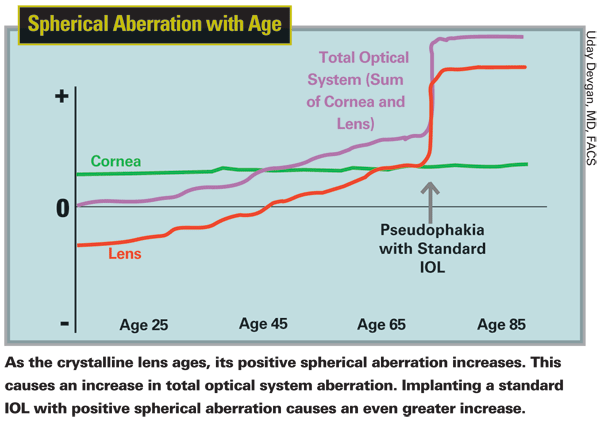
Aspheric lenses—those de-signed to avoid adding positive spherical aberration to an optical system—are in wide use in today's world. You can find them in telescopes, cameras, many spectacles and in the optical equipment in most ophthalmology offices and operating rooms. Unfortunately, standard aphakic intraocular lenses increase the positive spherical aberration of the visual system, which has already been increased by the aging of the crystalline lens. Implanting an aspheric IOL avoids increasing this aberration—and an IOL with negative spherical aberration may even return the optical system to zero spherical aberration by offsetting the cornea's slight positive aberration.
Currently, a number of aspheric IOL designs (both monofocal and multifocal) are available in the
Here, three surgeons with extensive experience using these lenses share their thoughts on these and other related questions.
Can Patients Tell the Difference?
In reality, the difference made by addressing asphericity is usually very small compared to correcting spherical error and astigmatism. Certainly, asking patients to pay more for a lens only makes sense if there is a noticeable gain in visual quality. But is there?
Jay S. Pepose, MD, PhD, medical director of the Pepose Vision Institute and professor of clinical ophthalmology at Washington University School of Medicine and
"It's very pupil size dependent," agrees Uday Devgan, MD, FACS, partner at the Maloney Vision Institute in
Mark Packer, MD, FACS, in private practice in
"My experience suggests that if the refractive error is plano or very close to plano in both eyes, or if the patient has enough residual refractive error that he or she chooses to wear spectacle correction, then the patient will notice a difference in terms of color, clarity and brightness, favoring the aspheric lens," he says. "However, about two-thirds of these patients have residual refractive error between ±0.25 D and ±0.75 D. Their uncorrected visual acuity is adequate, so they don't wear glasses; however, they favor the eye that is closer to emmetropia rather than the eye with the aspheric lens. (These might be the same eye, but they also might not.) In short, lower-order aberrations—sphere and cylinder—have a greater impact than higher-order aberrations such as spherical aberration."
Dr. Devgan agrees. "Many surgeons worry about whether to use an aspheric, and which one to choose," he says. "While I believe in using aspheric IOLs for nearly all patients, it may be more fruitful to hone your lens calculations and astigmatism treatment. A patient with an older style lens and a
Dr. Pepose also notes that studies have demonstrated patients often can't tell the difference between the available aspheric lenses. "Wavefront analysis usually shows some differences between the lenses," he says. "But one recent study found that if you don't preselect the patients—if they're randomized, with a different aspheric lens in each eye—most patients don't express a strong preference for any of three lenses.2 In fact, this study found no significant measurable differences in contrast sensitivity between three implanted aspherics at any spatial frequency under photopic or mesopic conditions. It's true that studies randomizing between spherical and aspheric lenses have demonstrated a measurable difference in contrast sensitivity, but most of those studies didn't ask the subjects if they had a preference. So it's not clear if the average person can distinguish in that situation, either.
