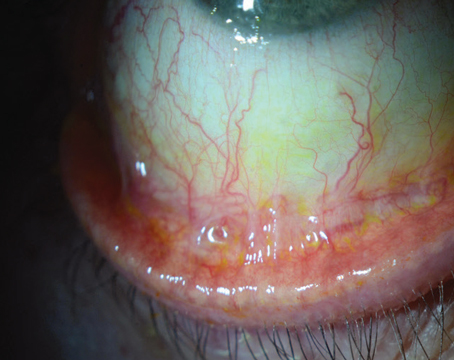
Because ocular surface issues such as dry eye can affect patients' outcomes after cataract or refractive surgery, it is important to establish a healthy ocular surface preoperatively.
A recent study conducted at Schepen's Eye Research Institute in Boston found that preoperative tear volume may affect recovery of the ocular surface after LASIK and may increase the risk for chronic dry eye.1 Additionally, a literature review found that optimizing the ocular surface before surgery decreases the incidence and severity of dry eye postoperatively.2 The literature review found that optimization of the ocular surface using artificial tears, nutrition supplements, punctal occlusion or topical cyclosporine A in patients with preoperative dry-eye symptoms decreases the incidence of more severe symptoms postoperatively.
"People with ocular surface issues can be divided into two categories: Those who have lid disease and those who don't have lid disease," says Samuel Masket, MD, who is in private practice at Advanced Vision Care in Los Angeles and a clinical professor at Geffen School of Medicine-UCLA. "In the people who don't have lid disease, we are primarily concerned with dryness because patients who have dry eye will always be more symptomatic after any ocular surgery, whether it is cataract surgery or refractive surgery."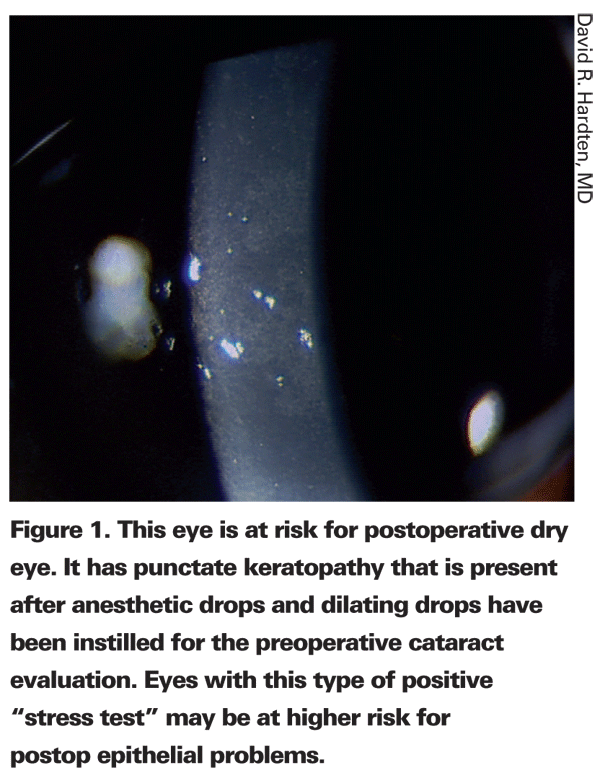
Even patients who do not have ocular surface or lid margin issues preoperatively are given a corticosteroid and an antibiotic preoperatively to prepare the ocular surface for surgery. Many surgeons also routinely use a nonsteroidal. Karl G. Stonecipher, MD, director of the
Dry Eye
Dry eye is a common condition in patients presenting for cataract or refractive surgery. Approximately 7 million Americans suffer from dry-eye disease, and the prevalence of dry eye increases with age, making it especially common in cataract surgery patients. While 6 percent of the population older than 40 suffers from dry eye, 15 percent of the population older than 65 years suffers from dry eye.
If a patient has dry eye, surgeons need to establish whether it is mild, moderate or severe. "If it is moderate to severe, the major consequence is that it can affect surgical outcomes," says William Trattler, MD, who is in private practice at the Center for Excellence in Eye Care in
Dr. Trattler treats refractive surgery patients who have mild dry eye with Restasis (cyclosporine ophthalmic emulsion 0.05%) and punctal plugs to suppress the inflammation and raise the tear film. He uses Restasis preoperatively and inserts punctal plugs on the day of surgery. For patients with moderate to severe dry eye, he inserts punctal plugs preoperatively and then treats the patients with Restasis and a short course of topical steroids.
In addition to these treatments, Dr. Masket encourages his patients with dry eye to take 2,000 mg a day of flaxseed oil.
