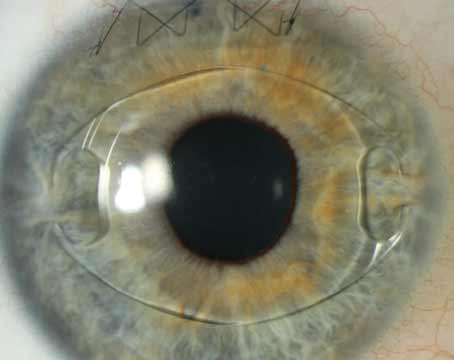
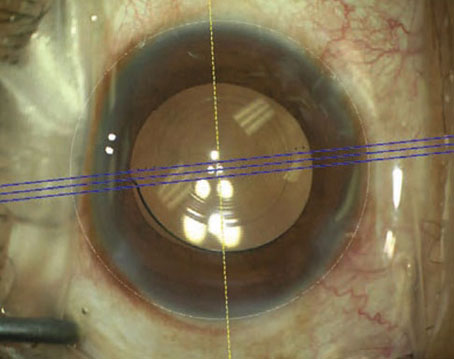
The European School for Advanced Studies in Ophthalmology recently conducted a study to inform surgeons about presbyopic IOLs.1 Vito Romano, MD, cornea specialist at University of Brescia, Italy, coordinated the study. “This study was planned because the multifocal IOL market isn’t equally distributed in Europe,” he says. “There are many more surgeons that can plant multifocal IOLs in Spain compared to all the other European countries.”
ESASO’s steering committee sectioned 105 items into four sections: preoperative; intraoperative; postoperative; and IOL selection. “[The committee] took 10 experts throughout Europe, put them all together, and did a Delphi consensus,” says Prof. Romano. “We chose the experts geographically with publication experience, and we asked them to review questions about complications, or complaints, when implanting a presbyopic IOL. We reached a consensus with about 70 percent of them.”
Preoperative considerations included 68 items, and consensus was achieved in 48 of them (70.6 percent). Consensus was reached in 10 out of the 14 intraoperative issues (71.9 percent) and in 10 out of the 13 postoperative considerations (76.9 percent).
Preoperatively, a patient’s age, habits, work type and motivations were all considered important when recommending a presbyopic IOL. Experts considered age as an important factor, but they didn’t determine an age-range for this study. Researchers noted that age should be balanced with other preoperative aspects, such as the patient’s ocular health.
The steering committee considered variables in the study related to preoperative contraindications. Out of the possible choices, four were agreed upon as contraindications: previous uveitis; previous squint (strabismus) surgery; epiretinal membrane; and previous ocular surgery. There wasn’t an agreement on whether these represented an absolute or relative contraindication.
The experts agreed that the potential postoperative visual acuity is crucial in deciding the type of presbyopic IOL. They noted that patients with a potential postop corrected distance visual acuity less than 0.5 (20/40 Snellen) should consider extended-depth-of-focus IOLs or non-diffractive IOL designs. Those expected to emerge postop with better than 0.5 may benefit from a multifocal lens.
Recommending presbyopic IOLs achieved consensus in categories of refraction, keratometry and IOL power, but axial length saw discrepancy among the panel. Keratometry between 40 to 45 D and IOL power between 10 and 27 D were considered most suitable for a presbyopic IOL. Researchers suggest any eyes outside these diopter ranges should be managed with caution. Despite axial length discrepancies, agreement on IOL power reveals that short and long eyes should be managed with care.
Pupil size was also considered important, with both small and large pupils potentially causing more risks. Accordingly, the panel of experts agreed that an optimal range of pupil diameter for presbyopic IOLs is larger than 2.8 mm under photopic conditions and smaller than 6 mm under scotopic conditions.
Seven preoperative tests to reduce postoperative complications were agreed upon, including corneal topography and tomography, static pupillometry, biometry/biometry formula, optical coherence tomography for assessment of the retinal nerve fiber layer and macula.
During the study, researchers observed a lack of consensus for IOL selection, and the experts couldn’t agree upon parameters for choosing IOL characteristics. However, consensus was reached on the importance of patient habits for optic design selection. “I think the reason IOL selection didn’t reach a consensus was because it’s difficult to find a surgeon that utilizes all the different kinds of lenses, all the different types of material and optic designs,” says Prof. Romano.
Prof. Romano notes that this study merely provides recommended guidelines for ophthalmic surgeons. “The aim was to give guidance to young surgeons and to deliver [information] in an unbiased way,” he says. “[The experts] never talked about brands. They never talked about lenses that were better than others, but rather their recommendations to let young surgeons, or surgeons who aren’t cornea/refractive experts, a chance to learn about these lenses.”
Romano V, Madrid-Costa D, Alfonso JF, et al. Recommendation for presbyopia-correcting intraocular lenses: A Delphi consensus statement by the ESASO study group. Am J Ophthalmol. May 24, 2023. [Epub ahead of print].
Isotretinoin and Tear Dysfunction
Isotretinoin was found to alter meibomian gland morphology, causing lipid abnormalities.1
Known by its brand name Accutane, isotretinoin is the most effective treatment for refractory acne vulgaris cases. The oral medication travels through the bloodstream, affecting oil glands and reducing sebum production all over the body, including in the face and eyelids. Dry eye and meibomian gland dysfunction with isotretinoin use have both been reported in the literature.
To better characterize the drug’s ocular side effects, researchers in Poland conducted a study of individuals with an acne vulgaris diagnosis. As a result of their research, they reported increased ocular complaints from the study patients and reversible changes in meibomian glands.
The study included 48 eyes of 24 patients with acne vulgaris. Each patient underwent an ophthalmic exam before initiating isotretinoin therapy, three months after the start of treatment and one month after completion of the treatment.
The researchers reported significant increases in Ocular Surface Disease Index score during and after treatment compared with pretreatment values. During treatment with isotretinoin, there was substantial meibomian gland loss and decreases in meibum quality score and lid margin abnormality score. These measures improved once treatment was stopped.
Additionally, the authors reported that the frequency of artificial tear use was positively associated with meibomian gland loss during and after treatment. They also noted in their paper that meibomian gland atrophy was significantly correlated with meibum quality scores during and after treatment. During isotretinoin treatment, decreased tear breakup time values correlated with an increase in lid margin abnormality score. Schirmer’s test scores and blink rates seemed unaffected by the treatment.
“Systemic therapy with a retinoid derivative is an independent risk factor for dysfunction and atrophy of the meibomian glands in patients with acne vulgaris,” the researchers concluded in their paper. “Interestingly, the statistical analysis carried out in the follow-up study unambiguously showed that the side effects induced by isotretinoin started to subside.” The investigators added that further study into this occurrence will hopefully shed light on the mechanism for meibomian gland regeneration to help patients suffering from meibomian gland dysfunction.
1. Zakrzewska A, Wiacek MP, Słuczanowska-Głabowska S, et al. The effect of oral isotretinoin therapy on meibomian gland characteristics in patients with acne vulgaris. Ophthalmol Ther. June 10, 2023. [Epub ahead of print].