|
Presentation
A 79-year-old man presented to the Wills Eye Institute with the complaint of sudden vision loss in the left eye associated with throbbing pain, now resolved. He had seen a retina specialist the day before and was told he had "bleeding behind the eye." He also noted a red left eye for the past six months, along with some initial proptosis, which had since resolved.
Medical History
The patient's past medical history was significant for diabetes mellitus, hypertension and coronary artery disease. He had recently been diagnosed with glaucoma in the left eye one month prior to presentation.Surgical history included a cholecystectomy, cardiac stents, a left knee replacement and cataract extraction with intraocular lens implantation in both eyes. The patient was on glyburide, simvastatin, metoprolol, lisinopril, aspirin and Flomax. Ocular medications included latanoprost (Xalatan), brinzolamide (Azopt) and brimonidine tartrate/timolol maleate (Combigan) for treatment of his glaucoma in the left eye. The patient denied any significant social or family history. Review of systems, other than ocular complaints, was negative. The patient denied any recent trauma, fevers, malaise or weight loss.
Examination
The patient's best-corrected visual acuity was 20/20 in the right eye and 20/200 in the left eye. Extrocular motility was intact and confrontation visual fields were full in both eyes. Intraocular pressure was 16 in the right eye, 14 in the left eye. Pupils showed a trace relative afferent pupillary defect in the left eye. Color plates were 10/10 in the right eye and 5/10 in the left eye. No proptosis was noted.
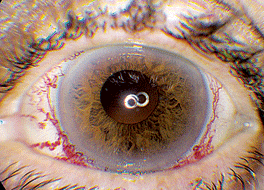
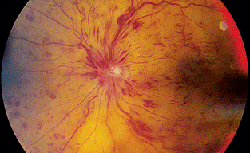
Anterior exam was normal in the right eye and showed diffuse injection with dilated vasculature in the left eye (See Figure 1). Posterior exam was normal in the right eye, but showed 360 degrees of extensive hemorrhages and multiple cotton wool spots in the left eye (See Figure 2).
What is your differential diagnosis? What further workup would you pursue?