|
Teresa C. Chen, MD |
In years past, children with pediatric glaucoma had a poor prognosis. In many cases, surgeons could do little to prevent them from progressing to blindness. Fortunately, the prognosis today is much better; in the majority of cases we can now control intraocular pressure and preserve vision.
Here, we'd like to share some of what surgeons have learned in recent years about diagnosing and treating pediatric glaucomas.
Primary Surgical Options
Pediatric glaucoma is generally managed surgically. As a primary treatment, medical therapy often fails to produce long-term IOP control, so it's largely reserved for use as an adjunctive treatment.
In general, surgical therapy for pediatric glaucomas is broken down into primary and secondary surgeries. In the United States, goniotomy and trabeculotomy are considered to be the primary surgical options for most types of pediatric glaucoma. This includes congenital glaucoma, which occurs in about one in 10,000 babies, usually during their first year of life. This makes it one of the most common problems in the pediatric glaucomas.1
Here are brief summaries of the primary surgical approaches.
• Goniotomy. This was initially described in the 1930s by American ophthalmologist Otto Barkan. The technique involves passing a goniotomy knife across the anterior chamber through the peripheral cornea and incising the trabecular meshwork to improve aqueous flow. The success rate of this approach is roughly 80 percent in children who have the surgery between 1 month and 1 year of age. Complications are very uncommon, especially in the hands of an experienced surgeon.
• Trabeculotomy. This is an alternative to goniotomy, useful when corneal edema prevents a gonioscopic view. A recent study by Japanese researcher Hanako Ikeda, MD, and coworkers2 found a success rate of more than 80 percent after an average of almost 10 years.
Some comparative studies of trabeculotomy and goniotomy have found differences in success rates and efficacy, but many surgeons still consider trabeculotomy to be useful as a primary treatment for primary congenital glaucoma. Goniotomy is a shorter operation than trabeculotomy and also does not require conjunctival dissection. However, trabeculotomy is very useful for patients with corneal edema and is familiar to most glaucoma surgeons.
Some patients fail to achieve the desired endpoint after primary treatment with goniotomy or trabeculotomy. In this case, many clinicians repeat the goniotomy or trabeculotomy, which is reasonable; sometimes IOP is controlled after the second treatment.
• A combination of trabeculotomy and trabeculectomy. Some patients, particularly members of certain ethnic populations originating in India, are not good candidates for goniotomy surgery because as many as 90 percent of their infants present with corneal edema.3 Patients in the Middle East are also not good candidates for, or don't respond well to, goniotomy or trabeculotomy.4,5 Although trabeculotomy may be performed, many of these patients have better success rates with a combination of trabeculotomy and trabeculectomy.3
This procedure begins with a typical trabeculotomy. Then a sclerostomy is performed under the same flap used for the trabeculotomy, followed by an iridectomy. The flap is then sutured in much the same way as a standard trabeculectomy. For these patients, Anil K. Mandal, MD, and coworkers found the probability of success to be 94.4 percent at one year, down to 63.1 percent by the sixth year.3
Goniotomy: Multiple Uses
Although it's well known that goniotomy is useful for treating congenital glaucoma, it's less well known that goniotomy is also effective in two other situations: as a means to treat childhood uveitic glaucoma; and as prophylactic surgery to prevent the development of aniridic glaucoma.
Pediatric uveitic glaucoma needs to be treated differently than the adult form of this disease. Common surgical procedures for adult uveitic glaucoma include trabeculectomy surgery with antimetabolites and tube shunt surgery, but all of these cause scarring of the conjunctival tissue, decreasing the prognosis for future glaucoma surgeries. This is a serious concern when managing pediatric patients.
