 |
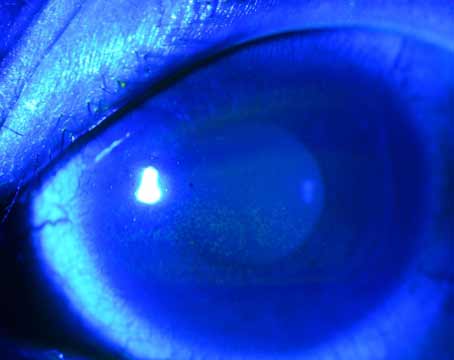
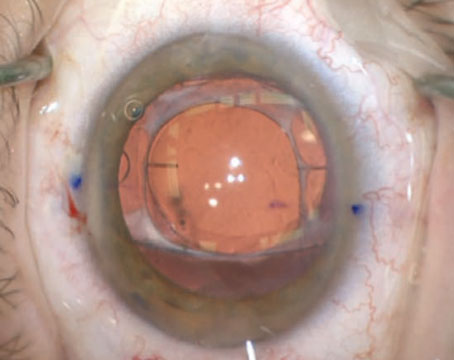
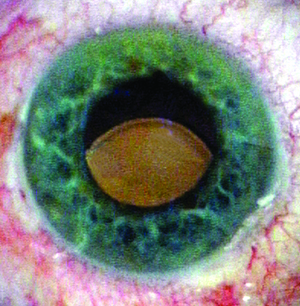
| Figure 1. Sunsetting three-piece IOL placed in the ciliary sulcus. (All images courtesy Richard Hoffman, MD.) |
Most cataract procedures are performed with no complications. The IOL is placed securely in the capsular bag, and it stays there for the duration of the patient’s life. However, in some cases, the IOL can become dislocated to the point where a secondary intervention is required. In this article, expert surgeons share the techniques they use when faced with a dislocated lens.
The Scope of the Problem
According to Richard Hoffman, MD, who is in practice in Eugene, Oregon, IOL dislocations can be divided into five categories:
• A lens that’s decentered within an intact capsular bag.
• An IOL that’s partially
• A lens that’s in the sulcus, so there is a compromised capsular bag. The lens is in the sulcus, and that lens is decentered.
• An IOL that’s in the capsular bag, and both are
• An IOL that’s completely dislocated and is sitting on the retina.
“Each of these can be approached using multiple techniques, so there isn’t one best technique for all scenarios,” Dr. Hoffman explains.
Uday Devgan, MD, who is in practice in Los Angeles and a professor at UCLA, notes that the operative report from the original cataract surgery can help determine whether there were complications. “Determine if the IOL was placed in the capsular bag, or perhaps in the ciliary sulcus. Loose zonules may have been noted during the original procedure. Was the case uneventful or was there a posterior-capsule rupture? Finally, note which type of IOL was placed and its dioptric power,” he says. Videos of how to manage dislocated IOLs can be seen on Dr. Devgan’s website: cataractcoach.com.
Decentered IOL in the Bag
Some IOLs are decentered but still in the bag. This can occur spontaneously or as a result of trauma.
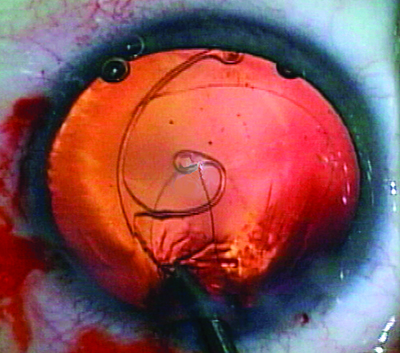 |
| Figure 2. Ahmed segment with 9-0 Prolene suture being placed in the capsular bag following cataract extraction. |
“The classic example of this is pseudoexfoliation syndrome,” says Alan Crandall, MD, senior vice-chair of Ophthalmology and Visual Sciences, and director of
For a decentered IOL within an intact capsular bag, Dr. Hoffman says the best approach is to
Partially Subluxed IOL
If an IOL is partially in the capsular bag and partially out of the capsular bag, Dr. Hoffman says he would
An IOL in the Sulcus
If a three-piece lens is placed in the sulcus without any type of fixation, the lens will stay centered most of the time. On occasion, the IOL will work its way through the zonules and become decentered. “For these lenses, I will iris-fixate them with 9-0 or 10-0 Prolene,” Dr. Hoffman explains.
