Dry eye is pervasive among my patients. I would estimate that at least 15 percent of my overall patient population suffers from dry eye, but the rates are much higher among key sub-groups including: those with autoimmune disorders or acne rosacea; contact lens wearers; patients taking certain systemic medications, such as antihistamines, beta blockers and antidepressants; and those who are post-LASIK or post-cataract surgery.
The good news for those who suffer from dry eye is that this once "boring" condition is suddenly the topic du jour at professional ophthalmology meetings. Higher patient expectations, multifocal intraocular lenses, new research, new instruments that measure corneal wavefront aberrations, higher-quality tears, omega-3 vitamins and new anti-inflammatory therapies have all contributed to the buzz about dry eye.
The downside is that most of these new treatments are quite expensive for patients, requiring ongoing compliance with drops and/or oral supplements that often don't fully resolve their symptoms. Furthermore, I am not convinced that inflammation is truly the culprit for many older dry-eye patients, particularly given my underwhelming experience thus far with topical cyclosporine therapy in patients older than 50 years. Certainly, there are patients who benefit from inflammatory suppression. Younger dry eye patients, those with autoimmune disorders, patients with very advanced symptoms or obvious conjunctival inflammation and injection are good candidates for Restasis and/or topical corticosteroids.
But the majority of dry-eye patients may simply have age-related cicatricial changes to the lacrimal glands,1 perhaps compounded by systemic medications2 or preserved topical agents3 that prevent them from producing sufficient tear volume. As the tear volume decreases, the concentration of inflammatory mediators in the tears rises. Patients then rub their uncomfortable eyes, releasing more inflammatory cytokines. So, while there is sub-clinical inflammation, we may be able to resolve it without the expense, hassle and potential side effects of anti-inflammatory therapy.
Punctal occlusion has previously been reported to be very effective for the treatment of dry eye, relieving symptoms and enabling patients to reduce their use of lubricants.4,5 I have had excellent results with punctal plugs in the past and wanted to measure in a more meaningful way the benefits of punctal plugs in my patients with dry-eye syndrome.
Prospective Study
I undertook a prospective, non-randomized study of punctal plugs in patients who had failed artificial tears and had chosen to try punctal occlusion after an explanation of several alternative options.
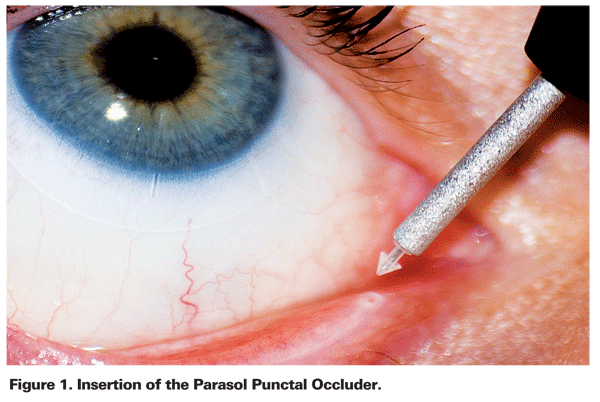
A total of 108 patients (216 eyes) with symptoms of dry eye and Schirmer scores <10 mm were enrolled. The average age was 63 ±14 years. None of the subjects were using any other topical drops or oral supplements for dry eye. Parasol Punctal Occluders (Odyssey Medical) were inserted bilaterally in all subjects (See Figure 1). Patients were seen for a follow-up visit two to four weeks after insertion of the plugs, and again at one year.

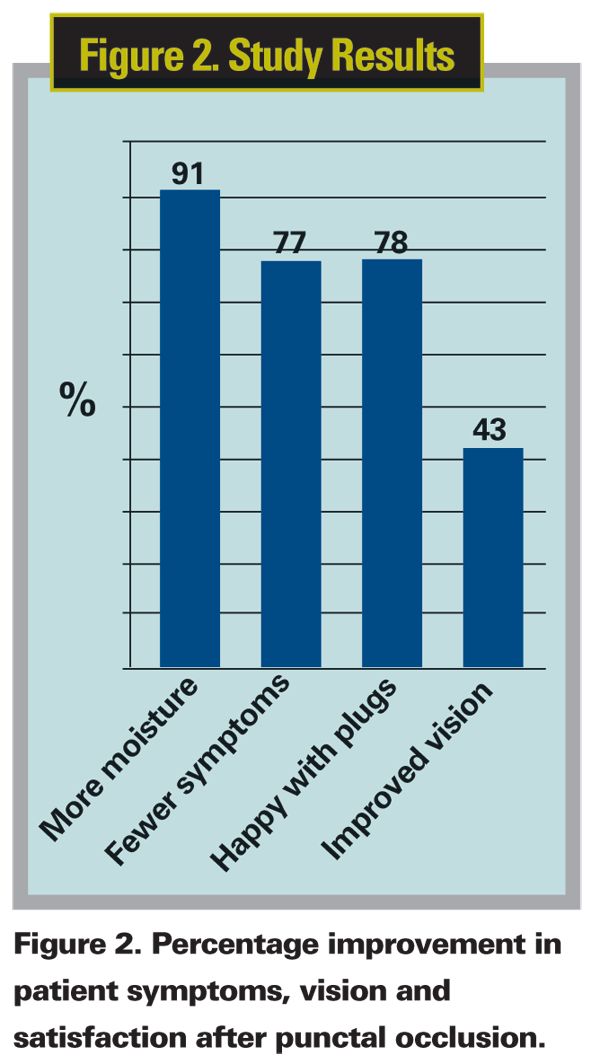
At the first follow-up visit, 91 percent of patients reported that their eyes had more moisture, and 77 percent said they had fewer dry-eye symptoms (See Figure 2). Most (78 percent) were very pleased with the plugs, which is a much more positive response than I have seen anecdotally to cyclosporine therapy. Additionally, Snellen acuity improved by one or more lines (average of two lines improvement) in 43 percent of the eyes. These gains in comfort and vision held steady at the one-year visit.
