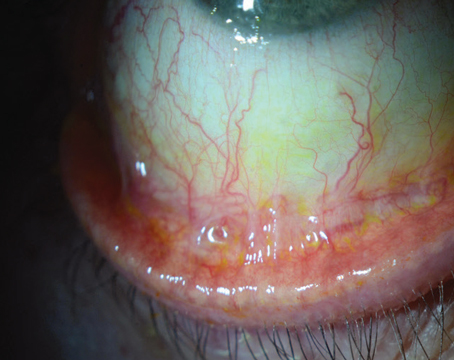
Dacryoadenitis is an inflammation of the lacrimal gland. The initial symptoms typically consist of discomfort in the region of the lacrimal gland (i.e., the superotemporal orbit) and occasionally, pain.1 However, severe cases may be characterized by swelling, tenderness, heat and redness in the tissues surrounding these glands. The inflammation may also lead to reduced function of the lacrimal glands and, consequently, symptoms consistent with dry eyes. The disease may occur unilaterally or bilaterally and is thought to be quite rare. Additional eye symptoms such as photophobia, tearing, production of discharge or a foreign body sensation may also occur. These eye symptoms are likely produced when the local inflammation from an enlarged gland causes compression into the globe.
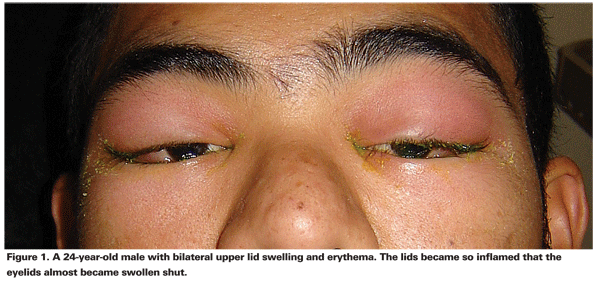
The timing of onset of lacrimal gland inflammation can be a useful distinction when making a diagnosis. Determining whether a patient's presentation is acute or chronic can aid in determining etiology and choosing therapy. The presentation of dacryoadenitis may be quite variable. Acute cases usually present with more severe symptoms. On physical exam, patients with acute dacryoadenitis typically present with an abrupt onset of swelling of the upper lids that is most prominent laterally. The skin overlying the lacrimal glands is usually red and swollen (See Figure 1) and may be warm and tender to palpation. Physical findings that may be associated with the enlarged glands include conjunctival injection, chemosis, and ipsilateral preauricular lymphadenopathy (See Figure 2). Patients with dacryoadenitis may also present with fever or leukocytosis.
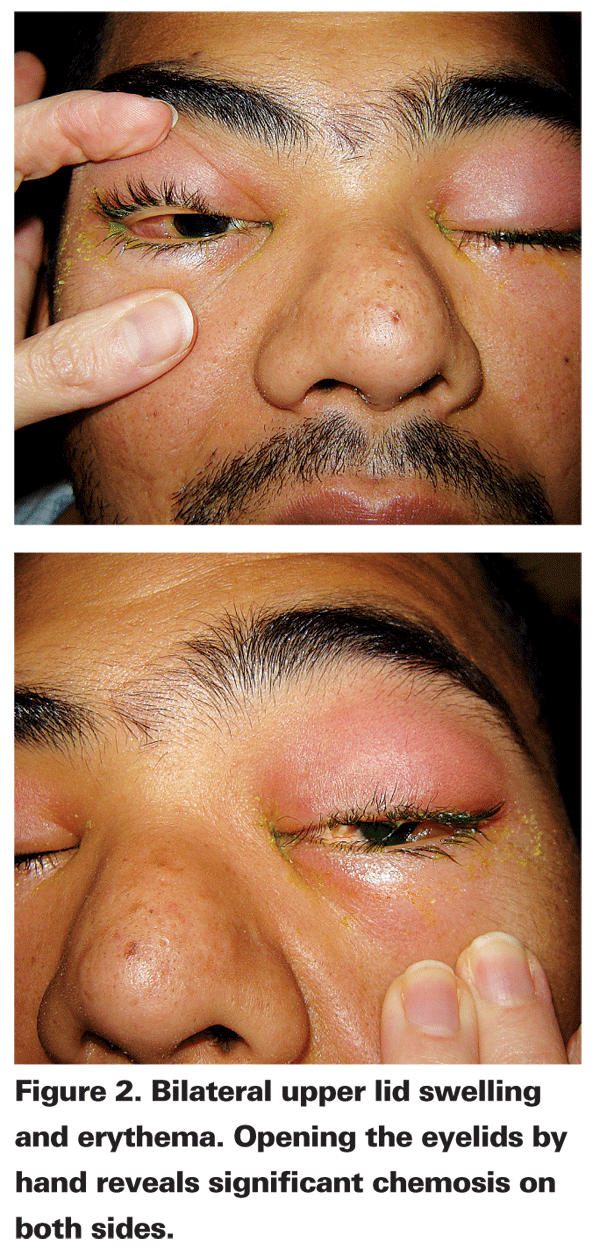
Chronic dacryoadenitis, on the other hand, often presents in a more indolent manner. Patients may notice an enlargement of the lateral eyelids over several months or years. The glands may feel irregular, rather than smooth, on palpation. When taking a history from a patient with dacryoadenitis, focusing on the time course of presentation is very important in determining the likely etiology.
The list of potential etiologies of dacryoadenitis is very extensive. However, each cause may be placed into one of two major categories. These include infectious causes or inflammatory reactions.
Infectious Causes
The possible infectious causes of dacryoadenitis comprise a wide range of pathogens. They include viruses, bacteria, fungi and parasites. Infectious agents are most likely to cause dacryoadenitis to present in an acute fashion. In terms of the infectious causes of dacryoadenitis, viruses are thought to be the most common etiology. Viruses have been recognized as potential causes of lacrimal gland inflammation for several decades. Since the 1950s, EBV has been identified as a frequent viral source of inflammation.2 Other viral causes include cytomegalovirus, herpes simplex virus3 and varicella zoster virus.4
