|
The ophthalmologist should be able to evaluate these complaints in a systematic fashion. I explain to my patients that three factors affect drooping of the upper lids: lowering of the lid margin (true ptosis); excess tissue between the eyebrows and eye lashes (dermatochalasis or pseudoptosis); and dropping of the eyebrows (brow ptosis). These distinctions are important in that each problem is addressed with a different surgical procedure or technique. By demonstrating these separate components of the droopy upper lid to the patient, you can participate in a much more informed discussion regarding surgical options and patient expectations.
While the ophthalmologist may be comfortable with techniques to address ptosis and dermatochalasis, brow lifting techniques may be less familiar and potentially more daunting. This article will address the current spectrum of brow lifting techniques, with an emphasis on patient selection and surgical considerations of each approach.1,2
Patient Evaluation
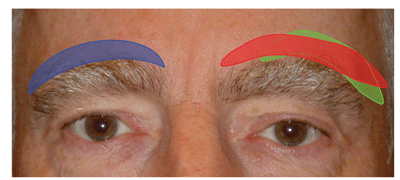
Patients rarely present with specific complaints of sagging eyebrows, and this component of the droopy lid complex may need to be demonstrated to the patient. Although the ideal brow position is subjective, the medial and lateral edges of the brow should be roughly on the same horizontal plane, with an arch that peaks over the lateral limbus. In men, the brow typically rests vertically at the level of the superior orbital rim, whereas in women the brow should rest above the orbital rim.1 Old patient photographs may be helpful when discussing changes in the brow position, and surgical goals should be tailored to the individual patient. For example, a patient who has never had high, arched brows is typically more interested in restoration rather than alteration of his appearance to this idealized norm.
While not all brow lift candidates will have functional deficits, nearly all will be concerned with their postoperative appearance. Therefore, the amount of dermatochalasis, height of the forehead, depth and location of horizontal forehead rhytids, thickness of the skin, shape of the hairline, and the color, density and length of the eyebrow cilia must be factored when evaluating the potential for visible scarring and post-operative alopecia.
|
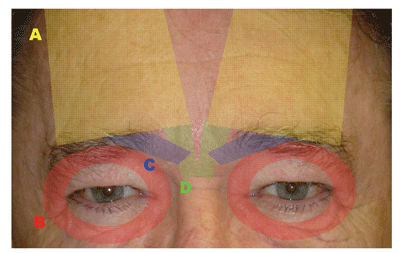
Brow position is determined by tissue elasticity, gravitational forces, ligamentous attachments to underlying tissue, and the actions of elevating and depressing muscles (See Figure 1). The frontalis muscle is the primary elevator of the brow, whereas the orbicularis oculi, corrugator supercilii and procerus muscles all act as brow depressors. These muscles are innervated by branches of the facial nerve. The lateral brow is usually the first to droop.
For the purposes of this article, I will discuss the different approaches to rejuvenation of the brow complex from an ophthalmological viewpoint, categorized by location of the surgical incisions. An emphasis will be given to surgical pearls for the ophthalmologist.
Direct Brow Lifts
The closer the incision is to the brow line, the more control the surgeon has over the final height and contour of the brow. The mechanical advantage drops with increasing distance from the incision, primarily due to elasticity of the tissue. The direct brow lift is the gold standard in terms of control over the final brow shape and position.3 However, this surgical approach is inappropriate for a large percentage of patients, and has the greatest risk of generating visible or cosmetically unacceptable scarring. In direct brow lifts, the surgical incision is created immediately over the brow hairs to camouflage the incisions. I will also include mid-forehead brow lifts in this category, since they involve similar surgical techniques and risks.
• Patient selection. According to conventional wisdom, the ideal candidate for a direct brow lift has functional blockage of the superior visual field attributable to low brow position, and dark, thick ("bushy") brow cilia. Due to the risk of visible scarring, I generally avoid this technique in younger patients and patients who would be bothered by scarring, which includes most cosmetic patients. With good patient selection and meticulous surgical technique, the incisions can be barely visible.