Dr. Stonecipher doesn't hesitate to begin dry-eye treatment. "If I see any signs or if patients report any symptoms, I will initiate treatment, he says. "During the early postoperative period, if I see superficial punctate keratopathy or lissamine green stains or if the patient says that his or her vision is fluctuating, I have a low threshold to put this patient on Restasis," he explains.
For patients with moderate dry eye who can wear contact lenses but whose eyes feel dry by the end of the day, he uses Restasis for approximately a month before surgery. He and Neil McMackin, OD, recently conducted a study, as yet unpublished, showing that dry eye typically responds to Restasis within three to five weeks. Most (81 percent) of the patients included in the study had undergone LASIK. In the patients who had undergone LASIK, 29 percent reported symptom relief within one week of initiating treatment with Restasis, 65 percent reported symptom relief within three weeks, and 94 percent reported symptom relief within five weeks.
Patients with severe dry eye are treated with Restasis for two to three months preoperatively and then re-examined before proceeding with LASIK. Dr. Stonecipher notes that he prefers to re-examine and operate on these patients during more humid months to minimize their dry-eye symptoms. "We have to be careful with these patients, especially with hyperopic perimenopausal women," he adds.
A Japanese study recently presented at the 2008 annual meeting of the Association for Research in Vision and Ophthalmology found significant gender-related differences in meibomian gland physiology. (Suzuki T, et al. IOVS 2008;49:ARVO E-Abstract 92.) This study included six women in their 20s who had regular 28-day menstrual cycles and six men in their 20s. In all patients, the volume of meibum by meibometry, fluorescein tear-film breakup time, the diameter of the meibomian gland orifice using slit-lamp photography with high magnification, meibomian gland morphology by meibography, and the serum concentration of sex steroid hormones were evaluated every three to five days for five consecutive weeks.
In women, there were cyclical changes in fluorescein tear-film breakup time, the volume of meibum, meibomian gland orifice diameter and meibomian gland morphology during the menstrual cycle. Additionally, the average fluorescein tear-film breakup time was 6.8 ±0.9 seconds in women and 8.6 ±0.2 seconds in men. The volume of meibum was 0.073 ±0.014 optical density units in women and 0.117 ±0.005 ODU in men, and the meibomian gland orifice diameter was 0.174 ± 0.002 mm in women and 0.187 ±0.002 mm in men.
A separate study presented at ARVO found that both age and gender have an effect on tear film and lipid layer dynamics. (Maissa C, et al. IOVS 2008;49:ARVO E-Abstract 91.) Tear film stability was mostly influenced by age. Tear breakup time was statistically significantly shorter for presbyopes compared with non-presbyopes, but no difference was found with regard to gender. The lipid layer was significantly thinner in the presbyopic population, and the lipid layer of presbyopic women was significantly thinner than that of presbyopic men and than that of non-presbyopic women.
Hyperopic patients also present a unique challenge. "Patients with hyperopia who present in their late 20s to early 50s have latent hyperopia," Dr. Stonecipher says. "As young children, they were able to accommodate for their hyperopia, but as they have lost their accommodative amplitude and become more presbyopic, they can't take care of that residual refractive error as they could as a child. So, we find that we need to steepen that person's cornea. If you steepen it significantly, the lids may not be able to lubricate or cover the area as well as they did preoperatively. All of this is on a microscopic level, of course, but it can have macroscopic effects when dealing with the post-LASIK patient with regard to dry-eye symptoms."
For these reasons, he has been encouraging many hyperopic patients to consider refractive lensectomy rather than LASIK. However, multifocal lenses in a dry-eye patient can be problematic; therefore, the restrictions of LASIK surgery in the dry-eye patient apply with refractive lensectomy and multifocal lenses.
He tries to minimize dry eye after refractive surgery by using a nasal-hinged flap. He notes that it has been shown that using nasal-hinged flaps damages fewer nerves, which results in less severe dry eye postoperatively.
ABM Dystrophy
Dr. Masket lists anterior basement membrane dystrophy as another concern. "It can be a subtle condition or it can be very obvious," he explains. "In my practice, the patients who are referred to me for poor results with a multifocal intraocular lens often have this condition, but it has not been diagnosed. It can worsen over time and can cause irregular corneal astigmatism. It can be missed during the IOL power calculations, and it can affect the quality of vision after surgery, particularly in those patients who are candidates for premium IOLs."
