Collagen vascular diseases comprise a group of autoimmune diseases in which the body’s own immune system attacks connective tissues, skin and organs. Examples include rheumatoid arthritis, systemic lupus erythematosis, Sjögren’s syndrome and scleroderma. While blanket prevalence estimates are hard to come by, arthritis and rheumatic conditions present large public-health challenges.1 So it stands to reason that some patients looking for laser corneal refractive surgery will have one (or more) of these conditions. Should you always turn them away? Below, an expert corneal refractive surgeon shares his thoughts on balancing his duty to protect his patients with allowing a select few to have these procedures.
Until fairly recently, operating on CVD patients was practically verboten, according to Majid Moshirfar, MD, FACS, research director of the HDR Research Center and professor of ophthalmology at the University of Utah’s Moran Eye Center. The FDA’s original approval of LASIK designated CVDs and autoimmune diseases as absolute contraindications, although many surgeons currently consider them a strong, but relative, contraindication in affected patients. At the time FDA approval studies were done for LASIK and PRK, known CVD patients were excluded and, as a group, tended to present clinically as more symptomatic than they do now. “There was a time when our patients with RA, for example, were not really controlled with any medication and were pretty sick, so they didn’t really even ask for such refractive surgeries,” Dr. Moshirfar recalls.
“But as refractive surgery outcomes and predictability became better thanks to the increasing precision of equipment and lasers, people began asking themselves, ‘Now that the flaps are better and we have better ways of doing things, why not try?’ ” he continues, adding that rheumatologic treatments for CVD have also improved. “Rheumatologists can now diagnose these patients at much younger ages, when they’re healthier. They can also treat them with immunosuppressive and immune-modulating medications that were previously unavailable,” he says.
“I remember when Robert Maloney co-wrote a paper2 about a group of patients with CVD,” Dr. Moshirfar continues, citing a 2006 study that followed 49 eyes that underwent LASIK in patients with conditions including SLE, RA and psoriatic arthritis over a period spanning more than six years. The authors concluded that LASIK could be safe for patients with autoimmune diseases under good control. “That was one study that helped make it seem a little bit more acceptable for these patients to undergo refractive surgery,” he says.
Dr. Moshirfar emphasizes that the literature on refractive cornea surgery in CVD remains “very skimpy,” however, cautioning,“There’s no reason to get on a loudspeaker and offer LASIK to patients with lupus, for example. We must not be cavalier about doing corneal refractive surgery on patients with CVD.”
To be considered for these surgeries, Dr. Moshirfar has a list of criteria patients must meet:
• The treating rheumatologist must be involved. CVD patients with good topographic maps, TBUT, staining, and no sign of cataract formation must also be in active treatment with a rheumatologist. “The ophthalmologist needs an official document from the rheumatologist acknowledging that the patient wants to undergo surgery. You need a new rheumatologic examination and a new titer of serologic testing. The rheumatologist needs to certify that the patient hasn’t had a relapse of any systemic problems in their body or joints in the last 18 months, in my opinion,” says Dr. Moshirfar.
• Find out why the patient wants LVC—and give strong warnings. “Once patients meet the medical conditions, you as a physician need to find out why the patient is looking for surgery,” says Dr. Moshirfar. “Are they contact-lens intolerant? If not, that makes things somewhat more promising; but if they are becoming contact-lens intolerant, then you need to really dwell on the question of whether or not to do this surgery.
“Do not be cavalier in making recommendations,” he warns. “These procedures are still a strong relative contraindication in these patients. I always tell them, ‘You may go blind. You may develop corneal melt. You may need a corneal transplant. Your life may change as a result of this.’ I say that to all my patients—and most definitely to patients in this category.” After this conversation, Dr. Moshirfar sends patients home for further deliberation. “I tell patients to go home and talk with family, and to really think about it before calling us back,” he says. “Don’t let patients make the decision on the spot right after you’ve talked to them.”
• Enhance your informed consent. A key element of Dr. Moshirfar’s due diligence is customized informed-consent language. “I write into the informed consent that the laser that we’re going to use is not FDA-approved for patients with autoimmune diseases; that w
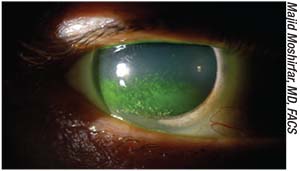 |
| Keratoconjunctivitis sicca due to Sjogren’s syndrome. Although select CVD patients may be able to safely undergo LVC, SS may remain strongly contraindicated. |
e have very limited literature, and that we currently don’t know what the long-term results will be. Then I sign it and have the patient countersign it. This is an addendum to the standard informed consent,” he says.
• Choose the procedure wisely. Dr. Moshirfar prefers LASIK to PRK for these patients, and it appears he’s not alone. On the question of whether to perform LASIK or PRK on patients with CVD, A 2014 review of the literature on laser vision correction in CVD and other conditions led the authors, from the Wilmer Eye Institute, to lean towards LASIK over PRK due to LASIK’s faster healing time in corneas with potentially compromised epithelial cells, and LASIK’s relatively lower risk of stromal haze and scarring in these eyes.3
“I think PRK carries a higher risk of stromal reactions, melt, thinning and necrosis of the keratocytes. In LASIK, the boundary of the epithelium is not insulted as much,” he says. “With PRK you’ve taken the epithelium and Bowman’s layer off; for six or seven days, the stroma is exposed, even though you place a bandage contact lens. I’m not saying you can never do PRK on a patient with RA, but if I ever had to do a refractive procedure on a patient with well-controlled RA, I’d prefer to do SMILE or LASIK.”