The patient with very deep horizontal forehead furrows may be a candidate for a mid-forehead incision, which can be hidden within the forehead wrinkles. Of all the surgical approaches, I believe the mid-forehead incision is the most difficult to hide, and can lead to the most visible scarring. Since the mid-forehead lift results in tightening of the skin, wrinkles that seemed like good places to hide an incision preoperatively may be much less prominent postoperatively. This approach should be performed infrequently and limited to functional patients with alopecia of the brows and scalp.
Since the direct brow approach relies on removal of tissue to provide lift, rather than contraction of brow elevator muscles or elimination of brow depressor muscles, it is a commonly used technique in patients with facial nerve palsies. These patients usually have functional problems due to severe brow ptosis. The direct brow lift can easily be performed unilaterally.
|
The supraciliary incision is created just within the uppermost hair of the brow to best hide the scar. The inferior incision is beveled parallel to the hair shafts to prevent postoperative hair loss. The superior incision is then beveled to the same degree to facilitate closure. The ellipse of skin and subcutaneous tissue is then excised, and hemostasis is maintained with directed cautery. Undermining is usually not required, and care should be taken to avoid the supraorbital vessels. If the brow is excessively floppy, it can be suspended to the galea above the superior incision using 4-0 nonabsorbable, monofilament sutures. Meticulous subcutaneous dermal closure is performed using 5-0 absorbable sutures to provide realignment and good eversion of the wound edge to minimize scarring. The skin edge is then closed using 6-0 monofilament sutures that can be removed in seven to 10 days. If a blepharoplasty is needed, it can be performed after the brow lift (See Figure 3).
The most common complications after a direct brow lift are visible scarring and paresthesias. Numbness of the forehead is common, but usually temporary. Scarring is most noticeable due to shadowing from a depressed scar, so hyper-eversion of the wound edges with mattress sutures is sometimes beneficial. Postoperative scarring can be masked with large spectacles or topical concealers. Microdermabrasion and laser resurfacing can also help to blend the scar.
Hairline Approaches to Brow Lift
|
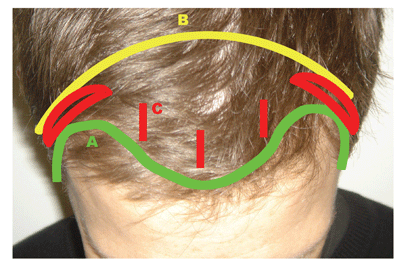
I have included in this hairline category pretrichial, coronal and endoscopic brow lift incisions (See Figure 4). There is a very large body of literature addressing variations on these techniques.1,2,8,9 Since these approaches are uncommonly used by general ophthalmologists, I will address only the salient points here.
• Patient selection. Pretrichial incisions are located just anterior to the hairline, whereas coronal incisions are located posterior to the hairline. Both involve long incisions from "ear to ear," which some patients (and surgeons) may find intimidating. With the popularity of surgical documentaries on television, a surprising percentage of patients are familiar with, and have pre-formed opinions about, open "facelift" surgeries.
|
Over the past two decades, great advances have been made in the field of minimal incision and endoscopic surgeries. The result has been decreased morbidity, surgical time and recovery time. Endoscopic brow lifts are more readily accepted by younger patients than open techniques. An ideal candidate for endoscopic brow surgery has a normal to low hairline and thick hair. Acceptable results can be achieved in men with "widow's peak" hair patterns as well.10 Endoscopic brow lifts are better suited to the repair of mild to moderate brow ptosis, whereas open techniques can address greater degrees of brow ptosis.
• Surgical considerations. The pretrichial and coronal approaches do not require specialized instrumentation, and can be performed under intravenous sedation or general anesthesia. Tumescent anesthesia helps with the surgical dissection and hemostasis. The incisions can be tailored to the surgeon's preference, but should be beveled as for the supraciliary direct brow lift. Surgical staples, elastic bands or tape can facilitate keeping hair out of the wound.
Dissection is carried anteriorly and inferiorly towards the superior orbital rim in a subgaleal or subperiosteal plane. The subgaleal plane allows direct access to the brow depressor muscles and less flap tension at closure,11 while the subperiosteal plane better preserves the vascular and sensory innervation of the coronal flap. If a subgaleal plane is used, then it can be taken subperiosteally about 2.5 cm above the orbital rim. The periosteum is dissected free from the arcus marginalis and the lateral orbital rim towards the fronto-zygomatic suture to mobilize the lateral brow. Glabellar furrows can be addressed with stripping or scoring of the brow depressors. Excellent visualization is achieved with these approaches, important in the region of the supraorbital and supratrochlear nerves.
