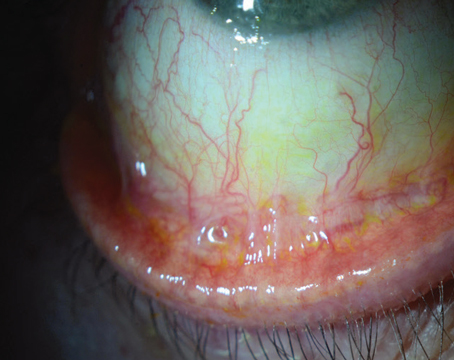
Everyone likes a good mystery, except when it involves finding the cause of peripheral corneal thinning. Possible causes abound, from autoimmune disease to staph hypersensitivity ulcers, and it's up to the ophthalmologist to sort them out and come up with the right one. In this article, corneal specialists explain how you can determine the cause of a patient's thinning peripheral cornea and start the proper treatment as quickly as possible.
Thinning in the 'Quiet' Eye
When a patient presents with some thinning in his corneal periphery, one of the first questions physicians ask is whether or not the eye is inflamed. If it's not, ophthalmologists say you can then look for the following causes:
• Dellen. In the absence of inflammation, one of the more likely causes of the thinning is a dell, or an area of non-wetting that thins and then breaks down, observes Sadeer Hannush, MD, a corneal specialist and attending surgeon at the Wills Eye Institute. "In this case, the treatment is lubrication, maybe punctal occlusion, and a bandage contact lens," he says. "If necessary, you can perform a temporary tarsorraphy."
• Furrow degeneration. This is a variety of peripheral thinning, typically between the limbus and the arcus senilis, that usually occurs in elderly patients. "It can sometimes be illusory because the arcus is there to thicken up the cornea," says Deepinder Dhaliwal, MD, director of cornea and external disease at the University of Pittsburgh Medical Center. "Or, sometimes, there's true thinning. However, the hallmark signs of furrow degeneration are that the thinning, if it's present at all, is very shallow, non-progressive and isn't visually significant; the eye is white and quiet, there's no vascularization and there's no possibility for perforation." As for management, physicians say furrows only need to be monitored at the patient's normal office visits, and no actual treatment is necessary.
• Pellucid marginal degeneration. This is a cousin to keratoconus, says Wills Eye Institute corneal specialist Christopher Rapuano. "However, where keratoconus tends to mean central or paracentral thinning, pellucid is peripheral," he says. "Some patients with pellucid can have severe thinning, usually inferiorly, within a couple of millimeters of the limbus. Though there's no redness, pain or inflammation, it causes significant irregular astigmatism, so the patient tends to complain of a slow, progressive worsening of vision." On topography, PMD will have an area of inferior steepening that resembles a crab claw, physicians note. "For PMD, glasses sometimes help, though the management typically involves a rigid gas permeable contact lens or a hybrid lens like the Synergize," explains Dr. Rapuano. "Rarely, you'll need to do a corneal transplant."
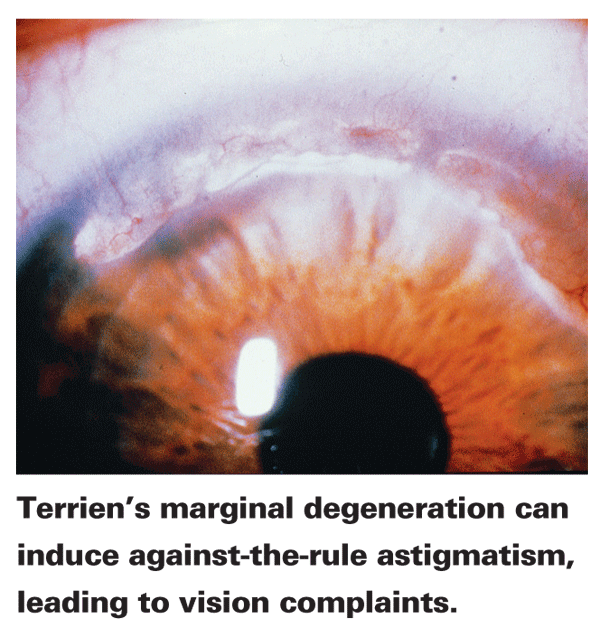
• Terrien's marginal degeneration. This presents as a marginal furrow, usually bilateral, and is most common in men between 20 and 40 years of age. It starts as a non-ulcerated area of thinning located superiorly, and it slowly progresses from there. "You'll see vascularization in addition to the thinning, often with a leading edge of lipid," explains Dr. Dhaliwal. "However, the epithelium is also intact with this condition. The thinning can be progressive, and can progress circumferentially or centrally. And, since it starts superiorly, the patient usually gets against-the-rule astigmatism." Dr. Rapuano says that, though there's no treatment for the thinning, you can manage the astigmatism with glasses or, failing that, RGPs or hybrid lenses.
In some cases, a graft may be necessary. "If a perforation is imminent and the vision is significantly impaired, or you're worried about a spontaneous perf or a perforation occurring from mild trauma, you could do a graft," says Dr. Dhaliwal.