He adds that management also depends on the presentation and type of IOL. If there’s a single-piece lens in the sulcus, it typically needs to be replaced with a three-piece lens. “For patients with
Decentered IOL and Bag
In-the-bag posterior chamber IOL dislocations can be managed by exchange with an anterior chamber IOL or by repositioning the posterior chamber IOL.1
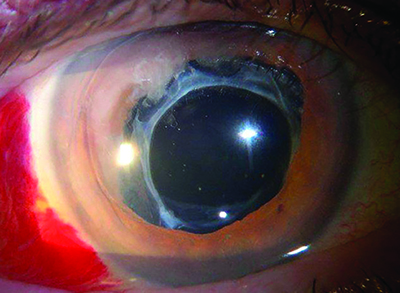 |
| Figure 3. IOL with capsular tension ring |
For the scenario in which the IOL is in the capsular bag and the whole bag has come loose and
In these cases, the lens does well for 12 to 14 years after routine cataract
Dr. Crandall notes that his treatment of choice depends on the IOL that has been implanted and the patient’s vision before surgery. “If the patient’s vision was good, the IOL is not damaged and the bag is intact or has a capsular tension ring, I would identify the optic-haptic junction either intraoperatively or preoperatively,” he explains. “I would then mark 180 degrees from that, open up the conjunctiva, clear off back to 3 to 4 mm posterior, and then find the surgical limbus and go 2 mm posterior to that and make an incision into the sclera,” he explains.
Then, he makes a lasso, lassoes the lens and the secures it to the sclera with 8-0 Gore-Tex, which is an off-label use, or with 9-0 or 10-0 Prolene sutures. He notes that there are a few different ways to accomplish this. One example is an ab
Garry Condon, MD, professor of ophthalmology at the Drexel University College of Medicine, Allegheny Program, in Pittsburgh, Pennsylvania, has described a simplified modification to the ab
A description of Dr. Condon’s technique: Under anesthesia, he creates a
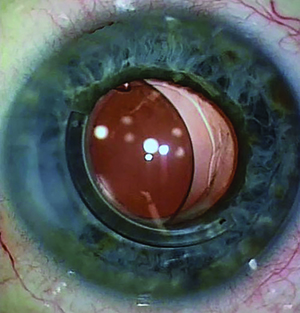 |
| Figure 4. Pseudophakic eye with |
The surgeon then uses Sharp Westcott scissors to create a 3-mm vertically oriented, temporal, conjunctival and Tenon’s capsule dissection 2 mm posterior to the limbus. Then, a diamond blade is used to create a 3-mm, one-third-thickness scleral groove 2 mm posterior to the limbus. Next, at one end of the partial-thickness groove, a single 1-mm,
The surgeon then passes a 9-0 polypropylene double-armed suture on a long curved needle (D8229, Ethicon) through the margin of the partial-thickness scleral groove opposite the stab incision, up through the optic-haptic portion of the IOL-capsular bag complex, and out the peripheral cornea. If the needle won’t pass easily through the complex, the surgeon can apply counter traction with an intraocular microforceps to ensure successful passage of the needle. Then, a 30-degree iris hook is passed through the full-thickness scleral incision to retrieve the polypropylene suture anterior to the posterior capsule IOL-capsular bag complex.
The surgeon then cuts the needle so the suture can be tied at the scleral groove. To allow subsequent IOL centration, a slipknot is placed, and the same process is repeated at the nasal aspect to secure the fellow optic-haptic portion of the IOL-capsular bag complex. The nasal polypropylene suture needle pass and 1-mm stab incision for suture retrieval counter the temporal sites to prevent IOL tilt. The surgeon adjusts the suture tension on both haptics to center the IOL before securing and burying the knots. A single buried 8-0 polyglactin suture is used to close the conjunctiva. Also, limited 23-gauge pars plana vitrectomy either early or at the conclusion of fixation may be necessary, depending on the extent of vitreous involvement with the dislocated IOL-capsular bag complex.
