Presentation
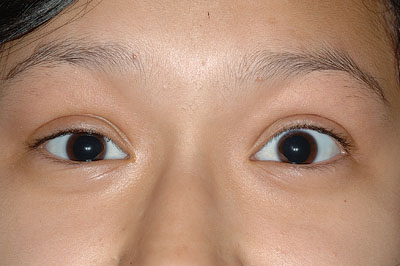
An 11-year-old Hispanic female presented to the Ocular Oncology Service at Wills Eye Institute for evaluation of a right upper eyelid (RUL) mass. The patient initially complained of three weeks of RUL swelling associated with lateral eyelid pain and erythema (See Figure 1).
Her symptoms resolved following a single dose of 80 mg of oral prednisone and a 10-day course of amoxicillin/clavulanate prescribed by her primary ophthalmologist. Nine months later, her RUL swelling recurred. At the same time, the patient was hospitalized for a new-onset asthma exacerbation following one week of intermittent itching and epistaxis. While admitted, the patient had an elevated platelet count but otherwise normal complete blood count, including white blood cell differential, erythrocyte sedimentation rate (32 mm/hr), C-reactive protein (0.8 mg/L), and basic metabolic panel. The patient was discharged and treated with a seven-day course of 60 mg of oral prednisone daily followed by a four-day course of 80 mg of oral prednisone daily. The patient was referred to Wills Eye Institute for further evaluation, as there was no improvement in her symptoms.
|
Medical History
The patient’s past medical history was unremarkable except for seasonal allergies. The patient was not taking systemic medications prior to admission. Her social history was noteworthy for one-month trips to Mexico every year.
Examination
Visual acuity was 20/40 in both eyes without correction, improving to 20/25 in both eyes with pinhole correction. Pupils were equal and reactive without a relative afferent pupillary defect. Extraocular motility and visual fields were full and intraocular pressures were within normal limits. The patient identified nine of nine color plates in both eyes, and exophthalmometry revealed no proptosis. Dilated fundoscopy was within normal limits bilaterally.
What is your differential diagnosis? What further workup would you pursue?