"In any case," he adds, "practical issues may make all of this a moot point, at least for the time being. One recent study indicated that the most useful residual amount of asphericity to target may depend on the full spectrum of corneal higher order aberrations, not just on corneal spherical aberration alone.3 This is because of the way spherical aberration interacts with other higher-order aberrations—sometimes dampening them—and also has effects on residual defocus, as well as chromatic aberration."
The Imprecision of Surgery
Whether surgery is precise enough to avoid offsetting the potential benefit of an aspheric IOL is also an issue. "We're not at a point yet in cataract surgery that we can predict a refractive outcome with absolute certainty," notes Dr. Pepose. "We can't tell a patient he's definitely going to come out emmetropic or plus or minus a quarter or even a half diopter. We're not doing ray tracing based on the patient's corneal aberrations or creating a model predicting the exact effective position of the IOL. Furthermore, the capsular bag can contract as part of the healing process, shifting the axial position or centration of the lens. And being centered in the bag may not be the same as being centered in the line of sight. In fact, there could be some advantage to leaving a little bit of spherical aberration to offset other refractive errors that may occur as a result of the surgery."
In terms of the surgery itself altering spherical aberration, Dr. Packer believes that any effect is probably insignificant. "One study found that the mean surgically induced spherical aberration for small-incision cataract surgery is 0.03 ±0.17 µm.4 In my own study, I was able to get 86.7 percent of eyes within ±0.10 µm of the intended asphericity. So the impact of surgically induced spherical aberration appears to be negligible."
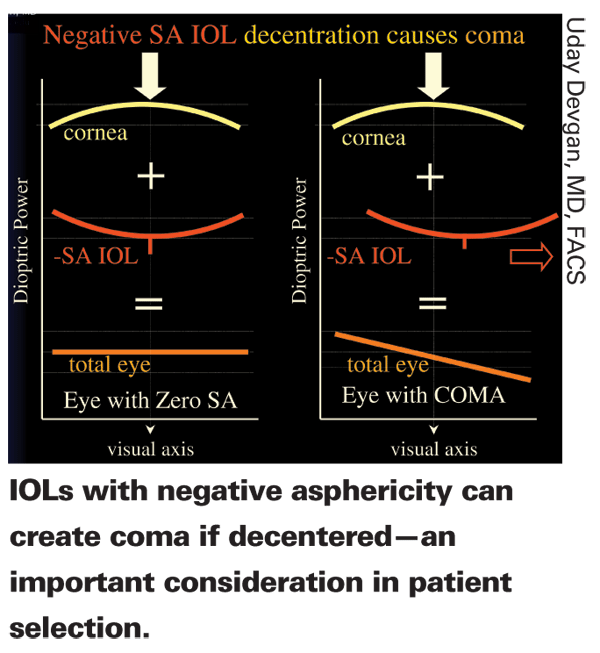
Centration is another concern that is more of an issue with some aspheric lenses. Standard IOLs, which add positive spherical aberration to the optical system, do not create major problems if they decenter. However, a lens designed to have negative aberration is a different matter. (See diagram, p. 35.) "Zero spherical aberration means that the power of that lens is the same in the center and at every point out to the periphery," explains Dr. Devgan. "The advantage of a lens with zero spherical aberration is that if it's decentered it won't confound any existing aberrations. So if you're concerned that the lens may decenter after implantation because of significant pseudoexfoliation or because the capsular bag has broken during surgery, you should choose a lens that has zero spherical aberration. You might also want to make this choice if the patient has an eccentric pupil."
"I use a zero-aberration lens in most cases because I don't want to worry about the lens shifting off-center and inducing coma," says Dr. Pepose. "Fortunately, with the new designs, most lenses stay well-centered under normal conditions, although shifting can occur during healing. Besides, these lenses still have problems such as dysphotopsia. For most patients, I think those problems are a bigger concern than maintaining centration."
Choosing the Right Aspheric
Given the relatively small differences between aspheric lenses—not to mention between standard and aspheric lenses—deciding which one to implant in a given patient can be a challenge. However, many surgeons are using the specific asphericity of each lens as a way to tailor the choice to the individual's optical system. Dr. Packer says he does this for his monofocal IOL patients.
