Presentation
A 55-year-old Hispanic male presented to the Wills Eye Institute’s Oculoplastic and Orbital Surgery Service for a second opinion regarding bilateral lower lid swelling, “bulging” eyes and diplopia. Two years prior, he had been diagnosed with thyroid eye disease (TED) by an outside ophthalmologist and treated with a six-month course of oral prednisone. Initial thyroid function tests were within normal limits. While tapering the oral corticosteroids over the ensuing 18 months, the patient experienced a flare of symptoms. When orbital radiation therapy was recommended, the patient elected to seek a second opinion from the Wills Eye Institute.
Medical History
Past medical history was significant only for borderline diabetes and allergic rhinitis. Family history was significant for diabetes and thyroid disease. The patient was a lifelong nonsmoker, but did consume a moderate amount of alcohol. Medications included cetirizine and aspirin. Review of systems was otherwise negative.
|
Examination
Ocular examination revealed an uncorrected visual acuity of 20/40 in each eye. Pupils were equal, reactive and without a relative afferent pupillary defect. Ishihara color plates were 8/8 briskly in each eye. Intraocular pressure measured with applanation tonometry was 24 mmHg in each eye, increasing to 36 mmHg in upgaze.
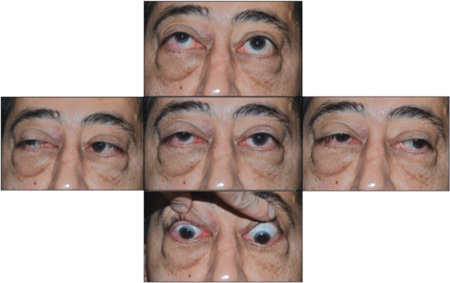
Bilateral lower lid festooning was present but there was no obvious upper lid retraction. He displayed bilateral lagophthalmos and inferior chemosis. Resistance to retropulsion was increased, more so on the right side. Hertel exophthalmometry confirmed symmetric proptosis of 29 mm bilaterally measured with a base of 96 mm. A right hypertropia was present in primary gaze with restricted extraocular motility bilaterally (See Figure 1).
Dilated funduscopic examination showed anomalous discs but no evidence of disc edema, venous congestion or chorioretinal folds. Automated perimetry was normal on both sides.
What is your differential diagnosis? What further workup would you pursue?