The skin is then re-draped superiorly to lift the brows and reduce forehead rhytids. The open brow lift procedures rely on tissue removal and re-adhesion of the galea or periosteum to provide lift. Typically, excision of 1.5 to 2.5 cm of tissue is required to provide adequate brow elevation. The galea is then re-approximated with absorbable sutures, and the skin can be closed with running sutures or staples. Residual tension on the wound can lead to postoperative scarring and alopecia. Paresthesias posterior to the incision are expected, but typically improve over the next six months.
The endoscopic approach greatly reduces the amount of paresthesias, pain, bleeding and scarring.4,5 Unlike the open hairline incisions, no (or minimal) tissue is excised, and lift is generated by repositioning and re-adhesion of the periosteum, as well as weakening of the brow depressors. I use a mid-sagittal incision and two paramedian incisions, approximately 1 to 2 cm posterior to the hairline and 2 cm long, to gain access to the frontal subperiosteal space. I make two elliptical temporal incisions to provide extra lateral lift.
Dissection is carried out through the central three incisions in a subperiosteal plane under endoscopic guidance down to the superior orbital rim, as with the open procedures. Care is taken to avoid the supraorbital neurovascular bundle medially, as brisk bleeding can be difficult to control. Once the arcus marginalis is released, attention is turned towards stripping or scoring of the brow depressors. Dissection is then performed from the lateral incisions in a plane deep to the superficial tempero-parietal fascia to prevent injury to branches of the facial nerve. The lateral orbital rim is released, taking care to avoid injury to the sentinel veins laterally. Dissection is then performed medially, through the conjoined fascia, to join the central, subperiosteal plane, completely mobilizing the forehead and brows. Superior traction is placed on the forehead.
Since minimal tissue is removed, the endoscopic brow lift requires keeping the periosteum in the elevated position until it is completely re-adhered. According to animal models, it takes roughly two to four weeks for periosteal re-adhesion to stabilize,12,13 although most surgeons feel that it takes one to two months for maximal adhesion. Therefore, fixation methods are very important, and a wide variety have been used, including suspension sutures and wires, cortical bone tunnels, internal plates and screws, Mitek anchors and tissue glues.1,2
One of the simplest fixation systems to use is the Endotine fixation system (Coapt Systems Inc.), which is a bioabsorbable implant that is fixed into a small osteotomy.14 The implant uses three small tines to distribute tension, and it is absorbed over about six months, allowing adequate time for re-adhesion of the periosteum. The skull is thickest medially and posteriorly, and tends to be thinner in males.15 This should be taken into account when performing bony fixation, due to the risk of cerebrospinal fluid leaks. The implant also adds extra cost to the procedure.
Brow Lift via the Lid Crease Incision
Ophthalmologists are perhaps most familiar with the blepharoplasty incision through the eyelid crease. Frequently, there is some degree of dermatochalasis or eyelid ptosis accompanying the brow ptosis, and there is great appeal in using a single incision to lift both the lid and the brow. The lid crease incision is very well hidden, and scarring is a minor concern with good technique.
|
• Patient selection. Lid crease incisions are ideal for patients with thinning or receding hairlines or with sparse brow cilia. "Heavy brows" are more difficult to lift from this approach. The transblepharoplasty approach is good for patients with mild to moderate brow ptosis that require minimal downtime and are reluctant to undergo more invasive procedures.
• Surgical considerations. A standard blepharoplasty incision is created through the lid crease, and dissection is performed in a suborbicularis plane to the superior orbital rim. With the internal browpexy procedure, the lateral brow fat pad is suspended to the deep temporalis fascia just above the orbital rim using nonabsorbable sutures.19 This technique provides a slight lift of the brow, but it can result in visible dimpling of the skin.