Plug retention was very high, at 92 percent. Of the 8 percent of plugs that were lost, the average retention was 70 days, with a mean of 21 days. In several prior studies, the reported plug retention rates have been much lower, between 49.3 percent and 69.5 percent.4-7 The higher retention rate in my study may be due to a combination of proper sizing and insertion, plug quality and patient education (See sidebar).
Better Vision
The positive impact of punctal occlusion on visual acuity in this study is very exciting, although it is not a total surprise. The tear film is the first refracting surface of the eye, so it stands to reason that it would affect acuity. We know, too, that fluctuating vision is a common symptom of dry eye and that dry eye is a major source of patient dissatisfaction with refractive surgical results.8
In fact, there is a growing body of evidence in the refractive surgery literature that treating dry eye (with plugs or otherwise) has benefits in terms of visual outcomes and patient satisfaction. For example, researchers at the New York Eye & Ear Infirmary recently reported that patients considering refractive surgery for very low refractive errors were able to achieve sufficient visual improvement with plugs alone.9 In this study, 18 of 21 eyes had a one- to three-line improvement in visual acuity one month after punctal plug insertion. Only one patient went on to have refractive surgery.
Another group reported that dry eye increased the risk for regression after refractive surgery.10 That regression may have just been dry-eye-related reduced acuity. Punctal occlusion has also been shown to significantly reduce higher-order aberrations in post-LASIK eyes.11
In treating dry eye, we tend to measure improvements in tear breakup time (TBUT), corneal staining or ocular surface disease index (OSDI) scores. But from the patient's perspective, an improvement in vision is the most satisfying result.
Advantages of Punctal Occlusion
As part of our armamentarium for the management of dry eye, punctal plugs have a number of advantages. They are generally covered by insurance, so the financial burden for the patient is low, yet the physician is fairly compensated for their insertion. Plugs are not dependent on patient adherence or dexterity for efficacy and, in fact, reduce the burden of compliance on patients by reducing the need for artificial lubricants.4,5,12
Punctal occlusion is reversible and, with most types of plugs, the safety profile is very high, with epiphora, conjunctival irritation and extrusion typically being the only complications.
There is no single, best "recipe" for treating the dry-eye patient. As clinicians, we should do our best to determine the underlying etiology of the disorder and treat accordingly, tailoring dry-eye therapy to the needs and personality of the patient, his financial situation and the clinical presentation. Certainly, there remains an important role for punctal occlusion in such a paradigm.
Dr. McCabe is a clinical instructor at
1. Obata H, Yamamoto S, Horiuchi H, Machinami R. Histopathologic study of human lacrimal gland. Statistical analysis with special reference to aging. Ophthalmology 1995;102:678-86.
2. 2007 Report of the International Dry Eye WorkShop (DEWS). The Ocular Surface 2007;5(2).
3. Broadway DC, Grierson I, O'Brien C, Hitchings RA. Adverse effects of topical antiglaucoma medication: 1. The conjunctival cell profile. Arch Ophthalmol 1994;112:1437-45.
4. Tai MC, Cosar CB, Cohen EJ, et al. The clinical efficacy of silicone punctal plug therapy. Cornea 2002;21:135-9.
5. Balaram M, Schaumberg DA, Dana MR. Efficacy and tolerability outcomes after punctal occlusion with silicone plugs in dry eye syndrome. Am J Ophthalmol 2001;131:30-6.
6. Horwath-Winter J, Thaci A, Gruber A, Boldin I. Long-term retention rates and complications of silicone punctal plugs in dry eye. Am J Ophthalmol 2007;144:441-4.
7. Burgess PI, Koay P, Clark P. SmartPlug versus silicone punctal plug therapy for dry eye: A prospective randomized trial. Cornea 2008;27(4):391-4.
8. Levinson BA, Rapuano CJ, Cohen EJ, et al. Referrals to the Wills Eye Institute Cornea Service after laser in situ keratomileusis: Reasons for patient satisfaction. J Cataract Refract Surg 2008;34:32-9.
9. Khalil MB, Latkany RA, Speaker MG, Yu G. Effect of punctal plugs in patients with low refractive errors considering refractive surgery. J Refract Surg 2007;23(5):467-71.
10. Albietz JM, Lenton LM, McLennan SG. Chronic dry eye and regression after laser in situ keratomileusis for myopia. J Cataract Refract Surg 2004;30:675-84.
11. Huang B, Mirza MA, Qazi MA, Pepose JS. The effect of punctal occlusion on wavefront aberrations in dry eye patients after laser in situ keratomileusis. Am J Ophthalmol 2004;137:52-61.
12. Roberts CW,