Presentation
A 24-year-old man presented to the Wills Eye emergency room complaining of blurred vision in his left eye for one day. He noted the "top part" of his vision was most affected. The patient was myopic but denied any other ocular history. He also denied symptoms of flashes, floaters, pain, photophobia or trauma.
Medical History
The patient reported no significant past medical history, took no medications and had no family history of any eye problems. Review of systems, other than his ocular complaint, was negative. The patient denied cough, shortness of breath, chest pains, fevers, chills, night sweats, rashes, weight loss, joint pain or sexually transmitted diseases. The patient had moved to the
Examination
Best-corrected visual acuity was 20/20 in the right eye and 20/50 in the left eye with no pinhole improvement. Extraocular motility was normal and confrontation visual fields were full in both eyes. A relative afferent papillary defect was noted in the left eye. Color plates were eight out of eight in each eye. Intraocular pressure measured 12 mmHg for both eyes. Anterior examination was normal in both eyes. There was no proptosis, no conjunctival injection, and the anterior chamber was deep and quiet.
Posterior exam was normal in the right eye. In the left eye, dilated fundus exam showed diffuse retinal hemorrhages, tortuous veins, venous sheathing, sclerotic vessels, macular exudates and edema and neovascularization of the disc (See Figure 1). Trace white blood cells and pigment were seen in the anterior vitreous.
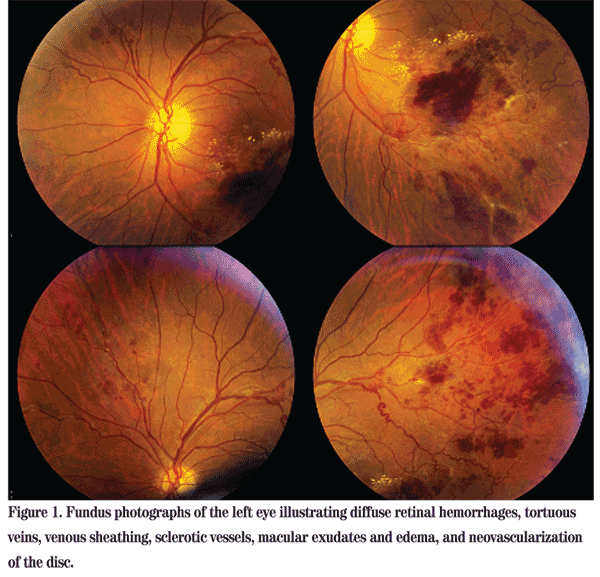
Diagnosis, Workup and Treatment
This patient presented with a one-day history of blurry vision in his left eye with no other systemic or ocular complaints. Fundus examination was concerning for vascular occlusion or inflammation (vasculitis). Included in the differential diagnosis were infectious causes (tuberculosis, syphilis, Lyme disease), inflammatory causes (sarcoidosis, Behçet's disease, SLE, IRVAN, Wegener's granulomatosis, Eales' disease), and hematologic/vascular abnormalities (malignant hypertension, sickle cell, leukemia, Factor V Leiden disease, protein C or S deficiency, antithrombin III deficiency, etc.)
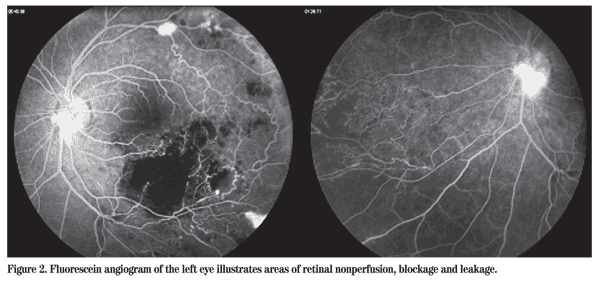
The patient followed up at the Wills Eye Institute Retina Service, where a fluorescein angiogram was performed. Areas of retinal nonperfusion and blockage (from blood) were noted along with leakage (See Figure 2).
A full systemic workup was performed, including CBC, hemoglobin A1C, sickle screen, PT/PTT, basic metabolic panel, RPR, FTA-Abs, ANA, ANCA, ACE, Lyme, HIV and a chest X-ray. Upon questioning, the patient reported a history of receiving the BCG vaccine, so a Quantiferon test was ordered instead of placing a PPD. (The Quantiferon test detects Mycobacterium tuberculosis infection by measuring the release of interferon-gamma from lymphocytes after exposure to M. tuberculosis antigen. Its test agents are not present in the BCG vaccine, so its results are not affected by prior BCG vaccination.) The patient also noted that his father had tuberculosis, which was treated in the past.
All labs came back negative except for the Quantiferon test, which was positive. A chest X-ray showed left hilar prominence, and a chest CT was recommended for further evaluation. Given this patient's history, examination and workup, Eales' disease was high on the differential. Sar-coidosis and tuberculosis were also considered, although no signs of granulomatous inflammation were seen on exam.
