|
Our eyes construct and maintain a functional tear film by orchestrating a complex balance between lacrimation, mucin and meibum production and secretion and, of course, by blinking. When the tear film is challenged, that balance is modified to adapt and compensate in an effort to protect the ocular surface and maintain proper visual function. Tear production may increase, blink behavior may change, and even the palpebral fissure dimensions adapt in compensatory response to factors that promote ocular drying. And while most of these responses occur naturally, patient input combined with careful observation can provide vital clues to understanding the underlying cause (or causes) for pathological drying of the ocular surface.
In recent columns we’ve discussed developments in dry-eye therapies and dry-eye diagnostics. This time, we’ll complete the picture of dry-eye disease by exploring the dynamics of different compensatory mechanisms. By understanding how and why our patients compensate for an insufficient tear film, we’re in a better position to make more accurate diagnoses and adopt the best, most individualized approach to treat our patients’ dry eye.
Zeroing in on Blink
While the interaction between the lids and the tear film helps to define the integrity of the ocular surface, the importance of blink and its role in dry-eye pathology is often underappreciated.
Each blink facilitates the drainage of tears, excretion of lipids from the meibomian glands, spreading of lipids across the corneal surface and elimination of debris from the tear film.2 Blinks can be complete or incomplete, and blink rate can vary significantly, both between patients and for individuals at different times. The variations in blink behavior generally occur autonomously, so patients are unlikely to be able to provide useful information on their blink behavior. Despite this, blink dynamics have been, and continue to be, a central part of dry-eye diagnosis.
|
From the ability to measure the stability of the tear film with the advent of tear-film breakup time by Michael Lemp, MD, in the 1970s3 to the development of the Ocular Protection Index,4 evaluations for dry eye have steadily improved. Studies at Ora Inc., have led to the development of the OPI 2.0 System, which provides a real-time measurement of tear-film stability via an automated analysis system. The simultaneous capture of interblink interval and TFBUT, in addition to a measure of tear-film breakup area, allows for a more comprehensive evaluation of ocular surface protection under a natural blink pattern and normal visual conditions.5 Custom blink pattern recognition software has also been developed to track both blink type and IBI using a high definition video camera and computer analysis system.6 This software tracks the upper and lower lid to compute data on blink frequency and magnitude over time while the subject performs a controlled visual task. By tracking the movement of critical points along the lid margin, the automated blink capture program can successfully track the extent of lid movement to better characterize blink patterns. These new technologies are valuable for patient characterization and selection in clinical trials, and provide the basis for new metrics (such as breakup area) that we hope will make it to the ophthalmologist’s clinic in the near future. They also provide the tools for a more comprehensive analysis of tear-film dynamics such as tear-film breakup patterns.
The combination of basic science and clinical observation has established the importance of blink properties in a patients’ dry-eye diagnosis, but the blink is also a key factor in related diseases such as meibomian gland dysfunction. As discussed earlier, the mechanical activity of blinking distributes the meibomian glands’ lipids over the ocular surface and, in doing so, provides a key component of the tear film. However, when a patient has a lower blink rate than normal, her meibum distribution may be impaired. A recent single-center study used variations in blink as a diagnostic tool, separating 14 subjects into two groups: normals and patients with MGD. They then differentiated the groups by blink patterns. (Welch D, et al. IOVS 2011;52:ARVO E-Abstract 946) The proportion of full blinks was significantly greater in MGD subjects than normals (p=0.044). This finding suggests that MGD patients may alter their own blink patterns by including more complete and squeeze blinks in order to aid in their deficiency of meibum secretions.
Custom Compensation
Research surrounding the properties of blinking and differing blink patterns has highlighted the importance of this mechanism for better understanding dry eye. A link between blink pattern and blink rate has been established, where subjects with mild to moderate dry eye tend to have shorter interblink intervals and a higher proportion of full blinks compared to partial blinks than normal subjects. (White R, et al. IOVS 2010;51:E-Abstract 3366) These findings are consistent with other research demonstrating that normal patients tend to have a spontaneous incomplete blink ratio of 75 percent or more.6 Because of the higher proportion of full blinks in dry-eye subjects and the increase in the number of partial blinks in normal subjects without dry eye, some experts have theorized that normal subjects utilize partial blinks to better support their visual function by limiting the interference of constant and obstructive full blinks with the visual axis.7
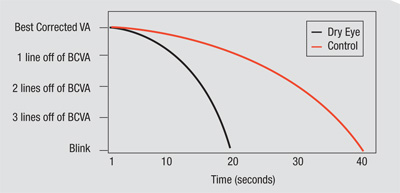
Clinical experience has shown that while normal individuals typically demonstrate an improvement in visual function from morning to evening, individuals with dry eye actually exhibit the opposite phenomenon. Individuals suffering from dry eye experience significant diurnal variations in their visual function and in the signs and symptoms of their condition. Many dry-eye patients complain of blurriness when performing everyday activities such as reading, watching television or driving at night. Because the severity of dry-eye signs and symptoms may relate to a patient’s interblink visual acuity, the disruption of visual function and ocular surface stability caused by dry eye can be quantified by the interblink interval visual acuity decay test, also known as IVAD. The impact of dry eye on quality of life is often substantial, as best-corrected acuity decreases in the evening.7 These findings may account for the visual disturbances reported by dry-eye patients and implicates visual function as a crucial component of dry eye.
