Cataract surgeons will often do whatever it takes to eliminate patients’ astigmatism and bring them as close to emmetropia as possible. They sometimes run into limits in terms of how much astigmatism they can effectively correct, however—though they say that patients can sometimes tolerate low levels of cylinder without much complaint. Following is some expert advice for managing astigmatism in your next case.
The Impact of Astigmatism
Mitchell P. Weikert, MD, MS, associate professor at the Cullen Eye Institute, Baylor College of Medicine, says the impact of astigmatism depends on multiple factors, such as visual task, interaction with other aberrations, pupil size, accommodative state, neuroadaptation and subjective blur threshold. “In all cases,” he says, “it leads to meridional variation in retinal image blur and a reduction in distance, near, stereo and contrast visual acuity.”
Dr. Weikert cites a 2013 study on the relation between uncorrected astigmatism and visual acuity in pseudophakia that shows that as hyperopic and myopic astigmatism increases, distance visual acuity decreases, independent of the axis.1 “But one interesting finding,” Dr. Weikert notes, is that “as higher-order aberrations increase, the image quality improves for near objects.” Likewise, a 2014 study on image quality analysis of pseudophakic eyes with uncorrected astigmatism found that distance visual acuity decreases with higher order aberrations, while near image quality increases.2 Dr. Weikert explains this, saying, “when you have myopic astigmatism, as objects come closer, the conoid of Sturm gets pushed closer to the retina.
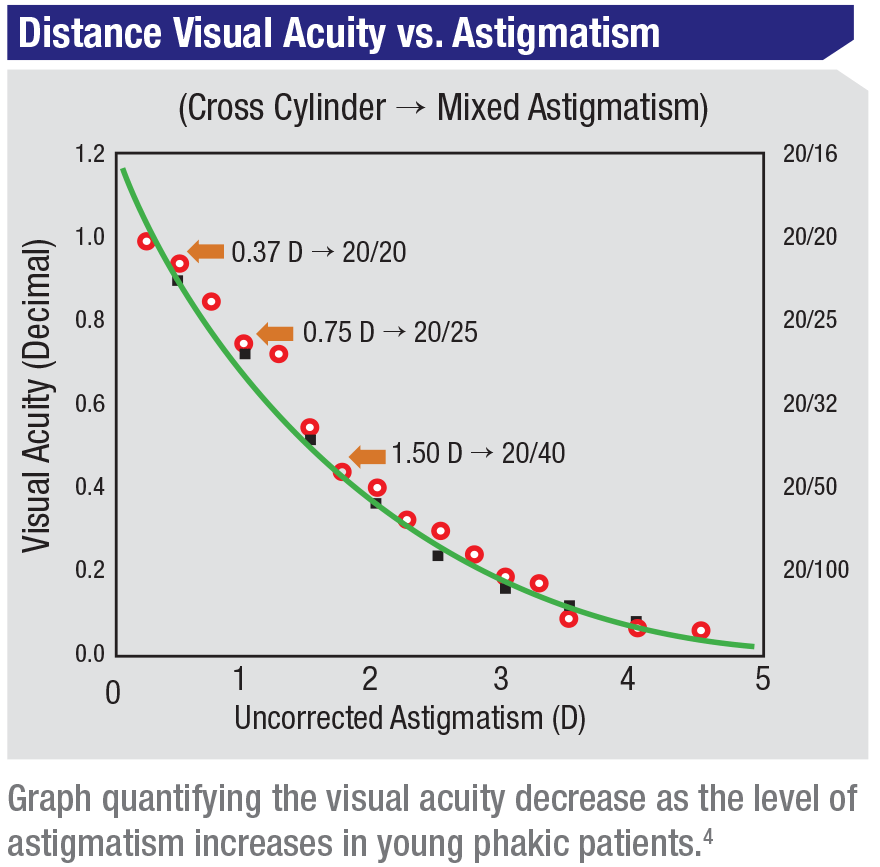
“The astigmatism threshold at which the average person notices a decrease in vision is about
0.25 D,” says Dr. Weikert. “Studies have shown that in young phakic patients, visual acuity decreases as astigmatism increases. At around 0.37 D people can still see 20/20, but at 0.75 D, this drops to 20/25 and at 1.5 D to 20/40.”
Dr. Weikert notes that pupil size also makes a difference when it comes to astigmatism levels. “The smaller the pupil, the better the acuity—it’s intuitive,” he says. “As pupil size gets smaller, you get more of a pinhole effect, so the effect of the astigmatism decreases. Astigmatism effects are not as great for smaller pupils.”
Treating the Astigmatism
Like many surgeons, Dr. Weikert prefers a toric IOL to corneal relaxing incisions for correcting astigmatism.
“The Barrett formula is good across the board,” he says, “but formula choice these days is dictated by length of the eye rather than toric versus non-toric.” Dr. Weikert says he doesn’t hang his hat on just one formula. He likes to have at least three measurements to compare. “My go-to formula is the Barrett, along with the Holladay 1 and the Hill RBF.”
