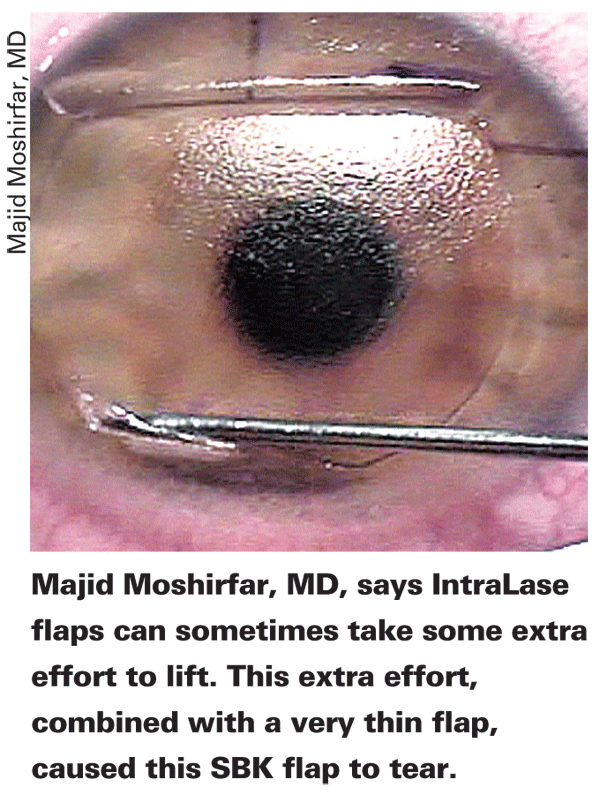
Thin-flap LASIK, sometimes specif-referred to as sub-Bowman's keratomileusis, uses thinner, and occasionally smaller-diameter, flaps in order to preserve stromal tissue in an effort to reduce the risk of ectasia. Further, its proponents say it also reduces the incidence of postop dry eye by virtue of severing fewer corneal nerves. Some surgeons argue, however, that, if it's safety you're concerned about, surgeons already have a procedure that severs even fewer nerves, all but eliminates the risk of ectasia by keeping the structure of the cornea intact, and makes enhancements a breeze because you don't have to try to work with a flimsy ultra-thin flap months postop: surface ablation. Here, several surgeons weigh the pros and cons of SBK and PRK.
Outcomes Compared
For surgeons who argue that PRK is just as good, however—they're right. In a study performed by Drs. Durrie, Slade and their colleague John Marshall of
The Differences Explored
San Francisco
In addition to patients who participate in contact sports and may have the flap displaced if hit in the eye, surgeons say dry-eye risk may also be a consideration when deciding between surface ablation and even a thin-flap procedure such as SBK. "I think there's a little less dry eye with surface ablation than with any flap procedure," says
Finally, there's the argument of structural integrity. SBK proponents say the procedure's better for the structural integrity of the cornea because it severs fewer collagen fibrils than the creation of a thicker flap does. However, PRK severs even fewer, so some might wonder if it results in a stronger cornea over the long term.
"My indication for SBK would be a patient who has a somewhat thin cornea but which is otherwise normal on topography and slit-lamp exam," says Dr. Faktorovich. "If a cornea is asymmetric, for example it has inferior steepening greater than 1.5 D, irregularity or there's evidence of epithelial basement membrane dystrophy, I do PRK. An interesting study would be to analyze the long-term outcomes of SBK vs. PRK in patients with mild corneal asymmetry and/or irregularity. Because they're different; with SBK, typically you end up ablating deeper than with PRK. Also, SBK is a different procedure structurally because Bowman's is interrupted peripherally with SBK, whereas PRK involves ablating through Bowman's membrane centrally. That's why I hesitate to do SBK on patients who may potentially have a predisposition toward corneal weakening based on their topographic maps."
Surgeons say, however, that any structural concerns are balanced out by the well-established healing issues with surface ablation. "I understand Dr. Marshall's hypothesis and the importance of the anterior lamellar integrity," says Dr. Moshirfar.
"But let's not forget that we still have no definite knowledge about wound healing's effects. A PRK form -8 D is less predictable than a -8 D SBK because of wound healing.
In PRK, there's an acute phase of seven to 10 days of epithelial healing and keratocyte migration, and there's a large area of stromal exposure because of the 7- or 8-mm epithelial defect. There's a lot more corneal remodeling at the level of Bowman's for a -7 or -8 D PRK. With a 90- or 95-µm SBK flap, however, you're still respecting the biomechanics of the cornea to a degree, but you're not dealing with the haphazard wound healing of surface ablation that we haven't mastered yet."
Also, the length of time it takes for a patient to recover his or her vision is also a strike
against PRK, and may ultimately be the main reason flaps, thick or thin, continue to trump surface ablation. "If someone came up with a way to make PRK have the same speed of visual recovery and comfort as SBK, I'd quit doing SBK and do PRK on everyone, because it's easier, quicker and less expensive," says Dr. Durrie. "However, PRK's disadvantages are why LASIK was invented."
1. Durrie DS, Slade SG, Marshall J. Wavefront-guided excimer laser ablation using photorefractive keratectomy and sub-Bowman's keratomileusis: A contralateral eye study. J Refract Surg 2008 Jan;24:1:S77-84.