Decades ago, cataract sur-gery was performed with the aid of an air bubble to keep the anterior chamber formed during the capsulotomy and even lens insertion. The air bubble did very little to protect the corneal endothelium, and its ability to partition or pressurize the eye was marginal. This is part of the reason why surgical complications, from ruptured capsules to corneal decompensation, were prevalent. This changed with the advent of viscoelastics, now more commonly referred to as ophthalmic viscosurgical devices.
First used in ophthalmic surgery in 1972 as a replacement for vitreous and aqueous humor, OVDs have revolutionized the way cataract surgery is performed, so much so that the term viscosurgery is used to describe surgical procedures using these solutions. OVDs are routinely used in cataract surgery to protect delicate ocular structures, compartmentalize within the eye, pressurize the anterior chamber, and provide a faster and safer surgery with better visual recovery for our patients. The first commercially available OVD, Healon, changed cataract surgery for the better and started a new class of surgical products.
To use OVDs appropriately, an understanding of their properties is needed to allow surgeons to choose between the many different commercially available OVDs for the specific surgical task.
Composition and Properties
The uniqueness of the properties of each OVD is more than simply a function of their fundamental constituents. It's a function of a number of variables including concentration, molecular weight and size of molecular building blocks of the material.
The commonly used OVDs are composed of the following three building blocks:
• sodium hyaluronate (
• chondroitin sulfate (CS): another biopolymer, a major mucopolysaccharide in the cornea; and
• hydroxypropyl methycellulose (HPMC): a component of plant fibers.
It's important to note that very similar viscoelastics can be made out of sodium hyaluronate as well as chondroitin sulfate, and that it is the molecular size, weight and concentration that determine the characteristics of the OVD, and not so much the specific chemical component.
The rheological properties of viscolastics determine the classification, behavior and utility of each OVD. These include viscoelasticity, viscosity, pseudoplasticity and surface tension. These are useful to understand when making the right choice for use in ophthalmic surgery.
• Viscosity describes the resistance to flow. OVDs have flow properties not described by a single value of viscosity, which makes them distinct from other solutions like water.
Their viscosity changes with different flow rates. The faster the flow of OVDs, the greater the decrease in the viscosity, which measures the ease of injection of the material.
Zero flow, or zero shear rate, gives the maximum viscosity of a viscoleastic, which determines the material's stabilizing effect. Medium viscosity occurs at medium flow of fluid which describes the mobilizing effects of OVDs.
• Viscoelasticity describes the elastic component of the solution in being able to return to its original shape after being stressed. It describes the material's ability to reform after an external force is applied to the anterior chamber and then removed.
• Psuedoplasticity is the property of OVDs that refers to the ease of ability of a material to change from being highly viscous at rest to being watery at higher shear rates.
• Surface tension, or coatability of an OVD, describes the surface tension of the OVD itself and also to the contact tissue, surgical instrument or IOL.
Classification
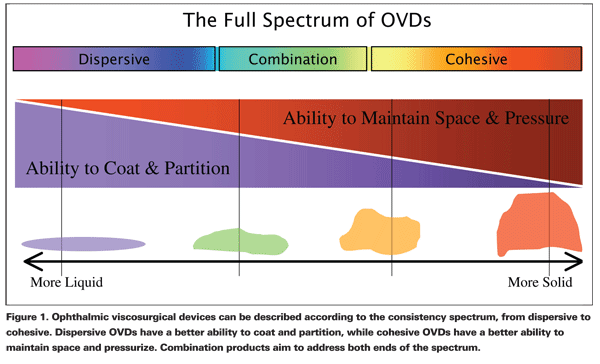
Cohesiveness and dispersiveness are useful constructs in describing the clinical behavior of OVDs, helping us to better understand the interaction among the various rheological properties described above. Cohesive OVDs are characterized as being materials with high viscosity, adhering to themselves well by intramolecular interactions, and therefore resisting being split apart. These are the higher molecular weight OVDs, which tend to be long chains that are stuck together so they exhibit a high degree of psueoplasicity and higher surface tensions. Dispersive OVDs exhibit the opposite characteristics since they have a lower viscosity and have a high coatability, which is the ability to stick to and coat tissues, IOLs and instruments. These have small chains and lower molecular weights that allow them to break apart easily, with lower surface tension and lower pseudoplasicity.
For the sake of simplicity, it is easy to divide viscoelastics into four broad categories: 1) dispersives, 2) cohesives, 3) combination agents and 4) visco-adaptives.
Dispersive OVDs
With a lower viscosity, dispersive OVDs have the ability to coat intraocular structures, and they tend to stay in place during the fluidics of phacoemulsification surgery. Think of these agents as similar to molasses or honey. And since they are retained when injected, they are good for partitioning spaces within the eye, such as after a rupture of the posterior capsule. Due to this retentiveness, removal of dispersive OVDs requires more effort at the end of surgery. Dispersive viscoelastics can also serve to lubricate injector cartridges to aid in IOL insertion.
