|
A 51-year-old white male presented to the Wills Eye Hospital Emergency Room with a chief complaint of a five-day history of a worsening, migrating blind spot in his right eye. It started in the upper right corner of his vision and then migrated centrally. He had similar visual disturbances in the left eye approximately one month prior, which improved with eye rubbing.
The patient denied redness, pain or diplopia. Review of systems was notable for a chronic cough and intermittent headache. He denied any fever, chills, meningitis-like symptoms or rash.
Medical History
Past medical history was significant for arthritis, hepatitis, HIV for the past 23 years and a many pack-year history of smoking. His only chronic medication was HAART medication Complera. After the initiation of the Complera a few months prior, his CD4 had decreased to less than 160 cells/mm3 but was steadily climbing. He had never been on any prophylactic antivirals or antibiotics. Family history was noncontributory.
Examination
Vital signs were stable and within normal limits. Visual acuity was 20/200 in the right eye and 20/20 in the left eye. Color vision was full in the left eye, but the patient could not see the test plate with the right eye. Pupils were equal and reactive without an afferent pupillary defect. Extraocular motility was full, and intraocular pressure was normal in both eyes. Visual fields were diffusely depressed and the patient could not see an Amsler grid. Both tests were normal in the left eye.
| ||||||
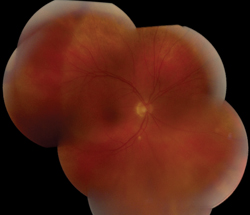
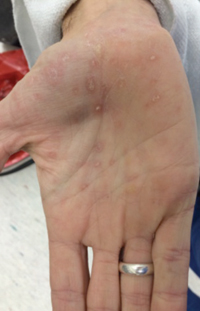
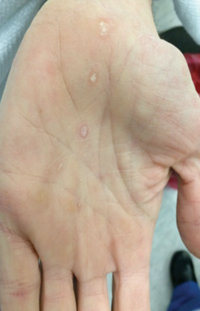
External exam was normal without any mass, ptosis or proptosis. Anterior segment exam was only remarkable for anterior chamber and vitreous cell in both eyes. Funduscopic exam was significant for a large, pale-yellow placoid lesion involving the macula and posterior pole in both eyes and a discrete, yellow-white lesion near the optic disc in the right (See Figure 1). A maculopapular rash was also noted on the patient’s hands (See Figure 2).
Please click this link for diagnosis, workup, treatment and discussion.