Presentation
A 23-year-old female with no past ocular history was referred to the Wills Oculoplastic and Orbital Surgery Service for treatment of an orbital fracture. Ten days prior to presentation, the patient was head-butted in the right eye while hospitalized at an outside facility. A computed tomography scan performed at the facility that day was interpreted by the hospital's radiologist as a right inferior wall orbital fracture. Upon presentation, the patient complained of swelling around her right eye. She had no change in vision and no diplopia.
Medical History
The patient had a past medical history of mild mental retardation, anxiety and post-traumatic stress disorder. She was an inpatient at a local hospital's psychiatric unit. Her trauma occurred accidentally through contact with another inpatient. Her medications included venlafaxine, lamotrigine and folate. In addition, she was placed on amoxicillin and a tobramycin/dexamethasone eye ointment after being diagnosed with an orbital fracture. Family history was significant for glaucoma in both grandmothers, and review of systems was noncontributory.
Examination
Visual acuity with correction was 20/200 in the right eye, improving to 20/25 with pinhole. Visual acuity was 20/30 in the left eye. Pupils were equal, round, reactive to light and without evidence of an afferent defect. Extraocular motility was full in both eyes. Intraocular pressures by applanation tonometry were 18 mmHg in the right eye and 21 mmHg in the left. Confrontation testing revealed a constricted field in the right eye, but this was felt to be secondary to periorbital edema. Visual field was full to confrontation testing in the left eye. There was hypesthesia in the distribution of cranial nerve V2 on the right. Hertel'sexophthalmometry was unable to be performed secondary to severe periorbital edema. The patient had a large hematoma of the forehead on the right side with edema of the right upper and lower eyelids. Slit lamp exam and dilated fundus exam were normal in both eyes. The CT images were reviewed and appear below.
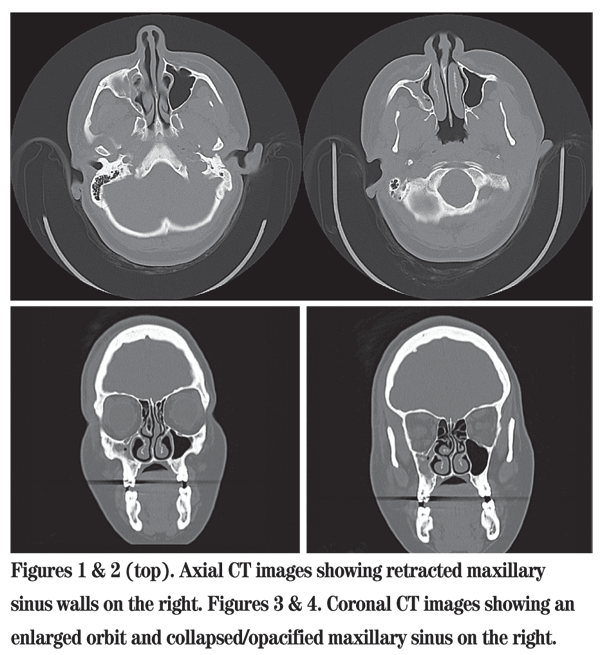
Diagnosis, Workup and Treatment
Although the patient presented with a diagnosis of orbital fracture after trauma, a review of the CT images did not show any fracture. Pertinent findings in the above images include a hypoplastic and opacified maxillary sinus on the right with an enlarged orbit. There is retraction of the right anterior and medial maxillary sinus walls. The right orbital floor protrudes into the maxillary sinus lumen, and there is hypoglobus. The findings in this case are consistent with a rare entity known as silent sinus syndrome.
The patient was referred for consultation with an otolaryngologist, and a combined sinus aeration and orbital reconstruction surgery was performed. The sinus aeration was performed using functional endoscopic sinus surgery (FESS) with turbinate reduction and conchabullosa resection. The orbital reconstruction was done via a transconjunctival approach using hydroxyapatite crystals and a 0.4-mm Medpor implant to re-form the orbital floor and augment the orbital volume.
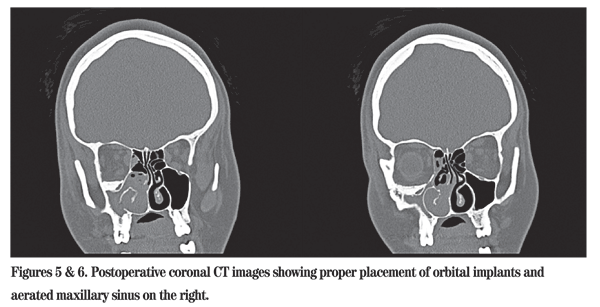
The patient was discharged home one day after surgery, having tolerated the procedure well. Two days later, she was admitted to an outside hospital for nausea and vomiting. Evaluation by an ophthalmologist revealed no evidence of extraocular muscle entrapment or retrobulbar hemorrhage. A repeat orbital CT scan was performed with images shown below.
These images reveal the expected postoperative findings, including appropriately placed hydroxyapatite crystals in the right orbital floor and a newly enlarged right maxillary sinus. Further workup of the patient's nausea and vomiting eventually lead to upper gastrointestinal endoscopy and a diagnosis of herpes simplex esophagitis. These symptoms resolved and the patient was again discharged home.
Discussion
Silent sinus syndrome is a process of chronic, asymptomatic maxillary sinus collapse.
