
Presentation
A 39-year-old Hispanic woman presented to the Wills Eye Emergency Room complaining of blurred vision in both eyes for the previous week. She had been experiencing transient visual blackouts in both eyes intermittently throughout the day, but this was not associated with body position or head movement. She also reported mild pain with eye movement. One day prior to presentation, she also had begun experiencing mild ringing in both ears without hearing loss and a mild bifrontal headache that had not improved with acetaminophen.
Medical History
She denied any past ocular history. She also denied past medical history, medication use, smoking, alcohol use or illicit drug use. She recently had bought a new cat but denied any cat scratches or bites. Review of systems was positive for occasional fingertip numbness of both hands. She denied any recent weight gain or loss, trauma or other recent illness.
Examination
On examination in the Wills Eye Emergency Department her visual acuity was 20/50 OD and 20/100 OS. Her pupils were round, equal, briskly reactive and without a relative afferent pupillary defect. Extraocular motility and confrontational visual fields were full in both eyes. Intraocular pressures were 14 mmHg OU. Slit-lamp exam of the right eye was normal. Examination of the left eye was significant for trace conjunctival injection and trace white blood cells in the anterior vitreous. Dilated funduscopic exam of both eyes revealed optic disc edema, retinal striae and subretinal fluid (See Figures 1A and 1B).
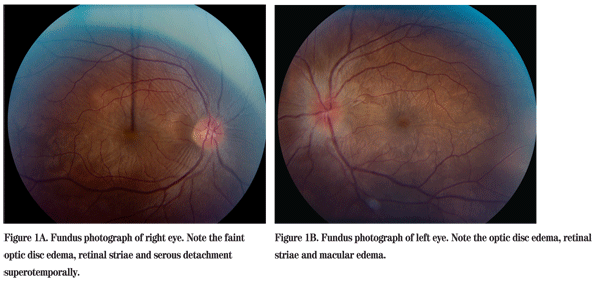
Diagnosis, Workup and Treatment
The differential diagnosis in this patient with exudative retinal detachments includes Vogt-Koyanagi-Harada syndrome, posterior scleritis, sympathetic ophthalmia (unlikely, as no history of penetrating injury or ocular surgery), hypertensive retinopathy (unlikely, as normal blood pressure), lyme, tuberculosis, syphilis and lupus choroidopathy.
Due to the bilateral optic disc edema and new onset headache, an MRI was ordered in the ER, which was normal. The patient was referred to the Wills Eye Institute retina service for further evaluation and management. Fluorescein angiography showed hyperfluorescence of the optic disc, and pinpoint and placoid areas of hyperfluorescence scattered throughout the posterior pole of both eyes (See Figures 2A and 2B). Optical coherence tomography (Stratus, Zeiss 4.0) showed serous detachments in both eyes with an intact retinal pigment epithelium (See Figures 3A and 3B). A uveitis/scleritis workup for syphilis, lyme, tuberculosis, toxoplasmosis and sarcoidosis was negative.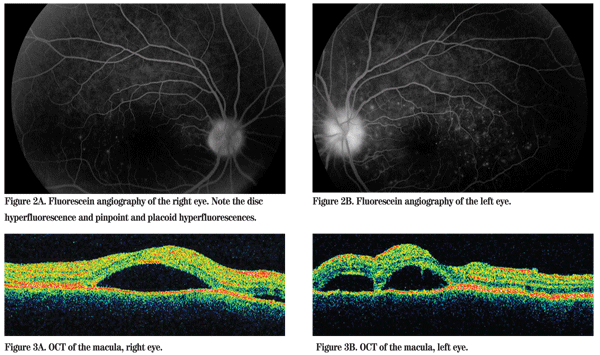
Based on the clinical presentation, and supported by an unremarkable medical workup, the patient was diagnosed with Vogt-Koyanagi-Harada syndrome. The patient was started on 60 mg of oral prednisone daily. Two weeks after starting treatment, she had less optic disc edema and subretinal fluid in both eyes (See Figures 4A and 4B). Three months after presentation, her vision was 20/25 in the right eye and 20/30 in the left eye, the headache and tinnitus had resolved, and the subretinal fluid had resolved. She is maintained on low dose oral prednisone and methotrexate.