That's why goniotomy is one of the best surgical options for children with uveitic glaucoma; in many cases it will lower the eye pressure but spare the conjunctiva. This surgery may be most effective if the child is less than 10 years of age and has less than 180 degrees of peripheral anterior synechiae.6,7 However, older children, including teenagers, may be treated using this technique.8
The other indication for goniotomy surgery, described by David S. Walton, MD, is to prevent the development of aniridic glaucoma.9 It's important for the clinician to realize that, left alone, as many as half of young patients with aniridia develop glaucoma later in life as a result of the iris progressively blocking the angle.
If you are aware of this possibility and you see these progressive angle changes occurring over months or years, you can use a goniotomy knife to peel the iris tissue away from the angle. This is an effective way to prevent many of these patients from developing glaucoma. Usually, this prophylactic procedure is done when the patient is still a child.
Secondary Surgical Options
Despite their effectiveness in most cases, goniotomy and trabeculotomy fail to control IOP in a significant percentage of patients. In those cases, the basic secondary surgical options are trabeculectomy with antifibrosis drugs; glaucoma drainage implants; and cyclodestructive procedures.
• Trabeculectomy with antifibrosis drugs. One of the risk factors associated with trabeculectomy failure is young age. Using mitomycin-C in this situation increases the likelihood of success and also tends to produce a lower mean IOP postop.
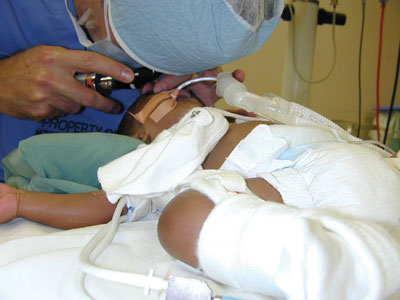 |
| An examination under anesthesia is performed prior to surgery for primary congenital glaucoma. Goniotomy and trabeculotomy are considered primary treatments for this condition. Peter A. Netland, MD, PhD |
Of course, complications can occur with the use of mitomycin-C, including hypotony maculopathy, chronic bleb leaks, blebitis and endophthalmitis. For this reason, most of us try to minimize its use. No definite dosage has been universally agreed upon, and one series done in Riyadh, Saudi Arabia by Ali Al-Hazmi, MD, Johan Zwaan, MD, PhD, and coworkers, found that there was no definite correlation between the amount of mitomycin-C used and success rates.10 In any case, if mitomycin is used, the patient must be monitored closely for potential long-term complications.
• Glaucoma drainage implants. Drainage implants can be very effective in lowering IOP in patients with intractable glaucomas; success rates range from 56 to 95 percent.1
One-stage implantation is preferable in children when a valved drainage implant is used; two-stage implantation can also be used in high-risk eyes when a non-valved drainage implant is used. In the latter technique, the implant plate is sutured into position and the tube is left underneath the conjunctiva next to the limbus. The eye is allowed to recover for three to four weeks so a pseudocapsule can form around the plate; then the tube is inserted into the anterior chamber. The pseudocapsule minimizes the risk of postoperative hypotony.
When deciding whether trabeculectomy with mitomycin-C or a drainage implant is best for the patient, the surgeon must carefully weigh many factors1 which include the following: the etiology of the glaucoma;11 the state of the conjunctiva; the history of past ocular surgeries; the ability for postoperative follow-up; etc. For either surgery, the use of adjunctive glaucoma medications may eventually be needed, and postoperative complications can always occur. Fortunately, the majority of complications are not vision-threatening in either group.
• Laser cyclophotocoagulation. Patients generally tolerate this procedure quite well. However, it's still considered a treatment of last resort. The advantage of this procedure is that it doesn't require incisional therapy, but patients can suffer serious complications, including vision loss and phthisis. Success rates in the literature range from 38 to 59 percent—typically around 50 percent.1 With retreatment, reported rates of success do go up a little bit—in some cases as high as 79 percent— but clinicians generally don't choose this as a primary surgery because much better alternatives are available. Nevertheless, in some situations, it can be useful if a patient has failed other glaucoma surgeries. Note: If you do use this option, it's crucial to inform the patient's family about the risks.