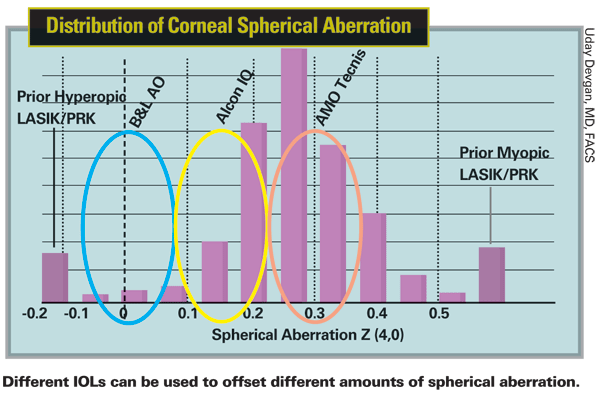
In a recent study, Dr. Packer measured preoperative corneal topographic spherical aberration at the 6-mm optical zone, based on elevation data, using the iTrace instrument from Tracey Technologies. (This measurement is independent of axial length and IOL position because the spherical aberration is based on topography, not ocular wavefront.) He then selected an aspheric IOL based on this measurement and the IOL's labeled spherical aberration, so that the sum of the values was closest to zero. (Dr. Packer notes that corneal spherical aberration can also be measured using any topographer with VOL-CT software from Sarver and Associates [saavision.com/company.aspx].) Thus, for corneal spherical aberration <+0.1 µm, he selected the SofPort; for corneal spherical aberration >+0.1 µm but <+0.235 µm he selected the AcrySof IQ; and for corneal spherical aberration >+0.235 µm he selected the Tecnis Z9000 or Tecnis Z9002.
"My principal selection factor is corneal spherical aberration at the 6-mm zone," he explains. "However, other factors do come into the decision-making process. For example, a patient with a traumatic zonular dialysis, in whom decentration is likely, would benefit more from an IOL with close to zero spherical aberration—although a silicone IOL would be relatively contraindicated because of the zonular dialysis." He also considers factors such as transmission spectrum, refractive index and Abbe number of the material.
"In general, though, these differences don't override choosing the lens to create a customized correction of spherical aberration," he says.
Some surgeons, however, are skeptical that current measurements are precise enough to warrant this. "Myopic LASIK tends to increase positive spherical aberration, so a patient who has had myopic LASIK should receive an AMO Tecnis," says Dr. Pepose. "Beyond that, there is some question of how accurately we can measure spherical aberration.
"The other issue is that we don't fully understand how aberrations interact," he continues. "A little spherical aberration may be desirable as a way to offset chromatic aberration, which can decrease contrast sensitivity by as much as 200 percent. So trying to reduce spherical aberration to zero may not always produce the best visual outcome."
In the case of a multifocal lens, two of which are now available in aspheric models, Dr. Devgan says that in theory choosing an aspheric lens should help to offset the image quality loss caused by splitting the light into multiple focal points. "I've seen anecdotal reports that putting in an aspheric Alcon ReSTOR rather than a regular ReSTOR lens has led to happier patients," he reports, "but I haven't seen concrete published data. I don't know if asphericity is sufficient to counteract the inherent problems of multifocality. Nevertheless, it's probably the right thing to do. We'll shortly have the AMO Tecnis multifocal available and that may further support this point."
Dr. Packer agrees that asphericity is worth adding to a multifocal IOL. "Asphericity improves image quality and reduces dysphotopsia," he says.
The Air Force Pilot Argument
Some surgeons believe that patients should be left with a slight amount of positive spherical aberration in their optical system because this appears to be true in the eyes of Air Force fighter pilots. Dr. Devgan disagrees. "Most fighter pilots are in their mid-30s," he notes. "Generally, younger people have the best vision. Why not aim to equal the vision those pilots had when they were 21?"