The mumps virus has long been known to be a cause of bilateral dacryoadenitis.5-7 However, due to the widespread practice of immunization in developed countries, infection with the paramyxovirus that causes mumps has become very rare. Mumps usually presents 14 to 21 days after exposure to the virus.8 Although it typically presents with parotitis, the disease course can be quite variable. Multiple organ inflammations may occur, including meningitis, orchitis and pancreatitis.8 In addition, hepatitis, thyroiditis, neuritis, myocarditis and nephritis may occur. It is important to remember when performing a physical exam that viral infections are often associated with regional lymphadenopathy.
The bacterial infectious agents that may cause dacryoadenitis include both gram positive and gram negative organisms. While staphylococci, streptococci and gonococci are often noted as the most frequent bacterial pathogens, haemophilus, moraxella and pseudomonas organisms have also been identified as culprits.2,9 Rare cases of dacryoadenitis have also been associated with brucellosis, tuberculosis, syphilis and Lyme disease.10,11,12
Isolated reports of dacryoadenitis from more unusual pathogens such as cysticercus cellulosae have also been documented and should be considered when evaluating a patient.13
Inflammatory Reactions
The inflammatory etiologies of dacryoadenitis are thought to be more common than the infectious causes. Inflammatory reactions within the lacrimal gland may be associated with sarcoidosis, Wegener's granulomatosis,14 thyroid ophthalmopathy, Sjögren's syndrome and orbital pseudotumor. Dacryoadenitis has also been found in association with inflammatory bowel disease.15
In an article recently published in the Journal of Ophthalmic Plastic and Reconstructive Surgery, a case of bilateral dacryoadenitis was found to be associated with reactive arthritis, following an episode of urethritis. The patient had been diagnosed with urethritis due to Chlamydia trachomatis one month prior to presentation. A lacrimal gland biopsy was found to be negative for any specific infectious etiology. The authors suggested that the patient's dacryoadenitis may represent an autoimmune process similar to the mechanisms that cause conjunctivitis, reactive arthritis, and dermatological manifestations following recent urethritis or enteric infection.16
Orbital pseudotumor may also be a cause of dacryoadenitis, but is generally considered a diagnosis of exclusion. This disease often presents in an acute fashion and is hypersensitive to corticosteroid therapy.
