 |
| The SimVis instrument is a wearable, see-through device that allows patients to experience different visual corrections in the office, including simulated multifocal and monofocal options. (Image courtesy 2Eyes Vision.) |
Simulating Visual Options
One of the challenges when attempting to help a patient with presbyopia is allowing the patient to experience some of the treatment options open to him (such as multifocality) before enacting them, to increase the likelihood that the choice the patient makes won’t leave him unhappy. As any clinician knows, explaining something like multifocal vision in words to a cataract patient is a poor substitute for the actual experience.
Now, a company spun off from the Visual Optics and Biophotonics Lab at the Institute of Optics in Madrid, Spain, has created a wearable device that allows patients to experience different types of correction in real-life situations, including the improved near vision and reduction in distance visual quality associated with multifocal lenses. Because the device can simulate simultaneous vision, it’s called SimVis.
“Our laboratory has long been involved in research and development of adaptive-optics visual simulators, such as devices that allow us to manipulate the optics of the eye through deformable mirrors and/or spatial light modulators,” explains Susana Marcos, PhD, professor of research at the Institute of Optics and co-founder of 2Eyes Vision, the company marketing the device. “These instruments allow us to do very useful research on neural adaptation and help us understand vision with new corrections, but due to the reflective nature of the adaptive optics mirrors and their high cost, these instruments tend to be bulky and expensive. Also, the visual stimuli are generally projected as displays inside the instruments.
“In order to reduce the cost and dimensions of visual simulators we turned to the concept of superimposing near and far images—simultaneous vision—to simulate multifocal corrections,” she continues. “Our first prototype allowed the simulation of bifocal corrections, with different additions and near/far energy ratios. Our current instrument allows simulation of the clinically available multifocal corrections, including bifocal, trifocal and extended-depth-of-focus designs. The device is compact, wearable and see-through.”
Professor Marcos explains that the device works by superimposition of images focused at different distances. “Different lens designs are pre-programmed and controlled automatically from a portable device,” she says. “The current version of the headset is binocular, and in addition to multifocal corrections it can simulate other presbyopia-correcting combinations such as monovision and modified monovision, combining monovision and multifocality. The device corrects for the individual’s existing refractive error, so there’s no need to use any additional refractive correction.
“Because the instrument is wearable and see-through,” she continues, “the patient can visually experience the real world through the different simulated corrections. Patients can perform standard visual function tests, compare the perceived quality across lens designs by rapidly flipping across programmed lenses, or simply walk around the office or other environ-
ments wearing the simulated lenses.”
Asked how patients react to being able to try different options, Professor Marcos says it has made a difference in their satisfaction with the final result. “We’ve tested the system on presbyopes and simulated presbyopes in a laboratory environment, as well as in patients with cataracts who were scheduled for cataract surgery,” she says. “Patients with normal cataracts were able to perform the test, and they found that using SimVis was tremendously helpful in making the decision about which intraocular lens to implant. The clinical experiments we’ve conducted included measurements of visual acuity with different simulated multifocal designs. They also tested subjective preference and scoring of corrections that included monofocal, bifocal, trifocal, monovision and modified monovision corrections in realistic visual settings with near, intermediate and far stimuli. The subjects report clear differences in their preferred corrections.
“On average,” she continues, “a subject’s preference was in line with the expectations we had based on the through-focus optical performance of the lens—i.e., trifocal designs were generally preferred for intermediate distances and monofocal corrections were generally preferred for distance. However, there were important intersubject differences in the subjective preference of one particular design over the others. We’re planning several more studies that will hopefully demonstrate that the SimVis improves satisfaction levels and visual performance postoperatively.”
Professor Marcos says the company hopes to have the SimVis on the market by the end of this year. “We have several other technologies licensed to other companies, ranging from diagnostic devices to multifocal lens designs,” she notes. “Other technologies in the pipeline include new patented paradigms for accommodating IOLs and for IOL engagement to the capsular bag. We believe these concepts will move presbyopic corrections to new stages of application.”
Slowing Advancing Presbyopia
Another new instrument called Ocufit (SOOFT italia, Fermo, Italy) appears to help middle-aged individuals delay the progression of early presbyopia. The device, which has received the CE Mark, uses ciliary body electrostimulation to passively exercise and strengthen the ciliary muscles, significantly improving accommodation in many patients, the company says.
 | 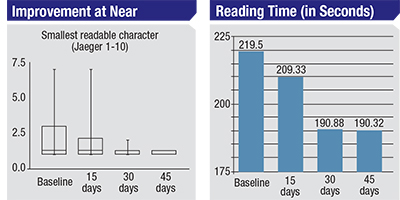 |
| The Ocufit system uses electrodes embedded in a contact lens (above, left) to repeatedly stimulate the ciliary muscles during eight-minute sessions. The repeated contractions exercise and appear to strengthen the ciliary muscles, thus potentially improving accommodation. Early presbyopic emmetropes undergoing the treatment report improvement in near vision and reading speed. The charts above show vision test results for 60 early users; results were statistically significantly improved at 30 days compared to baseline in both datasets. | |
The lens is placed on the patient’s eye for a series of eight-minute treatments. Patients feel a tingling sensation during treatment, but it is generally not painful. Early clinical testing indicates that the treatment may improve accommodation and increase reading speed in emmetropes with early presbyopia. (See charts, p. 16.)