Dr. Packer also sees the pilot argument as specious. "Spherical aberration does not correlate with the 'super normal' high-contrast visual acuity described in the Air Force pilot study," he says. "It correlates with peak contrast sensitivity at three to six cycles per degree. Compare the data from the Air Force pilot study5 and a study of 532 preop LASIK eyes.6 The first study looked at spherical aberration in 35 fighter pilots with eyes that were ≥20/15 UCVA; their spherical aberration was 0.110 ±0.077 µm. But spherical aberration in the preop LASIK eyes was 0.128 ±0.074 µm—almost the same. It seems clear that the spherical aberration can't account for the super-normal acuity exhibited by the pilots."
Are They Worth It?
Because aspheric lenses are more expensive than standard lenses and may involve extra measurements for the clinician, do the benefits outweigh the extra cost and time? Some studies have found potential cost savings for society: The Potomac Institute evaluation of the Tecnis night driving simulation study suggests that improved driving performance as a result of reduced spherical aberration with the Tecnis lens could prevent automobile accidents, translating into annual cost savings ranging from $450 million in 2004 to $2.4 billion by 2014.7 But what about the time and cost for the doctor and patient?
"The average surgeon may not be ready to devote extra time to measuring corneal asphericity, or excited about the prospect of having to inventory many more lenses in the ASC," observes Dr. Pepose. "Most surgeons will choose their favorite lens and that's what they'll use. That may not be such a bad thing, since studies are suggesting that there's often very little noticeable difference between the aspheric lenses from the patient's perspective. And the reality is that a lot of people have done very well with standard spherical lenses for many years.
"Nevertheless, I would choose an aspheric lens for most patients," he continues. "I think aspheric lenses are the new standard for most patients undergoing cataract surgery. A number of studies have shown better contrast sensitivity with them, and there are studies showing night driving simulation improvement. Admittedly, some of those tests had to be repeated several times to show any statistical significance, and I don't think asphericity of the lens makes a tremendous difference for the average patient. But since we have aspheric lenses available, I would choose to implant one in most cases."
Dr. Devgan notes that it's still important to keep the issue of asphericity in perspective. "If you really want patient happiness," he says, "do a clean surgery and really nail the lower aberrations. In most cases, you should probably use an aspheric lens, but the one you choose may not be the most critical part of the surgery. Throw the marketing nonsense out the window and see what works for you in your hands and with your patients."
Dr. Pepose is a consultant for Bausch & Lomb; Dr. Devgan is a consultant for Advanced Medical Optics and Bausch & Lomb, and owns stock in Alcon; Dr. Packer consults for AMO and Bausch & Lomb.
1. Fry LL. Tecnis Z9000 versus various other lenses: patient assessment of vision quality. Paper presented at: The ASCRS/ASOA Symposium on Cataract, IOL, and Refractive Surgery; April 15, 2003;
2. Caporossi A, Martone G, Casprini F, Rapisarda L. Prospective randomized study of clinical performance of 3 aspheric and 2 spherical intraocular lenses in 250 eyes. J Refract Surg 2007;23:7:639-48.
3. Koch DD, Wang L. Custom optimization of intraocular lens asphericity. Trans Am Ophthalmol Soc 2007;105:36-41.
4. Guirao A, Tejedor J, Artal P. Corneal aberrations before and after small-incision cataract surgery. Invest Ophthalmol Vis Sci 2004; 45:4312-4319
5. Levy Y, Segal O, Avni I, Zadok D. Ocular higher-order aberrations in eyes with supernormal vision. Am J Ophthalmol 2005;139:2:225-8.
6. Wang L, Koch DD. Ocular higher-order aberrations in individuals screened for refractive surgery. J Cataract Refract Surg 2003;29:10:1896-903.
7. McBride DK, Matson W. Assessing the significance of optically produced reduction in braking response time: Possible impacts on automotive safety among the elderly. Potomac Institute for Policy Studies, April 1, 2003.