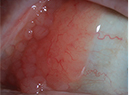
A 17-month-old Caucasian male presented for evaluation of a cyst on his left iris. The cyst had been forming on the inferior aspect of his iris over the past several weeks, causing superotemporal displacement of the pupil. The patient’s parents had noted their son to have worsening vision and photophobia in the left eye, causing difficulty in compliance with recommended patching of the right eye.
Medical History
The patient was otherwise healthy and with normal development. There was no relevant medical history. He was not taking medications. Family history was noncontributory.
Nine months prior to presentation, the patient sustained an accidental traumatic injury to the left eye, caused by a kitchen knife piercing the left eye. The knife dropped from his mother’s hand while she was cutting cooked chicken sprinkled with pepper. The patient presented two days after the initial injury when he developed redness of the left eye. Exam at this time revealed a 4-mm superotemporal, full-thickness, corneal laceration with a peaked pupil and iris prolapse. The anterior chamber was otherwise normal. The ruptured globe was repaired at an outside facility with five interrupted 10-0 nylon sutures. He healed well after his surgery and patching of the right eye was initiated. Six months after initial repair, an inferior iris cyst was noted, prompting a referral to Wills Eye for further evaluation.
Examination
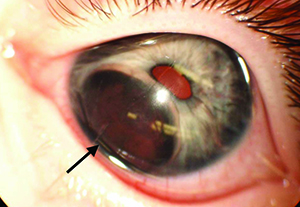 |
| Figure 1. RetCam photograph of the left eye showing a large inferior iris cyst (arrow) causing superior displacement of the pupil. |
Please click this link for diagnosis, workup, treatment and discussion.