According to Dr. Crandall, another option is to go underneath, the same way as described above, but then dock the lens with a 26- or 27-ga needle inserted through a stab incision 180 degrees away. “Then, you pull that out and reverse it,” he says. “This time, you go above the bag and just outside. Both options are easy and fast, and they work very well. Then, you’ve secured the IOL complex.”
However, if the patient’s preoperative vision wasn’t good or the lens is damaged, the surgeon may need to do a lens replacement. “If it’s an older PMMA lens, then you must make an incision that’s at least 5, 5.5, or maybe 6 mm depending on the implant,” Dr. Crandall advises. “Once the old lens has been removed, you can implant a lens like the Alcon CZ70BD, which is a large PMMA lens that has eyelets on it. You just put the lens in, and you’ve already got sutures through the eyelets. You pull them out posterior to the limbus. In this case, you’ve obviously made a large incision that will require sutures. It works well, but it’s not the preferred technique because these eyes usually have some other issues, and you’re risking glaucoma, infections, et cetera.”
IOL Lying on the Retina
In cases where the IOL is completely dislocated onto the retina, Dr. Hoffman coordinates with a retina specialist. “If it was a three-piece lens, the retina specialist would do a vitrectomy and pull the lens up, and then I would iris-fixate it,” he says. “But, I don’t do that anymore because
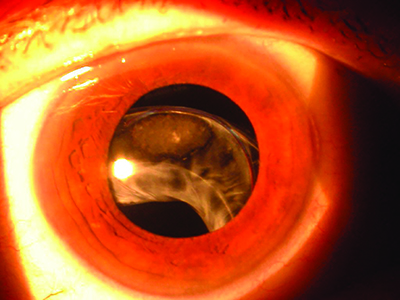 |
| Figure 5. Subluxed IOL/capsular bag/capsular tension ring in a patient with pseudoexfoliation. |
The lens tends to move around a lot and sometimes causes chronic hyphemas or uveitis. So, in those situations, I now have the retina surgeon bring the lens up into the anterior chamber, and then I remove the lens. Then, I will scleral-fixate a new lens using a scleral incarceration technique. The latest one is the Yamane technique.”
The Yamane technique for transconjunctival
Preoperatively, the mean best-corrected visual acuity was 0.25 logMAR units (around 20/35 Snellen), which significantly improved postoperatively to 0.11 (slightly worse than 20/25) at six months, 0.09 (slightly worse than 20/24) at 12 months, 0.12 (20/26) at 24 months, and 0.04 (slightly worse than 20/20) at 36 months.
Mean corneal endothelial cell density decreased from 2,341 cells/mm2 preoperatively to 2,313 cells/mm2, 2,240 cells/mm2, 2,189 cells/mm2 and 2,244 cells/mm2 postoperatively at six, 12, 24, and 36 months, respectively, and mean IOL tilt was 3.4 ±2.5 degrees. Postoperative complications included iris capture by the IOL in eight eyes (8 percent), vitreous hemorrhage in five eyes (5 percent), and cystoid macular edema in one eye (1 percent). No patients experienced postoperative retinal detachment, endophthalmitis or IOL dislocation.
According to Dr. Crandall, the surgeon should use whatever technique he is comfortable with. “If you have not performed some of these techniques, I think it’s a good idea to watch another surgeon do them in person and not just on YouTube, because many subtleties of the techniques are edited out. Many of these subtleties can make the surgery much easier,” he adds. REVIEW
1. Gross JG, Kokame GT, Weinberg DV; Dislocated in-the-bag intraocular lens study group. In-the-bag intraocular lens dislocation. Am J Ophthalmol 2004;137:4:630-635.
2. Chan CC, Crandall AS, Ahmed IK. Ab
3. Kirk TQ, Condon GP. Simplified ab
4. Yamane S, Sato S, Maruyama-Inoue M, Kadonosono K. Flanged