A rare condition that consists of symmetric enlargement of the lacrimal, submandibular and parotid gland is known as Mikulicz's disease.17 In this condition, the swelling is chronic and benign. The lacrimal glands are infiltrated with lymphocytes and the patient's serum has elevated levels of rare antibodies. It has been thought that this disease is a variant of Sjögren's syndrome, however, recent research has revealed that the conditions are different both clinically and histopathologically.18,19 The diagnosis is usually made clinically, once other known etiologies of gland enlargement have been excluded.17 The clinical course is usually self-limited.
Other causes of inflammation in the area of the lacrimal gland that must not be forgotten when evaluating a patient include neoplasms. Malignancy may masquerade as dacryoadenitis. These masses infrequently present in an acute manner.1 Potential malignant lesions of the lacrimal gland that may mimic dacryoadenitis include pleomorphic adenoma,20 lymphoma, melanoma and adenoid cystic carcinoma. If the diagnostic suspicion is high for these tumors, a biopsy is often necessary for diagnosis.
Should one of these diagnoses be obtained on pathology, consultation with a hematologist or oncologist should be done in a timely fashion.
Clinical Evaluation
When a diagnosis of acute dacryoadenitis is suspected, a focused workup of the condition should be initiated. A thorough history and physical is the essential first step.
A detailed history may identify potential risk factors for the condition, such as past medical problems, associated systemic symptoms, history of recent travel and prior immunizations. The physical exam should include a detailed inspection of the gland and surrounding tissue. Examination of other glands of the face, such as the parotid gland, is important to identify any abnormality that may aid in the differential diagnosis. A thorough eye exam is also essential to look for local effects from the inflammation.
In acute cases, where patients appear very ill and exhibit fevers, a CBC and blood cultures should be ordered. Viral serologies, specifically looking for antibodies to EBV, HSV, CMV and mumps may also be ordered. Any discharge that may be present from the gland or eye should be cultured for microbiological analysis.
In cases that may be related to inflammatory disorders, several other diagnostic tests should be considered. These include a chest X-ray, ACE level and gallium scan to evaluate for sarcoidosis. A PPD and CT of the chest may be ordered to evaluate for suspected tuberculosis. A serum c-ANCA will help evaluate for Wegener's granulomatosis, and syphilis serology may also be useful.
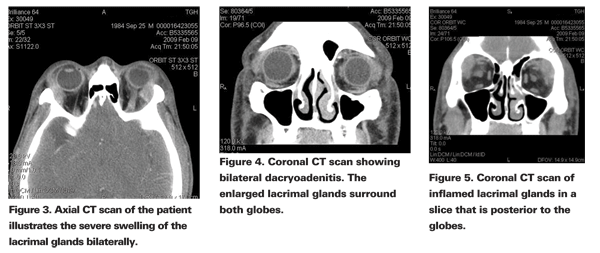
Imaging of the lacrimal gland initially requires a CT scan of the orbit. This is important to identify any other orbital abnormalities that may be associated with dacryoadenitis or radiologic features inconsistent with the diagnosis.
Based on the clinical presentation, systemic workup and clinical course, a decision can be made whether or not a lacrimal gland biopsy is necessary. A biopsy is essential for accurate diagnosis if there is a high suspicion of malignancy.
Treatment
The treatment of dacryoadenitis depends on the etiology. If the etiology is not clearly determined after the clinical and laboratory evaluation, it is often most prudent to treat empirically with antibiotics. This is important because the dacryoadenitis may be due to an undiagnosed bacterial infection, which may respond to medicine. If a bacterial cause is identified, treatment for mild cases may be managed with an oral penicillin derivative, such as amoxicillin, or a cephalosporin, such as cephalexin. In severe cases, treatment with intravenous broad-spectrum antibiotics on an inpatient basis may be necessary. Adjustment of the antibiotic regimen should be based on clinical response.