When taken together, these results provide a compelling case for viewing blink pattern alterations as a compensatory mechanism in dry-eye subjects. The tracking of spontaneous blink activity can give the clinician valuable information about the clinical state of a dry-eye patient, as changes in blinking behavior occur in response to myriad factors that may indicate a disease, a diagnosis or even a state of mind.
|
Another study demonstrated that blink duration decreased significantly when comparing blinks immediately before and after one of these micro-sleeps, thus representing a beneficial effect on the fatigue state of a subject.10 This observation provides evidence for the beneficial effect of these ultra-short naps on the patient’s level of fatigue.
Seizing on this phenomenon, the auto maker Mercedes-Benz developed a novel safety tool in its cars with an attention-assist driver drowsiness monitor to keep drivers from engaging in micro-sleep.11 As most studies estimate that between 10 and 20 percent of serious traffic accidents are attributed to drowsiness, their system is an innovative safety tool, utilizing parameters such as blink duration, delay of lid reopening and IBI in order to monitor drivers’ drowsiness to protect them from accidents. The method used by Mercedes-Benz to determine a driver’s eye blink frequency consists of an infrared camera that is aimed at the driver’s head. This camera constantly monitors the driver’s interblink interval, enabling the rapid detection of micro-sleep the instant the person’s eyes stay closed for a certain predetermined period of time. When micro-sleep is detected, the car then attempts to warn the driver with an audible alarm signal as well as a flashing text warning on the dashboard’s instrument cluster.
The evaluation of micro-sleeps in fatigue studies prompted ophthalmic researchers to question whether similar blinking mechanisms may help relieve ocular stress in dry-eye patients, as well. While dry-eye subjects may try to compensate for an insufficient tear film with a series of rapid blinks, inordinately high levels of blinking can also interfere with a patient’s ability to successfully complete an ongoing visual task.12
When dry eye interferes with the ability to complete routine visual tasks, examining patients’ blinks to determine whether they are compensating or not is of the utmost importance. In a study presented at the 2012 Tear Film and Ocular Surface Society’s Asia meeting by the staff of Ora Inc., researchers investigated the possible beneficial effect of a micro-sleep by comparing the ratio of the length of the IBI immediately preceding the micro-sleep to the length of the IBI immediately following it (a value that was termed the IBI ratio). The results of this analysis demonstrated that median IBI ratios at a micro-sleep increased by 50 percent in dry-eye patients and 20 percent in normal patients. Dry-eye subjects also exhibited longer lid duration contact time than normal subjects, which had a lengthening effect on the subsequent IBI value.
Through a combination of changing blink rates, blink patterns and blink strength we are in a constant process of tear-film compensation. The relative ease of tracking blink behavior allows for a more efficient analysis of these blink patterns and has begun to realize their potential as a quantifiable mechanism of compensation in dry-eye patients. From such reliable, objective metrics come more accurate diagnoses, new therapies and improved patient outcomes. REVIEW
Dr. Abelson is a clinical professor of ophthalmology at Harvard Medical School and senior clinical scientist at the Schepens Eye Research Institute.
1. Nichols KK, Nichols JJ, Mitchell GL. The lack of association between signs and symptoms in patients with dry eye disease. Cornea 2004;23:8:762-770.
2. Holly FJ. Formation and rupture of the tear film. Exp Eye Res 1973;15:5:515-525.
3. Holly FJ, Lemp MA. Tear physiology and dry eyes. Surv Ophthalmol 1977;22:2:69-87.
4. Ousler GW, 3rd, Hagberg KW, Schindelar M, Welch D, Abelson MB. The Ocular Protection Index. Cornea 2008;27:5:509-513.
5. Abelson R LK, Rodriguez J, Johnston P, Angjeli E, Ousler G, Montgomery D. Validation and verification of the OPI 2.0 System. Clin Opthalmol 2012, 6.
6. Doane MG. Interactions of eyelids and tears in corneal wetting and the dynamics of the normal human eyeblink. Am J Ophthalmol 1980;89:4:507-516.
7. Walker PM, Lane KJ, Ousler GW, 3rd, Abelson MB. Diurnal variation of visual function and the signs and symptoms of dry eye. Cornea 2010 ;29:6:607-612.
8. Luckiesh M, Moss F. The science of seeing. New York: Van Nostrand, 1937.
9. Luckiesh M, Moss F. Reading as a visual task. New York: Van Nostrand, 1942.
10. Schleicher R, Galley N, Briest S, Galley L. Blinks and saccades as indicators of fatigue in sleepiness warnings: looking tired? Ergonomics 2008;51:7:982-1010.
11. Umbehr J. Mercedes develops anti-microsleep system. http://medgadget.com/2006/11/mercedes_develo_1.html. Accessed August 4, 2011.
12. Stern JA, Boyer D, Schroeder D. Blink rate: A possible measure of fatigue. Hum Factors 1994;36:2:285-297.