Thinning in the 'Hot' Eye
Patients can also present with peripheral thinning accompanied by ulceration and general inflammation. These are the presentations that ophthalmologists are more con-cerned about, as actual tissue is being lost. Since several of the ul--cerative conditions have similar ap-pearances, it takes more diagnostic detective work to narrow down the cause in these cases. Here are the main issues to consider.
• Narrowing it down. "If the eye is red and painful, and there's peripheral thinning with an epithelial defect, then you first assess the de-fect's size, location and whether it's associated with a hypopyon," says Dr. Hannush. "None of the immune conditions cause a hypopyon, while the bacterial ones do." If there's a hy-popyon, corneal specialists say to proceed as if it's a bacterial infection until proven otherwise. "Scrape it, culture it and put the patient on antibiotics," says Dr. Hannush.
When presented with a non-infectious peripheral ulcerative keratitis, however, first suspect rheumatoid arthritis or another autoimmune condition. If a patient doesn't already have a diagnosis of rheumatoid, physicians also suspect Wegener's granulomatosus, a serious vasculitis; or Mooren's ulcer, which is peripheral ulcerative keratitis of unknown etiology. Unfortunately, all three ulcerative conditions have similar characteristics, and serologic testing is often the key to making the diagnosis. Corneal specialists say many patients who present with PUK often have already been diagnosed with rheumatoid disease and are on some type of systemic medication for it already, which aids the diagnosis. This isn't always the case, however.
"If the patient doesn't already have a diagnosis of a systemic disease associated with peripheral corneal thinning with ulceration, then we order a panel of blood work," ex-plains Dr. Dhaliwal. "We check for rheumatoid factor, order an ery-throcyte sedimentation rate, an antinuclear antibody test, an anti-neutrophil cytoplasmic antibody test and a complete blood count. Also, in cases in which we don't know or suspect the cause, we'll also check for hepatitis-C, because there's one form of peripheral thinning that looks like peripheral ulcerative keratitis or Mooren's ulcer but which is actually associated with hepatitis-C and is very responsive to interferon therapy. You don't want to miss that."
If autoimmune disease isn't the cause, the other two frequent diagnoses, Wegener's granulomatosus and Mooren's ulcer, have similar ap-pearances. "Wegener's is one of the main differentials in PUK be--cause, if it's missed, it can kill someone," says Dr. Hannush. "So, the ophthalmologist can play a huge role with his diagnosis. Wegener's is a vasculitis that manifests with peripheral corneal ulcers that mimic a Mooren's ulcer, in which there's a nasal or temporal immune-looking ulcer—in other words, there's no hypopyon in the anterior chamber. The patient needs a chest X-Ray or a CAT scan of the chest because the Wegener's patient will have a classic diagnostic picture in that region. If a mass is observed, a biopsy is necessary in some cases." With Wegener's in mind, Dr. Hannush reiterates the need for an ANCA in all cases of PUK. Dr. Rapuano adds that, if a patient's ulceration involves the sclera as well as the cornea, suspect Wegener's.
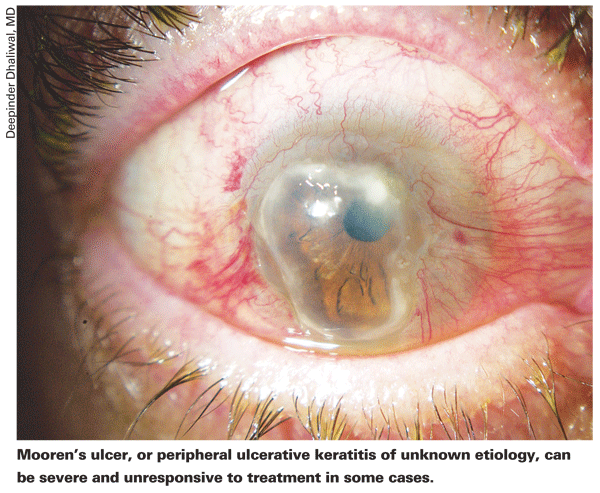
If the PUK isn't from an autoimmune condition like RA, Wegener's or hepatitis, it's classified as Mooren's ulcer, or a peripheral ulcerative keratitis of unknown etiology.
"Mooren's is typically more chronic, progressive and very painful," says Dr. Dhaliwal.
"It will begin in the periphery and spread both circumferentially and centripetally. The key sign is that there will be a leading, undermined edge of de-epithelialized tissue. There will also usually be blood vessels crossing the edge." Dr. Hannush notes that there's also a milder form of Mooren's ulcer that's more limited and actually responds well to medical therapy consisting of lubrication and low-dose steroids and tarsorraphy, if necessary.
There are also less common causes that need to be kept in mind, as well. "Corneal melting can occur in the setting of the neurotrophic cornea or from the frequent use of topical anesthetics or topical non-steroidal anti-inflammatories like Acular, Xibrom and Nevanac," advises Dr. Rapuano. "Another cause, which was more common when we did more scleral surgery, is surgically induced necrotizing scleritis, in which there's melting of the sclera from an old cataract wound. This was rare to begin with, and it still is, but it's worth being aware of."