There is usually no history of trauma, making the initial diagnosis in this case particularly difficult. The maxillary sinus collapse leads to spontaneous enophthalmos and hypoglobus. In this case, review of the patient's old photographs indeed showed she had enophthalmos and hypoglobus months prior to any orbital trauma. The first reports of this entity were in 1964 by William W. Montgomery, MD, who reported two cases.1
The term "silent sinus syndrome" was first reported by Charles Soparkar, MD, PhD, and colleagues in 1994.2 The peak age of presentation is the fourth decade, with men and women equally affected.3
The pathogenesis is related to hypoventilation of the maxillary sinus caused by ostial obstruction. Numerous mechanisms have been proposed to cause this obstruction, including mucous inspissation, nasal polyps, mucosal inflammation, a hypermobile medial infundibular wall and maxillary sinus hypoplasia.4 The exact inciting event remains unclear. It is theorized that resorption of sinus fluid then causes negative pressure within the sinus, leading to retraction of the sinus walls. Maxillary sinus manometry has showed subatmospheric pressures in affected patients, supporting the role negative pressure may play in silent sinus syndrome.5 Inferior bowing of the orbital floor leads to numerous ophthalmic complaints, including hypoglobus, enophthalmos, upper eyelid retraction, deepening of the superior sulcus, oscillopsia and diplopia.6
Rarely, an audible clicking sound may occur with blinking. This has been attributed to trapping of air in the conjunctival recesses.7 Patients usually present to their ophthalmologists with complaints of enophthalmos and hypoglobus. Enophthalmos may range from 1 to 6 mm and hypoglobus from 0 to 6 mm.6 Visual acuity is unaffected, but extraocular motility restriction may occur. These patients do not have associated nasal and sinus symptoms, hence the "silent" nature of this disease. Remote symptoms of congestion and sinus pressure may be recalled, but are usually absent. In Dr. Soparkar's original description of the disease, only 36 percent of patients reported some symptoms related to sinus disease.2
Diagnosis is generally made through CT. MRI may also be used, but the poorer visualization of bony details makes it less useful than CT. Radiologic findings include an enlarged orbit and maxillary sinus atelectasis. There is often maxillary sinus opacification and mucosal thickening.8,9 As seen in this case, there is usually retraction of the maxillary sinus walls. Retraction of the superior maxillary wall and inferior orbital wall bowing lead to hypoglobus. The bones involved are usually thinned (osteopenic), but may also be thickened. Extraocular muscles descend with the globe, but orbital soft tissues otherwise appear normal. Silent sinus syndrome occurs as a unilateral process.6 In the absence of such radiographic findings, other causes for spontaneous hypoglobus and enophthalmos to consider include trauma, scirrhous carcinoma, orbital varix, osteomyelitis, Parry-Romberg syndrome, linear scleroderma and lipodystrophy.10,11
Management includes otolaryngologic consultation to aerate the maxillary sinus and restore its volume. In the past, this surgical repair was done with Caldwell-Luc sinus surgery,4 a technique that involves incising the mucosa above maxillary teeth (upper jaw) to enter the sinus. Endoscopic sinus surgery has largely replaced traditional incisional surgery and usually involves a maxillary antrostomy and uncinectomy.
Postoperative imaging may or may not show changes to the maxillary sinus configuration. Either way, hypoglobus and enophthalmos generally do not progress once the maxillary sinus has been aerated.6 Orbital reconstruction to rebuild the orbital floor may be performed simultaneously or may be done later. Some authors recommend staging the surgery, as enophthalmos may improve after sinus aeration alone. This is surgeon dependent and varies by case. A transconjunctival approach is most commonly used to access the orbital floor, where plates or hydroxyapatite granules are implanted to restore it.
The author would like to thank Jacqueline R. Carrasco, MD, FACS, of the Wills Eye Oculoplastic and Orbital Surgery Service for her assistance with this case.
1.
2. Soparkar CN, Patrinely JR, Cuaycong MJ, et al. The silent sinus syndrome: A cause of spontaneous enophthalmos. Ophthalmology 1994;101:772-778.
3. Boyd JH, Yaffee K, Holds J. Maxillary sinus atelectasis with enophthalmos. Ann OtolRhinolLaryngol 1998;107:34-39.
4. Vander Meer JB, Harris G, Toohill RJ, Smith TL. The silent sinus syndrome: a case series and literature review. Laryngoscope 2001;111:975-978.
5. Kass ES, Salman S, Montgomery WW. Manometric study of complete ostial occlusion in chronic maxillary atelectasis. Laryngoscope 1996;106:1255-1258.
6. Buono, LM. The silent sinus syndrome: Maxillary sinus atelectasis with enophthalmos and hypoglobus. CurrOpinOphth 2004;15:486-489.
7. Dailey RA, Cohen JI. Surgical repair of the silent sinus syndrome.OphthalPlastReconstrSurg 1995;11:261-268.
8. Wilkins RB, Kulwin DR. Spontaneous enophthalmos associated with chronic maxillary sinusitis. Ophthalmology 1981;88:981-985.
9. Illner A, Davidson HC, Harnsberger HR, Hoffman J: The silent sinus syndrome: clinical and radiographic findings. AJR Am J Roentgenol 2002, 178:503-506.
10. Burroughs JR, Hernandez Cospin JR, Sorparkar CN, Patrinely JR. Misdiagnosis of silent sinus syndrome. OphthalPlastReconstrSurg 2003;19:449-454.
11. Cline RA, Rootman J. Enophthalmos: A clinical review. Ophthalmology 1984;91:229-237.



