Presentation
A 9-month-old female infant presented to the Wills Eye Pediatric Service with a history of a darker right iris for several months and tear-drop shaped pupil for the past 10 days. Photographs provided by the parents verified normal-appearing pupils two months prior to presentation. There was no known trauma; however, the child had recently started cruising.
Medical History
The patient was born after a full-term gestation via spontaneous, uncomplicated vaginal delivery. She had no medical problems and no prior ocular history. She had been meeting all developmental milestones. There was no relevant family history.
Examination
The visual acuity was central, steady and not maintained in the right eye; and the left eye was central, steady and maintained. The eyes were well-aligned, and ocular motility was full. Intraocular pressure of both eyes was normal by finger tension testing. Anterior segment examination revealed corectopia of the right pupil, peaking at 12 o’clock. There was no relative afferent pupillary defect. Anterior segment examination of the left eye was unremarkable.
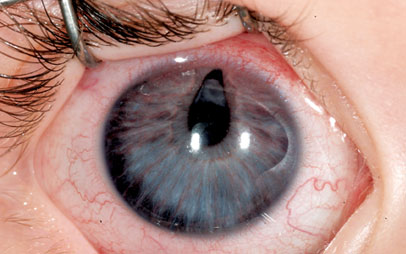
Handheld slit lamp examination confirmed corectopia with ectropion uveae at 12 o’clock. There was florid neovascularization of the right iris (See Figure 1). There was no ectopia lentis, and there was a grayish opacity posterior to the iris superiorly. During this first office visit, it could not be determined whether this opacity represented a cataract or mass. Dilated fundus exam of both eyes was within normal limits. Cycloplegic refraction revealed symmetric mild hyperopia.
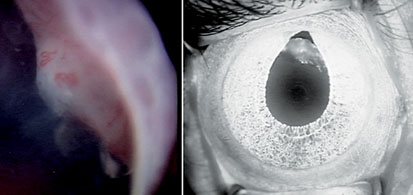
Because handheld slit lamp examination was limited on this 9-month-old child, an examination under anesthesia was performed. This confirmed the presence of a ciliary body mass in the right eye (See Figure 2). The mass extended from 9 o’clock to 3 o’clock and was 3.1 mm thick. IOPs were 18 mmHg OU. An anterior segment intravenous fluorescein angiogram confirmed 360-degree neovascularization of the iris, and the mass was hyperfluorescent. Ultrasound biomicroscopy revealed multiple cysts within the mass. Fine needle aspirate biopsy was performed. While under anesthesia, 0.05 ml of bevacizumab was injected into the anterior chamber to prevent neovascular glaucoma.
|
What is your differential diagnosis? What further workup would you pursue?