Ocular Allergy
Before surgery, it is also important to control ocular allergy symptoms. According to David R. Hardten, MD, of Minnesota Eye Consultants in
Rosacea
Another condition to assess preoperatively is rosacea. According to Dr. Stonecipher, rosacea is more evident in some patients than in others. "Many times, this condition occurs in women who cover it up with makeup, so you may not be able to see it," he says. "Some patients may not know they have it, and some patients may not mention that they have it because they don't know that it will affect their refractive surgery."
He typically treats patients with rosacea for two weeks before surgery with an antibiotic/steroid combination and with 50 to 100 mg of doxycycline twice daily. He has also started using Azasite (azithromycin ophthalmic solution 1%, Inspire Pharmaceuticals) in these patients because of its anti-inflammatory properties. He also recommends lid hygiene preoperatively. Previously, he routinely used baby shampoo or a dandruff shampoo, but he currently prefers lid foams.
Blepharitis/MGD
The most common lid issue affecting cataract and refractive surgery patients is blepharitis or meibomian gland dysfunction. This lid condition affects the quality of the tear film, which can affect the surgical outcome.
"If MGD is present, I will start cataract or refractive surgery patients on Azasite once a day at bedtime and warm compresses," Dr. Trattler says. "Then, I have them return in three to four weeks for a re-examination. After achieving improvement in the MGD, we typically get better readings on our preoperative tests. Sometimes, treatment of MGD requires a delay in scheduling surgery, but if you achieve a better postoperative result, it is worth waiting." He also recommends oral omega-3s in these patients.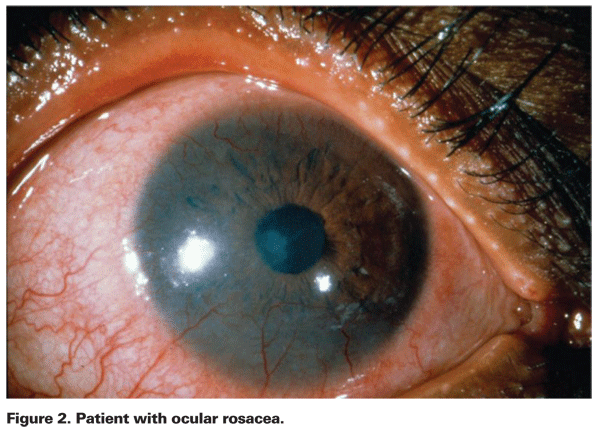
Dr. Masket has found that blepharitis patients typically require treatment with topical agents for at least a week. In some cases, systemic agents may be required to control the condition. "It has been my pattern to treat anterior blepharitis with bacitracin ointment, but recently I have also evaluated the benefits of Azasite," he says. "This is a very viscous agent that tends to stick well on the lid margins. I have also had good results with bacitracin over the years. For posterior margin disease that requires a steroid, I use Zylet (loteprednol etabonate 0.5% and tobramycin ophthalmic suspension, Bausch & Lomb) or TobraDex (tobramycin and dexamethasone ophthalmic suspension, Alcon). In some cases, patients will need to take oral doxycycline if their disease does not respond to topical agents."
Dr. Stonecipher has found that Restasis and Azasite are effective for patients with blepharitis. He also recommends lid hygiene as previously described for a week or two before surgery. "Most meibomian gland disease is so mild that perioperative treatment will take care of it," he says. "But the person with more serious blepharitis or meibomian gland dysfunction will receive treatment similar to that of the rosacea patient. If these patients are not quite where they need to be on the day of surgery or if they are noncompliant, don't hesitate to postpone surgery."
Dr. Hardten recommends lid scrubs the night before and the morning of surgery for all patients, not just those with lid margin concerns. For patients with significant blepharitis or dry eye, he tailors the treatment to the individual patient. Treatment typically starts two to four weeks preoperatively and may include hygiene, tears, ketoconazole shampoo, Restasis, Azasite to the lids, doxycycline and steroids.
He also notes that some lid malpositions should be analyzed and possibly surgically corrected before cataract surgery. These malpositions are uncommon in the refractive surgery population because of these patients' younger age. Lid issues to look for include entropion/ectropion, floppy lids and lagophthalmos.
1. Konomi K, Chen LL, Tarko RS, et al. Preoperative characteristics and a potential mechanism of chronic dry eye after LASIK. Invest Ophthalmol Vis Sci 2008;49:168-174.
2. Ambrosio R Jr, Tervo T, Wilson SE. LASIK-associated dry eye and neurotrophic epitheliopathy: pathophysiology and strategies for prevention and treatment. J Refract Surg 2008;24:396-407.