Presentation
A 44-year-old Caucasian female presented to the Wills Eye Emergency Room complaining of sudden onset of seeing a “thousand shades of gray, which later turned to black patches” in her right eye associated with pain with eye movement and dull headache. Her symptoms began 10 days prior and were progressively worsening.
Review of systems was notable for fevers, chills, night sweats, a recent intentional 90-pound weight loss, tinnitus, nausea and vomiting. She denied any muscle, joint, dermatologic or genitourinary complaints currently or in the past.
Medical History
She was diagnosed with multiple sclerosis 20 years prior, after having three episodes of “visual disturbances” in her right eye, presumably repeat bouts of optic neuritis. After being treated with glatiramer acetate, discontinued 18 years ago, she denied any new visual complaints. The remainder of her past medical history was remarkable for hypertension, controlled with verapamil and clonidine.
The patient worked as a nurse, without history of needle sticks or use of intravenous drugs. She was a non-smoker and denied any recent travel outside the Philadelphia area or having pets.
Two months prior she underwent a non-emergent laporoscopic cholecystectomy with a complicated postoperative course, resulting in an extended admission. Since then, she states she just has not “felt right.”
|
Vital signs were normal with a blood pressure of 126/82. Visual acuity uncorrected was 20/200 in her right eye with no improvement with pinhole and 20/20 in her left eye. Pupils were significant for a relative afferent pupillary defect in the right eye. The patient was able to identify only the test plate in the right eye and 10/10 color plates in the left eye. Confrontation visual fields and ocular motility were normal in both eyes. Intraocular pressure was 19 mmHg and 16 mmHg in the right and left eyes, respectively.
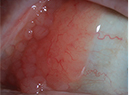
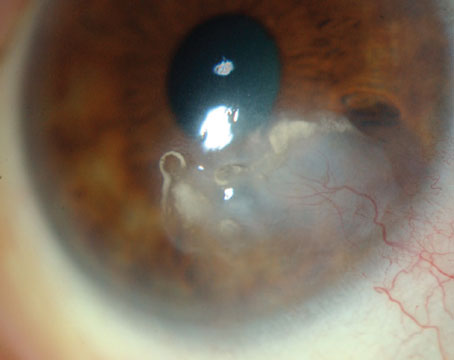
The anterior segment examination of her right eye revealed diffuse flat conjunctival injection, fine keratic precipitates inferiorly, 1+ white blood cells in the anterior chamber, and 2+ WBC in the anterior vitreous. There were no posterior synechiae, iris nodules or visually significant cataract. The left eye anterior segment examination was unremarkable with no signs of ocular inflammation.
The posterior exam of the right eye revealed significant vitreous cell, disc edema, peripapillary hemorrhages and cotton wool spots, an occlusive arteritis along all four vascular arcades and macular edema (See Figure 1). The veins were slightly engorged but did not show any inflammatory changes. Dilated funduscopic exam of the left eye was normal without evidence of prior inflammatory episodes.
What is your differential diagnosis? What further workup would you pursue?