The cause may also be just staph marginal hypersensitivity, a relatively mild condition. "In blepharitis and other lid disease, patients can get small white infiltrates at the limbus," says Dr. Rapuano. "Those infiltrates can be associated with some thinning and, when they heal, they can result in some scarring and thinning, but they're not that serious."
• Managing the patient. Though the patient will be referred to an internist or rheumatologist for proper treatment if there's a systemic cause for the PUK, whatever the cause, the ophthalmologist will still need to handle the ulcerative condition and quiet the eye.
"The goal is to get the epithelium to heal; then the melting will stop," says Dr. Rapuano. "Ways to go about doing that are artificial tears and lubrication, lots of ointment and sometimes Restasis if you think the patient's dry and the inflammation might benefit from the drug."
Dr. Dhaliwal says she may take further steps if the condition warrants it. "Oral doxycycline can be helpful," she says, "as can conjunctival resection in the area adjacent to the area of melting."
"Usually, if the cause is rheumatoid disease, you're going to use systemic steroids," says Dr. Hannush. Experts base the dose on body weight, but say it usually ends up being around 60 mg per day. "The patient may already be on steroids, and you may need to increase them, or, he may be on another biologic agent like Enbrel or Remicade, and you'll have to add an oral steroid to that," adds Dr. Hannush.
The use of topical steroids in these cases is controversial. "Topical steroids have properties that break down collagen, but these patients' collagen is already breaking down. So, I'll usually use oral steroids unless the patient's on a Wegener's treatment of cyclophosphamide or other potent immunosuppressives. Most of us don't think there's a role for topical steroids unless the cause is something simple we've skipped over completely, like staph marginal hypersensitivity ulcers.
"I'm not saying topical steroids should be avoided altogether," Dr. Hannush continues. "But, certainly, if there's a thinning disorder, you should avoid them. If there's an ulcer but without significant thinning, and you suspect an immune phenomenon, you can use them, though. I'm fond of FML ointment because it lubricates and protects the ocular surface while delivering some steroid. For example, in Mooren's ulcer, what do you do?
There's no systemic treatment for it like in rheumatoid disease, but the patient has a hot eye, and many of these cases don't respond to oral steroids, so you may have to treat them with something like FML ointment."
• Perforations. In some cases, the thinning will progress to the point of perforation, or near perforation.
"There are many options in this case," says Dr. Hannush. "If it's about to perforate, the question is, how big is the crater? You can put medical-grade cyanoacrylate glue in it and cover the eye with a bandage contact lens. Or, you can stuff the crater with amnion and put a piece of amnion on top of the entire area. If the perforation is in the very periphery of the cornea, you can create a conjunctival bridge over it. If it's in the center, you can do an optical graft because you know that, even if you heal the perforation, the patient's going to have a scar or irregular cornea for which he'll need a graft anyway, so you can do a central large optical graft right then and there."
• Fostering teamwork. If you're dealing with a PUK due to autoimmune disease, you'll have to work closely with the individual's rheumatologist to treat both the eye and the rest of the body. This cooperation isn't always easy, however. "It can be frustrating," says Dr. Hannush. "I just saw an RA patient today who was doing great on 35 mg of methotrexate but his rheumatologist decreased it to 30 mg, and his eye flared up. When asked why his other doctor did this, he said that the rheumatologist said it was because his joints looked fine and he was doing well. However, I told him that his eye is a manifestation of his rheumatoid disease, and now that the methotrexate has been decreased, his eye has flared up. From the rheumatologist's perspective, he's treating the symptoms of the rheumatoid disease, not the [diagnostic] numbers; he's not impressed that the rheumatoid factor is very high. Even though he acknowledges that the eye is part of the body, he won't increase treatment just because the eye is inflamed. We, on the other hand, feel the ocular symptoms are symptoms of uncontrolled rheumatoid disease. So, if the eye is inflamed, the patient doesn't need topical steroids, he needs to increase his oral steroid or switch to something like Remicade. But the rheumatologist might say, 'OK, if you want to increase their oral steroids, you manage their diabetes, their hypertension and their broken hips.' However, we ophthalmologists just want to have a partner in treating the disease."
Dr. Hannush says if a conflict over medication dosage arises, he'll usually make a call to the rheumatologist and explain the situation. Sometimes, his colleague is accommodating. Other times, the rheumatologist will balk at increasing the steroid since the patient recently broke a hip, but will be open to an alternative, such as using methotrexate in combination or cyclosporine.
In still other cases, Dr. Hannush will hit a stone wall. "This is what I'll do," the rheumatologist will say. "You do what you have to do for the eye, and I'll do what I have to do for the joints." In such cases, you have to make a decision, says Dr Hannush. "You may have to have someone else take care of the eye," he says, "or, if you've been taking care of the patient, you may have to feel the patient out to see if he'd be interested in switching to a different rheumatologist."
Though it can sometimes be difficult managing one of these patients with another physician, in many cases outside of severe Mooren's, you and your colleagues can manage peripheral thinning successfully and make sure the eye stays quiet.