Viral dacryoadenitis is best managed with intermittent cool compresses, antipyretics and analgesics, until resolution. It has also been suggested that dacryoadenitis from EBV responds well to systemic steroids.21
Inflammatory etiologies should be managed based on the specific treatment for the etiology. In addition, local supportive care to the lacrimal gland region should be administered. Orbital pseudotumor usually responds to oral corticosteroids within one to two days and this quick response to treatment may aid in diagnosis. In cases where this diagnosis has been suspected, but the inflammation does not respond quickly to the oral steroid, alternative etiologies should be sought.
Dacryoadenitis is an unusual condition with many different potential etiologies. A physician who is equipped with the knowledge of its possible causes can institute appropriate management and minimize morbidity.
The Construction Worker with Heavy Eyelids
A 24-year-old Hispanic male with a past medical history significant for asthma and a laceration of his hand two years ago presented to the emergency room complaining of fever and intermittent episodes of nausea. A construction worker for the past three years, he had noticed for the past five days that his eyes were red and his upper eyelids swollen. His medications consisted of an albuterol inhaler that he used twice per week on average. He had no known drug allergies. He had no history of recent travel and had no pets. He had grown up in
He had no eye problems in the past. He also stated that he was concerned because his eyelids had never looked like this before.
Examination
On exam, his visual acuity was 20/50 OU. His intraocular pressure was 22 mmHg OD and 19 mmHg OS. He had no relative afferent pupillary defect and saw 14/14 Ishihara color plates bilaterally. His extraocular movements were limited in all directions bilaterally. Confrontational visual fields, although difficult to obtain due to lid swelling, were full OU. The slit lamp exam revealed significant bilateral upper lid edema and erythema that was most severe along the lateral edge of the orbit. His conjunctiva exhibited chemosis bilaterally and 2+ injection OU. The rest of the slit lamp exam was unremarkable. The dilated fundus exam was normal. Cervical lymphadenopathy was noted bilaterally.
Diagnosis
A systemic workup of the patient was initiated. CBC was normal. CMP was remarkable for an AST of 154, ALT of 197, Alk Phos. of 386, T Bili of 1.3. The GGT was 495. TSH, Rheumatoid Factor, RPR, ANA and ACE levels were normal. Two sets of blood cultures were drawn during the admission, which were both negative. A chest X-ray and abdominal ultrasound were also performed and were normal. A complete panel of serology for viral hepatitis was negative. The patient was PPD negative. Antibodies in the serum for EBV were negative, including a heterophile and monospot test. CMV IgG was positive, but the IgM was negative. The IgG antibody to the measles virus was negative, but the IgM antibody to the mumps virus was positive.
The patient stated that he had never received any immunizations while growing up in
Pathogenesis
The mumps virus is a paramyxovirus that usually presents 14 to 21 days after exposure.
Although it typically presents with parotitis, the disease course can be quite variable.
Multiple organ inflammations may occur, including meningitis, orchitis and pancreatitis.
In addition, hepatitis, thyroiditis, neuritis, myocarditis, nephritis and dacryoadenitis may occur. The patient had a history of not receiving any immunizations as a child, consequently putting him at risk for possible infection.
Prognosis and Management
Infection by the mumps virus is self-limited. The resolution of symptoms, however, may take many weeks.
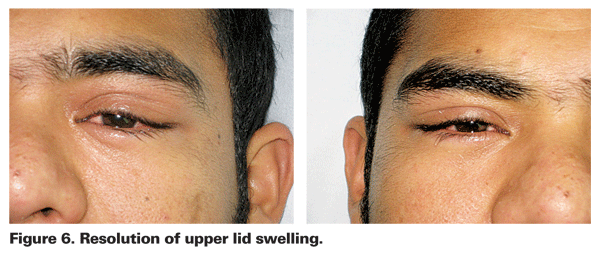
Initially, there was a concern for a bacterial etiology to the patient's dacryoadenitis and he was treated with a course of antibiotics. Once the diagnosis was made, however, this was discontinued. He gradually improved and, after two weeks, his swelling and erythema of his lids had subsided and he no longer had any chemosis.
