we've followed that aspect of the guidelines fairly closely—maybe not with checkmarks on a list, but we plan our treatment regimen pretty much as suggested in the guidelines. I'd say the result is that we're giving better patient care."
Dr. Wilson believes that one of the most important treatment ideas reinforced by the guidelines is that cyclosporine is a valuable resource when used properly. "These guidelines go hand in hand with the new understanding that dry eye has an underlying inflammatory basis that leads to tissue dysfunction in the lacrimal glands and results in an inflammatory situation on the ocular surface," he says. "The guidelines help to drive home the idea that first of all, this is a disease, and second, in the majority of patients there is an inflammatory component that can be treated with anti-inflammatory medications such as cyclosporine, or treated transiently with corticosteroids, especially when you're initiating treatment in a patient with severe disease.
"I believe that at least in some patients, cyclosporine can halt the progression of the disease," he continues. "The guidelines point out that patients who are still early in the disease, at stage two, may really benefit from this treatment. If you're saving cyclosporine for the most severe patients you see in your practice, it's probably not going to work; at that point in the disease the eye may not have the capacity to respond. You really want to catch these people early in their disease course."
Dr. Asbell notes that the idea of staging disease, as recommended in the guidelines, is appropriate. "Classifying disease and using that classification to determine prognosis and treatment is the modern standard for all disease processes," she says. "Cancer is staged; surgeons use staging both to determine the best treatment and to help the patient understand the prognosis.
"We'd like to do the same for patients who have ocular surface disease," she continues. "Unfortunately, at this time we don't have a definite test or series of tests that will help us do this; the process is still very much in its infancy. We need more science, which is what I and many others are working on. One hundred years ago, people diagnosed anemia by looking at your nail bed and deciding whether you looked pale; today, we use blood tests to determine whether a patient is anemic, and then decide treatment and monitor the effectiveness of the treatment. In terms of dry-eye disease, we're still looking at nail beds. But guidelines like this, as described in the DEWS report and the
Spreading the Word
Everyone seems to agree that the guidelines won't need any further updates until new approaches to diagnosis or treatment become available. "The DEWS meetings were a pretty arduous process, so I don't see revisions happening in the near future," says Dr. Pflugfelder. "People need to use the guidelines for a while before any substantive changes are made."
What the surgeons we spoke to would like to see is further dissemination of the existing guidelines, as a means to improve treatment for dry-eye patients everywhere. "Unless you see the guidelines more than once, it's a little hard to grasp everything they contain," observes Dr. Koffler. "We need a little more education and promotion of the guidelines so they become more commonly used. Without that, I don't think they'll catch on."
Dr. Pflugfelder agrees. "It takes a while for guidelines to be adopted," he notes. "It will take coverage in publications and lectures and maybe getting into textbooks for people to really start embracing them. But I think it will happen."
1. Behrens A, Doyle JJ, et al. Dysfunctional tear syndrome: a
2. Dry Eye Workshop Panel. 2007 Report of the Dry Eye Workshop. Ocul Surf 2007;5:2:65-204.
3. Wilson SE, Stulting RD. Agreement of physician treatment practices with the international task force guidelines for diagnosis and treatment of dry eye disease. Cornea. 2007;26:3:284-9.