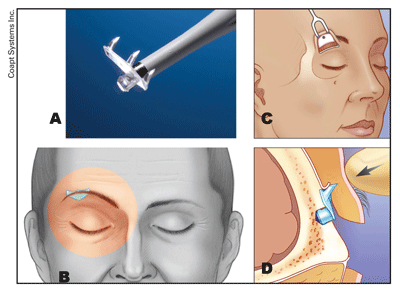
With the transblepharoplasty Endotine fixation system (Coapt), the periosteum is incised lateral to the supraorbital notch, less than a centimeter above the arcus marginalis.17,18 The incision is carried over the lateral orbital rim. Dissection is then turned superiorly in a subperiosteal plane as far as possible. Occasionally, bone wax may be required for small perforating vessels. The conjoined tendon is then separated laterally, and dissection is carefully performed along the deep tempero-parietal fascia.
An osteotomy is then performed with a low speed or manual drill roughly 1.0 to 1.5 cm above the orbital rim, centered where maximal lift is desired. The drill bit is supplied with the Endotine device, which comes in 3.0- or 3.5-mm tines. Penetration of the frontal sinus is possible, and thin bone should be avoided if possible. The implant is then popped into the osteotomy. The brow tissues are retracted superiorly over the implant, and then pressed firmly onto the tines to secure the brow in place. The periosteum can be impaled through the device or bunched above it. The blepharoplasty is then closed as per routine. There is a relatively short learning curve for this technique, and the anatomy is very familiar to the ophthalmologist.
|
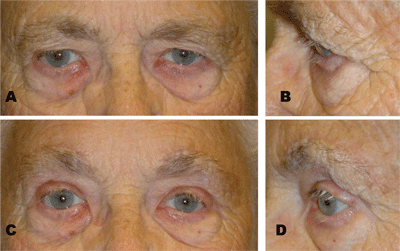
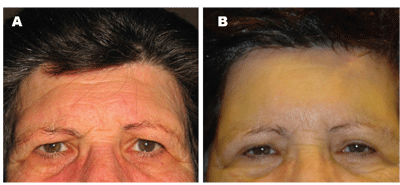
Postoperatively, there is edema over the brows, and the implant may be palpable through the skin, especially in individuals with thinner skin. I have found that paresthesias are relatively common, but usually fade within a few weeks. Some patients complain of tenderness over the implant or occasional shooting pains, but these seem to dissipate as the implant dissolves over a time frame of three to six months. The degree of lift is modest, averaging a few millimeters, but patient satisfaction is high. Since the transblepharoplasty version of the Endotine system has been available for only two years, long-term experience is still pending, but initial results have been good (See Figure 7).
Chemical Brow Lifts
Botulinum toxin A (Botox, Allergan) is used by many ophthalmologists to treat blepharospasm as well as dynamic periocular rhytids. When applied to the frontalis muscle, it can decrease forehead wrinkling, but exacerbate brow ptosis. When applied to the glabella, it can induce a medial brow lift by paralyzing the medial brow depressors.
• Patient selection. The ideal candidate for a chemical brow lift is a young patient with mild, predominantly lateral brow ptosis. They must be willing to undergo repeated injections every three to four months at accumulating expense. Chemical brow lifts are a reasonable alternative for patients who do not wish to have a surgical procedure. Botox also provides a very useful adjunct to surgical brow lifts by inactivating the brow depressors during the postoperative phase, allowing the periosteum to re-adhere without being actively pulled downwards.
• Surgical considerations. Botox is injected directly into the target muscles using standard techniques. Medially, approximately 15 to 25 units of Botox is sufficient to neutralize the corrugator supercilii and procerus. Laterally, approximately 2.5 to 10 units is applied to the lateral orbicularis to provide a temporal lift. Roughly 1-mm of brow lift can be achieved over the mid-pupil, and 4.8-mm brow lift over the lateral canthus, demonstrating that Botox injections are most useful for a temporal brow lift.20,21 Complications from periocular Botox injections include bruising, mild discomfort, ptosis and inconsistent degrees of brow lift.
|
A wide range of surgical techniques to elevate the brows has been described (See Table 1, above). When considering the most appropriate approach for a patient, one must evaluate the patient's anatomy, functional status and aesthetic goals. Direct, lid crease and chemical brow lifts can be readily performed by the ophthalmologist, as can hairline approaches, with proper training. Brow lifting is an important skill set for anyone treating the droopy upper lid.