Examples of common dispersive OVDs include Healon D (AMO), Viscoat (Alcon), and OcuCoat (B&L). Note that Healon D is sodium hyaluronate; viscoat is both sodium hyaluronate and chondroitin sulfate; and Ocucoat is hydroxy-propyl-methylcellulose (HPMC). The specific constituents of these products are not the primary determinants of the performance of these dispersive OVDs, rather it is the final rheological characteristics that are critical. This is why Healon D and Viscoat perform nearly identically in the eye, while OcuCoat is somewhat different in performance.
Cohesive OVDs
With a higher viscosity, cohesive OVDs are able to pressurize the eye and create space, such as during IOL insertion. Because they are more viscous and more solid in their behavior, they are ideal for flattening the anterior capsule to facilitate capsulorrhexis creation or for deepening a shallow anterior chamber. Think of these agents as more of the consistency of jam or jelly. Due to their cohesiveness, the entire mass of viscoelastic tends to stick together. This makes removal at the end of the case easy, however it makes chamber retention less effective. These are ideal products to use during capsulorrhexis creation and during IOL insertion.
Examples of common cohesive OVDs include Healon (AMO), Healon GV (AMO), Provisc (Alcon), and Amvisc (B&L). Note that all of these products are composed of sodium hyaluronate, and by changing the concentration different characteristics can be achieved. Healon is cohesive while Healon GV is even more cohesive, with the GV standing for greater viscosity.
Combination OVDs
For routine cases, much effort has been put into making a single agent with both dispersive and cohesive properties. This is a challenge since it is difficult to provide the full spectrum of properties with a single agent. Protecting the corneal endothelium throughout the surgery is a dispersive characteristic, while flattening the anterior lens capsule during capsulorrhexis is a cohesive attribute. Examples of these agents include DiscoVisc (Alcon) and Amvisc Plus (B&L), both of which aim to be a good single-syringe agent for routine cases. With characteristics of both higher viscosity cohesives as well as lower viscosity dispersives, these agents can be thought of as highly viscous dispersive OVDs.
Realizing that two separate OVDs offer more versatility than a single agent, companies offer dual-viscoelastic systems, which incorporate a dispersive OVD and a cohesive OVD in separate syringes. Alcon's DuoVisc system consists of Viscoat (dispersive) and ProVisc (cohesive), while AMO's combination system allows the choice of Healon D+H, which is Healon D (dispersive) and Healon (cohesive), or Healon D+GV, which is Healon D (dispersive) and Healon GV (greater viscosity cohesive). Bausch & Lomb's agents, AmVisc (cohesive) and OcuCoat (dispersive), can be opened together, though they are not packaged as such.
Visco-Adapative OVDs
A new class of OVDs was created when AMO introduced Healon 5, which is a pseudo-dispersive, ultra-viscous cohesive. This is a visco-adaptive OVD which behaves as a super- cohesive viscoelastic to pressurize and create space, yet can provide the protection of dispersives. It takes advantage of both properties of viscoelastics, by being a substance that changes its behavior at different flow rates. The lower the flow rate, the more viscous and cohesive the OVD becomes. The higher the flow rate, the more pseudodispersive the viscoelastic is allowing for better protection of the corneal endothelial cells from injury during the phacoemulsification step.
The low-flow, slow-motion phaco technique pioneered by Robert Osher, MD, allows for the use of Healon 5 for the entire phacoemulsification surgery. At high flow rates, Healon 5 tends to be removed from the eye. Many surgeons prefer to use Healon 5 in combination with another, more dispersive viscoelastic, in the "soft-shell" technique.
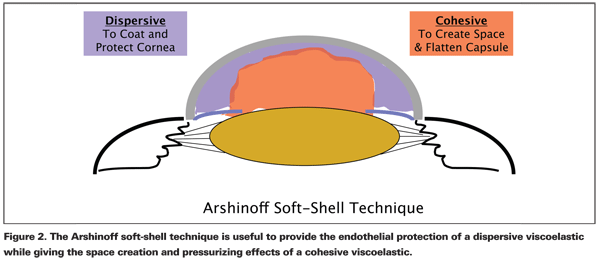
The Soft-Shell Technique
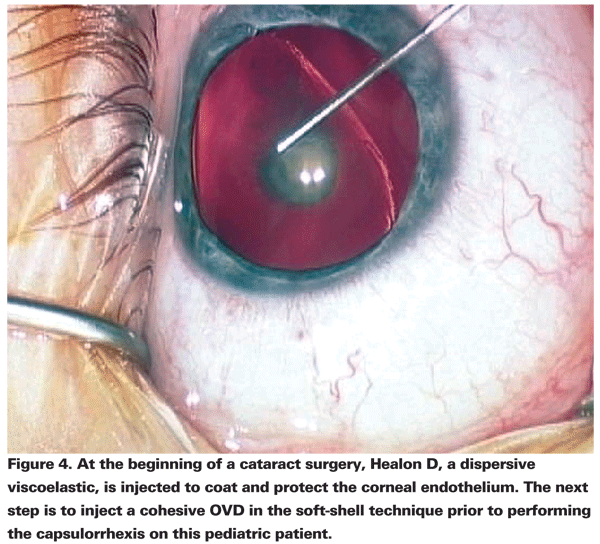
Steve Arshinoff, MD, has described the soft-shell technique (SST), which is a way to use two viscoelastic agents simultaneously. The dispersive OVD is placed first to coat the corneal endothelium, then the cohesive OVD is injected centrally to flatten the anterior lens capsule, deepen the anterior chamber, and force the dispersive OVD towards the cornea.