Using Medical Therapy
As mentioned earlier, surgery is considered the definitive treatment for most pediatric glaucomas. Medical therapy is primarily thought of as an adjunctive technique; it often fails to produce long-term IOP control, and it can produce more systemic side effects than it does when treating adults. Medical treatment may be used, for example, to temporarily reduce the IOP and improve clarity of the cornea prior to goniotomy surgery.
Each medical option has pros and cons:12
• Beta blockers. These can be very effective. However, it's advisable to use a 0.25% concentration initially rather than a 0.5% formulation.
• Carbonic anhydrase inhibitors (CAIs). These aqueous suppressants, which are available in topical or systemic form, can be useful when treating children. Using them systemically, however, may produce more side effects. Also, for systemic use with younger children, you may need to have a pharmacist prepare the drug as a suspension. Topical CAIs avoid this problem, so they are generally preferred, as long as they're effective enough to lower the IOP. However, in some children, topical absorption may be variable; in those cases, systemic CAIs may be more reliable.
• Prostaglandins. These can be helpful, although response rates may be lower than in adults. However, prostaglandins have fewer serious systemic side effects and therefore may be beneficial.
• Cholinergic drugs. These are less commonly used for pediatric glaucoma, as they can cause problems relating to ciliary spasm and/or trigger a myopic shift. However, they may be useful as an adjunct for some surgical treatments.
• Alpha 2-agonists. Drugs such as brimonidine should generally be avoided in younger children and only used with great caution in older children. They are associated with sedation and side effects that can be potentially fatal in these age groups.
• Age of the child. If a child is younger than 2 or 3, he or she may respond best to goniotomy, as opposed to other options like trabeculectomy surgery. |
Aphakic Glaucoma
After congenital glaucoma, the second most common type of pediatric glaucoma is aphakic glaucoma. When a child is born with congenital cataracts, they must be removed early so that vision can develop normally. As a result, many of these babies have surgery within the first year of life.
Unfortunately, once the cataract is removed these patients have, on average, a 20-percent chance of developing aphakic glaucoma over an average of 11 years of follow-up.13 It's also important to realize that this type of glaucoma can occur even decades later.14 In fact, with more than a decade of follow-up, it's probable that the incidence is even higher, making glaucoma the most common complication of pediatric lensectomy surgery.
Nobody knows the exact reason for the connection, although there are many theories. We do know which babies are at higher risk for this devastating surgical complication: those who have surgery within the first year of life; those with corneal diameters less than 10 mm; those with the nuclear or complete cataract types; and those who have surgical complications from their cataract surgery.15 The problem is that, unlike congenital glaucoma, which is easier to diagnose because the eye looks abnormal, many children who develop aphakic glaucoma have no obvious external signs or symptoms. In an older child, the eye may look normal despite the high eye pressure, and the child won't complain until most of the peripheral vision is already permanently lost. As a result, aphakic glaucoma can remain undiagnosed for many years, leading to irreversible loss of vision. The important message here is that clinicians need to be aware of this problem; if general ophthalmologists don't know that these patients are at risk for developing glaucoma, they won't look for it.
 |
| A child with congenital glaucoma. This condition affects about one in 10,000 babies, making it one of the most common pediatric glaucomas. Teresa C. Chen, MD |
Although aphakic glaucoma may occur three to four years after cataract surgery,13-14 life-long screening for aphakic glaucoma is needed since aphakic glaucoma can occur decades after the initial lensectomy surgery. Life-long screening often doesn't happen, because many ophthalmologists believe that once a child has had congenital cataract surgery and the amblyopia issues have been resolved, he or she is out of danger. Hopefully, correcting this mistaken impression will cause doctors to perform glaucoma screening exams on all patients who've had congenital cataract surgery. Also, spreading the word may help get these patients to understand that they can't just disappear and not have an eye exam for 10 years.
How often should these patients be checked? That depends on the patient. If the patient has more risk factors, she may need to be screened for glaucoma every three to four months. If there are fewer risk factors, then she may only need to be screened every six to 12 months. The ophthalmologist must decide how often the patient needs to return.