Dr. Mandeville is in private practice and is on the Active Staff at the Massachusetts Eye and Ear Infirmary. Contact him at Eye Health Services, Inc., 1900 Crown Colony Dr., Suite 301, Quincy, MA 02169. E-mail:
jmande ville@eyehealthservices.com. Phone: (617) 770-4400. He has no financial interest in the products discussed herein.
1. Arneja JS, Larson DL, Gosain AK. Aesthetic and reconstructive brow lift: Current techniques, indications, and applications. Ophthal Plast Reconstr Surg 2005; 21:6:405-11.
2. Dailey RA, Saulny SM. Current treatments for brow ptosis. Curr Opin Ophthalmol 2003;14:260-6.
3. Booth AJ, Murray A, Tyers AG. The direct brow lift: Efficacy, complications, and patient satisfaction. Br J Ophthalmol 2004;88:688-91.
4. Chiu E, Baker DC. Endoscopic brow lift: A retrospective review of 628 consecutive cases over 5 years. Plast Reconstr Surg 2003;112:628-33.
5. Jones BM, Grover R. Endoscopic brow lift: A personal review of 538 patients and comparison of fixation techniques. Plast reconstr Surg 2004;113:1242-50.
6. Ortiz-Monasterio F. Aesthetic surgery of the facial skeleton: The forehead. Clin Plast Surg 1991;18:19-27.
7. Flowers RS, Caputy GC, Flowers SS. The biomechanics of brow and frontalis function and its effect on blepharoplasty. Clin Plast Surg 1993;20:255-68.
8. Puig CM, LaFerriere KA. A retrospective comparison of open and endoscopic brow-lifts. Arch Facial Plast Surg 2002;4:221-5.
9. Steinsapir KD, Shorr N, Hoenig J, et al. The endoscopic forehead lift. Ophthalmic Plast Reconstr Surg 1998;14:107-18.
10. Tower RN, Dailey RA. Endoscopic pretrichial brow lift: Surgical indications, technique and outcomes. Ophthal Plast Reconstr Surg 2004;20:268-73.
11. Nassif PS, Kokoska MS, Homan S, et al. Comparison of subperiosteal vs. subgaleal elevation techniques used in forehead lifts. Arch Otolaryngol Head Neck Surg 1998;124:1209-15.
12. Kim JC, Crawford Downs J, Azuola ME, Devon Graham H. Time scale for periosteal readhesion after brow lift. Laryngoscope 2004;114:50-5.
13. Boutros S, Bernard RW, Galiano RD, et al. The temporal sequence of periosteal attachment after elevation. Plast Reconstr Surg 2003;111:1942-7.
14. Berkowitz RL, Jacobs DI, Gorman PJ. Brow fixation with the Endotine Forehead device in endoscopic brow lift. Plast Reconstr Surg 2005;116:1761-7.
15. Walden JL, Orseck JM, Aston SJ. Current methods for brow fixation: Are they safe? Aesthetic Plast Surg 2006;30:541-6.
16. Kikkawa DO, Miller SR, Batra MK, Lee AC. Small incision, non-endoscopic browlift. Ophthal Plast Reconstr Surg 2000;16:28-33.
17. Baker SS, Holck DE, Holloman EL. Brow lifting: Operative techniques using transblepharoplasty approach with internal fixation device. Presented at the annual meeting of the American Society of Ophthalmic Plastic and Reconstructive Surgery, Chicago 2005.
18. Mack WP, Rose JG Jr., Licarelli MJ, Burkat CN. Presented at the annual meeting of the American Society of Ophthalmic Plastic and Reconstructive Surgery, Chicago 2005.
19. Niechajev I. Transpalpebral browpexy. Plast Reconstr Surg 2004; 113:2172-80.
20. Ahn MS, Catten M, Maas CS. Temporal brow lift using botulinum toxin A. Plast Reconstr Surg 2000; 105:1129-35.
21. Huilgol SC, Carruthers A, Carruthers JD. Raising eyebrows with botulinum toxin. Dermatol Surg 1999;25:373-5.