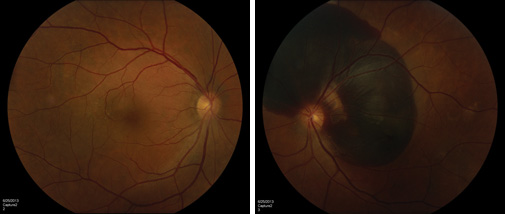
A 59-year-old Cambodian male presented to the Wills Eye Emergency Department with a one-day history of vision loss in the left eye. The patient stated he previously had equal vision in both eyes and awoke with significantly decreased vision in the left eye on the day of presentation. He denied any history of trauma, straining, coughing, lifting, pain, headache or neurologic symptoms.
Medical History
The patient’s past ocular history was only significant for mild cataracts in both eyes. His past medical history was significant for hypertension. His medications included amlodipine, indapamide, low-dose aspirin and fish oil supplements. Allergies included shellfish derivatives. He denied any recent travel and had no pets at home. Social history was negative for tobacco, alcohol or drug use.
Examination
The patient’s corrected visual acuity was 20/25 in the right eye and count fingers in the left without improvement on pinhole. Pupils were normal without afferent pupillary defect. Confrontational visual fields were full to finger counting in both eyes. Amsler grid testing revealed a significant central scotoma in the left eye. Motility was full in both eyes. There was no proptosis. Intraocular pressure was within normal range and equal in both eyes. Nuclear sclerotic changes were present. His funduscopic exam was significant for some macular retinal pigment epithelium changes in the right eye consistent with a pigment epithelium detachment. A large subretinal hemorrhage involving the macula and peripapillary region without peripheral pathology was noted in the left eye (See Figure 1). Blood pressure was 130/70. Neurologic exam was unremarkable without weakness, paresthesias, loss of reflexes or ataxia.
|
Please click this link for diagnosis, workup, treatment and discussion.