A chest CT was obtained which showed an enlarged left hilar node and multiple scattered lung nodules. The patient was referred to a pulmonologist, who did not think that the patient had active tuberculosis and did not recommend commencing systemic therapy. The patient was scheduled to obtain a repeat chest CT in three months and follow up with the pulmonologist.
After discussion with the patient, an injection of intravitreal bevacizumab and laser panretinal photocoagulation were performed. Six weeks after the patient's initial presentation, his best corrected visual acuity had improved to 20/25 in the left eye. The neovascularization was noted to be regressing.
Discussion
First described by Henry Eales, a British ophthalmologist, in 1880, Eales' disease is now more commonly found on the Indian subcontinent and areas of the
Eales' disease is currently characterized by three stages: an initial inflammatory stage; an ischemic stage; and finally, a proliferative stage. Our patient had reached the proliferative stage before noticing any symptoms, which were likely due to his macular hemorrhage and edema. Macular changes in Eales' disease are uncommon, found in only 18 percent of patients. Neovascularization of the optic disc, which this patient also had, is even more infrequent, only seen in 9 percent of patients. The main cause of loss of vision in patients with Eales' disease is vitreous hemorrhage and retinal detachment secondary to the neovascularization. Severe visual loss in patients with Eales' disease is rare; a review of 800 cases (1,214 eyes) showed that only 0.33 percent of patients had a vision of 20/200 or worse.
The etiology of Eales' disease is unknown. Systemic associations with multiple diseases have been reported, including tuberculosis, multiple sclerosis, cerebral stroke, parasitic infections and hematologic disorders, but no definitive link has been found. The associations most often reported have been between Eales' disease and both tuberculosis and a hypersensitivity to the tuberculin protein. Small studies of vitreous samples and epiretinal membranes in patients with Eales' disease showed the presence of M. tuberculosis DNA by PCR. One theory is that patients may carry nonviable organisms or DNA of M. tuberculosis in the eye which somehow triggers an inflammatory response, and the lower incidence of Eales' disease in developed countries is due to the lower incidence of tuberculosis in those countries. Another theory is that the retina is sensitized against the tuberculin protein and upon re-exposure to the antigen, an allergic vasculitis occurs, leading to the findings of Eales'. A positive PPD test has been noted in anywhere between 42 and 98 percent of patients with Eales'.
However, Eales' disease can be seen in PPD-negative patients, and a recent study from India showed no statistically significant difference in PPD positivity between those with Eales' disease and those without Eales', as 67 to 90 percent of healthy adults in some areas of India are PPD positive.
Treatment of Eales' disease includes observation if the vasculitis appears inactive, corticosteroids in the inflammatory stage, panretinal photocoagulation in the proliferative phase, vitrectomy for vitreous hemorrhage or tractional retinal detachments, and anti-VEGF intraocular injections. There is also a role for concurrent administration of anti-tuberculosis medications, although this is controversial.
The author would like to thank Marc Spirn, MD, Wills Eye Institute Retina Department, for his time and assistance.
1. Biswas J, Narain S, Roy S, Madhavan HN. Evaluation of lymphocyte proliferation assay to purified protein derivative, enzyme linked immunosorbant assay, and tuberculin hypersensitivity in Eales' disease. Indian J Ophthalmol 1997 Jun;45(2):93-7.
2. Biswas J, Sharma T, Gopal L, Madhavan HN, Sulochana KN, Ramakrishnan S. Eales disease--an update. SurvOphthalmol 2002;47(3):197-214.
3. Biswas J, Therese L, Madhavan HN. Use of polymerase chain reaction in detection of Mycobacterium tuberculosis complex DNA from vitreous sample of Eales' disease. Br J Ophthalmol 1999;83(8):994.
4. Chanana B, Azad RV, Patwardhan S. Role of intravitreal bevacizumab in the management of Eales' disease. IntOphthalmol 2010 Feb;30(1):57-61.
5. Das T, Pathengay A, Hussain N, Biswas J. Eales' disease: Diagnosis and management. Eye (Lond). 2010 Mar;24(3):472-82.
6. Madhavan HN, Therese KL, Gunisha P, Jayanthi U, Biswas J. Polymerase chain reaction for detection of Mycobacterium tuberculosis in epiretinal membrane in Eales' disease. Invest Ophthalmol Vis Sci 2000 Mar;41(3):822-5.
7. Nagpal, PN, Sharma, RK, Joshi, BS, Patel, AM. Management of Eales' disease: Analysis of 800 cases (1,214 eyes).
8. Narain R, Kirishnamurthy MS, Anantharaman DS. Prevalence of non-specific sensitivity in some parts of