Dr. Witmer is a second-year resident in the department of ophthalmology at the
1. Kanski JJ. Acute dacryoadenitis. In: Clinical Ophthalmology. A Systematic Approach. 6th ed. Butterworth, Heineman, Elsevier; 2008:178-179.
2. Rhem MN, Wilhelmus KR, Jones DB. Epstein-barr virus dacryoadenitis. Am J Ophthalmol 2000;129:372-5.
3. Foster WJ Jr, Kraus MD, Custer PL. Herpes simplex virus dacryoadenitis in an immunocompromised patient. Arch Ophthalmol 2003;121:911-3.
4. Obata H, Yamagami S, Saito S, et al. A case of acute dacryoadenitis associated with herpes zoster ophthalmicus. Jpn J Ophthalmol 2003;47:107-9.
5. Galpine JF, Walkowski J. A case of mumps with involvement of the lacrimal glands. Br Med J 1952;1(4767):1069-70.
6. Krishna N, Lyda W. Acute suppurative dacryoadenitis as a sequel to mumps. Arch Ophthalmol 1958;59:350-1.
7. Paufique, Hugonnier, Garde. Dacryoadenitis and unilateral paralysis of the elevator muscles due to mumps. Bull Soc Ophtalmol Fr 1955;(9):695,7; discussion, 697-8.
8. Shelburne S, Shandera WX. Infectious diseases: Viral and rickettsial: Mumps. In: Tierney LM, McPhee SJ, Papadakis MA, eds. Current Medical Diagnosis and Treatment. 43rd edition ed. Lange Medical Books/ McGraw-Hill;2004:1307-1308.
9. Mawn LA, Sanon A, Conlon MR, et al. Pseudomonas dacryoadenitis secondary to a lacrimal gland ductule stone. Ophthal Plast Reconstr Surg 1997;13(2):135-8.
10. Bekir NA, Gungor K. Bilateral dacryoadenitis associated with brucellosis. Acta Ophthalmol Scand 1999;77(3):357-8.
11. Nieto JC, Kim N, Lucarelli MJ. Dacryoadenitis and orbital myositis associated with lyme disease. Arch Ophthalmol 2008;126:1165-6.
12. Sen DK. Tuberculosis of the orbit and lacrimal gland: A clinical study of 14 cases. J Pediatr Ophthalmol Strabismus 1980;17(4):232-8.
13. Sen DK. Acute suppurative dacryoadenitis caused by a cysticercus cellulosa. J Pediatr Ophthalmol Strabismus 1982;19(2):100-2.
14. Kiratli H, Sekeroglu MA, Soylemezoglu F. Unilateral dacryoadenitis as the sole presenting sign of Wegener's granulomatosis. Orbit 2008;27(3):157-60.
15. Dutt S, Cartwright MJ, Nelson CC. Acute dacryoadenitis and crohn's disease: Findings and management. Ophthal Plast Reconstr Surg 1992;8(4):295-9.
16. Madge SN, James C, Selva D. Bilateral dacryoadenitis: A new addition to the spectrum of reactive arthritis? Ophthal Plast Reconstr Surg 2009;25(2):152-3.
17. Lee S, Tsirbas A, McCann JD, et al. Mikulicz's disease: A new perspective and literature review. Eur J Ophthalmol 2006;16(2):199-203.
18. Tsubota K, Fujita H, Tsuzaka K, et al. Mikulicz's disease and Sjögren's syndrome. Invest Ophthalmol Vis Sci 2000;41:1666-73.
19. Yamamoto M, Harada S, Ohara M, et al. Clinical and pathological differences between Mikulicz's disease and Sjögren's syndrome. Rheumatology (
20. Halhal M, Meyer A, Morel X, et al. Pleomorphic adenoma mimicking dacryoadenitis. J Fr Ophtalmol 2004;27(10):1200-3.
21. Aburn NS, Sullivan TJ. Infectious mononucleosis presenting with dacryoadenitis. Ophthalmology 1996;103:776-8.