Worth the Effort
In addition to treatment considerations, ongoing care of these young patients often involves a multidisciplinary, team approach. In many cases parents, teachers, mobility instructors and low-vision specialists may need to help with patient care. This kind of coordination may mean spending extra time and effort on these already challenging cases.
Nevertheless, we've come a long way from years ago when the prognosis for childhood glaucoma was poor. Knowing that we may be able to save the vision of many of these patients is a great reward.
For more information about congenital glaucoma see reference #1 or visit childrensglaucoma.org (the Children"s Glaucoma Foundation); pgcfa.org or gl-foundation.org.
Dr. Chen is a glaucoma specialist at the Massachusetts Eye and Ear Infirmary and an assistant professor of ophthalmology at Harvard Medical School. Dr. Netland is the Siegal Professor, director of glaucoma and vice chair for academic affairs in the Department of Ophthalmology at the Hamilton Eye Institute, University of Tennessee Health Science Center, Memphis, Tenn.
1. Mandal AK, Netland PA. The Pediatric Glaucomas. Edinburgh: Elsevier, 2006.
2. Ikeda H, Ishigooka H, Muto T, Tanihara H, Nagata M. Long-term outcome of trabeculotomy for the treatment of developmental glaucoma. Arch Ophthalmol. 2004;122:8:1122-8.
3. Mandal AK, Bhatia PG, Bhaskar A, Nutheti R. Long-term surgical and visual outcomes in Indian children with developmental glaucoma operated on within 6 months of birth. Ophthalmology. 2004;111:2:283-90.
4. Elder MJ. Congenital glaucoma in the West Bank and Gaza Strip. Br J Ophthalmol 1993; 77:413-416.
5. Mandal AK, Naduvilath TJ, Jayagandan A. Surgical results of combined trabeculectomy-trabeculotomy for developmental glaucoma. Ophthalmology 1998;105: 974-982.
6. Ho CL, Wong EY, Walton DS. Goniosurgery for glaucoma complicating chronic childhood uveitis. Arch Ophthalmol 2004;122:6:838-44.
7. Ho CL, Walton DS. Goniosurgery for glaucoma secondary to chronic anterior uveitis: prognostic factors and surgical technique. J Glaucoma 2004;13:6:445-9.
8. Freedman SF, Rodriguez-Rosa RE, Rojas MC, Enyedi LB. Goniotomy for glaucoma secondary to chronic childhood uveitis. Am J Ophthalmol 2002;133:617-621.
9. Chen TC, Walton DS. Goniosurgery for prevention of aniridic glaucoma. Arch Ophthalmol 1999;177:9:1144-48.
10. Al-Hazmi A, Zwaan J, Awad A, al-Mesfer S, Mullaney PB, Wheeler DT. Effectiveness and complications of mitomycin C use during pediatric glau
coma surgery. Ophthalmology 1998;105:10:1915-20.
11. Chen TC, Bhatia LS, Walton DS. Ahmed valve surgery for refractory pediatric glaucoma: A report of 52 eyes. J Pediatr Ophthalmol Strabismus 2005:42:274-83.
12. Maris PJG Jr, Mandal AK, Netland PA. Medical therapy of pediatric glaucoma and glaucoma in pregnancy. Ophthalmol Clin N Am 2005;18:461-468.
13. Chen TC, Bhatia LS, Walton DS. Complications of pediatric lensectomy in 193 eyes. Ophthalmic Surg Lasers Imaging 2005;36:6-13.
14. Chen TC, Walton DS, Bhatia LS. Aphakic glaucoma after congenital cataract surgery. Arch Ophthalmol 2004;122:1819-25.
15. Chen TC, Bhatia LS, Halpern EF, Walton DS. Risk factors for the development of aphakic glaucoma. J Pediatr Ophthalmol Strabismus and the Transactions of the American Ophthalmological Society, in press.