In addition to the three formulas, Dr. Weikert employs biometers like the IOLMaster 700 or LenSTAR, topography and tomography to measure the front and back of the cornea, and Pentacam to measure posterior corneal astigmatism. “It’s nice when you see agreement among multiple measurements of magnitude and axis of astigmatism,” he says.
 |
Dr. Weikert prefers to take measurements of both the front and back of the cornea. “Most formulas just measure the anterior surface to predict the back of the cornea,” he notes. “Now though, people are trying to measure the front and the back to get accurate measures of true corneal astigmatism.” In a well-known 2012 study on the contribution of posterior corneal astigmatism to total corneal astigmatism, in which he participated, he and his co-authors found that taking posterior corneal measurements instead of relying only on anterior corneal measurements can help avoid “overcorrection in eyes that have with-the-rule astigmatism and undercorrection in eyes that have against-the-rule astigmatism”3 when selecting IOLs.
Dr. Weikert says measuring many patients over the years has taught him a lot about the best way to approach astigmatism correction. “Since individual measurement on a person-to-person basis doesn’t seem to explain the whole picture, most surgeons use population norms to try to figure out how much astigmatism to target in patients,” he says. “You need to be meticulous in your preop planning and measurements. You want to make sure you have good-quality measurements.”
If toric IOLs aren’t within a patient’s means, Dr. Weikert’s second choice for correcting astigmatism is incisions, which are effective for low amounts of astigmatism. “You don’t have as great a range of correction as IOLs and can’t treat as high levels of astigmatism, and you have more variability of what you achieve versus what you can target, however,” he explains. “If a patient presents with lower levels of astigmatism but has variable measurements, I might defer astigmatism correction until after cataract surgery, especially if the patient doesn’t have enough astigmatism for a toric IOL.”
Accounting for SIA
Dr. Weikert says surgically induced astigmatism may not be that big of a factor in the final outcome.
“It may be helpful to look at your own SIA data, if you have time,” he says, “[but] the data for SIA is very noisy. You have to compare measurements preop and postop, and the data tends to be all over the map. Measuring only the cornea is noisy, for example. You can have variations up to 0.5 D of astigmatism in the same person from week to week.”
Surgically induced astigmatism accounts for only very small changes, Dr. Weikert avers. “The overall spherical power of the lens and the overall refractive power of the cornea don’t change too much,” he says. “Maybe a tiny bit in a hyperopic direction, but not much.”
Some toric calculators, such as the Barrett calculator, factor in SIA. Dr. Weikert also finds the Baylor nomogram useful for determining the level of astigmatism your surgery might produce. When gauging this, you have to calculate the SIA yourself. “It’s small,” he says.
Acceptable Astigmatism
Low levels of astigmatism still warrant correctional surgery, but at a certain point, changes in visual acuity become less significant, Dr. Weikert says. “Looking solely at image quality, when you remove higher order aberrations, image quality improves as astigmatism decreases,” he notes. “Going from 0.5 D to
0.3 D will offer some improvement in acuity, but it doesn’t make a huge difference. From 0 to 0.5 D astigmatism, image quality doesn’t really change much.”
In the case of high-contrast vision, Dr. Weikert says that acuity improves slightly with decreasing levels of astigmatism. But “once you get below 0.3 D, it doesn’t matter—there’s no improvement. And low-contrast acuity is pretty much independent of astigmatism.”
Dr. Weikert points out that there are some cases where a small amount of astigmatism is desirable. “You want to shoot for a little residual with-the-rule astigmatism,” he advises. “As people age, they shift from with-the-rule to against-the-rule astigmatism by about 0.38 D over a decade.” Dr. Weikert recommends leaving about 0.25 D of WTR astigmatism as a cushion for this transition.
When further correction won’t significantly improve visual acuity, it’s time to stop. Ultimately, Dr. Weikert says surgeons should aim for no more than 0.5 D of postop astigmatism. “Or 0.3 D or less if you really want to get it down,” he adds. REVIEW
Dr. Weikert is a consultant to Alcon Laboratories and Ziemer Ophthalmic Systems.
1. Singh A, Pesala V, Garg P, Bharadwaj SR. Relation between uncorrected astigmatism and visual acuity in pseudophakia. Opto Vis Sci 2013;90:4:378-84.
2. Pesala V, Garg P, Bharadwaj SR. Image quality analysis of pseudophakic eyes with uncorrected astigmatism. Opto Vis Sci 2014;91:4:444-51.
3. Koch DD, Ali SF, Weikert MP, Shirayama M, Jenkins R, Wang L. Contribution of posterior corneal astigmatism to total corneal astigmatism. J Refract Surg 2012;38:12:2080-7.
4. Moon BY, Kim SY, Cho HG. Predicting of uncorrected astigmatism from decimal visual acuity in spherical equivalent. J Optical Society of Korea 2013;17:2:219-223.



