For several years now, some patients with reduced vision due to conditions such as age-related macular degeneration have been able to benefit from having an Implantable Miniature Telescope placed inside the eye. Unfortunately, because the device is a Galilean-style telescope, it can't be reduced in size beyond a certain point; nearly the entire cornea must be lifted to implant it, and it obstructs peripheral vision. The latter limitation prevents it from being feasible as a binocular implant and makes it difficult to examine or treat the retina after implantation.
Now, however, the inventor of the IMT, Isaac Lipshitz, MD, chairman and CEO of OptoLight Vision Technology in
How It Works
Unlike the IMT, the new IOL, called the Lipshitz Macular Implant (LMI), is similar to a standard IOL—just a little thicker. Encased inside the IOL are two miniature mirrors in Cassegrain telescopic configuration. (See image, below.) The posterior, doughnut-shaped mirror captures light coming into the central visual field and focuses it onto the anterior, retina-facing mirror—a smaller, circular mirror located in front of the "doughnut hole." The smaller mirror focuses the light back onto the retina, causing the object of regard to be enlarged about two and a half times. Light passing through the area around the mirrors is unaffected, leaving peripheral vision undisturbed. The result is that the patient sees a magnified central image and a normal, non-magnified periphery. Because of the optics, the image is continuous and the patient is visually unaware of the mirrors.
"Essentially, when a patient with this lens goes into the supermarket, everything will appear at normal size except objects that the patient looks directly at," explains Dr. Lipshitz. "These will appear magnified. But because peripheral vision remains normal, navigation is unaffected." He also says that the brain doesn't seem to have trouble with the central image being magnified. "The patients are ecstatic," he reports. "They function very well."
In its prototype version, the optic of the IOL is about 6.5 mm; the posterior mirror is about 2.8 mm in diameter, while the anterior mirror is about 1.4 mm. "All the components of the lens are biocompatible," explains Dr. Lipshitz. "The mirrors are dielectric—they're made of multiple layers of titanium oxide and silica oxide, and they're about 1 to 1.5 microns thick." 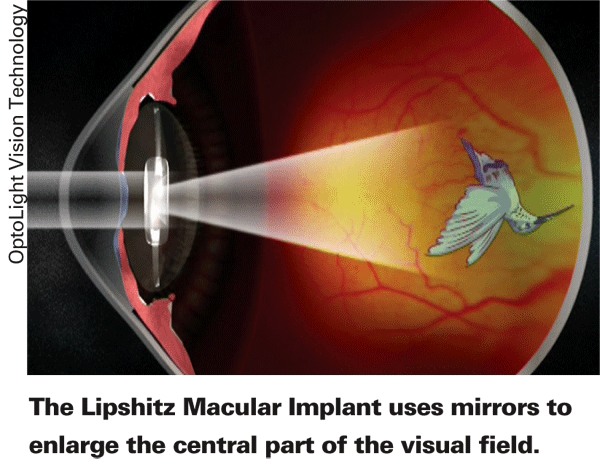
Dr. Lipshitz notes that because the lens is projecting the image onto the retina, many variations are possible. "It's a bit like a projector television, which can project the image onto a wall and change its size, contrast, prismatic characteristics and location," he says. "For example, if a patient has hemianopsia, this lens can both enlarge the image and project it onto the functioning part of the visual field."
Dr. Lipshitz adds that although the lens will be available in more than one size to accommodate the internal dimensions of the eye, the lens is not intended to correct refractive error; that will have to be accomplished with glasses. "Glasses can also be used to increase the magnification factor if the patient has deteriorated," he says.
Implanting the LMI
Amar Agarwal
"The lens is only slightly thicker than a normal IOL, so implanting it is not very difficult, unlike the earlier option," he notes. "This lens should work well bilaterally, and it doesn't restrict our view of the fundus. We've been able to examine the patients' retinas postop very comfortably. In fact, we can do angiography or use argon laser."
Both Dr. Lipshitz and Prof. Agarwal note that an important part of patient evaluation involves having the potential patient try using an external telescope. "If he doesn't do better with the external telescope, then magnifying the image is not a helpful solution," says Prof. Agarwal.
Results of Early Cases
Prof. Agarwal says that outcomes with the early implants have been very good. "It's important to understand that we're not talking about normal patients," he points out. "These patients are nearly blind, so this is a last resort for them; if we can make them 20/100 instead of counting fingers, that is a major improvement. Of course, we counsel them so they understand the realities of the situation.
"We've implanted six eyes so far," he continues. "The first patient has had the lens for more than a year. We've seen no internal reaction to the lens, and the optical results have been very good. We did an endothelial study to see if the LMI was causing any damage and found nothing significant. We checked each eye with anterior segment OCT, and lens position was good in all cases. We also checked perceived quality of life pre- and post-surgery; every patient has been very happy with the outcome." An article describing the detailed results for all six patients has been accepted for publication in an upcoming issue of the Journal of Cataract and Refractive Surgery.
"I haven't had any feedback that it took patients time to adjust to having a larger image in the center," he adds. "And patients have no problem using both eyes at once." In fact, Dr. Lipshitz believes the IOL should be ideal for bilateral implantation, noting that two patients in
What's Next?
Drs. Lipshitz and Agarwal agree that using mirror technology inside the eye creates a lot of possibilities for treating diseases beside AMD, given its ability to alter the location, size and characteristics of the central image. "The LMI may help patients with macular dystrophies as well," says Prof. Agarwal. "This is just the tip of the iceberg."
Dr. Lipshitz says he's working on a new, "more elegant" design that hasn't been tested in human eyes yet. "The first prototype was designed to prove the concept and make sure that patients could really see," he explains. We're working on an advanced version right now that employs a totally different construction." In addition, he says his company is working on a virtual reality unit that will allow prospective patients to experience what vision will be like with the lens implanted. Beyond that, Dr. Lipshitz expects future designs to have a dynamic element that will let the mirror move or change its curvature. "This might even provide a way to treat presbyopia," he says.
In terms of when the lens will be commercially available, Dr. Lipshitz hopes to obtain the CE mark for the LMI in the second quarter of 2008. "We're already starting to work with the FDA," he says. "We're planning to do Phase One testing in