The ultimate soft-shell technique (USST) adds a third step of placing a layer of balanced salt solution between the cohesive OVD and the anterior lens capsule. This is particularly useful in white cataracts where a capsular dye, such as Trypan blue, is used to stain the anterior lens capsule.
The combined use of both a cohesive OVD and dispersive OVD is also helpful in challenging cases. For cases of floppy iris syndrome, the soft-shell technique can hold the iris in place throughout the surgery. For cases of broken zonules, the dispersive OVD can compartmentalize the eye and keep vitreous pushed posteriorly, while the cohesive OVD keeps the anterior chamber formed and pressurized.
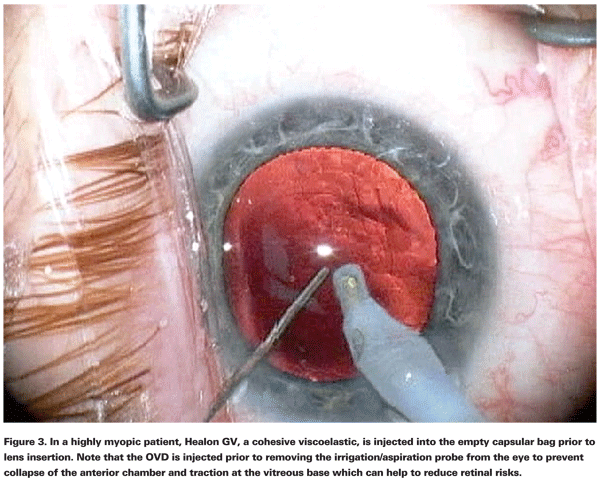
In highly myopic eyes, dispersive OVDs protect the cornea, while re-application of cohesive OVDs to pressurize the anterior segment can minimize traction on the vitreous base and decrease retinal risk.
Choosing a Viscoelastic
The ideal OVD depends on the step of surgery. To facilitate capsulorhexis creation, the OVD should be cohesive to flatten the anterior capsule yet elastic and pseudoplastic enough to allow freedom of movement within the anterior chamber. To shield the corneal endothelial cells, a dispersive OVD tends to have the best chamber retention and more protective effects. For loading an IOL into an injector cartridge, a dispersive OVD provides good lubrication. To expand the capsular bag for IOL insertion, a cohesive OVD works well and has the benefit of easy removal at the end of the surgery.
OVDs have become indispensable tools in cataract surgery and multiple other ophthalmic procedures. With so many different viscoelastics available from the major manufacturers, it's clear that there is no one single OVD that is perfect under all circumstances. The right choice of OVD is dependent not only on the surgeons surgical style, with flow rates producing different viscosities in the OVDs, but also on multiple physiochemical characteristics of OVDs and the desired effect to be achieved for each step of the surgical process.
The best way to determine which OVDs work well with your surgical technique is a test drive. For almost all cases, I have found that two agents are better than one, so I prefer a dual viscoelastic system to provide the best results during the different parts of the surgical procedure. For others, a single agent may be more useful for routine cases. Keep an open mind and try multiple viscoelastics in order to find the right combination to suit your surgical style and patient population.
Dr. Afsari is an ophthalmologist in training at the
Adina B. The influence of viscoelastic substances on the corneal endothelium during cataract surgery by phacoemulsification. Oftalmologia 2008;52(1):84-9.
Arshinoff SA. Modified SST-USST for tamsulosin-associated intraoperative [corrected] floppy-iris syndrome. J Cataract Refract Surg 2006;32:559-61.
Arshinoff SA, Jafari M. New classification of ophthalmic viscosurgical devices—2005. J Cataract Refract Surg 2005;31:2167-71.
Arshinoff SA, Wong E. Understanding, retaining, and removing dispersive and pseudodispersive ophthalmic viscosurgical devices. J Cataract Refract Surg 2003;29:2318-23.
Arshinoff SA. Using BSS with viscoadaptives in the ultimate soft-shell technique. J Cataract Refract Surg 2002;28:1509-14.
Arshinoff SA. Dispersive-cohesive viscoelastic soft shell technique. J Cataract Refract Surg 1999;25:167-73.
Garg A., Fry L., Tabin G., Pandey S., Guteirrez-Carmona F., Phaco Manual Clinical Practice in Small Incision Surgery.
Marques DM, Marques FF, Osher RH. Three-step technique for staining the anterior lens capsule with indocyanine green or trypan blue. J Cataract Refract Surg 2004;30:13-6.
Osher RH. Slow motion phacoemulsification approach. J Cataract Refract Surg 1993;19:667.