Although he hasn’t performed SMILE on any CVD patients, Dr. Moshirfar has on patients with subclinical dryness on the ocular surface; patients with lagophthalmos; and Bell’s palsy patients. “There are patients who will walk into our offices with Sjögren’s syndrome, RA, and SLE, and we’ll likely decide that we don’t want to give them LASIK. But what about SMILE? When you do LASIK on these patients, you’re cutting the corneal nerves and creating a neurotrophic keratopathy, and they may not heal as well as other patients. Maybe SMILE would be better because instead of creating a 270-degree incision all the way around, you’re just making a little 30-degree incision superiorly underneath the eyelid, possibly reducing the risk of a problem,” he says.
• Treat topically and systemically. “If you proceed with any laser vision correction, you’ll have to aggressively optimize the corneal surface. Studies suggest that if you put these patients on cyclosporine, you improve the nerve-growth factors,” says Dr. Moshirfar. “You basically do the surgery on several weeks of prior cyclosporine. After surgery, if these patients become a lot drier than expected, that’s when you need to be aggressive. You basically throw everything but the kitchen sink at them: I think that these patients respond really well to tacrolimus 0.03% or 0.01%. I sometimes also put these patients on 5% albumin. I also think blood serum has a role, but not at 20%—more like 50%—for these patients. Plug them, and use both oil-based and aqueous artificial tears. If we don’t respect the integrity of the epithelium within the first eight to nine weeks postop, these patients will definitely regress and become more myopic, and they will not only have very bad UCDVA; they will also have very poor best-corrected vision,” he emphasizes.
Increased risk of corneal melt means that topical NSAIDS need to be used judiciously, if at all. Signs of melt should prompt a call to the rheumatologist to discuss doubling up on immunosuppressant drugs, says Dr. Moshirfar. “If they develop a flap-edge necrosis and start to have actual melts, you need to topically and systemically ramp up everything,” he says. “You most likely need to talk with the rheumatologist and increase the dosages of the existing immunosuppressants. Working with the rheumatologist, add another medicine to the existing medications. Let’s say they’re on methotrexate; add Cellcept to it. If they’re on Cellcept, add valproic acid. Also immediately put them on oral prednisone, usually 1 to 5 mg/kg/day, for anywhere from two to 10 weeks. The systemic steroid is important in the acute phase of exacerbation.”
Amped-up immunosuppression can create additional risks, however, including postop herpes. “These patients are at risk for viral keratitis and bacterial infections, especially during the acute phase, specifically because they’re immunosuppressed. In doing LASIK on these patients, I haven’t had a case like that, probably because they’re on steroids for a short interval. But I’ve had patients referred to me who were on long-term topical steroid drops, and they can run into problems,” says Dr. Moshirfar.
Dr. Moshirfar has also seen on referral the results of ill-advised laser corneal refractive surgery. “Unfortunately, I’ve encountered that,” he says. “The patient had scleroderma, which in my opinion is an absolute contraindication to corneal refractive surgery. This patient had definite scleroderma findings that you could see even without a workup. In cases like this, you need to use contact lenses; sometimes you have to use therapeutic bandage contact lenses. The patient may even need to be fitted long-term with the PROSE contact lens (BostonSight; Needham, Massachusetts).”
The Unknowns Persist
The only consensus on corneal refractive surgery in CVD appears to be that the research must evolve. The review of the literature conducted by researchers at the Wilmer Eye Institute led them to conclude that patients with mild and well-controlled CVD with no history of ocular involvement; no systemic multidrug regimen; a minimum of six months without symptom flare; clearance from a treating rheumatologist and/or uveitis specialist; normal preop testing, including Schirmer’s and TBUT; and informed consent regarding the off-label nature of LASIK and PRK for them, may be suitable candidates.3 The authors also recommended that patients have negative serology for Sjögren’s, and concluded that a large, multicenter, controlled trial should take place examining the safety and efficacy of LRS for patients with CVD and other systemic diseases. A 2016 retrospective case series looking at a larger population of patients with CVDs (622 patients; 1,224 eyes) led the authors to conclude that excimer laser refractive surgery could be safely performed on patients with well-controlled disease, although they recommended against it for Sjögren’s patients or patients with keratoconjunctivitis sicca.4 The authors also acknowledged the study’s retrospective nature as a limitation.
Dr. Moshirfar says that LVC patients with CVDs and other autoimmune diseases are not as uncommon as one might think, and agrees that they merit more study. “We all have a few such patients that have undergone surgery, and some are 10 or 15 years out,” he says. “If you talk with a group of surgeons, you’ll hear, ‘Yeah, I have patients like that.’ We need to collect more data in order to help the literature advance.” REVIEW
Dr. Moshirfar reports no relevant financial interests.
1. Helmick CG, Felson DT, Lawrence RC, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part I. Arthritis Rheum 2008;58:1:15-25.
2. Smith RJ, Maloney RK. Laser in situ keratomileusis in patients with autoimmune diseases. J Cat Refract Surg 2006;32:1292-5.
3. AlKharashi M, Bower KS, Stark WJ, Daoud YJ. Refractive surgery in systemic and autoimmune disease. Middle East Afr Ophthalmol 2014;21:1:18-24.
4. Schallhorn JM, Schallhorn SC, Hettinger KA, Venter JA, et al. Outcomes and complications of excimer laser surgery in patients with collagen vascular and other immune-mediated inflammatory diseases. J Cat Refract Surg 2016;42:1742-52.