Discussion
Vogt-Koyanagi-Harada syndrome is a chronic, bilateral granulomatous panuveitis with exudative serous retinal detachments and skin and central nervous system involvement. It was initially described in the early 1900s. VKH is more common in women and individuals with darker skin pigmentation such as Asians, Native Americans, Hispanics, Asian Indians and persons of Middle Eastern extraction. However, it is important to note that VKH is distinctly less common in persons of African decent, suggesting that the development of VKH is more related to genetics than degree of skin pigmentation. VKH occurs most commonly in people between the age of 20 and 50, though it has occurred in children as young as 4 years old. 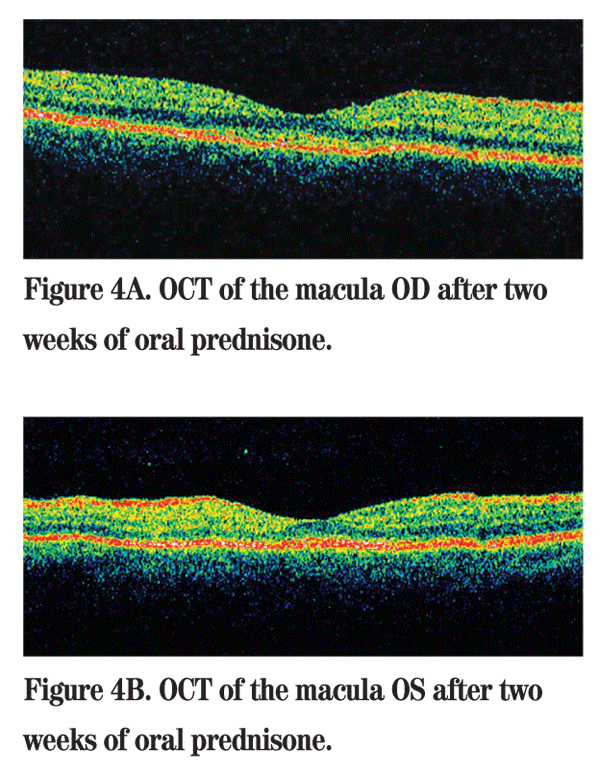
The extraocular manifestations of VKH have been categorized based on time course. The prodromal phase affects melanocytes in the meninges and inner ear causing headache, nuchal rigidity, dysacousia and tinnitus. Patients with auditory complaints may develop permanent hearing loss without prompt and aggressive treatment. Cerebrospinal fluid analysis demonstrates pleocytosis with melanin-laden macrophages. The acute uveitic phase follows the prodromal phase and manifests as optic disc edema and a diffuse choroiditis that causes leakage of fluid from the choroid through the retinal pigment epithelium and subsequent serous retinal detachments. Fluorescein angiography shows a focal delay in choroidal perfusion with diffuse pinpoint leakage (starry-sky appearance), placoid hyperfluorescence and optic nerve head staining. Our patient presented in the acute uveitic phase with prodromal symptoms of headache and tinnitus. The chronic phase describes the depigmentation signs of VKH, including Sugiura's sign of depigmentation at the limbus, the sunset sign of loss of choroidal melanocytes, and vitiligo, alopecia and poliosis.
VKH is treated initially with daily systemic corticosteroids, usually prednisone 1 to 2 mg/kg/day. Some authors advocate the use of IV steroids initially followed by oral prednisone. A slow taper is crucial to minimize recurrence and complications. Adjunctive immunomodulatory therapy is usually employed to avoid systemic side effects of long-term steroid use. Cyclosporine, azathioprine, cyclophosphamide, chlorambucil, methotrexate, FK506, mycophenolate mofetil and anti-TNF agents have all been used as adjunctive therapy with variable success in cases of VKH.
Dr. Luo would like to thank
Read RW, Holland GN, Rao NA, et al. Revised diagnostic criteria for Vogt-Koyanagi-Harada disease: Report of an international committee on nomenclature. Am J Ophthalmol 2001;131:647-52.
Andreoli CM, Foster CS. Vogt-Koyanagi-Harada Disease. Int Ophthalmol Clin 2006;46:111-22.
Read RW. Vogt-Koyanagi-Harada disease. Ophthalmol Clin N Amer. 2002;15:333-41.
Moorthy RS, Inomata H, Rao NA. Vogt-Koyanagi-Harada Syndrome. Surv Ophthalmol 1995;39:265-92.
Rajendram R, Evans M, Rao NA. Vogt-Koyanagi-Harada disease. Int Ophthalmol Clin 2005;45:115-34.