Luca Gualdi, MD, an anterior segment surgeon at Studio Oculistico Gualdi, in Rome, Italy, has been testing the device on emmetropes with early presbyopia, at the request of the manufacturer, for about a year. “This technique for managing presbyopia is not surgical and there are no side effects,” he notes. “The patient doesn’t have pain or lose vision after the treatment. The worst possible outcome is seeing no effect from the treatment.
“The company gave us the instrument to test because we have a large practice in a metropolitan area and we own many instruments that are useful for monitoring vision,” he continues. “I’ve performed 300 treatments on 60 patients so far. Among emmetropes between 40 and 50 years old, 95 percent of the patients I’ve treated are happy because they’ve seen a positive effect.”
Dr. Gualdi explains that the idea for this type of electrostimulation is not new. “In the past this type of stimulation has been used to treat optic atrophy, glaucoma, macular degeneration and progressive myopia,” he says. “One scientist demonstrated that stimulating the ciliary muscle moves the trabecular meshwork, leading to a decrease in intraocular pressure after treatment. The Ocufit can also be used to do that, although it requires running a different program.”
Dr. Gualdi explains that the rhythmic contractions caused by the electrostimulation produce an increase in the efficiency of the ciliary muscle, leading to an increase in accommodative range that can last for several months. Currently, each eight-minute session involves two seconds of electrostimulation out of every eight seconds. The stimulation affects the entire muscle, not just where the electrodes are located, much as it does when this type of electrostimulation is used for other purposes such as physical therapy.
“You have to tell the patient that this is not surgery,” Dr. Gualdi notes. “It’s exercise, like going to the gym. If you don’t train, your muscles get smaller. So, you have to keep training your ciliary muscles if you want to put off wearing glasses. If you keep the muscles in shape, instead of starting to wear glasses at age 41, you might be able to wait until age 50.”
Although patients usually feel no pain, Dr. Gualdi notes that the reaction is different from patient to patient. “Some say they feel nothing at all,” he says. “Other patients receiving a higher level of stimulation say they feel a little discomfort during the first treatment. You can regulate the power, so if your patient is more sensitive you can reduce the intensity. That will also reduce the effect, but it’s important that the patient be comfortable during the procedure. For that reason, we start with less energy for the first treatments and gradually increase it over the course of the treatments. We just keep asking the patient if he or she is OK.”
Dr. Gualdi says the company asked him to use the device partly to test the duration of the effect. “We have about one year of follow-up at this point,” he says. “Our current protocol is to do a series of three or four treatments during the first two months, one every 15 days or so. After that, one treatment every three months is sufficient to maintain the effect, on average. Younger patients may be able to go for longer than three months.
“The average patient says he can tell a difference after the first or second treatment,” he notes. “Some patients don’t report a difference after one treatment, but when I check I do find there’s been an increase in their visual parameters. By the second treatment most patients say they can tell the difference. They’ve been able to decrease the size of the letters on their smartphone screen, or they’re reading better without reading glasses, especially in dim-light conditions.
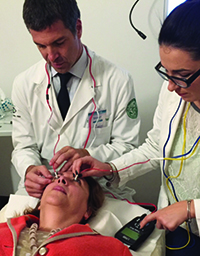 |
| Patients receiving the Ocufit treatment generally report a tingling sensation but no pain. Treatment intensity is adjustable. |
Dr. Gualdi says the treatment does not appear to cause cataract. “Our studies have shown that the treatment does cause a slight negativization of spherical aberration curvature during accommodation,” he says. (Ultrasound biomicroscopy showed a significant increase in lens thickness during accommodation, along with a decreased posterior and especially anterior curvature of the crystalline lens.) “This change, however, does not seem to affect distance vision at all. In fact, that’s one of the best things about this treatment. Almost every treatment for presbyopia causes a decrease in distance vision, whether the treatment is monovision, presbyopic inlay, multifocal lenses or presbyLASIK. With this treatment, distance vision is not affected.”
In terms of the cost to the patient, Dr. Gualdi notes that his practice is one of the first to offer this service, and they’re keeping the cost fairly low. “After three or four months the effect of the treatment wears off, so it can’t be too expensive or patients won’t opt for it. We’re currently charging 100 Euro per treatment. We want to give the world an effective presbyopia treatment that is not painful; we’re not doing this to make a lot of money.”
Dr. Gualdi says the company is just beginning to market the product in Italy. “They’re starting slowly,” he says. “They don’t want everyone to have the machine at first; some doctors might use it on everybody, people who are too old to benefit, for example, resulting in no effect and the procedure getting a bad reputation. They want to be sure the treatment is in the hands of doctors who understand how to use it, who can help develop the best protocol. The company definitely does plan to market this in the United States.
“I intend to try this on myopes with early presbyopia next,” Dr. Gualdi adds. “I want to see whether the increased accommodation will allow those patients to need fewer pairs of glasses.” REVIEW
Professor Marcos is co-owner of three patents relating to SimVis. Dr. Gualdi has no financial interest in the Ocufit instrument.



